Artículo
Comprando el artículo el PDF del mismo podrá ser descargado
Precio 19,34 €
Comprar ahora
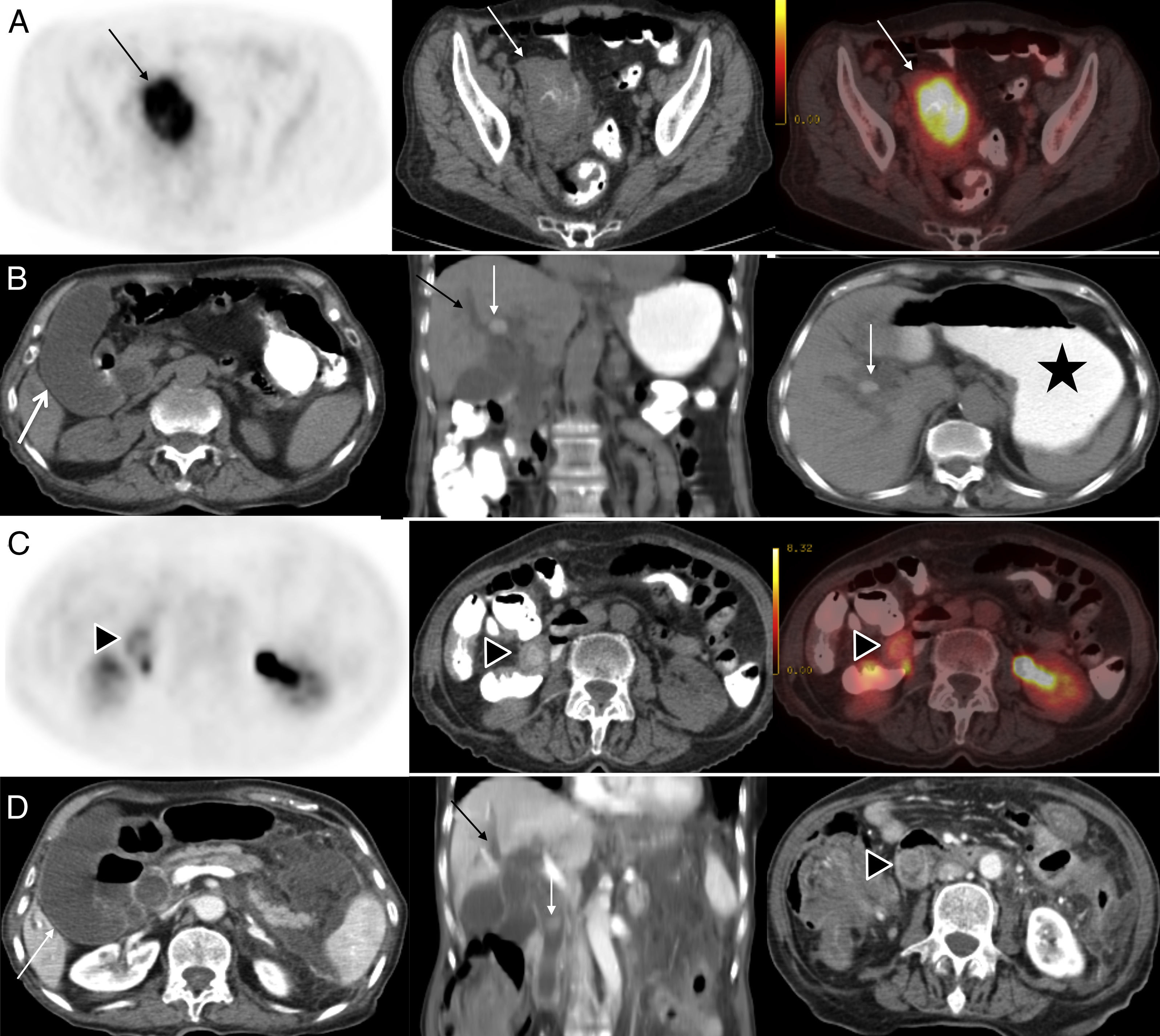
array:24 [ "pii" => "S2253654X13001546" "issn" => "2253654X" "doi" => "10.1016/j.remn.2013.08.004" "estado" => "S300" "fechaPublicacion" => "2014-03-01" "aid" => "537" "copyright" => "Elsevier España, S.L. and SEMNIM" "copyrightAnyo" => "2013" "documento" => "article" "crossmark" => 0 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2014;33:125-6" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 601 "formatos" => array:3 [ "EPUB" => 11 "HTML" => 387 "PDF" => 203 ] ] "Traduccion" => array:1 [ "en" => array:19 [ "pii" => "S2253808914000354" "issn" => "22538089" "doi" => "10.1016/j.remnie.2014.02.010" "estado" => "S300" "fechaPublicacion" => "2014-03-01" "aid" => "537" "copyright" => "Elsevier España, S.L. and SEMNIM" "documento" => "article" "crossmark" => 0 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2014;33:125-6" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 449 "formatos" => array:2 [ "HTML" => 310 "PDF" => 139 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting image</span>" "titulo" => "Bouveret's syndrome on FDG PET/CT: A rare life-threatening complication of gallstone disease" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "125" "paginaFinal" => "126" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "El síndrome de Bouveret en FDG PET/TC: Una complicación rara y potencialmente mortal de la enfermedad de cálculos biliares" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1341 "Ancho" => 1502 "Tamanyo" => 292024 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Besides hypermetabolic mass in the cecum (arrows in A: axial PET, CT and fusion PET/CT images, SUVmax<span class="elsevierStyleHsp" style=""></span>=<span class="elsevierStyleHsp" style=""></span>11.1) and neighbouring enlarged lymph nodes, initial staging PET/CT also showed dilated gallbladder (large white arrow in B: non-contrast enhanced CT of the PET/CT) and intra/extrahepatic biliary ducts (black arrow in B), gallstone in the gallbladder (small white arrows in B) and dilated stomach (star in B). When carefully examined, another gallstone with accompanying hypermetabolic wall thickening was seen in the lumen of the descending duodenum (arrow heads in C: axial PET, CT and fusion PET/CT images, SUVmax<span class="elsevierStyleHsp" style=""></span>=<span class="elsevierStyleHsp" style=""></span>4.7). The follow-up contrast enhanced CT scan of the abdomen also demonstrated dilated gallbladder (large white arrow in D) and biliary ducts (black arrow in D) and gallstones in the gallbladder (small white arrow in D) and in the lumen of the duodenum (arrow head in D).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Mustafa Aras, Sabahat Inanir, Davut Tuney" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Mustafa" "apellidos" => "Aras" ] 1 => array:2 [ "nombre" => "Sabahat" "apellidos" => "Inanir" ] 2 => array:2 [ "nombre" => "Davut" "apellidos" => "Tuney" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2253654X13001546" "doi" => "10.1016/j.remn.2013.08.004" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X13001546?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808914000354?idApp=UINPBA00004N" "url" => "/22538089/0000003300000002/v1_201403190010/S2253808914000354/v1_201403190010/en/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2253654X13001340" "issn" => "2253654X" "doi" => "10.1016/j.remn.2013.07.010" "estado" => "S300" "fechaPublicacion" => "2014-03-01" "aid" => "531" "copyright" => "Elsevier España, S.L. and SEMNIM" "documento" => "article" "crossmark" => 0 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2014;33:127-8" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 1058 "formatos" => array:3 [ "EPUB" => 8 "HTML" => 857 "PDF" => 193 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting image</span>" "titulo" => "Primary spinal leptomeningeal gliomatosis in a 3-year-old boy revealed with MRI and FDG PET/CT mimicking tuberculosis meningitis" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "127" "paginaFinal" => "128" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Gliomatosis leptomeníngea medular primaria en un niño de 3 años de edad, identificada por RM y FDG PET/TC imitando meningitis tuberculosa" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0015" "etiqueta" => "Fig. 3" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr3.jpeg" "Alto" => 662 "Ancho" => 1000 "Tamanyo" => 70994 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall">Anterior (A) and lateral (B) view of maximum intensity projection (MIP) images, and axial PET (C) and axial fusion (D) images did not demonstrate any primary tumor.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "E.B. Erdogan, S. Asa, S. Yilmaz Aksoy, M. Ozhan, A. Aliyev, M. Halac" "autores" => array:6 [ 0 => array:2 [ "nombre" => "E.B." "apellidos" => "Erdogan" ] 1 => array:2 [ "nombre" => "S." "apellidos" => "Asa" ] 2 => array:2 [ "nombre" => "S." "apellidos" => "Yilmaz Aksoy" ] 3 => array:2 [ "nombre" => "M." "apellidos" => "Ozhan" ] 4 => array:2 [ "nombre" => "A." "apellidos" => "Aliyev" ] 5 => array:2 [ "nombre" => "M." "apellidos" => "Halac" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2253808914000366" "doi" => "10.1016/j.remnie.2014.02.011" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808914000366?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X13001340?idApp=UINPBA00004N" "url" => "/2253654X/0000003300000002/v1_201403040016/S2253654X13001340/v1_201403040016/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2253654X13001285" "issn" => "2253654X" "doi" => "10.1016/j.remn.2013.08.001" "estado" => "S300" "fechaPublicacion" => "2014-03-01" "aid" => "525" "copyright" => "Elsevier España, S.L. and SEMNIM" "documento" => "article" "crossmark" => 0 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2014;33:122-4" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 664 "formatos" => array:3 [ "EPUB" => 8 "HTML" => 540 "PDF" => 116 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting image</span>" "titulo" => "Added value of fused somatostatin receptor imaging/magnetic resonance imaging in a rare case of paraganglioma of the urinary bladder" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "122" "paginaFinal" => "124" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Valor añadido de la fusión de las imágenes de gammagrafía de receptores de somatostatina con imágenes de resonancia magnética en un caso inusual de paraganglioma de la vejiga" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 888 "Ancho" => 1400 "Tamanyo" => 110684 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Whole-body SRS in anterior (A1) and posterior (A2) view 4<span class="elsevierStyleHsp" style=""></span>h after <span class="elsevierStyleSup">111</span>In-pentetreotide injection showing no areas of abnormal radiopharmaceutical uptake. Maximum intensity projection SRS image 24<span class="elsevierStyleHsp" style=""></span>h after radiopharmaceutical injection (B) showing an area of increased uptake corresponding to the urinary bladder (arrow).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "G. Treglia, L. Ceriani, E. Merlo, T. Ruberto, G. Paone, L. Giovanella" "autores" => array:6 [ 0 => array:2 [ "nombre" => "G." "apellidos" => "Treglia" ] 1 => array:2 [ "nombre" => "L." "apellidos" => "Ceriani" ] 2 => array:2 [ "nombre" => "E." "apellidos" => "Merlo" ] 3 => array:2 [ "nombre" => "T." "apellidos" => "Ruberto" ] 4 => array:2 [ "nombre" => "G." "apellidos" => "Paone" ] 5 => array:2 [ "nombre" => "L." "apellidos" => "Giovanella" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2253808914000342" "doi" => "10.1016/j.remnie.2014.02.009" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808914000342?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X13001285?idApp=UINPBA00004N" "url" => "/2253654X/0000003300000002/v1_201403040016/S2253654X13001285/v1_201403040016/en/main.assets" ] "en" => array:16 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting image</span>" "titulo" => "Bouveret's syndrome on FDG PET/CT: A rare life-threatening complication of gallstone disease" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "125" "paginaFinal" => "126" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Mustafa Aras, Sabahat Inanir, Davut Tuney" "autores" => array:3 [ 0 => array:4 [ "nombre" => "Mustafa" "apellidos" => "Aras" "email" => array:1 [ 0 => "mustafa.aras@marmara.edu.tr" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">¿</span>" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Sabahat" "apellidos" => "Inanir" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 2 => array:3 [ "nombre" => "Davut" "apellidos" => "Tuney" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] ] "afiliaciones" => array:2 [ 0 => array:3 [ "entidad" => "Department of Nuclear Medicine, Marmara University School of Medicine, Istanbul, Turkey" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Department of Radiology, Marmara University School of Medicine, Istanbul, Turkey" "etiqueta" => "b" "identificador" => "aff0010" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author at: S.B. Marmara Universitesi Pendik Egitim ve Arastırma Hastanesi Nükleer Tıp Anabilim Dalı -1 kat A1 Blok Fevzi Cakmak Mahallesi Mimar Sinan Caddesi No:41 Ustkaynarca, Pendik, Istanbul, Turkey. Tel.: +90 505 553 35 24." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "El síndrome de Bouveret en FDG PET/TC: Una complicación rara y potencialmente mortal de la enfermedad de cálculos biliares" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 2850 "Ancho" => 3192 "Tamanyo" => 738262 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Besides hypermetabolic mass in the cecum (arrows in A: axial PET, CT and fusion PET/CT images, SUVmax<span class="elsevierStyleHsp" style=""></span>=<span class="elsevierStyleHsp" style=""></span>11.1) and neighbouring enlarged lymph nodes, initial staging PET/CT also showed dilated gallbladder (large white arrow in B: non-contrast enhanced CT of the PET/CT) and intra/extrahepatic biliary ducts (black arrow in B), gallstone in the gallbladder (small white arrows in B) and dilated stomach (star in B). When carefully examined, another gallstone with accompanying hypermetabolic wall thickening was seen in the lumen of the descending duodenum (arrow heads in C: axial PET, CT and fusion PET/CT images, SUVmax<span class="elsevierStyleHsp" style=""></span>=<span class="elsevierStyleHsp" style=""></span>4.7). The follow-up contrast enhanced CT scan of the abdomen also demonstrated dilated gallbladder (large white arrow in D) and biliary ducts (black arrow in D) and gallstones in the gallbladder (small white arrow in D) and in the lumen of the duodenum (arrow head in D).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">A 70-year-old female patient was admitted to our hospital with right upper quadrant pain, nausea and vomiting. An abdominal ultrasonography was requested. It revealed multiple gallstones in the gallbladder and a mass in the cecum (not shown). A colonoscopy was performed and the lesion in the cecum was biopsied. The histopathologic examination of the lesion was reported as adenocarcinoma. The patient was referred to FDG PET/CT for initial staging. Besides hypermetabolic mass in the cecum and neighbouring enlarged lymph nodes, it also showed dilated gallbladder and intra/extrahepatic biliary ducts, gallstone in the gallbladder and dilated stomach (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>A and B). When carefully examined, another gallstone with accompanying hypermetabolic wall thickening was seen in the lumen of the descending duodenum (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>C). The impacted stone in the duodenum caused partial obstruction and dilatation of the stomach which was consistent with Bouveret's syndrome. The follow-up contrast enhanced CT scan of the abdomen also demonstrated dilated gallbladder and biliary ducts and gallstones in the gallbladder and in the lumen of the duodenum (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>D). Gallstone ileus is a form of small bowel obstruction which is caused by impaction of one or more gallstones after they have migrated through a cholecysto-enteric fistula.