Journal Information
Vol. 47. Issue 4.
Pages 387-388 (April 2024)
Vol. 47. Issue 4.
Pages 387-388 (April 2024)
Image of the month
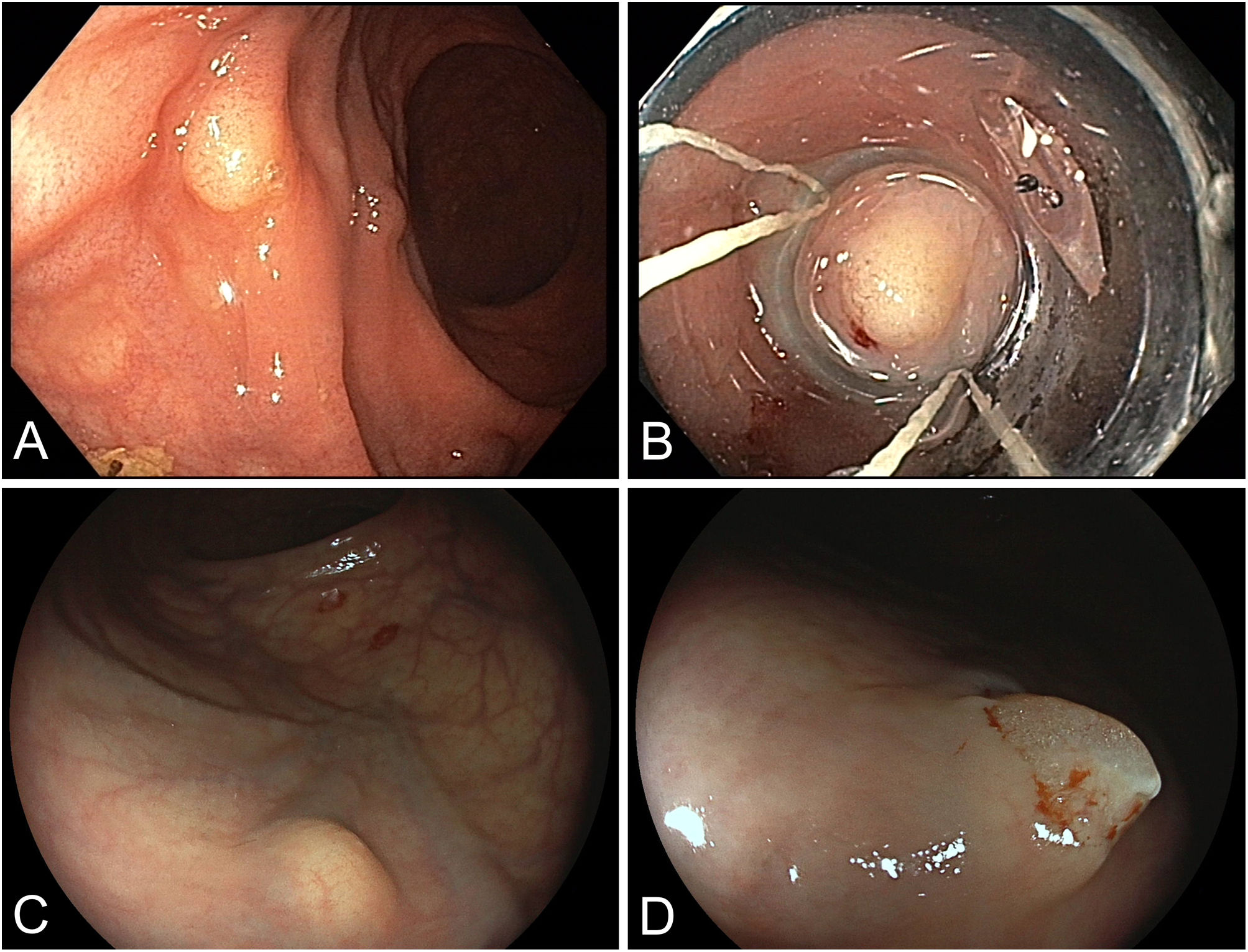
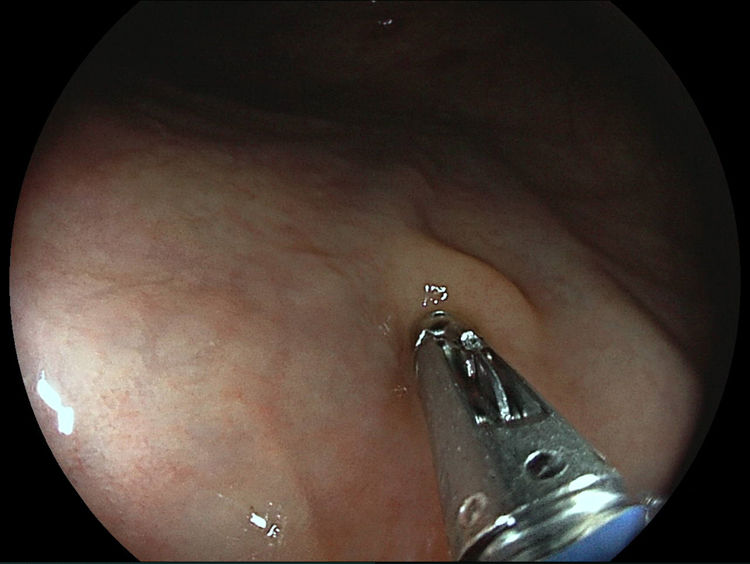
What shall we do with yellowish rectal lesions during screening colonoscopy?
¿Qué haremos con las lesiones rectales amarillentas durante colonoscopia de detección?
Article information
These are the options to access the full texts of the publication Gastroenterología y Hepatología (English Edition)
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail