Article

Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)
array:23 [ "pii" => "S2253808917302100" "issn" => "22538089" "doi" => "10.1016/j.remnie.2017.12.006" "estado" => "S300" "fechaPublicacion" => "2018-11-01" "aid" => "960" "copyrightAnyo" => "2017" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2018;37:384-6" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 8 "formatos" => array:2 [ "HTML" => 6 "PDF" => 2 ] ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S2253654X18300751" "issn" => "2253654X" "doi" => "10.1016/j.remn.2018.04.002" "estado" => "S300" "fechaPublicacion" => "2018-11-01" "aid" => "988" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Rev Esp Med Nucl Imagen Mol. 2018;37:380-1" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 58 "formatos" => array:2 [ "HTML" => 34 "PDF" => 24 ] ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Carta al Director</span>" "titulo" => "Pruebas de pureza radioquímica de radiofármacos marcados con <span class="elsevierStyleSup">99m</span>Tc: nada, excepto todo, es suficiente" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "380" "paginaFinal" => "381" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Radiochemical purity testing of <span class="elsevierStyleSup">99m</span>Tc-labelled radiopharmaceuticals: Nothing, except everything, is enough" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figura 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1147 "Ancho" => 1451 "Tamanyo" => 121600 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Probabilidad de detectar todos y cada uno de los productos defectuosos frente al porcentaje de preparaciones estudiadas para uno, 2 o 3 productos defectuosos.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "J.L. Gómez Perales, M.T. Gutiérrez Amares" "autores" => array:2 [ 0 => array:2 [ "nombre" => "J.L." "apellidos" => "Gómez Perales" ] 1 => array:2 [ "nombre" => "M.T." "apellidos" => "Gutiérrez Amares" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S225380891830034X" "doi" => "10.1016/j.remnie.2018.05.001" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S225380891830034X?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X18300751?idApp=UINPBA00004N" "url" => "/2253654X/0000003700000006/v3_201812190642/S2253654X18300751/v3_201812190642/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2253808917301258" "issn" => "22538089" "doi" => "10.1016/j.remnie.2017.10.010" "estado" => "S300" "fechaPublicacion" => "2018-11-01" "aid" => "937" "copyright" => "Elsevier España, S.L.U. and SEMNIM" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2018;37:387-9" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 4 "formatos" => array:2 [ "HTML" => 2 "PDF" => 2 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Staging and follow-up of a Ewing sarcoma patient using <span class="elsevierStyleSup">18</span>F-FDG PET/CT" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "387" "paginaFinal" => "389" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Estadificación y seguimiento terapéutico en un paciente con sarcoma de Ewing mediante PET/TC con <span class="elsevierStyleSup">18</span>F-FDG" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 1868 "Ancho" => 2498 "Tamanyo" => 219674 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Sagittal images of the CT component of the <span class="elsevierStyleSup">18</span>F-FDG PET/CT studies performed. Lytic involvement in bone, especially in L1, was shown in follow-up study 10 months after diagnosis (D), with transition to partial bone sclerosis at the 16-months study (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>F), and with variable outcome afterwards.