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> Obstruction at the level of the gastric outlet by a gallstone is defined as Bouveret's syndrome.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> Bouveret's syndrome is very rare and comprises only 1–3% of the cases.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1,2</span></a> It is usually seen in elderly female patients.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1–3</span></a> Nausea, vomiting, abdominal pain, haematemesis, recent weight loss, anorexia, constipation, melena, pyrexia and obstructive jaundice are the most common presenting signs and symptoms.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1,2</span></a> The existence of pneumobilia, the demonstration of duodenal obstruction, dilated stomach and cholecysto-duodenal fistula, visualization of gallstones by radiography, ultrasonography or CT can aid in the diagnosis.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> Advanced age of patients, associated comorbidities, insidious clinical presentation and lack of specific signs cause high mortality rates for this syndrome.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1,3</span></a> In our case, the gallstone in the duodenum caused partial obstruction due to its small size. However, the larger stones may lead to serious complications which may require urgent surgical interventions. In addition to familiarity of physiologic and pathologic patterns of bowel FDG uptake, careful correlation of any FDG uptake with CT portion of the combined PET/CT examination is recommended to identify this rare life-threatening complication of gallstone disease.</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><span id="sec2005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect2005">Conflicts of interest</span><p id="par2020" class="elsevierStylePara elsevierViewall">The authors have no conflicts of interest to declare.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:2 [ 0 => array:2 [ "identificador" => "sec2005" "titulo" => "Conflicts of interest" ] 1 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "fechaRecibido" => "2013-05-06" "fechaAceptado" => "2013-08-30" "multimedia" => array:1 [ 0 => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 2850 "Ancho" => 3192 "Tamanyo" => 738262 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Besides hypermetabolic mass in the cecum (arrows in A: axial PET, CT and fusion PET/CT images, SUVmax<span class="elsevierStyleHsp" style=""></span>=<span class="elsevierStyleHsp" style=""></span>11.1) and neighbouring enlarged lymph nodes, initial staging PET/CT also showed dilated gallbladder (large white arrow in B: non-contrast enhanced CT of the PET/CT) and intra/extrahepatic biliary ducts (black arrow in B), gallstone in the gallbladder (small white arrows in B) and dilated stomach (star in B). When carefully examined, another gallstone with accompanying hypermetabolic wall thickening was seen in the lumen of the descending duodenum (arrow heads in C: axial PET, CT and fusion PET/CT images, SUVmax<span class="elsevierStyleHsp" style=""></span>=<span class="elsevierStyleHsp" style=""></span>4.7). The follow-up contrast enhanced CT scan of the abdomen also demonstrated dilated gallbladder (large white arrow in D) and biliary ducts (black arrow in D) and gallstones in the gallbladder (small white arrow in D) and in the lumen of the duodenum (arrow head in D).</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:3 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Bouveret's syndrome. Narrative review" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:2 [ 0 => "A. Koulaouzidis" 1 => "J. Moschos" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Ann Hepatol" "fecha" => "2007" "volumen" => "6" "paginaInicial" => "89" "paginaFinal" => "91" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/17519830" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Bouveret's syndrome: revisiting gallstone obstruction of the duodenum" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "D. Dan" 1 => "D.W. Collure" 2 => "E.L. Hoover" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "J Natl Med Assoc" "fecha" => "2003" "volumen" => "95" "paginaInicial" => "969" "paginaFinal" => "973" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/14620710" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Bouveret's syndrome: CT findings" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:2 [ 0 => "D. Tüney" 1 => "C. Cimşit" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s003300000444" "Revista" => array:6 [ "tituloSerie" => "Eur Radiol" "fecha" => "2000" "volumen" => "10" "paginaInicial" => "1711" "paginaFinal" => "1712" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/11097393" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/2253654X/0000003300000002/v1_201403040016/S2253654X13001546/v1_201403040016/en/main.assets" "Apartado" => array:4 [ "identificador" => "7907" "tipo" => "SECCION" "es" => array:2 [ "titulo" => "Imágenes de interés" "idiomaDefecto" => true ] "idiomaDefecto" => "es" ] "PDF" => "https://static.elsevier.es/multimedia/2253654X/0000003300000002/v1_201403040016/S2253654X13001546/v1_201403040016/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X13001546?idApp=UINPBA00004N" ]
Consulte los artículos y contenidos publicados en este medio, además de los e-sumarios de las revistas científicas en el mismo momento de publicación
Esté informado en todo momento gracias a las alertas y novedades
Acceda a promociones exclusivas en suscripciones, lanzamientos y cursos acreditados
La Revista Española de Medicina Nuclear e Imagen Molecular, fundada en 1982, es el órgano oficial de expresión de la Sociedad Española de Medicina Nuclear e Imagen Molecular, que aglutina a más de 700 miembros. La revista, que publica seis números regulares al año, tiene como principal objetivo promocionar la investigación y la formación continuada en todos los ámbitos de la Medicina Nuclear. Para ello, sus secciones principales son Originales, Notas Clínicas, Imágenes de Interés y artículos de Colaboración especial. Los trabajos pueden enviarse en español o en inglés y son sometidos a un proceso de revisión por pares. En 2009 se convirtió en la primera revista española del ámbito de la Imagen Médica en tener Factor de Impacto.
Science Citation Index Expander, Medline, IME, Bibliomed, EMBASE/Excerpta Medica, Healthstar, Cancerlit, Toxine, Inside Conferences, Scopus
Ver másEl factor de impacto mide la media del número de citaciones recibidas en un año por trabajos publicados en la publicación durante los dos años anteriores.
© Clarivate Analytics, Journal Citation Reports 2022
SJR es una prestigiosa métrica basada en la idea de que todas las citaciones no son iguales. SJR usa un algoritmo similar al page rank de Google; es una medida cuantitativa y cualitativa al impacto de una publicación.
Ver másSNIP permite comparar el impacto de revistas de diferentes campos temáticos, corrigiendo las diferencias en la probabilidad de ser citado que existe entre revistas de distintas materias.
Ver más
¿Es usted profesional sanitario apto para prescribir o dispensar medicamentos?
Are you a health professional able to prescribe or dispense drugs?
Você é um profissional de saúde habilitado a prescrever ou dispensar medicamentos