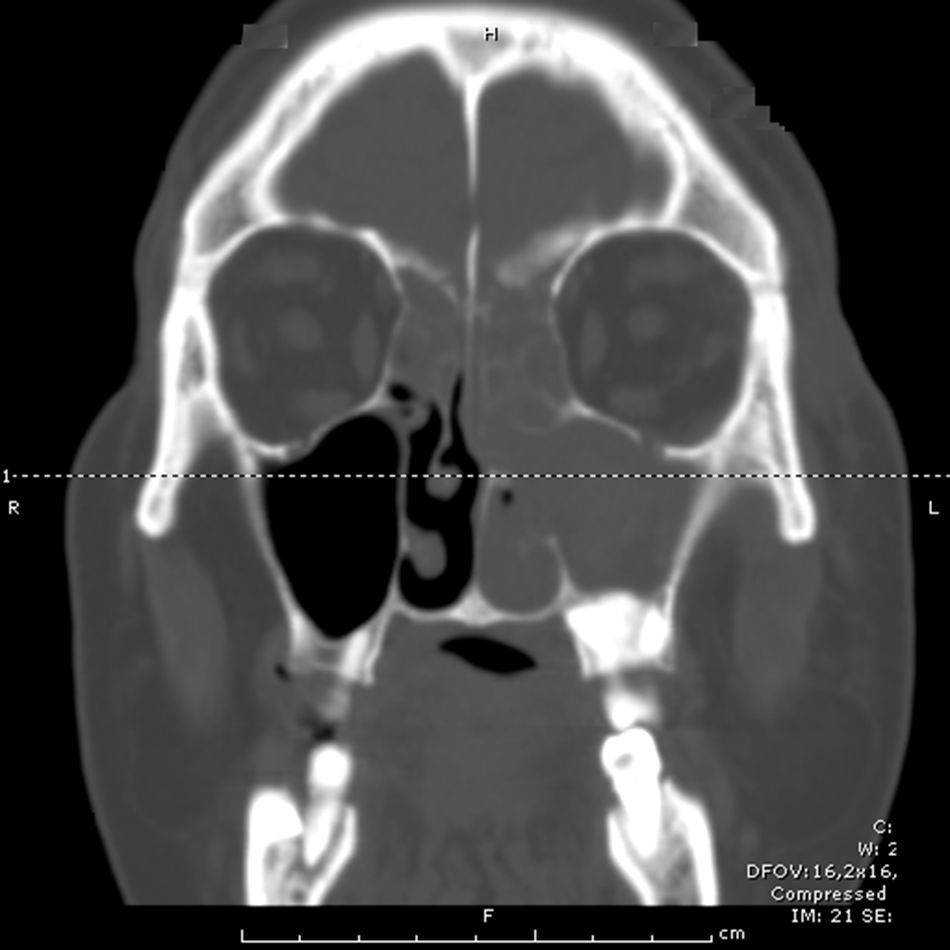
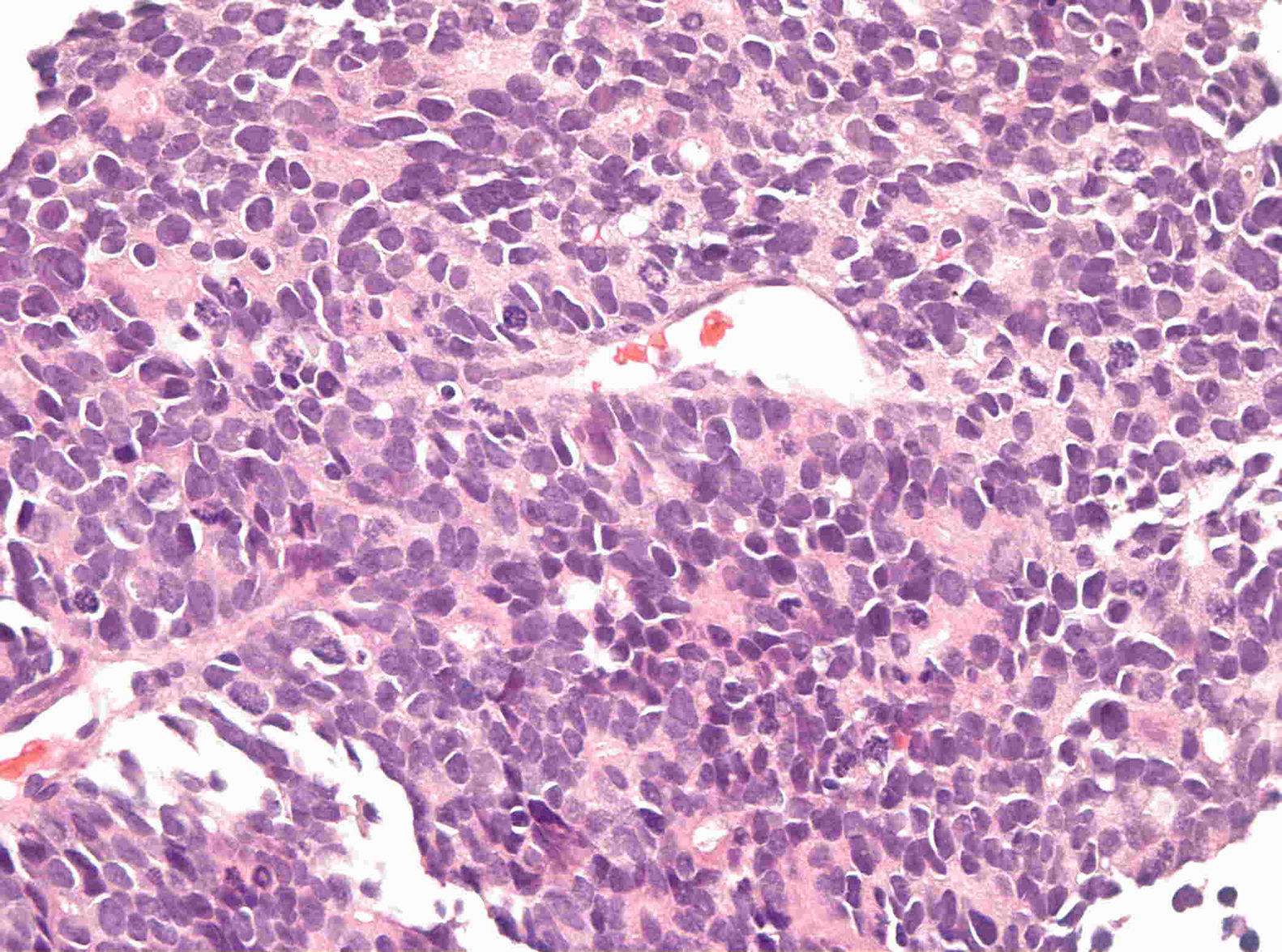
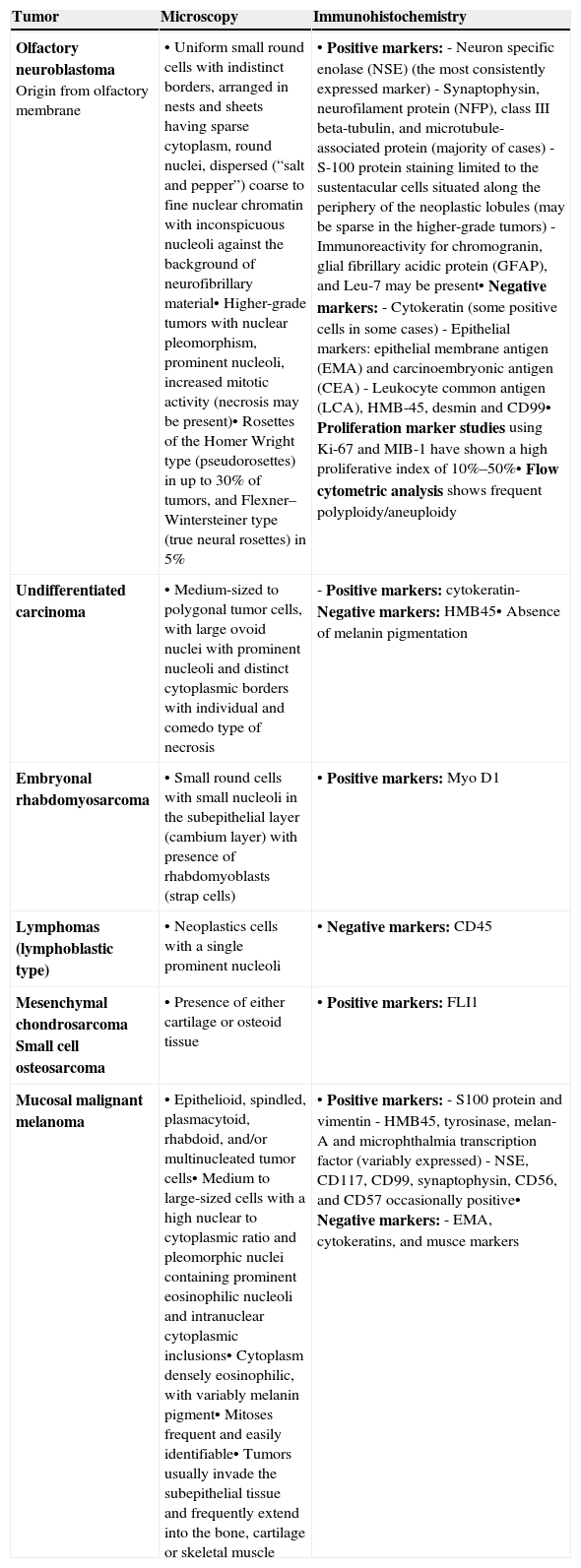
array:24 [ "pii" => "S2173573514000167" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2014.02.015" "estado" => "S300" "fechaPublicacion" => "2015-05-01" "aid" => "546" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "copyrightAnyo" => "2013" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:171-4" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 2850 "formatos" => array:3 [ "EPUB" => 82 "HTML" => 1958 "PDF" => 810 ] ] "Traduccion" => array:1 [ "es" => array:18 [ "pii" => "S0001651914000260" "issn" => "00016519" "doi" => "10.1016/j.otorri.2013.09.006" "estado" => "S300" "fechaPublicacion" => "2015-05-01" "aid" => "546" "copyright" => "Elsevier España, S.L.U. y Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:171-4" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 3884 "formatos" => array:3 [ "EPUB" => 81 "HTML" => 2891 "PDF" => 912 ] ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Caso clínico</span>" "titulo" => "Sarcoma de Ewing: una rareza en la región nasosinusal" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "171" "paginaFinal" => "174" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Ewing's sarcoma: A rarity in sinonasal region" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figura 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 940 "Ancho" => 1266 "Tamanyo" => 395358 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Sarcoma de Ewing (luz microscópica, hematoxilina y eosina).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Sara Cruz, Paula Azevedo, Nuno Trigueiros, Manuel Rodrigues e Rodrigues" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Sara" "apellidos" => "Cruz" ] 1 => array:2 [ "nombre" => "Paula" "apellidos" => "Azevedo" ] 2 => array:2 [ "nombre" => "Nuno" "apellidos" => "Trigueiros" ] 3 => array:2 [ "nombre" => "Manuel" "apellidos" => "Rodrigues e Rodrigues" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2173573514000167" "doi" => "10.1016/j.otoeng.2014.02.015" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573514000167?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651914000260?idApp=UINPBA00004N" "url" => "/00016519/0000006600000003/v2_201505090749/S0001651914000260/v2_201505090749/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2173573514000179" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2014.02.016" "estado" => "S300" "fechaPublicacion" => "2015-05-01" "aid" => "547" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:175-7" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 1732 "formatos" => array:3 [ "EPUB" => 47 "HTML" => 1252 "PDF" => 433 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case Study</span>" "titulo" => "Temporal Bone Myeloid Sarcoma" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "175" "paginaFinal" => "177" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Sarcoma mieloide del hueso temporal" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 647 "Ancho" => 800 "Tamanyo" => 43876 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Right otoscopy: otorrhea, tympanic membrane purple bulging.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Clara Silva, Natércia Silvestre, Ana Margarida Amorim, António Paiva" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Clara" "apellidos" => "Silva" ] 1 => array:2 [ "nombre" => "Natércia" "apellidos" => "Silvestre" ] 2 => array:2 [ "nombre" => "Ana Margarida" "apellidos" => "Amorim" ] 3 => array:2 [ "nombre" => "António" "apellidos" => "Paiva" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0001651914000272" "doi" => "10.1016/j.otorri.2013.09.007" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651914000272?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573514000179?idApp=UINPBA00004N" "url" => "/21735735/0000006600000003/v1_201506160927/S2173573514000179/v1_201506160927/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2173573515000423" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2015.05.003" "estado" => "S300" "fechaPublicacion" => "2015-05-01" "aid" => "638" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "article" "crossmark" => 1 "subdocumento" => "pgl" "cita" => "Acta Otorrinolaringol Esp. 2015;66:159-70" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 16163 "formatos" => array:3 [ "EPUB" => 117 "HTML" => 12747 "PDF" => 3299 ] ] "en" => array:13 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Review article</span>" "titulo" => "Recommendations for Management of Acute Pharyngitis in Adults" "tienePdf" => "en" "tieneTextoCompleto" => "en" "tieneResumen" => array:2 [ 0 => "en" 1 => "es" ] "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "159" "paginaFinal" => "170" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Recomendaciones para el manejo de la faringoamigdalitis aguda del adulto" ] ] "contieneResumen" => array:2 [ "en" => true "es" => true ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figure 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 1674 "Ancho" => 2731 "Tamanyo" => 198423 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0020" class="elsevierStyleSimplePara elsevierViewall">Management of sore throat in the community pharmacy. *Refer as per protocol.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Josep M. Cots, Juan-Ignacio Alós, Mario Bárcena, Xavier Boleda, José L. Cañada, Niceto Gómez, Ana Mendoza, Isabel Vilaseca, Carles Llor" "autores" => array:9 [ 0 => array:2 [ "nombre" => "Josep M." "apellidos" => "Cots" ] 1 => array:2 [ "nombre" => "Juan-Ignacio" "apellidos" => "Alós" ] 2 => array:2 [ "nombre" => "Mario" "apellidos" => "Bárcena" ] 3 => array:2 [ "nombre" => "Xavier" "apellidos" => "Boleda" ] 4 => array:2 [ "nombre" => "José L." "apellidos" => "Cañada" ] 5 => array:2 [ "nombre" => "Niceto" "apellidos" => "Gómez" ] 6 => array:2 [ "nombre" => "Ana" "apellidos" => "Mendoza" ] 7 => array:2 [ "nombre" => "Isabel" "apellidos" => "Vilaseca" ] 8 => array:2 [ "nombre" => "Carles" "apellidos" => "Llor" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0001651915000084" "doi" => "10.1016/j.otorri.2015.01.001" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651915000084?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573515000423?idApp=UINPBA00004N" "url" => "/21735735/0000006600000003/v1_201506160927/S2173573515000423/v1_201506160927/en/main.assets" ] "en" => array:17 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case Study</span>" "titulo" => "Ewing's Sarcoma: A Rarity in Sinonasal Region" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "171" "paginaFinal" => "174" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Sara Cruz, Paula Azevedo, Nuno Trigueiros, Manuel Rodrigues e Rodrigues" "autores" => array:4 [ 0 => array:4 [ "nombre" => "Sara" "apellidos" => "Cruz" "email" => array:1 [ 0 => "saramadalena@hotmail.com" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Paula" "apellidos" => "Azevedo" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 2 => array:3 [ "nombre" => "Nuno" "apellidos" => "Trigueiros" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 3 => array:3 [ "nombre" => "Manuel" "apellidos" => "Rodrigues e Rodrigues" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] ] "afiliaciones" => array:2 [ 0 => array:3 [ "entidad" => "Hospital Pedro Hispano, Matosinhos, Portugal" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Otolaryngology Department, Hospital Pedro Hispano, Matosinhos, Portugal" "etiqueta" => "b" "identificador" => "aff0010" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Sarcoma de Ewing: una rareza en la región nasosinusal" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 950 "Ancho" => 950 "Tamanyo" => 66714 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">SPN CT image of the left Ewing sarcoma (coronal view).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Case Report</span><p id="par0005" class="elsevierStylePara elsevierViewall">A 54-year-old man was presented in ENT to consult 2 months of progressive nasal obstruction and to epistaxis accompanied by progressive periorbitary and cheek swelling. He was a diabetic and hypertensive patient with a poor general state, submitted to a radical prostatectomy in 2007, followed by chemotherapy (QT) and radiotherapy (RT) to treat a prostate carcinoma with bone, liver and lung metastases.</p><p id="par0010" class="elsevierStylePara elsevierViewall">Rhinoscopy revealed a crispy neoformation that obstructed the left nasal cavity, without nasopharynx extension. Patient had a left periorbital and cheek swelling and no palpable cervical lymphadenopathy.</p><p id="par0015" class="elsevierStylePara elsevierViewall">The paranasal sinuses CT scan showed a large soft tissue density lesion completely filling the left maxillary sinus and nasal cavity, without bone erosions (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>). There were present cerebral metastases.</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0020" class="elsevierStylePara elsevierViewall">The histopathology revealed at microscopy fragments of nasal mucosa infiltrated by neoplasm composed of small cells with scanty cytoplasm, hyperchromatic and rounded nuclei, arranged in towel and sometimes in Homer-Wright rosettes type, with numerous mitotic figures. Immunohistochemistry was positive for CD99, vimentina, CAM 5.2 and chromogranin (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>). Synaptophysin, neuron specific enolase (NSE), neurofilament protein, S100 protein, GFAP, CK7, LCA and PSA were negative. The anatamopathological result was compatible with a soft tissue sinonasal Ewing's sarcoma.</p><elsevierMultimedia ident="fig0010"></elsevierMultimedia><p id="par0025" class="elsevierStylePara elsevierViewall">The patient underwent medical treatment with topic and systemic corticotherapy and systemic antibiotic. He was proposed for palliative care due to its poor general condition, advanced tumor stage and presence of a metastatic prostate tumor. He died three months after diagnosis.</p></span><span id="sec0010" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0010">Discussion</span><p id="par0030" class="elsevierStylePara elsevierViewall">Ewing's sarcoma (ES) is a highly malignant small round cell tumor of mesenchymal origin.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1,2</span></a> This was first described by Ewing in 1921.<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2,3</span></a> Ewings sarcoma (ES)/primitive neuroectodermal tumor (PNET) are closely related family of small round cell sarcomas with varying degrees of neuroectodermal differentiation.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1–3</span></a> PNETs show neuroectodermal differentiation, whereas ES lack them as assessed by light microscopy, immunohistochemistry, and electron microscopy.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a></p><p id="par0035" class="elsevierStylePara elsevierViewall">These tumors can arise from bone (skeletal type) or occasionally from soft tissues (extra skeletal type).<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> The skeletal type is more frequent and occurs in long bones of the extremities.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> The extra skeletal form has the same histological, immunohistochemical and molecular features of skeletal ES and affects soft tissue of lower limbs, paravertebral tissues, chest wall, retroperitoneum and rare in head and neck region (2%–7%).