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "J.R. Garcia, A. Castañeda, A. Morales, P. Bassa, M. Soler, E. Riera" "autores" => array:6 [ 0 => array:2 [ "nombre" => "J.R." "apellidos" => "Garcia" ] 1 => array:2 [ "nombre" => "A." "apellidos" => "Castañeda" ] 2 => array:2 [ "nombre" => "A." "apellidos" => "Morales" ] 3 => array:2 [ "nombre" => "P." "apellidos" => "Bassa" ] 4 => array:2 [ "nombre" => "M." "apellidos" => "Soler" ] 5 => array:2 [ "nombre" => "E." "apellidos" => "Riera" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S2253654X17301336" "doi" => "10.1016/j.remn.2017.09.001" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X17301336?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808917301258?idApp=UINPBA00004N" "url" => "/22538089/0000003700000006/v3_201812190625/S2253808917301258/v3_201812190625/en/main.assets" ] "itemAnterior" => array:18 [ "pii" => "S2253808918300089" "issn" => "22538089" "doi" => "10.1016/j.remnie.2018.02.005" "estado" => "S300" "fechaPublicacion" => "2018-11-01" "aid" => "972" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2018;37:382-3" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 3 "PDF" => 3 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting image</span>" "titulo" => "Usefulness of <span class="elsevierStyleSup">99m</span>Tc labelled heat-denatured red blood cell scintigraphy in the diagnosis of intramuscular splenosis" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "382" "paginaFinal" => "383" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Utilidad de la gammagrafía con hematíes desnaturalizados por calor marcados con <span class="elsevierStyleSup">99m</span>Tc en el diagnóstico de una esplenosis intramuscular" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1057 "Ancho" => 950 "Tamanyo" => 30703 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Planar images in anterior projection showed a large intense and irregular radiotracer uptake between mesogastrium and left flank (arrow), and another small adjacent focus (arrow head) with lower uptake and lateral to the larger lesion.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "E. Noriega, J. Suils, M.T. Bajén, A. Benítez, J. Rodríguez-Rubio, J. Mora Salvadó" "autores" => array:6 [ 0 => array:2 [ "nombre" => "E." "apellidos" => "Noriega" ] 1 => array:2 [ "nombre" => "J." "apellidos" => "Suils" ] 2 => array:2 [ "nombre" => "M.T." "apellidos" => "Bajén" ] 3 => array:2 [ "nombre" => "A." "apellidos" => "Benítez" ] 4 => array:2 [ "nombre" => "J." "apellidos" => "Rodríguez-Rubio" ] 5 => array:2 [ "nombre" => "J." "apellidos" => "Mora Salvadó" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S2253654X17303165" "doi" => "10.1016/j.remn.2018.01.006" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X17303165?