We have read the original article entitled “Radiography-based triage for COVID-19 in the Emergency Department in a Spanish cohort of patients”1 by Sempere-González A, et al.1 We want to congratulate the authors for this article and make some contributions.
The use of a test with low sensitivity to classify potentially infectious patients is stand out. Chest computed tomography (CT) has been suggested as an additional tool for the initial assessment of potentially infected patients, reporting an even higher sensitivity of up to 97%.2 However, its implementation is questionable, not only because of the logistical limitations that all Spanish emergency departments (ED) suffered in March 2020, with shortages of human resources, materials, and space,3 but also because of the radiation and the high costs involved in its implementation as a screening tool in mild patients.
Although it has been mentioned in their article, we would like to insist on the value of promoting the use of lung ultrasound in these patients. At high pandemic peaks, it is necessary not only to detect those who may worsen,4 but also to detect those who may become infectious, in order to insist on isolation measures. Implementation in early triage in the ED could be useful as it meets the priority objective of saving time in the diagnostic approach (chest scans of 7–10min may be enough) and avoiding the movement of potentially infectious patients. labeling the technique a useful screening test in patients with mild to moderate involvement.5
Compared with RT-PCR, lung ultrasound demonstrated outstanding sensitivity and NPV (93.3% and 92% respectively) while showing poor values for specificity and PPV, and accuracy (85.2% and 75.8% respectively).5 The most common findings a compatible lung ultrasound exam are considered a pattern of B-lines, isolated or confluent, irregular pleural lines, and/or subpleural consolidations. Most of them affecting posteroinferior and posterosuperior areas.5 Based on these data, the technique could be considered a useful screening test in patients with mild to moderate involvement. Furthermore, none of the imaging tests performed allow us to be sure of the etiology of the pulmonary involvement, so confirmation by molecular testing is necessary. In those patients in whom pulmonary ultrasound is affected, radiography or computed tomography can help to confirm and assess the severity and extent of pulmonary involvement.
