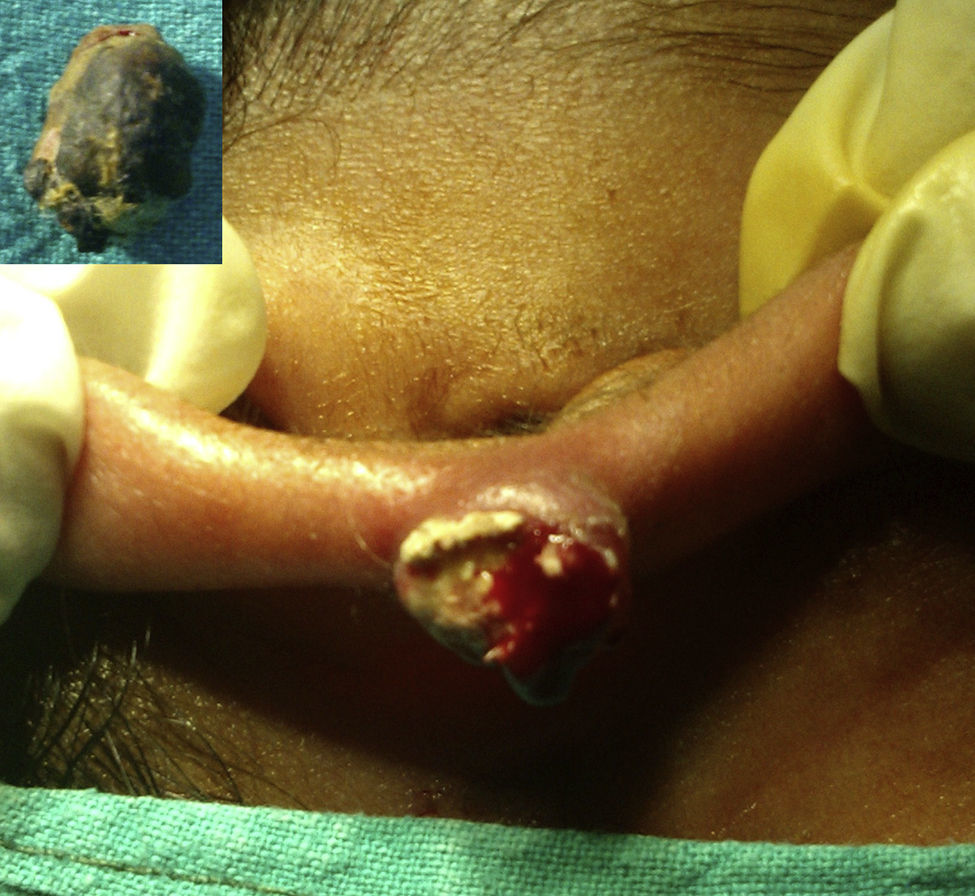
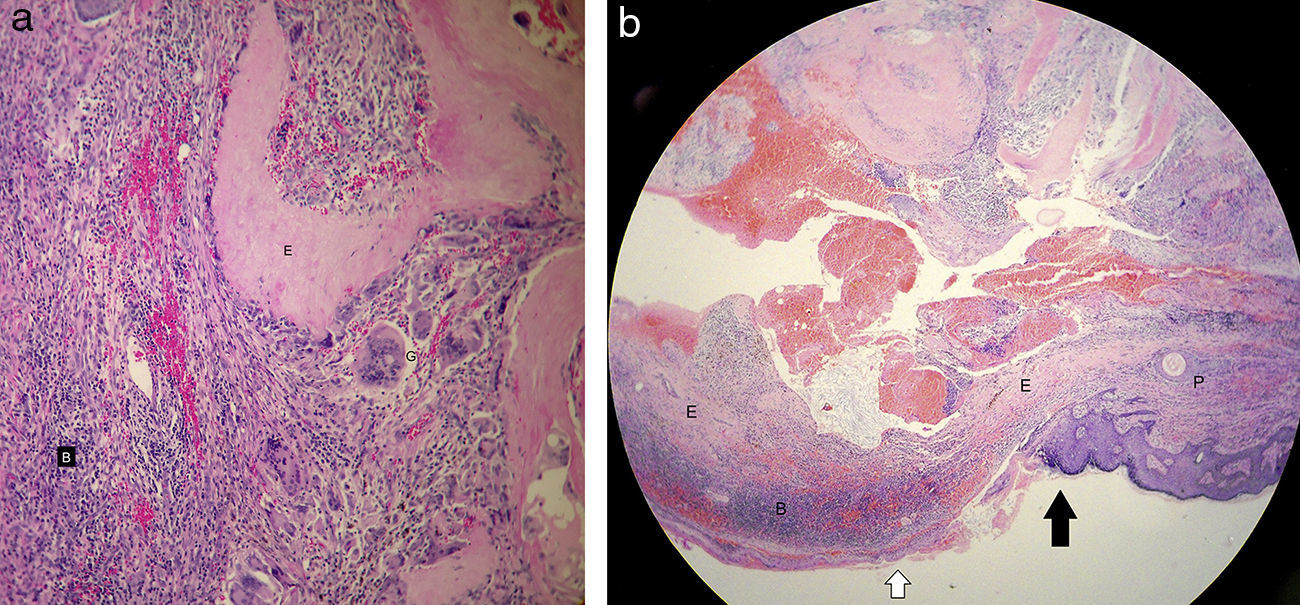
array:24 [ "pii" => "S2173573514000854" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2014.05.018" "estado" => "S300" "fechaPublicacion" => "2015-11-01" "aid" => "600" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "copyrightAnyo" => "2014" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:359-61" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 1799 "formatos" => array:3 [ "EPUB" => 43 "HTML" => 1300 "PDF" => 456 ] ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S0001651914001393" "issn" => "00016519" "doi" => "10.1016/j.otorri.2014.05.010" "estado" => "S300" "fechaPublicacion" => "2015-11-01" "aid" => "600" "copyright" => "Elsevier España, S.L.U. y Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:359-61" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 2065 "formatos" => array:3 [ "EPUB" => 35 "HTML" => 1686 "PDF" => 344 ] ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Caso clínico</span>" "titulo" => "Pilomatricoma perforante que se presenta como una úlcera en el hélix del pabellón auricular" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "359" "paginaFinal" => "361" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Perforating pilomatricoma presenting as an ulcer in the helix of the pinna" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figura 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 605 "Ancho" => 1301 "Tamanyo" => 289176 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">(A) La histopatología muestra una acumulación de células basales basofílicas (B) en la periferia, en un fondo de colagenización generalizada, y las células «fantasma/sombra» anucleadas eosinofílicas (E) en el centro. Nótese el granuloma diseminado (G) (hematoxilina-eosina ×<span class="elsevierStyleHsp" style=""></span>100). (b) La histopatología muestra una rotura epitelial (flecha negra) sin adelgazamiento adyacente (flecha blanca), permitiendo salida de «células fantasma/sombra» eosinofílicas (E) y células basales (B). Nótese la perla de queratina (P) [hematoxilina-eosina; ×<span class="elsevierStyleHsp" style=""></span>50].</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Mainak Dutta, Soumya Ghatak, Rahul Sarkar, Shaswati Sengupta" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Mainak" "apellidos" => "Dutta" ] 1 => array:2 [ "nombre" => "Soumya" "apellidos" => "Ghatak" ] 2 => array:2 [ "nombre" => "Rahul" "apellidos" => "Sarkar" ] 3 => array:2 [ "nombre" => "Shaswati" "apellidos" => "Sengupta" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2173573514000854" "doi" => "10.1016/j.otoeng.2014.05.018" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573514000854?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651914001393?idApp=UINPBA00004N" "url" => "/00016519/0000006600000006/v1_201511140020/S0001651914001393/v1_201511140020/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2173573515001039" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2014.04.002" "estado" => "S300" "fechaPublicacion" => "2015-11-01" "aid" => "586" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:e33-4" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 2482 "formatos" => array:3 [ "EPUB" => 36 "HTML" => 1900 "PDF" => 546 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case study</span>" "titulo" => "<span class="elsevierStyleItalic">Eikenella corrodens</span>: A Rare Cause of Deep Neck Infection" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "e33" "paginaFinal" => "e34" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Infección cervical profunda causada por <span class="elsevierStyleItalic">Eikenella corrodens</span>" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figure 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 947 "Ancho" => 800 "Tamanyo" => 78977 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Axial MRI diffusion slice. Hyper-intense lesion with diffuse edges located on the floor of the mouth.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Fernando Javier Rivas Castillo, Justo Ramón Gómez Martinez, Fernando López Álvarez, Fabián García Velasco" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Fernando Javier" "apellidos" => "Rivas Castillo" ] 1 => array:2 [ "nombre" => "Justo Ramón" "apellidos" => "Gómez Martinez" ] 2 => array:2 [ "nombre" => "Fernando" "apellidos" => "López Álvarez" ] 3 => array:2 [ "nombre" => "Fabián" "apellidos" => "García Velasco" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0001651914001253" "doi" => "10.1016/j.otorri.2014.04.001" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651914001253?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573515001039?idApp=UINPBA00004N" "url" => "/21735735/0000006600000006/v1_201512120041/S2173573515001039/v1_201512120041/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2173573514000866" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2014.07.002" "estado" => "S300" "fechaPublicacion" => "2015-11-01" "aid" => "599" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:356-8" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 2302 "formatos" => array:3 [ "EPUB" => 46 "HTML" => 1717 "PDF" => 539 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case study</span>" "titulo" => "Exostosis of the Internal Auditory Canal: 10-Year Follow-Up" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "356" "paginaFinal" => "358" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Exostosis del conducto auditivo interno: 10 años de seguimento" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1009 "Ancho" => 1400 "Tamanyo" => 181708 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">CT and MRI of 2002.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Guilherme Vianna Coelho, Guilherme Machado de Carvalho, Alexandre Caixeta Guimarães, Leopoldo Nizam Pfeilsticker" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Guilherme Vianna" "apellidos" => "Coelho" ] 1 => array:2 [ "nombre" => "Guilherme Machado" "apellidos" => "de Carvalho" ] 2 => array:2 [ "nombre" => "Alexandre Caixeta" "apellidos" => "Guimarães" ] 3 => array:2 [ "nombre" => "Leopoldo Nizam" "apellidos" => "Pfeilsticker" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0001651914001381" "doi" => "10.1016/j.otorri.2014.05.009" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651914001381?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573514000866?idApp=UINPBA00004N" "url" => "/21735735/0000006600000006/v1_201512120041/S2173573514000866/v1_201512120041/en/main.assets" ] "en" => array:18 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case Study</span>" "titulo" => "Perforating Pilomatricoma Presenting as an Ulcer in the Helix of the Pinna" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "359" "paginaFinal" => "361" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Mainak Dutta, Soumya Ghatak, Rahul Sarkar, Shaswati Sengupta" "autores" => array:4 [ 0 => array:4 [ "nombre" => "Mainak" "apellidos" => "Dutta" "email" => array:1 [ 0 => "duttamainak@yahoo.com" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Soumya" "apellidos" => "Ghatak" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 2 => array:3 [ "nombre" => "Rahul" "apellidos" => "Sarkar" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 3 => array:3 [ "nombre" => "Shaswati" "apellidos" => "Sengupta" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] ] "afiliaciones" => array:2 [ 0 => array:3 [ "entidad" => "Department of Otorhinolaryngology and Head-Neck Surgery, Medical College and Hospital, 88, College Street, Kolkata 700073, India" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Department of Otorhinolaryngology and Head-Neck Surgery, R. G. Kar Medical College and Hospital, Kolkata, India" "etiqueta" => "b" "identificador" => "aff0010" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Perforantes pilomatricomas presentación como una úlcera en el Helix del Pinna" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figure 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 605 "Ancho" => 1300 "Tamanyo" => 310019 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">(a) Histopathology shows aggregate of basophilic basaloid cells (B) at the periphery in a backdrop of generalized collagenization, and the eosinophilic anucleated “ghost/shadow” cells (E) in the center. Note the scattered granuloma (G) [Hematoxylin-Eosin; 100×]. (b) Histopathology shows breach of epithelium (black arrow) with adjacent thinning (white arrow), allowing egress of eosinophilic “shadow/ghost cells” (E) and basaloid cells (B). Note the keratin pearl (P) [Hematoxylin-Eosin; 50×].</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Case Presentation</span><p id="par0005" class="elsevierStylePara elsevierViewall">A 24-year-old woman presented with a painless swelling in her right pinna which was noticed about four months back and had a recent increase in size. On examination, a 1.5×1<span class="elsevierStyleHsp" style=""></span>cm, firm, non-tender skin-colored nodule was seen in the helix. A clinical diagnosis of keloid was rendered. Considering chances of recurrence following surgical excision and because the woman was not concerned about cosmesis, we preferred to wait-and-watch. We were skeptical about the provisional diagnosis though, as she gave no history of ear-prick, a custom common among women for wearing ear-rings, and also because there was a history of transient peri-lesional reddening one month back. She returned two weeks later with the swelling increased in size, erythematous, and covered by crust. The scab was removed and the raw, bleeding, necrotic surface exposed (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>). At this point, we considered some form of chronic granulomatous disease or pyogenic granuloma as alternative possibilities, and went for excision of the lesion. Histopathology revealed predominance of basophilic basaloid cells with scanty cytoplasm at the periphery and anucleated eosinophilic “ghost cells” at the center, with giant cells, foci of keratin and hyaline deposits interspersed in the stroma (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>a). There was a breach in the epithelium and part of it overlying the ulcer was thinned out allowing egress of the inner contents (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>b). The clinico-histologic features suggested perforating pilomatricoma. The patient was followed up for 8 months without any recurrence.</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><elsevierMultimedia ident="fig0010"></elsevierMultimedia></span><span id="sec0010" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0010">Discussion</span><p id="par0010" class="elsevierStylePara elsevierViewall">Pilomatricoma (calcifying epithelioma of Malherbe) is a benign ectodermal tumor of dermis/subcutaneous tissue that originates as a futile attempt of pluripotent cell expression in the germinal matrix center of hair follicles with differentiation toward cortical cells.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> Perforating pilomatricoma is an extremely rare variant characterized by epithelial breach (ulcer). More than 70% present in the head-neck region as ulcers which may ooze or remain covered by crusts, scab or scales, characteristically with peri-lesional erythema and preceded by a rapid spurt of growth.<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2–4</span></a></p><p id="par0015" class="elsevierStylePara elsevierViewall">The mechanism of epithelial thinning and ulceration is yet to be understood properly. The phenomenon has been explained by “transepithelial elimination”,<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a> though by original definition the term connotes channeling of the thickened epithelium that behaves as specific biologic connective tissue unit, and subsequent elimination of inner cellular content without any epithelial injury.<a class="elsevierStyleCrossRef" href="#bib0030"><span class="elsevierStyleSup">6</span></a> Interestingly, Ohnishi et al.