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808918300089?idApp=UINPBA00004N" "url" => "/22538089/0000003700000006/v3_201812190625/S2253808918300089/v3_201812190625/en/main.assets" ] "en" => array:15 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting image</span>" "titulo" => "Ethmoidal and extranodal Burkitt lymphoma in a child with bilateral kidney Burkitt lymphoma lesions incidentally detected by <span class="elsevierStyleSup">18</span>F-FDG PET/CT" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "384" "paginaFinal" => "386" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Mattia Bonacina, Mattia Bertoli, Domenico Albano, Francesco Bertagna, Francesco Laffranchi, Raffaele Giubbini" "autores" => array:6 [ 0 => array:4 [ "nombre" => "Mattia" "apellidos" => "Bonacina" "email" => array:1 [ 0 => "mattia.bonacina@gmail.com" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Mattia" "apellidos" => "Bertoli" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 2 => array:3 [ "nombre" => "Domenico" "apellidos" => "Albano" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 3 => array:3 [ "nombre" => "Francesco" "apellidos" => "Bertagna" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 4 => array:3 [ "nombre" => "Francesco" "apellidos" => "Laffranchi" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">c</span>" "identificador" => "aff0015" ] ] ] 5 => array:3 [ "nombre" => "Raffaele" "apellidos" => "Giubbini" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] ] "afiliaciones" => array:3 [ 0 => array:3 [ "entidad" => "Nuclear Medicine, Spedali Civili Brescia, Brescia, Italy" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Nuclear Medicine, University of Brescia and Spedali Civili Brescia, Brescia, Italy" "etiqueta" => "b" "identificador" => "aff0010" ] 2 => array:3 [ "entidad" => "Pediatric Radiology, Spedali Civili Brescia, Brescia, Italy" "etiqueta" => "c" "identificador" => "aff0015" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Linfoma de Burkitt etmoidal y extranodal en un niño con lesiones renales bilaterales de linfoma de Burkitt detectadas por <span class="elsevierStyleSup">18</span>F-FDG PET/TC" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 2841 "Ancho" => 2083 "Tamanyo" => 299044 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Maximum intensity projection (MIP) showing increased FDG uptake suggestive of malignant lesions in the ethmoidal sinus, bilateral cervical lymphadenopathies, several bone lesions and cortical lesions in both kidneys (A). Axial non-contrast enhanced CT with no pathological findings (B), axial PET/CT fused images (C) and axial PET (D) before treatment showing anomalous FDG distribution within the renal cortex, with focal increased uptake in the cortex of the right kidney (in this axial slice) corresponding to lesions visible on MRI (F); concordance between the PET and MR lesions were confirmed in PET/MR fusion images (E).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">In a 3-years-old child with nasal obstruction, Burkitt lymphoma (BL) was diagnosed through ethmoidal lesion biopsy; the patient underwent a staging 18 fluorine-fluorodesoxyglucose positron emission tomography/computed tomography (<span class="elsevierStyleSup">18</span>F-FDG PET/CT) before treatment. PET/CT images were acquired 60<span class="elsevierStyleHsp" style=""></span>min after the intravenous injection of 3.5<span class="elsevierStyleHsp" style=""></span>MBq/kg of <span class="elsevierStyleSup">18</span>F-FDG on a Discovery 690 tomograph (GE; Milwaukee, Wis; 