In contrast, similar inquiries using chest CT as index test, excellent sensitivity, specificity, NPV, and accuracy (80.0%, 86.7%, 95.6%, and 85.6%, respectively) were reported, beside a moderate value for PPV (54.5%).2
Apart from no radiation exposure, ultrasound has numerous other advantages. Low cost, high availability, bedside testing, and time between exam and result are the other main benefits, but also low threshold for testing vulnerable patients (e.g., children, pregnant women) and the possibility of being able to disinfect quickly after use make it an outstanding screening tool.
At the peak of the pandemic, one of the objectives was to detect patients at the highest risk of complications, something that was described in the first weeks by research groups of emergency physicians. However, it was also necessary to adequately isolate those potentially infectious and avoid unnecessary transfers.
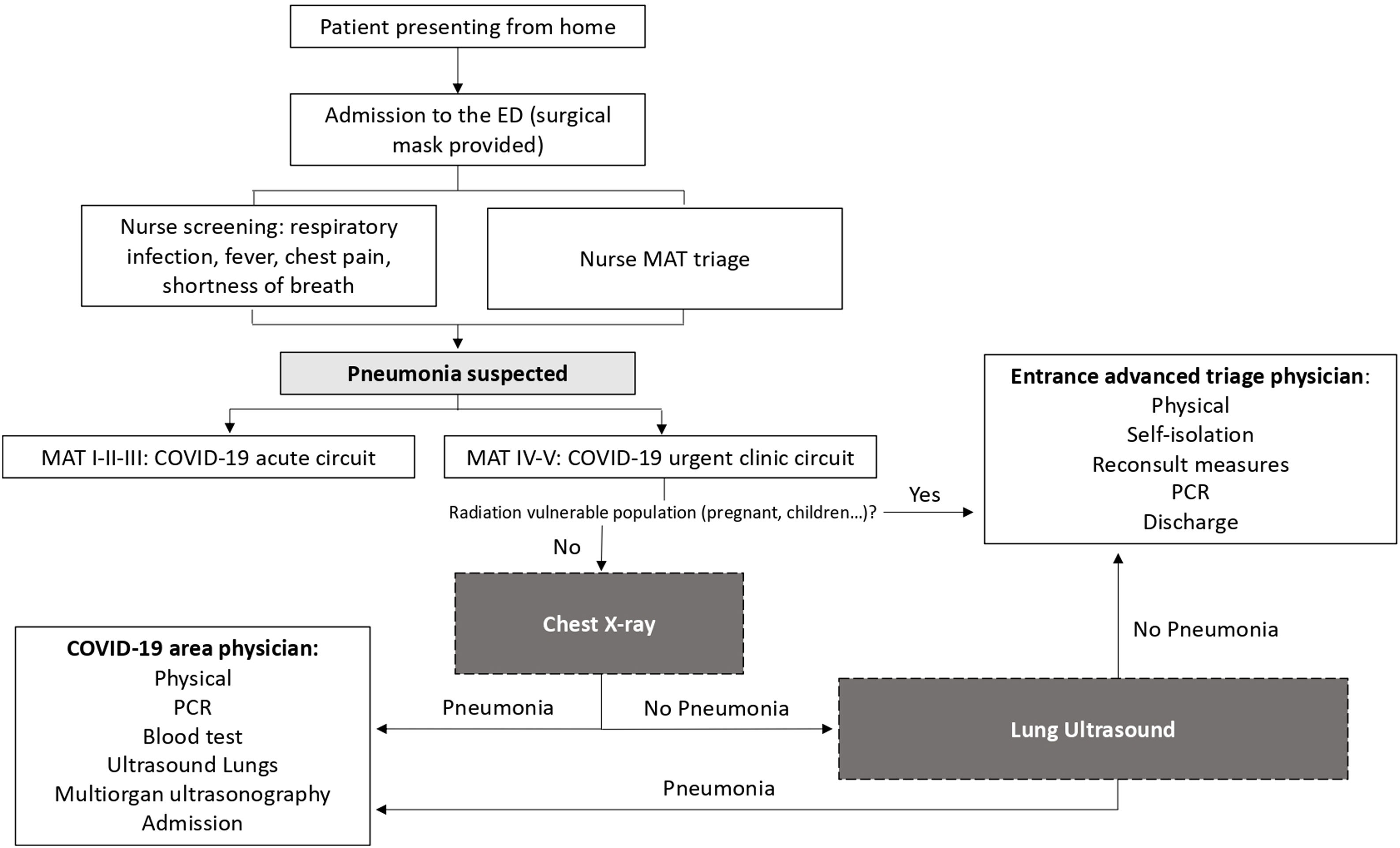
We propose an algorithm that integrates lung ultrasound as a screening tool to risk-stratify patients suspected pulmonary involvement of COVID-19 (Fig. 1).
We should not forget that there are other complications associated with COVID-19, which should be taken into account, such as pneumothorax or pulmonary thromboembolism. For these, ultrasound continues to have a very high sensitivity, above that of thoracic radiography. Therefore, although it is not the subject of this letter, the integration of several ultrasound windows in these patients is important for their early detection.
Thus, based on their results, by using lung ultrasound prior to other imaging tests, we are sure that the percentage of revisits to the emergency department due to worsening would have been reduced.
Author's contributionsAll authors read and approved the final manuscript. All authors have contributed to this work.
Ethical responsibilitiesNo patient data appear in the article, so written informed consent haven’t been obtained. All authors have confirmed the maintenance of confidentiality and respect for patients’ rights in the document of author responsibilities, publication agreement and assignment of rights to MEDICINA CLÍNICA.
FundingThis work has not been supported by public grants or financial support. No sources of funding were used to assist in the preparation of this study. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflict of interestThe authors declare that they have no conflict of interest in relation to this article.