<a class="elsevierStyleCrossRef" href="#bib0035"><span class="elsevierStyleSup">7</span></a> observed that the sites of ulceration did not corroborate with the foci of elimination; such examples did show epithelial channels and the ulcerations were mere co-existences. Presence of frank epithelial breach allowing egress of inner contents, as seen in our patient, is therefore not a common finding in the so-called “perforating” variant. In an aging tumor, the “ghost/shadow cells” are generally found as the predominant cellular entity in relation to the breached epidermis during elimination process. Incidentally, perforating pilomatricomas are often observed in the elderly. As the tumor ages, the inner eosinophilic “ghost cells” increase at the expense of the outer basophilic cells with formation of keratin debris, dystrophic calcification and collagenization which act as foreign entities needing expulsion. However, tumor aging does not always corroborate with the patient's age as such lesions are also seen in children and young adults in about 40% cases.</p><p id="par0020" class="elsevierStylePara elsevierViewall">More relevant clinically is their potential for being misdiagnosed. Conventional pilomatricomas are diagnosed correctly, combining clinico-radiologic and cytologic impressions, in only about 29% cases,<a class="elsevierStyleCrossRef" href="#bib0040"><span class="elsevierStyleSup">8</span></a> and perforating pilomatricoma being an extremely rare form is more liable to be misinterpreted. Like conventional pilomatricomas, they occur at areas of intermediate hair, like hair borders, mostly involving the scalp, neck, cheek and peri-orbita.<a class="elsevierStyleCrossRefs" href="#bib0020"><span class="elsevierStyleSup">4,6</span></a> Conventional pilomatricoma is primarily a disease of children and young adults,<a class="elsevierStyleCrossRef" href="#bib0045"><span class="elsevierStyleSup">9</span></a> but the perforating variant is more common in adults and the elderly. Thus, a reddish ulcer that oozes and crusts in this age-group in given anatomic areas could be misdiagnosed as basal or squamous cell carcinoma - and in the pinna, they might masquerade as pyogenic granuloma, keratoacanthoma, or amelanotic malignant melanoma.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> In such cases, a punch biopsy would be diagnostic. They are treated by simple excision with watchful follow-up for possible recurrences.<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">4</span></a></p><p id="par0025" class="elsevierStylePara elsevierViewall">Perforating pilomatricoma in the pinna is extremely rare – only two cases have been reported previously - one in the triangular fossa<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a>, the other in the lobule,<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> and helix as a subsite has never been documented before. Ear-prick has been the inciting event in one patient,<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> but is not a universal pre-requisite. Superficial location and vascular compromise might contribute, but not much is known about the specific factors that trigger such ulcerations. For otolaryngologists dealing with ulcerative lesions in the head-neck area, it is important to consider perforating pilomatricoma as a possible diagnosis. A firm, painless cutaneous lesion in the face and neck near hair borders that has persisted for months and has undergone a recent spurt of growth associated with or followed by ulceration, crusting, oozing and erythema should seriously be considered as perforating pilomatricoma, and should be subjected to a punch or excisional biopsy for histologic confirmation. In this report, we have illustrated a representative case of perforating pilomatricoma in the helix of the pinna; although seldom encountered and notoriously misdiagnosed, it has its characteristic clinical features that can distinguish it from the common ulcerative lesions of head and neck.</p></span><span id="sec0015" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0015">Conflict of Interest</span><p id="par0035" class="elsevierStylePara elsevierViewall">The authors have no conflicts of interest to declare.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:5 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Case Presentation" ] 1 => array:2 [ "identificador" => "sec0010" "titulo" => "Discussion" ] 2 => array:2 [ "identificador" => "sec0015" "titulo" => "Conflict of Interest" ] 3 => array:2 [ "identificador" => "xack197872" "titulo" => "Acknowledgment" ] 4 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "fechaRecibido" => "2014-04-12" "fechaAceptado" => "2014-05-25" "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Dutta M, Ghatak S, Sarkar R, Sengupta S. Perforantes pilomatricomas presentación como una úlcera en el Helix del Pinna. 2015;66:359–361.</p>" ] ] "multimedia" => array:2 [ 0 => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 896 "Ancho" => 975 "Tamanyo" => 176435 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">The ulcerative lesion with mild erythema and oozing of necrotic slough and blood seen in the helix of right pinna (inset: the operculum-like scab that covered the lesion at presentation).</p>" ] ] 1 => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figure 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 605 "Ancho" => 1300 "Tamanyo" => 310019 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">(a) Histopathology shows aggregate of basophilic basaloid cells (B) at the periphery in a backdrop of generalized collagenization, and the eosinophilic anucleated “ghost/shadow” cells (E) in the center. Note the scattered granuloma (G) [Hematoxylin-Eosin; 100×]. (b) Histopathology shows breach of epithelium (black arrow) with adjacent thinning (white arrow), allowing egress of eosinophilic “shadow/ghost cells” (E) and basaloid cells (B). Note the keratin pearl (P) [Hematoxylin-Eosin; 50×].</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:9 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Morphological stages of pilomatricoma" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "S. Kaddu" 1 => "H.P. Soyer" 2 => "S. Hodl" 3 => "H. Kerl" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Am J Dermatopathol" "fecha" => "1996" "volumen" => "18" "paginaInicial" => "333" "paginaFinal" => "338" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/8879294" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "A patient with ulcerated calcifying epithelioma of Malherbe in the pinna: case report" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "T. Upile" 1 => "W. Jerjes" 2 => "F. Sipaul" 3 => "A. Sandison" 4 => "P. Kafas" 5 => "M. Al-Khawalde" ] ] ] ] ] "host" => array:2 [ 0 => array:2 [ "doi" => "10.1186/1758-3284-4-25" "Revista" => array:5 [ "tituloSerie" => "Head Neck Oncol" "fecha" => "2012" "volumen" => "4" "paginaInicial" => "25" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/22613633" "web" => "Medline" ] ] ] ] 1 => array:2 [ "doi" => "10.1186/1758-3284-4-25" "WWW" => array:1 [ "link" => "http://www.headandneckoncology.org/content/4/1/25" ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Pilomatrixoma of the earlobe" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:5 [ 0 => "K. Sevin" 1 => "Z. Can" 2 => "S. Yilmaz" 3 => "A. Saray" 4 => "E. Yormuk" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Dermatol Surg" "fecha" => "1995" "volumen" => "21" "paginaInicial" => "245" "paginaFinal" => "246" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/7712097" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Pilomatrical neoplasms in children and young adults" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "A.J. Marrogi" 1 => "M.R. Wick" 2 => "L.P. Dehner" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Am J Dermatopathol" "fecha" => "1992" "volumen" => "14" "paginaInicial" => "87" "paginaFinal" => "94" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/1566981" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "General pathology: terminology" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "A.H. Mehregan" 1 => "K. Hashimoto" 2 => "D.A. Mehregan" 3 => "D.R. Mehregan" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "LibroEditado" => array:4 [ "titulo" => "Pinkus’ guide to dermatohistopathology" "paginaInicial" => "92" "edicion" => "6th ed." "serieFecha" => "1995" ] ] ] ] ] ] 5 => array:3 [ "identificador" => "bib0030" "etiqueta" => "6" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Perforating pilomatricoma: transepithelial elimination or not" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "Y. Honda" 1 => "T. Oh-i" 2 => "M. Koga" 3 => "Y. Tokuda" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "J Dermatol" "fecha" => "2002" "volumen" => "29" "paginaInicial" => "100" "paginaFinal" => "103" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/11890292" "web" => "Medline" ] ] ] ] ] ] ] ] 6 => array:3 [ "identificador" => "bib0035" "etiqueta" => "7" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Perforating pilomatricoma in a process of total elimination" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "T. Ohnishi" 1 => "Y. Nakamura" 2 => "S. Watanabe" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1067/mjd.2003.322" "Revista" => array:6 [ "tituloSerie" => "J Am Acad Dermatol" "fecha" => "2003" "volumen" => "49" "paginaInicial" => "S146" "paginaFinal" => "S147" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/12894105" "web" => "Medline" ] ] ] ] ] ] ] ] 7 => array:3 [ "identificador" => "bib0040" "etiqueta" => "8" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Pilomatrixoma: a review of 346 cases" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:5 [ 0 => "A. Pirouzmanesh" 1 => "J.F. Reinisch" 2 => "I. Gonzalez-Gomez" 3 => "E.M. Smith" 4 => "J.G. Meara" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1097/01.PRS.0000091160.54278.64" "Revista" => array:6 [ "tituloSerie" => "Plast Reconstr Surg" "fecha" => "2003" "volumen" => "112" "paginaInicial" => "1784" "paginaFinal" => "1789" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/14663221" "web" => "Medline" ] ] ] ] ] ] ] ] 8 => array:3 [ "identificador" => "bib0045" "etiqueta" => "9" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Pediatric parotideomasseteric pilomatrixoma in children" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "R. Salzman" 1 => "I. Starek" 2 => "H. Faisal" 3 => "T. Tichy" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.5507/bp.2013.063" "Revista" => array:2 [ "tituloSerie" => "Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub" "fecha" => "2013" ] ] ] ] ] ] ] ] ] ] "agradecimientos" => array:1 [ 0 => array:4 [ "identificador" => "xack197872" "titulo" => "Acknowledgment" "texto" => "<p id="par0030" class="elsevierStylePara elsevierViewall">We thank Debabrata Bandyopadhyay, MD, Professor and Head, Department of Dermatology, Venereology and Leprosy, Medical College and Hospital, Kolkata, India, for his kind advices in preparing the manuscript.</p>" "vista" => "all" ] ] ] "idiomaDefecto" => "en" "url" => "/21735735/0000006600000006/v1_201512120041/S2173573514000854/v1_201512120041/en/main.assets" "Apartado" => array:4 [ "identificador" => "5881" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Case Studies" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/21735735/0000006600000006/v1_201512120041/S2173573514000854/v1_201512120041/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573514000854?idApp=UINPBA00004N" ]
Journal Information
Vol. 66. Issue 6.
Pages 359-361 (November - December 2015)
Share
Download PDF
More article options
Vol. 66. Issue 6.
Pages 359-361 (November - December 2015)
Case Study
Perforating Pilomatricoma Presenting as an Ulcer in the Helix of the Pinna
Perforantes pilomatricomas presentación como una úlcera en el Helix del Pinna
Visits
1846
This item has received
Article information
These are the options to access the full texts of the publication Acta Otorrinolaringológica Española
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail