Malignant pheochromocytomas represent between 5% and 26% of all diagnosed pheochromocytomas.1 Treatment of these tumors should be multidisciplinary and based on surgery since aggressive surgical treatment provides the only possibility for long-term cure in these patients. In addition, surgery improves the effectiveness of other treatments such as 131I-MIBG.
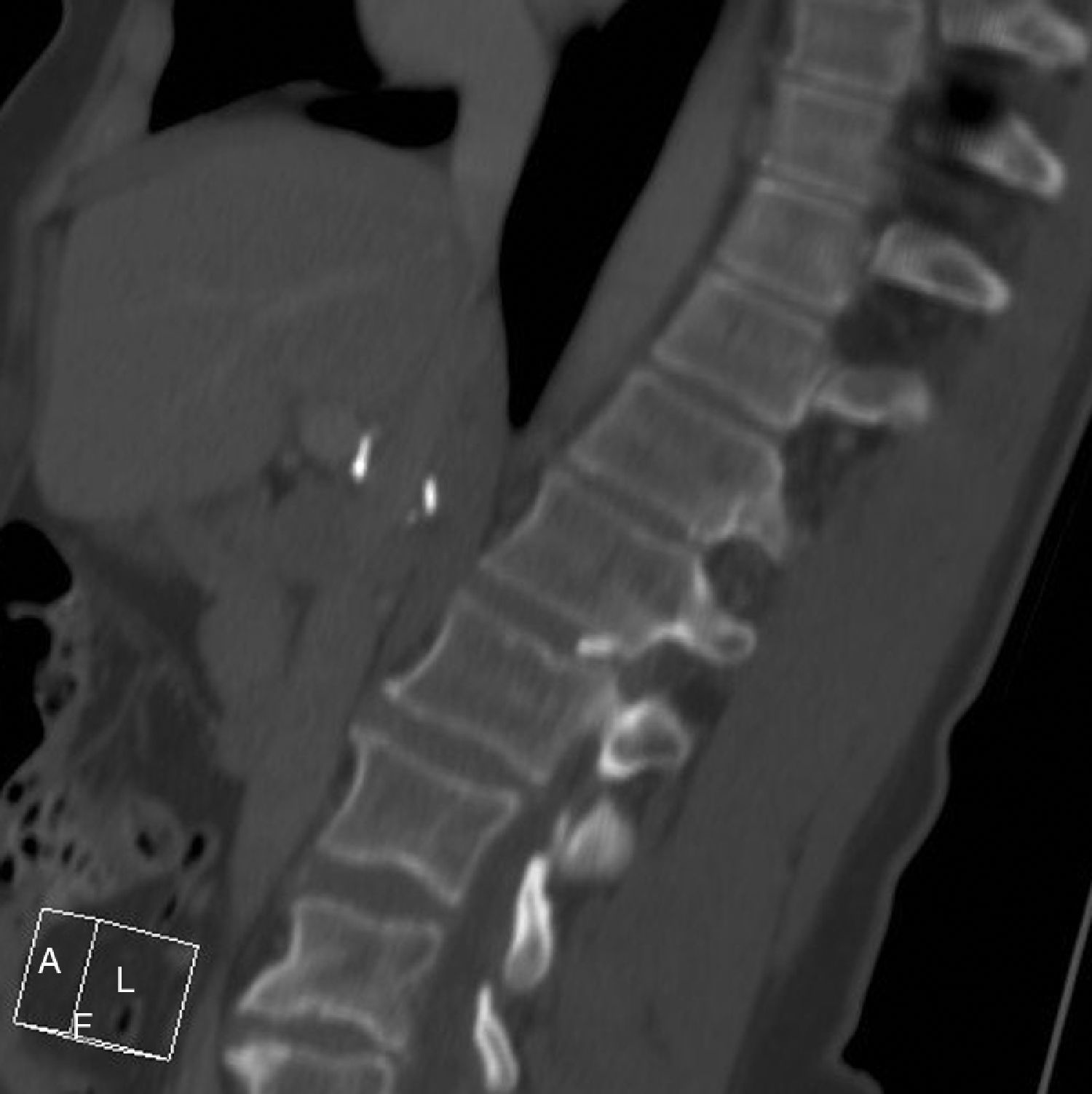
We report the case of a 53-year-old woman who was referred to our center to assess the surgical resection of a recurrent malignant pheochromocytoma. The patient had undergone open right adrenalectomy 12 years earlier due to pheochromocytoma. We had little information about this previous intervention; we only knew that it was a complex procedure and that the patient had been monitored with follow-up analyses and CT for 6 years, with no evidence of recurrence. The patient had undergone a CT scan for suspected diverticulitis, which revealed a mass measuring 5cm×12cm in the old surgical bed. This mass infiltrated segments 6 and 7 of the liver, the right kidney, and surrounded the retrohepatic vena cava (Fig. 1). In addition, there were pathologic lymphadenopathies in the hepatic hilum. As the only symptom, the patient reported headaches and self-limiting episodes of palpitations. Urine analysis of normetanephrine and metanephrine showed much higher levels than normal (metanephrineu/creatinineu ratio 16607 [0.1–260] and normetanephrineu/creatinineu 22793 [0.1–560]). Chromogranin A levels were also elevated (110ng/ml). The study of PTH, thyroid hormones, DHEAS and calcitonin was normal. Complementary studies included a SPECT-CT with 131I-MIBG, octreotide scan and FNA, which suggested pheochromocytoma recurrence without distant metastasis. After completing the studies, the patient was referred to our center.
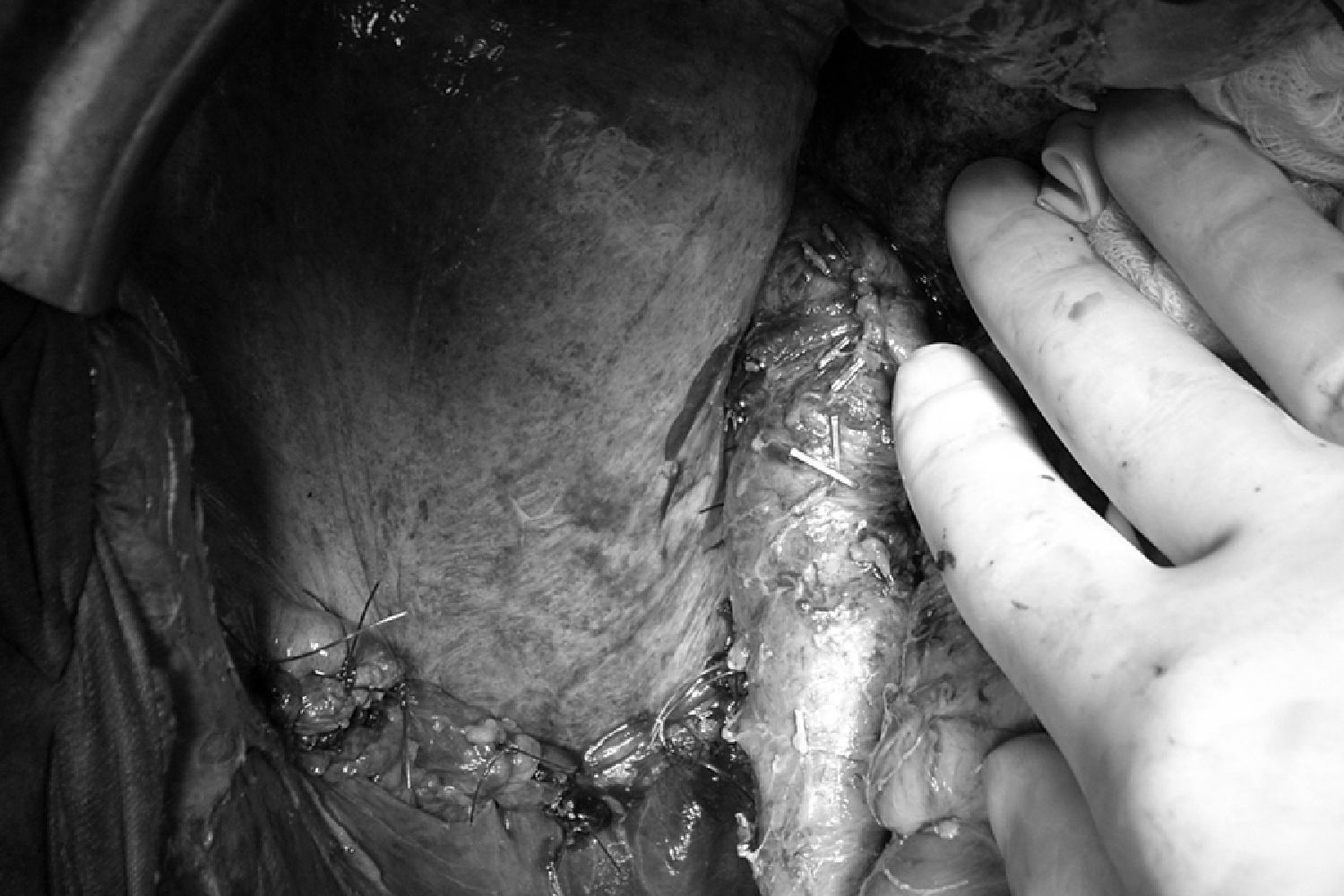
The patient was treated preoperatively with volume expansion and doxazosin. However, during surgery the patient presented hemodynamic lability with episodes of hypo- and hypertension. During surgery, resection of the mass was accompanied by right hepatectomy, right nephrectomy, partial resection of the diaphragm and lymphadenectomy of the inter-aorto-caval, retropancreatic and hepatic hilar regions (Fig. 2). Histopathology confirmed hepatic, lymph node and peritoneal pheochromocytoma metastases. The patient presented an uneventful recovery. The headache and palpitation episodes improved and there were no changes in blood pressure, which was normal before surgery.
The patient has currently been monitored for 21 months, with no relapse of the disease.
One of the biggest challenges when treating a patient with pheochromocytoma is the inability to pathologically differentiate benign from malignant tumors. However, there are a number of clinical parameters (age at diagnosis, tumors larger than 5cm, weight greater than 250g, multifocal, bilateral or extradrenal tumors and early postoperative AHT2), analytical parameters (marked elevation of chromogranin A3 in plasma or dopamine4 or metanephrine2 in plasma or urine, the expression of VEGF, COX-2 and MVD2 genes, and the existence of a mutation in the SDHB gene5) and pathological parameters (e.g. the PASS index designed by Thompson6) that have demonstrated their association with increased risk for malignancy. In the case we have presented, we have no information about the first intervention, but from the description of the patient we assume that it was a large tumor attached to the liver.
The treatment of malignant pheochromocytomas depends on the extension of the disease. Whenever possible, surgical resection should be attempted as it is the only treatment that provides long-term survival.7 There are published cases of multiorgan resections, such as the one performed in our patient.8 In fact, there have been reports of cases of resected pheochromocytomas with involvement of the inferior vena cava and the right atrium.9 Unfortunately, the cases published are isolated reports and there are no large series of patients with malignant pheochromocytomas who have required multivisceral resections. Furthermore, most of these publications simply describe the surgery performed without providing information about the mid- and long-term follow-up,8 so recurrence rates and overall survival of these patients is unknown. However, prolonged survival in some of these cases justifies conducting aggressive interventions, provided limited morbidity can be ensured.
Surgery should be performed, even if the resection cannot be completed, because reduction of the tumor mass facilitates the action of other therapies such as 131I-MIBG by allowing the radiopharmaceutical to become concentrated in the non-resected tumor remains.7
For patients with unresectable tumors or incomplete resection, 131I-MIBG or 90Y-DOTA-octreotide can be used, which obtain complete or partial responses in 30%–40% of patients.10 Chemotherapy may be useful; the most commonly used regime is a combination of cyclophosphamide, vincristine and dacarbazine, which has demonstrated partial remission or clinical improvement in 50% of patients.10 Other therapeutic options such as tyrosine kinase inhibitors or VEGF inhibitors have also been effective in selected patients.10
Please cite this article as: Cano-Valderrama O, Díez-Valladares L, Pérez-Aguirre E, García-Botella A, Torres García AJ. Hepatectomía derecha asociada a nefrectomía y resección de diafragma como tratamiento de un feocromocitoma maligno recidivado 12 años después de ser intervenido. Cir Esp. 2013;91:613–614.