<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2,3</span></a> Mandible and maxilla are the most common sites affected in the head and neck region and involvement of the paranasal sinuses is very rare.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1–3</span></a> Few cases of extra skeletal ES have been published in world literature.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a></p><p id="par0040" class="elsevierStylePara elsevierViewall">It usually affects individuals less than 20 years old, with a male preponderance.<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2,3</span></a> Although the exact etiology remains unknown, majority has a specific gene sequence <span class="elsevierStyleItalic">t</span>(11:22)(q24:q12) i.e., fusion between the 5′ end of the EWS gene from chromosome band 22q12 with the 3′ portion of the 11q24 FLI1 gene, a member of the ETS family of transcription factors.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1–4</span></a> This EWS/ETS fusion protein blocks the differentiation of pluripotent marrow stromal cells. Rest of the 10%–15% cases have <span class="elsevierStyleItalic">t</span>(21;22)(q22;q12) fusing EWS to a closely related ETS gene, ERG from chromosome band 21q22. In less than 1% of cases, <span class="elsevierStyleItalic">t</span>(7;22), <span class="elsevierStyleItalic">t</span>(17;22), <span class="elsevierStyleItalic">t</span>(2;22) and inv(22) have been found that give rise to fusions between EWS and the ETS genes like ETV1, E1AF, FEV, and ZSG, respectively. Mutations associated with P53 or P16/p14 ARF have high aggressive behavior and poor hemotherapeutic response.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a></p><p id="par0045" class="elsevierStylePara elsevierViewall">The clinic depends on the location of the tumor. Sinonasal tumors only provide sinus symptoms such as nasal obstruction and epistaxis, in very advanced stages, thus delaying its diagnostic.<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a></p><p id="par0050" class="elsevierStylePara elsevierViewall">Imaging exams, particularly computerized tomography (CT) are important for the diagnosis, however ES images are not specific. In this patient, the CT scan pointed more to a benign lesion with associated sinusitis than a malignant lesion, because there were no bone erosions suggestive of malignancy.</p><p id="par0055" class="elsevierStylePara elsevierViewall">The definitive diagnosis is made by histology of the lesion.<a class="elsevierStyleCrossRefs" href="#bib0015"><span class="elsevierStyleSup">3,5</span></a> At microscopy the ES are tumors composed of small round cells, with round nuclei, containing fine chromatin, scanty clear or eosinophilic cytoplasm with poorly defined limits, containing PAS positive intracytoplasmic glycogen granules.<a class="elsevierStyleCrossRefs" href="#bib0015"><span class="elsevierStyleSup">3,5</span></a> The essential diagnostic test is for the specific immunocytochemical CD99/013 marker. This is a surface protein detected by AC013 although is not specific for ES/PNET is found in almost all ES and PNETs and combination with other markers like FLI1, HNK1 and CAV1 gives more accurate diagnosis and helps to avoid erroneous diagnosis. This test has a sensitivity of 98%.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a></p><p id="par0060" class="elsevierStylePara elsevierViewall">The differential diagnosis involves a wide variety of small round cell tumors like poorly differentiated neoplasms of the sinonasal region as olfactory neuroblastoma, lymphoma, undifferentiated carcinoma, sinonasal melanoma, acute leukemia, embryonal rhabdomyosarcoma, sinus mesenchymal chondrosarcoma, osteosarcoma small cell and small neuroendocrine cell carcinoma.<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2,3</span></a> In <a class="elsevierStyleCrossRef" href="#tbl0005">Table 1</a> are listed some the characteristics of these tumors.</p><elsevierMultimedia ident="tbl0005"></elsevierMultimedia><p id="par0065" class="elsevierStylePara elsevierViewall">In our case synaptophysin, neuron specific enolase (NSE), neurofilament protein, S100 protein, GFAP, CK7, LCA and PSA were negative, ruling out the chances of small cell carcinoma, poorly differentiated sinonasal carcinoma, olfactory neuroblastoma or lymphoma.</p><p id="par0070" class="elsevierStylePara elsevierViewall">ES metastasizes in about 18% of cases, most often to the lungs (57%), bone (34%), brain and spinal cord, and rarely to the ganglia.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> In this case, the concomitant presence of another metastatic prostate tumor did not allowed to distinguish the origin of metastases.</p><p id="par0075" class="elsevierStylePara elsevierViewall">The prognosis depends on the age of the patient, anatomic location, tumor size and stage, being better in younger patients, with axial disease, small tumors (<8<span class="elsevierStyleHsp" style=""></span>cm diameter), with volume less than 100<span class="elsevierStyleHsp" style=""></span>ml and absence of metastasis at diagnosis. Bone metastases have better prognosis than lung metastases.<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2,3,5</span></a> The 5-year survival of patients with metastases at diagnosis is around 22% versus 55% in patients without metastases.<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2,3,5</span></a></p><p id="par0080" class="elsevierStylePara elsevierViewall">Therapeutic options are surgery, chemotherapy (QT) and/or radiotherapy (RT).<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a> Local control of the tumor with surgery and/or RT is subsequently followed by metastatic treatment with QT.<a class="elsevierStyleCrossRefs" href="#bib0015"><span class="elsevierStyleSup">3,5</span></a> The most effective treatment for these tumors is surgery followed by QT/RT. In cases where surgery is not possible due to the extension of the tumor or patient's co-morbidities, the QT/RT is a valid option.<a class="elsevierStyleCrossRefs" href="#bib0015"><span class="elsevierStyleSup">3,5</span></a> Combination chemotherapy (vincristine, doxorubicin, cyclophosphamide and actinomycin) is more effective than monotherapy.<a class="elsevierStyleCrossRefs" href="#bib0025"><span class="elsevierStyleSup">5,6</span></a> RT is reserved for patients in whom surgical excision was incomplete or not held because of the morbidity. Local control is achieved in 85% of cases with a 5-year survival rate of 55%–60%.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a></p><p id="par0085" class="elsevierStylePara elsevierViewall">This patient was not proposed initially to surgery because he has an advanced stage ES as well as a metastatic prostate carcinoma.</p><p id="par0090" class="elsevierStylePara elsevierViewall">The rarity of sinonasal ES and the difficult access to this anatomical region make it diagnosis and treatment difficult.</p></span><span id="sec0015" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0015">Conclusion</span><p id="par0095" class="elsevierStylePara elsevierViewall">Sinonasal primary Ewing's sarcoma is a very rare tumor, with a difficult diagnosis, for which it is important to the clinics complemented by image methods. However, it is the histological and immunohistochemical analysis that gives the diagnosis of certainty.</p></span><span id="sec0020" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0020">Conflicts of Interest</span><p id="par0100" class="elsevierStylePara elsevierViewall">The authors have no conflicts of interest.