Introduction
Every day more than a million people are treated safely and successfully in healthcare. However the advances in technology and knowledge in recent decades have created an immensely complex healthcare system. This complexity brings risks, and evidence shows that things will and do go wrong in healthcare. The effects of harming a patient are widespread. There can be devastating emotional and physical consequences for patients and their families. For the staff involved too, incidents can be distressing, while members of their clinical teams can become demoralised and disaffected. Safety incidents also incur costs through litigation and extra treatment.
Patient safety concerns everyone in healthcare, whether you work in a clinical or a non-clinical role. Tackling patient safety in healthcare collectively and in a systematic way can have a positive impact on the quality of care and efficiency of healthcare organisations.
Some organisations are already well advanced along the route to patient safety but many are right at the beginning of their journey. The Department of Health publication An Organisation with a Memory1, mobilised the patient safety movement in the UK. The report reviewed the growing body of international evidence on patient safety. It drew attention to the scale and pattern of potentially avoidable patient safety incidents (1) and the devastating consequences these can have on patients, their families and the healthcare staff involved. The report also acknowledged that, as in many other countries, there has been little systematic learning from these patient safety incidents and service failure.
It is difficult to accurately estimate the extent of unintended harm to patients across healthcare from the current studies. There is likely to be significant under-reporting and inadequate documentation of patient safety incidents within medical records (the usual source of information on unintended harm for most studies). On the best available data in England, extrapolating from a small study in 2 acute care trusts,it isestimated that around 10% (850,000) of patients admitted to UK hospitals have experienced a patient safety incident, and that up to half of these incidents could have been prevented2.This study also estimated that 68,000 of these incidents may contribute to the death of patients. This equates to slightly more than one incident per day per acute Trust in England.
In the US3,4, studies have found that between 44,000 and 98,000 incidents are estimated to contribute to patient deaths. This is viewed by many commentators as under-estimating the extent of the problem. Studies in Australia5, New Zealand and Denmark1,6 have suggested similar findings.
The analysis of international evidence in the United States led to 2 important conclusions7:
1. The potential for error in healthcare systems represents a significant and serious challenge that needs concerted effort to manage.
2. The best way of improving reporting and reducing error rates is to target the underlying systems failures rather than take action against individual members of staff.
An Organisation with a Memory proposed solutions based on developing a culture of openness, reporting and safety consciousness within healthcare organisations. The report identified four key areas that need to be addressed if healthcare is to modernise successfully its approach to learning from failure:
1. Unified mechanisms for reporting, and analysis when things go wrong.
2. A more open culture in which incidents or service failures can be reported and discussed.
3. Systems and monitoring processes to ensure that where lessons are identified the necessary changes are put into practice.
4. A much wider appreciation of the value of the systems approach in preventing, analysing and learning from patient safety incidents.
The National Patient Safety Agency (NPSA) faces the challenge of how to best influence the health service, a complex and multi-level system, to help deliver these objectives. While some organisations have well established patient safety systems, there are a large number that are right at the beginning of their journey. The NPSA has therefore developed new guidance for all staff, entitled "Seven Steps to Patient Safety". These steps are founded on a thorough review of literature from across the world (on patient safety, clinical governance, change management and risk management) and on experience of what works in patient safety.
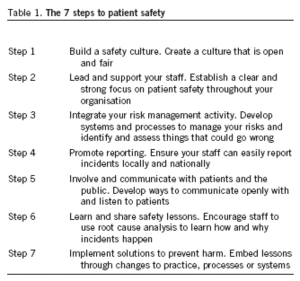
It is vital that healthcare staff can assess the progress they make towards delivering this safety agenda. Seven steps can be applied at both an organisational and departmental level. They provide a checklist to help plan activities and measure performance in patient safety. Following these steps will help ensure that the care provided is as safe as possible, and that when things do go wrong the right action is taken (table 1).
Step 1 Build a Safety culture that is open and fair
Creating a safety culture should be the first step towards a safer organisation. One of the key lessons learned in industry is that without proper changes in culture, perspective, and attitude towards incidents and their causes, they are unlikely to be reported and therefore any changes made. Improving a safety culture will help: reduce human cost in terms of patients suffering increased pain, disability, physical and psychological trauma and staff suffering distress, guilt, shame, loss of confidence and loss of morale; improve national targets around waiting times; reduce the requirements for extra treatment and extra beds. In the UK the cost of preventable patient safety incidents is estimated at £ 1 billion per annum in lost bed days alone; reduce the resources required for handling the investigations around incidents, complaints and claims; reduce the estimated wider financial and social costs which include lost working time, and disability benefits.
In order to help achieve a safety culture the NPSA organisations should undertake a baseline assessment of their safety culture and then repeat over time to measure improvement. The NPSA has also recruited a network of Patient Safety Managers who will work across England and Wales within geographical areas of each Strategic Health Authority or Region. They will provide expertise, support and coordination in the development and introduction of the national reporting and learning system, the root cause analysis toolkits and training and provide a crucial 2 way link between national and local perspectives. A key aim will be in translating national policy into local action.
Step 2 Provide leadership and support your staff
Effective team working is fundamental to the success of patient safety. There needs to be a multi-disciplinary approach to patient safety where the whole group are equal and interactive players. A guiding principle is 'If you're not sure it's safe, then it is not safe' and irrespective of your position you tell your superiors you are not sure it is safe by whatever means are available.
Crucially, in healthcare there are 2 key myths which need to be dispelled:
the perfection myth; if we try hard enough we will not make any errors;
the punishment myth; if we punish people when they make errors they will make fewer of them.
However, the truths are:
moving beyond a culture of blame does not mean an absence of accountability;
incidents are caused by complex systems, and factors which affect human beings and the way they work such as interruptions, short term memory, attention span, pressure
to hurry, fatigue, anxiety, fear, boredom, complacency and habit;
despite some high profile cases, the overwhelming majority of patient safety incidents are not caused by malicious intent or even lack of competence on the part of the individual delivering the care.
The NPSA has developed a tool to assess individual culpability called the Incident Decision Tree. This is a simple but effective tool which is designed to prompt a series of questions to enable a systematic and consistent approach to staff irrespective of organisation or profession. It is hoped that this tool will help reassure patients and the public that there is a formal framework for assessing the culpability of individuals involved in patient safety incidents and provide assistance to managers when reviewing individual staff roles within an incident. It is not meant to be a tool to use to discipline staff, fundamentally it actually steers managers to consider the systems failures which affected the performance
of the individuals involved. The tool kit can be found at www.npsa.nhs.uk/idt.
Step 3 Integrate your risk management systems
To be most effective, patient safety needs to be a fundamental part of the normal working processes of the organisation. Patient safety should cover all levels of an organisation's activities from strategic to operational and aid the achievement of goals and objectives. In practice, integrated risk management means:
Ensuring that health care organisations use the same systems for managing all their risk management functions, such as patient safety, health and safety, complaints, clinical litigation, employment litigation, financial and environmental risk.
When improvement, modernisation and clinical governance are considered, risk management is a key component to any project design.
Bringing together all sources of information related to risk and safety, for example "reactive data", such as patient safety incidents, clinical litigation claims, complaints and health and safety incidents, as well as 'proactive data', such as the results of risk assessments.
Using a consistent approach to the training, management, analysis and investigation for all potential risks and actual incidents.
Using a consistent approach and uniting all risk assessments of all types of risks for an organisation at every level. Incorporating all risks into an organisation risk assessment programme and risk register. This will mean organisations can plan more effectively and develop controls to reduce the effects of the risks identified.
Using the information gained through incidents and risk assessments to develop future business and strategic plans.
Step 4 Promote incident reporting
The first step in the pursuit of excellence in patient safety is to address the most critical question of "why do things go wrong in healthcare". Incident reporting is therefore a fundamental component of patient safety, however, to do it well it the management, review and understanding of incidents requires clinical expertise and a good understanding of the healthcare environment and the many factors which may contribute to a poor outcome. To create a safer healthcare system the NPSA was actioned with establishing a national reporting and learning system (NRLS) for patient safety incidents. This will provide us with information about patient safety problems across the health service with a view to learning lessons from these and developing solutions to minimise the risk of the same incident happening again.
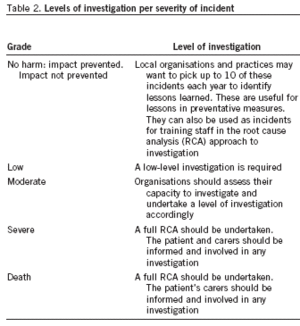
A patient safety incident is defined as "Any unintended or unexpected incident(s) which could have or did lead to harm for one or more persons receiving NHS funded healthcare". It could be a single incident or a series of incidents over time and includes incidents in relation to direct patient care, and indirect patient care such as equipment issues, staff shortages, confusing labels and so on. A patient safety incident which impacts on patients is then graded according to the severity of impact; no harm, low, moderate, severe, death, shown below. Key factors for severity categorisation are the patient's actual condition, i.e. the extent of the injury or harm, and the level of care required following the incident.
Step 5 - Involve and communication with your patients and their families
In the normal course of events if the patient is harmed in any way, then this information should be shared with the patient and or carers and relatives. Openness is a fundamental part of the partnership between patients and their care providers. "Being open" is defined as "the discussion between staff and patients and their relatives when a patient safety incident has led to harm". Incidents which were prevented from impacting on patients do not need to be disclosed to patients but nonetheless are essential for learning. The NPSA is developing a model policy which can be used to provide a framework for local organisations as a basis for developing their own policies and procedures for open disclosure. The development of local disclosure policies will help to facilitate cultural change and improve patient and public confidence:
The NPSA open disclosure policy advocates:
An acknowledgment and a factual explanation of what happened;
An apology;
An explanation as to the potential consequences and what steps are being taken to manage the incident;
Reassurance for patients and their families that lessons will be learnt from the incident to reduce the chance of a reoccurrence.
Step 6 Learn from your incidents
Reporting when things go wrong is essential in healthcare. But it is only part of the process of improving patient safety. It is equally important that health care organisations look at the underlying causes of patient safety incidents and learn how to prevent them from happening again. Often there are many underlying causes and in the majority of cases these extend beyond the individual staff member or team involved.
Research has shown that an RCA approach to incident investigation will achieve a number of patient safety benefits1,5,8. These include:
providing a structured and consistent approach to incident investigation across all care settings;
shifting the focus away from individuals and on to the system to help build an open and fair culture;
increasing awareness of patient safety issues and demonstrating the benefits of reporting incidents;
helping engage patients in the investigation;
focusing recommendations and change and developing real solutions as a result of identifying the root cause(s) of an incident.
Practical support for using RCA can be found in the NPSA's web-based e-learning toolkit (at: www.npsa.nhs.uk/rca). This includes advice on how to document and organise evidence, guidelines on patient and staff interviews, detail and illustrations of techniques for analysing incident information, barrier analysis tools and case studies to help staff familiarise themselves with the methodology.
All patient safety incidents should be subjected to an appropriate level of local investigation and analysis to determine the cause (table 2).
Step 7 Implement solutions to prevent harm
NHS organisations, staff that work in them and patients that experience them first hand, have a wealth of information about how systems are failing to provide optimum care. The aim of solutions development is to make it easy to do things right and difficult to do things wrong.
The local analysis and investigation of patient safety incidents should lead to a local action plan to ensure lessons are applied throughout the organisation. Local and national solutions to improve patient safety need to be realistic, sustainable and cost effective. They also need to be validated to make sure they work. Simple changes generally spread faster than complicated ones. Staff should work through each potential recommendation for change or each potential risk and prioritise them. It is all too easy to list over 30 recommendations following an investigation when in reality only three or four can be implemented effectively. Improvement and patient safety is not about introducing more work it is about working differently.
This could include redesigning systems and processes, actual examples include effective use packaging of medication to prompt compliance or to alert dispensing staff and patients
to different dose strengths; of computer-based support systems such as computerised records, and medication systems; new labelling techniques; and redesigning care delivery by reducing delays and improving patient flow and access; and training including electronic learning packages, face to face training, simulation training. Other examples are in the form of barriers to error. A barrier is a defence or control measure to prevent harm to vulnerable or valuable objects. A barrier in healthcare is either an obstruction (e.g. locked controlled drug cupboards) or preventative action (e.g. using a checklist). The fact that a patient safety incident has taken place means that one or more of the barriers have failed. This stage of solution development is known as 'barrier analysis'9-12, and is designed to identify:
which barriers should have been in place to prevent the incident;
why the barrier failed;
which barriers could be used to prevent the incident happening again.
It offers a structured way to visualise the events related to system failure and can be used reactively to solve problems or proactively to evaluate existing barriers. Physical barriers are the most reliable in terms of providing failsafe solutions to safety problems. Natural barriers, while less effective, generally provide a more robust solution than human action and administrative barriers. These are considered the least reliable barriers because they rely on human action and behaviour, and mistakes can be made (table 3).
Conclusion
Patient safety means different things to different people. There is also a huge variation in management and implementation of patient safety practices. The argument for patient safety is compelling. It is hoped that the NPSA guidance "Seven Steps to Patient Safety" will offer something useful to those who are the start of the patient safety journey as well as those who have traveled quite some way in the pursuit of excellence in patient safety.