64-slice CT, 80<span class="elsevierStyleHsp" style=""></span>mA, 120<span class="elsevierStyleHsp" style=""></span>kV; 2.5<span class="elsevierStyleHsp" style=""></span>min/bed; 256 matrix, 60-cm field of view). <span class="elsevierStyleSup">18</span>F-FDG PET/CT showed FDG increased uptakes in the lesion localized in the ethmoidal sinus, in bilateral laterocervical nodes, in multiple bone localizations and in both kidneys (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>A–D). These renal uptakes were not due to calyx and pelvis urinary outflow and were not correlated with anatomic CT alterations. Subsequently, the patient underwent an abdominal magnetic resonance imaging (MRI) scan. MRI images were performed with a Siemens Magnetom Symphony 1.5<span class="elsevierStyleHsp" style=""></span>T (Erlangen, Germany) with the following protocol: axial T1 sequences (in-out phase), T2 Haste with respiratory trigger acquired on the three planes of the space, axial T2 space spair, diffusion sequences (with <span class="elsevierStyleItalic">b</span> values 0, 50, 400, 800 and apparent diffusion coefficient (ADC) map b0_800), axial VIBE sequences before and after intravenous contrast administration (acquisition made untill 3<span class="elsevierStyleHsp" style=""></span>min after administration). MRI images showed an abnormal renal cortical profile in all sequences acquired and renal cortical lesions could be clearly detected in D b_800 sequences and in ADC map images (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>E and F); these lesions were steadily hypo intense with peripheral ring enhancement in early post-contrast images while they were not detectable in the non-enhanced sequences. Fusion images of PET and MRI clearly confirmed the overlap between the cortical lesions and the <span class="elsevierStyleSup">18</span>F-FDG uptakes. Studies performed with <span class="elsevierStyleSup">18</span>F-FDG PET/CT and MRI after finalising the chemotherapy treatment showed a complete remission of the lesions (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>).</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><elsevierMultimedia ident="fig0010"></elsevierMultimedia><p id="par0010" class="elsevierStylePara elsevierViewall">Burkitt lymphoma (BL) is a B-cell derivated neoplasm which is a consequence of a genetic translocation that involves the loci of c-Myc and immunoglobulines (translocation 8;14). It is strictly related to the Epstein–Barr virus infection and its presentation can be sporadic, endemic or immunodeficiency-associated. The sporadic form of BL can involve both nodal and extranodal sites. Extranodal involvement often includes the gastrointestinal tract, the ovaries, the breast and the central nervous system. PET/CT is routinely performed in staging and in assessing response to therapy in Burkitt lymphoma<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">1</span></a> although the renal localization of BL is an exceptional finding and only a few cases have been reported in the literature,<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">2</span></a> although none of them includes PET/CT imaging in the case report. Even if the detection of renal lesions with FDG PET/CT is relatively limited due to the urinary excretion of FDG it has been proven to be an accurate diagnostic tool.<a class="elsevierStyleCrossRef" href="#bib0030"><span class="elsevierStyleSup">3</span></a></p><p id="par0015" class="elsevierStylePara elsevierViewall">In conclusion, in our case, <span class="elsevierStyleSup">18</span>F-FDG PET/CT has proven to be useful in detecting a unique case of previously unknown kidney localization of BL lesions in a paediatric patient with BL.</p><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Conflict of interest</span><p id="par0020" class="elsevierStylePara elsevierViewall">The authors have no conflicts of interest to declare.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:2 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Conflict of interest" ] 1 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Bonacina M, Bertoli M, Albano D, Bertagna F, Laffranchi F, Giubbini R. Linfoma de Burkitt etmoidal y extranodal en un niño con lesiones renales bilaterales de linfoma de Burkitt detectadas por <span class="elsevierStyleSup">18</span>F-FDG PET/CT. Rev Esp Med Nucl Imagen Mol. 2018;37:384–386.</p>" ] ] "multimedia" => array:2 [ 0 => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 2841 "Ancho" => 2083 "Tamanyo" => 299044 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Maximum intensity projection (MIP) showing increased FDG uptake suggestive of malignant lesions in the ethmoidal sinus, bilateral cervical lymphadenopathies, several bone lesions and cortical lesions in both kidneys (A). Axial non-contrast enhanced CT with no pathological findings (B), axial PET/CT fused images (C) and axial PET (D) before treatment showing anomalous FDG distribution within the renal cortex, with focal increased uptake in the cortex of the right kidney (in this axial slice) corresponding to lesions visible on MRI (F); concordance between the PET and MR lesions were confirmed in PET/MR fusion images (E).</p>" ] ] 1 => array:7 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 2637 "Ancho" => 2083 "Tamanyo" => 236832 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Axial CT (A), axial PET/CT fused images (B), axial PET (C), axial PET/MRI fusion images (D), axial MRI images (E) and MIP (F) after the end of the chemotherapy treatment showing complete metabolic and morphological remission.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0015" "bibliografiaReferencia" => array:3 [ 0 => array:3 [ "identificador" => "bib0020" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Burkitt lymphoma: staging and response evaluation" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "J.T. Sandlund" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1111/j.1365-2141.2012.09026.x" "Revista" => array:6 [ "tituloSerie" => "Br J Haematol" "fecha" => "2012" "volumen" => "156" "paginaInicial" => "761" "paginaFinal" => "765" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/22296338" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0025" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "A child with Burkitt lymphoma with pleural, peritoneal, mesenteric omental, and renal involvement" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "X. Wang" 1 => "Z. Chen" 2 => "G. Tang" 3 => "X. Zhang" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1097/RLU.0b013e318217af84" "Revista" => array:6 [ "tituloSerie" => "Clin Nucl Med" "fecha" => "2001" "volumen" => "36" "paginaInicial" => "612" "paginaFinal" => "615" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/21637077" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0030" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Meta-analysis of the diagnostic performance of <span class="elsevierStyleSup">18</span>F-FDG PET in renal cell carcinoma" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "S.R. Martínez de Llano" 1 => "R.C. Delgado-Bolton" 2 => "A. Jiménez-Vicioso" 3 => "M.J. Pérez-Castejón" 4 => "J.L. Carreras Delgado" 5 => "E. Ramos" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Rev Esp Med Nucl Imagen Mol" "fecha" => "2007" "volumen" => "26" "paginaInicial" => "19" "paginaFinal" => "29" ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/22538089/0000003700000006/v3_201812190625/S2253808917302100/v3_201812190625/en/main.assets" "Apartado" => array:4 [ "identificador" => "7927" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Interesting images" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/22538089/0000003700000006/v3_201812190625/S2253808917302100/v3_201812190625/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808917302100?idApp=UINPBA00004N" ]
Consulte los artículos y contenidos publicados en éste medio, además de los e-sumarios de las revistas científicas en el mismo momento de publicación
Esté informado en todo momento gracias a las alertas y novedades
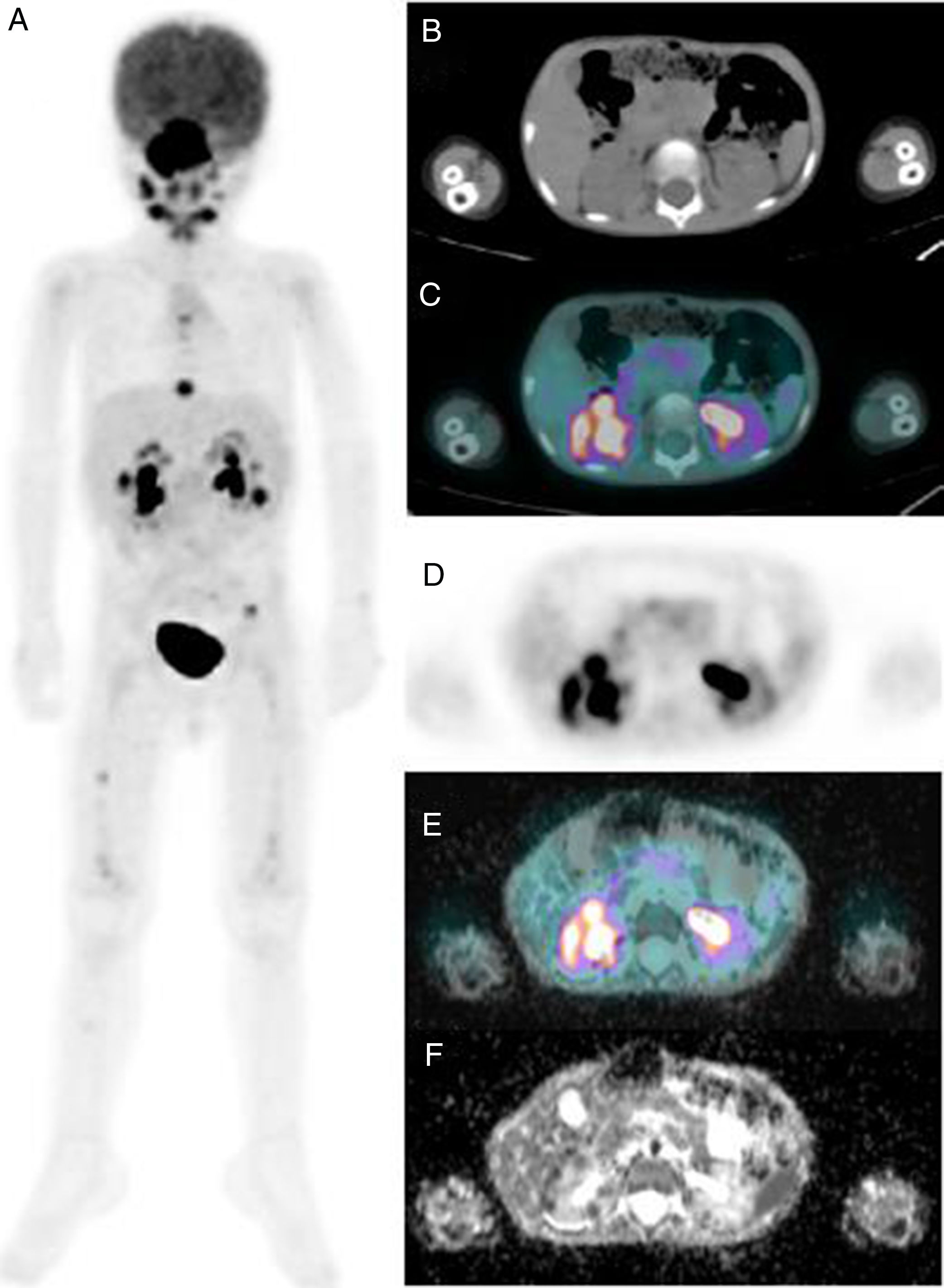
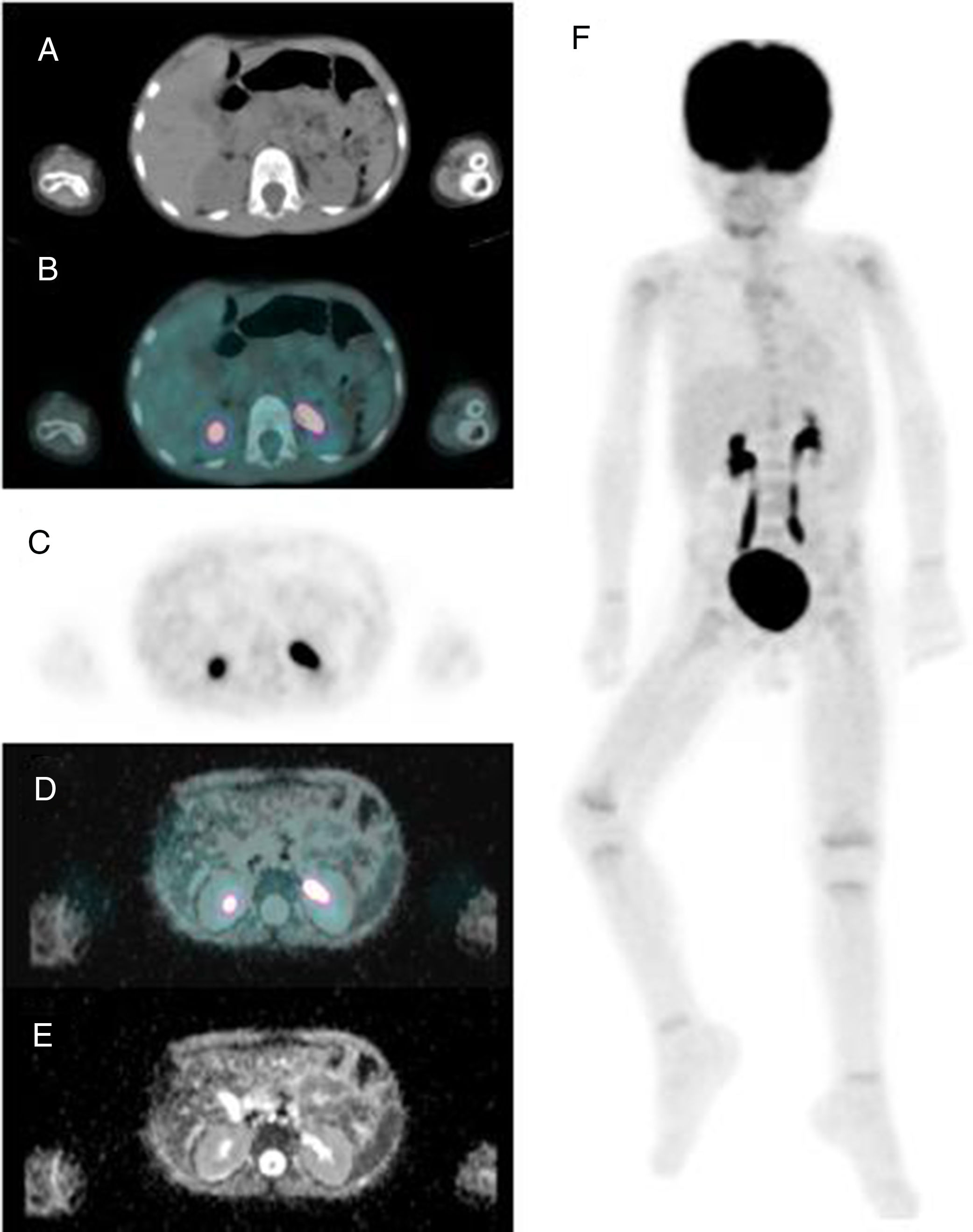
Acceda a promociones exclusivas en suscripciones, lanzamientos y cursos acreditados
The Revista Española de Medicina Nuclear e Imagen Molecular (Spanish Journal of Nuclear Medicine and Molecular Imaging), was founded in 1982, and is the official journal of the Spanish Society of Nuclear Medicine and Molecular Imaging, which has more than 700 members. The Journal, which publishes 6 regular issues per year, has the promotion of research and continuing education in all fields of Nuclear Medicine as its main aim. For this, its principal sections are Originals, Clinical Notes, Images of Interest, and Special Collaboration articles. The works may be submitted in Spanish or English and are subjected to a peer review process. In 2009, it became the leading Spanish journal in the field of Medical Imaging on having an Impact Factor , awarded by the Journal Citation Reports.
Science Citation Index Expander, Medline, IME, Bibliomed, EMBASE/Excerpta Medica, Healthstar, Cancerlit, Toxine, Inside Conferences, Scopus
See moreThe Impact Factor measures the average number of citations received in a particular year by papers published in the journal during the two preceding years.
© Clarivate Analytics, Journal Citation Reports 2022
SRJ is a prestige metric based on the idea that not all citations are the same. SJR uses a similar algorithm as the Google page rank; it provides a quantitative and qualitative measure of the journal's impact.
See moreSNIP measures contextual citation impact by wighting citations based on the total number of citations in a subject field.
See more
Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)

¿Es usted profesional sanitario apto para prescribir o dispensar medicamentos?
Are you a health professional able to prescribe or dispense drugs?
Você é um profissional de saúde habilitado a prescrever ou dispensar medicamentos