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:5 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Case Report" ] 1 => array:2 [ "identificador" => "sec0010" "titulo" => "Discussion" ] 2 => array:2 [ "identificador" => "sec0015" "titulo" => "Conclusion" ] 3 => array:2 [ "identificador" => "sec0020" "titulo" => "Conflicts of Interest" ] 4 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "fechaRecibido" => "2013-04-09" "fechaAceptado" => "2013-09-10" "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Cruz S, Azevedo P, Trigueiros N, Rodrigues e Rodrigues M. Sarcoma de Ewing: una rareza en la región nasosinusal. 2015;66:171–174.</p>" ] ] "multimedia" => array:3 [ 0 => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 950 "Ancho" => 950 "Tamanyo" => 66714 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">SPN CT image of the left Ewing sarcoma (coronal view).</p>" ] ] 1 => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figure 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 1175 "Ancho" => 1582 "Tamanyo" => 528450 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Ewing's sarcoma (light microscopy, hematoxylin and eosin).</p>" ] ] 2 => array:7 [ "identificador" => "tbl0005" "etiqueta" => "Table 1" "tipo" => "MULTIMEDIATABLA" "mostrarFloat" => true "mostrarDisplay" => false "tabla" => array:1 [ "tablatextoimagen" => array:1 [ 0 => array:2 [ "tabla" => array:1 [ 0 => """ <table border="0" frame="\n \t\t\t\t\tvoid\n \t\t\t\t" class=""><thead title="thead"><tr title="table-row"><th class="td" title="table-head " align="left" valign="top" scope="col" style="border-bottom: 2px solid black">Tumor \t\t\t\t\t\t\n \t\t\t\t</th><th class="td" title="table-head " align="left" valign="top" scope="col" style="border-bottom: 2px solid black">Microscopy \t\t\t\t\t\t\n \t\t\t\t</th><th class="td" title="table-head " align="left" valign="top" scope="col" style="border-bottom: 2px solid black">Immunohistochemistry \t\t\t\t\t\t\n \t\t\t\t</th></tr></thead><tbody title="tbody"><tr title="table-row"><td class="td" title="table-entry " align="left" valign="top"><span class="elsevierStyleBold">Olfactory neuroblastoma</span><span class="elsevierStyleHsp" style=""></span>Origin from olfactory membrane \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• Uniform small round cells with indistinct borders, arranged in nests and sheets having sparse cytoplasm, round nuclei, dispersed (“salt and pepper”) coarse to fine nuclear chromatin with inconspicuous nucleoli against the background of neurofibrillary material• Higher-grade tumors with nuclear pleomorphism, prominent nucleoli, increased mitotic activity (necrosis may be present)• Rosettes of the Homer Wright type (pseudorosettes) in up to 30% of tumors, and Flexner–Wintersteiner type (true neural rosettes) in 5% \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• <span class="elsevierStyleBold">Positive markers:</span><span class="elsevierStyleHsp" style=""></span>- Neuron specific enolase (NSE) (the most consistently expressed marker)<span class="elsevierStyleHsp" style=""></span>- Synaptophysin, neurofilament protein (NFP), class III beta-tubulin, and microtubule-associated protein (majority of cases)<span class="elsevierStyleHsp" style=""></span>- S-100 protein staining limited to the sustentacular cells situated along the periphery of the neoplastic lobules (may be sparse in the higher-grade tumors)<span class="elsevierStyleHsp" style=""></span>- Immunoreactivity for chromogranin, glial fibrillary acidic protein (GFAP), and Leu-7 may be present• <span class="elsevierStyleBold">Negative markers:</span><span class="elsevierStyleHsp" style=""></span>- Cytokeratin (some positive cells in some cases)<span class="elsevierStyleHsp" style=""></span>- Epithelial markers: epithelial membrane antigen (EMA) and carcinoembryonic antigen (CEA)<span class="elsevierStyleHsp" style=""></span>- Leukocyte common antigen (LCA), HMB-45, desmin and CD99• <span class="elsevierStyleBold">Proliferation marker studies</span> using Ki-67 and MIB-1 have shown a high proliferative index of 10%–50%• <span class="elsevierStyleBold">Flow cytometric analysis</span> shows frequent polyploidy/aneuploidy \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="left" valign="top"><span class="elsevierStyleBold">Undifferentiated carcinoma</span> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• Medium-sized to polygonal tumor cells, with large ovoid nuclei with prominent nucleoli and distinct cytoplasmic borders with individual and comedo type of necrosis \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">- <span class="elsevierStyleBold">Positive markers:</span> cytokeratin- <span class="elsevierStyleBold">Negative markers:</span> HMB45• Absence of melanin pigmentation \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="left" valign="top"><span class="elsevierStyleBold">Embryonal rhabdomyosarcoma</span> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• Small round cells with small nucleoli in the subepithelial layer (cambium layer) with presence of rhabdomyoblasts (strap cells) \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• <span class="elsevierStyleBold">Positive markers:</span> Myo D1 \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="left" valign="top"><span class="elsevierStyleBold">Lymphomas (lymphoblastic type)</span> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• Neoplastics cells with a single prominent nucleoli \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• <span class="elsevierStyleBold">Negative markers:</span> CD45 \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="left" valign="top"><span class="elsevierStyleBold">Mesenchymal chondrosarcoma Small cell osteosarcoma</span> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• Presence of either cartilage or osteoid tissue \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• <span class="elsevierStyleBold">Positive markers:</span> FLI1 \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="left" valign="top"><span class="elsevierStyleBold">Mucosal malignant melanoma</span> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• Epithelioid, spindled, plasmacytoid, rhabdoid, and/or multinucleated tumor cells• Medium to large-sized cells with a high nuclear to cytoplasmic ratio and pleomorphic nuclei containing prominent eosinophilic nucleoli and intranuclear cytoplasmic inclusions• Cytoplasm densely eosinophilic, with variably melanin pigment• Mitoses frequent and easily identifiable• Tumors usually invade the subepithelial tissue and frequently extend into the bone, cartilage or skeletal muscle \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">• <span class="elsevierStyleBold">Positive markers:</span><span class="elsevierStyleHsp" style=""></span>- S100 protein and vimentin<span class="elsevierStyleHsp" style=""></span>- HMB45, tyrosinase, melan-A and microphthalmia transcription factor (variably expressed)<span class="elsevierStyleHsp" style=""></span>- NSE, CD117, CD99, synaptophysin, CD56, and CD57 occasionally positive• <span class="elsevierStyleBold">Negative markers:</span><span class="elsevierStyleHsp" style=""></span>- EMA, cytokeratins, and musce markers \t\t\t\t\t\t\n \t\t\t\t</td></tr></tbody></table> """ ] "imagenFichero" => array:1 [ 0 => "xTab845283.png" ] ] ] ] "descripcion" => array:1 [ "en" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall">Microscopic and Immunohistochemistry Characteristics of Small Round Cell Tumors.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:6 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Ewing's sarcoma of the ethmoid sinus" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "M. Aferzon" 1 => "W.E. Wood" 2 => "J.R. Powell" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Otolaryngol Head Neck Surg" "fecha" => "2003" "volumen" => "128" "paginaInicial" => "897" "paginaFinal" => "901" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/12825045" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Rare case of extraskeletal Ewings sarcoma of the sinonasal tract" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:1 [ 0 => "S.K. Yeshvanth" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.4103/0973-1482.95197" "Revista" => array:6 [ "tituloSerie" => "J Cancer Res Ther" "fecha" => "2012" "volumen" => "8" "paginaInicial" => "142" "paginaFinal" => "144" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/22531536" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "A sinonasal primary Ewing's sarcoma" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "K.L. Howarth" 1 => "I. Khodaei" 2 => "A. Karkanevatos" 3 => "R.W. Clarke" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:7 [ "tituloSerie" => "Int J Pediatr Otorhinolaryngol" "fecha" => "2004" "volumen" => "68" "paginaInicial" => "221" "paginaFinal" => "224" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/14725990" "web" => "Medline" ] ] "itemHostRev" => array:3 [ "pii" => "S0016508508004290" "estado" => "S300" "issn" => "00165085" ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Ewing's sarcoma in the nasal cavity" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "L.V. Csokonai" 1 => "B. Liktor" 2 => "G. Arató" 3 => "F. Helffrich" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1067/mhn.2001.119486" "Revista" => array:6 [ "tituloSerie" => "Otolaryngol Head Neck Surg" "fecha" => "2001" "volumen" => "125" "paginaInicial" => "665" "paginaFinal" => "667" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/11743477" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Sarcome d’Ewing et localisations ORL: A propos d’un cas" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "B. Velche-Haag" 1 => "D. Dehesdin" 2 => "F. Proust" 3 => "J.P. Marie" 4 => "J. Andrieu-Guitrancourt" 5 => "A. Laquerriere" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Ann Olaryngol Chir Cervicofac" "fecha" => "2002" "volumen" => "119" "paginaInicial" => "363" "paginaFinal" => "368" ] ] ] ] ] ] 5 => array:3 [ "identificador" => "bib0030" "etiqueta" => "6" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Extraskeletal Ewing's sarcoma of the nose" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:5 [ 0 => "A. Böör" 1 => "I. Jurkovic" 2 => "I. Friedmann" 3 => "L. Plank" 4 => "P. Kocan" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "J Laryngol Otol" "fecha" => "2001" "volumen" => "115" "paginaInicial" => "74" "paginaFinal" => "76" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/11233634" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/21735735/0000006600000003/v1_201506160927/S2173573514000167/v1_201506160927/en/main.assets" "Apartado" => array:4 [ "identificador" => "5881" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Case Studies" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/21735735/0000006600000003/v1_201506160927/S2173573514000167/v1_201506160927/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573514000167?idApp=UINPBA00004N" ]
Journal Information
Vol. 66. Issue 3.
Pages 171-174 (May - June 2015)
Share
Download PDF
More article options
Vol. 66. Issue 3.
Pages 171-174 (May - June 2015)
Case Study
Ewing's Sarcoma: A Rarity in Sinonasal Region
Sarcoma de Ewing: una rareza en la región nasosinusal
Visits
2848
This item has received
Article information
These are the options to access the full texts of the publication Acta Otorrinolaringológica Española
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail