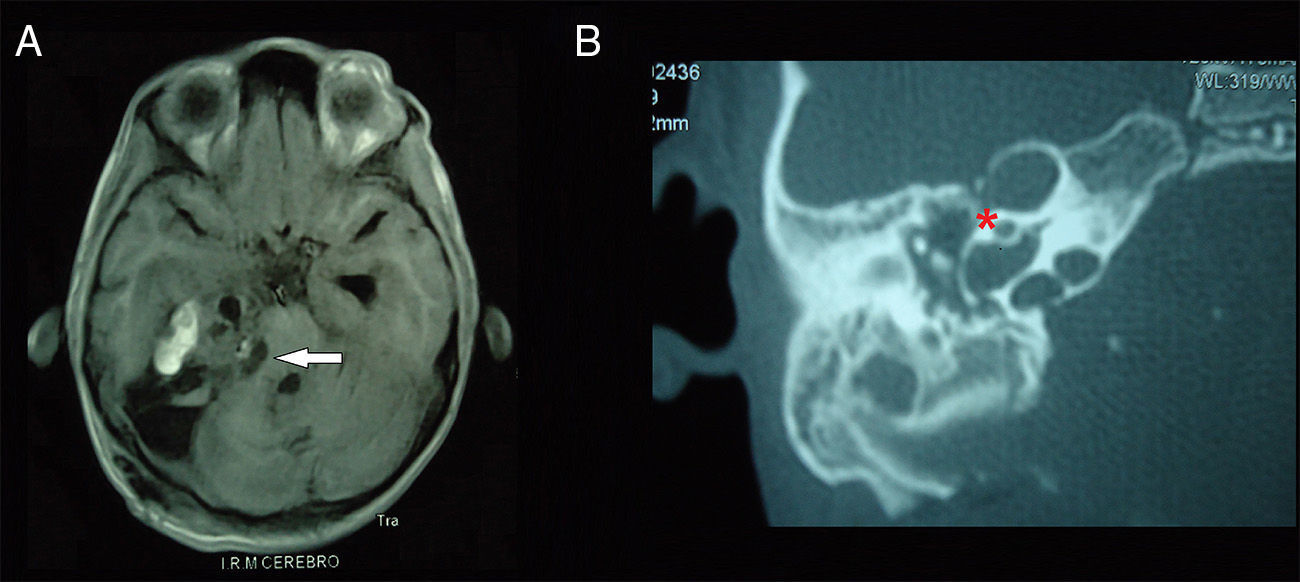
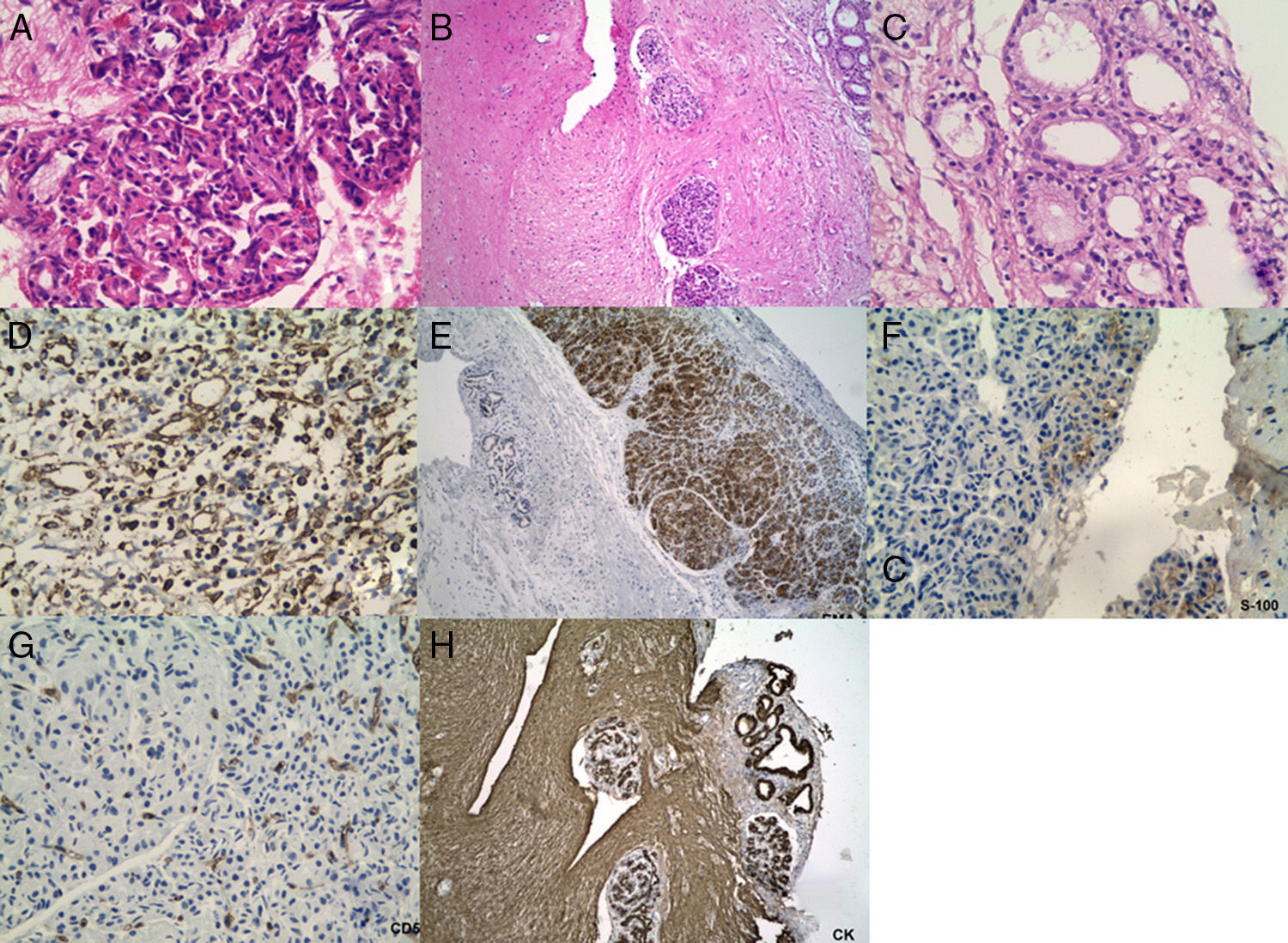
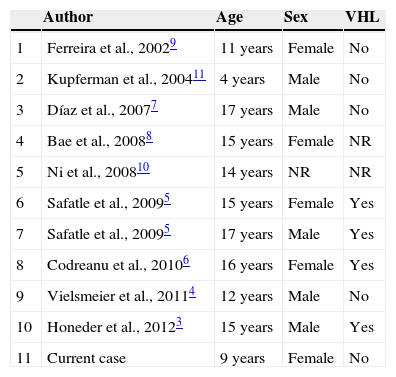
array:23 [ "pii" => "S2173573515000058" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2013.06.016" "estado" => "S300" "fechaPublicacion" => "2015-01-01" "aid" => "504" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "copyrightAnyo" => "2013" "documento" => "simple-article" "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:52-5" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 1620 "formatos" => array:3 [ "EPUB" => 40 "HTML" => 1119 "PDF" => 461 ] ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S0001651913001301" "issn" => "00016519" "doi" => "10.1016/j.otorri.2013.06.002" "estado" => "S300" "fechaPublicacion" => "2015-01-01" "aid" => "504" "copyright" => "Elsevier España, S.L.U. y Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "crossmark" => 0 "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:52-5" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 2051 "formatos" => array:3 [ "EPUB" => 34 "HTML" => 1556 "PDF" => 461 ] ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Caso clínico</span>" "titulo" => "Tumor papilar del saco endolinfático: presentación catastrófica en un escolar" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "52" "paginaFinal" => "55" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Papillary endolymphatic sac tumor: Catastrophic presentation in a child" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figura 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 582 "Ancho" => 1300 "Tamanyo" => 95061 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">A) Imagen axial de resonancia magnética (T1 con gadolinio). Se aprecia el tumor ocupando el ángulo pontocerebeloso derecho. Adicionalmente, se observa compresión extrínseca del tallo cerebral y cuarto ventrículo, asociado a dilatación del asta temporal del ventrículo lateral izquierdo (flecha blanca). B) Corte axial de tomografía axial computarizada de hueso temporal, donde se demuestra extensa destrucción del hueso temporal derecho (asterisco rojo).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Martha C. Tuñón-Pitalúa, Leonardo Domínguez-de la Ossa, Gabriel Alcalá-Cerra, Javier Baena-del Valle" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Martha C." "apellidos" => "Tuñón-Pitalúa" ] 1 => array:2 [ "nombre" => "Leonardo" "apellidos" => "Domínguez-de la Ossa" ] 2 => array:2 [ "nombre" => "Gabriel" "apellidos" => "Alcalá-Cerra" ] 3 => array:2 [ "nombre" => "Javier" "apellidos" => "Baena-del Valle" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2173573515000058" "doi" => "10.1016/j.otoeng.2013.06.016" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573515000058?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651913001301?idApp=UINPBA00004N" "url" => "/00016519/0000006600000001/v3_201706012022/S0001651913001301/v3_201706012022/es/main.assets" ] ] "itemSiguiente" => array:18 [ "pii" => "S2173573515000046" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2013.06.015" "estado" => "S300" "fechaPublicacion" => "2015-01-01" "aid" => "503" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:56-8" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 2238 "formatos" => array:3 [ "EPUB" => 58 "HTML" => 1576 "PDF" => 604 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case study</span>" "titulo" => "Extranasopharyngeal Angiofibroma of the Left Lower Turbinate: A Case Report" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "56" "paginaFinal" => "58" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Fibroangioma extranasofaríngeo de cornete nasal inferior: presentación de un caso" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 489 "Ancho" => 1300 "Tamanyo" => 78700 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Computed tomography of nose and sinuses with contrast, axial (a) and coronal (b) sections, in which a tumoural lesion that contacts the nasal septum and left inferior turbinate with limited contrast uptake can be seen.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Rodolfo Nazar, Alfredo Naser, Fabían Rubio, Gonzalo Ortega" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Rodolfo" "apellidos" => "Nazar" ] 1 => array:2 [ "nombre" => "Alfredo" "apellidos" => "Naser" ] 2 => array:2 [ "nombre" => "Fabían" "apellidos" => "Rubio" ] 3 => array:2 [ "nombre" => "Gonzalo" "apellidos" => "Ortega" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0001651913001295" "doi" => "10.1016/j.otorri.2013.06.001" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0001651913001295?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573515000046?idApp=UINPBA00004N" "url" => "/21735735/0000006600000001/v2_201503020128/S2173573515000046/v2_201503020128/en/main.assets" ] "itemAnterior" => array:18 [ "pii" => "S2173573515000034" "issn" => "21735735" "doi" => "10.1016/j.otoeng.2013.07.001" "estado" => "S300" "fechaPublicacion" => "2015-01-01" "aid" => "500" "copyright" => "Elsevier España, S.L.U. and Sociedad Española de Otorrinolaringología y Patología Cérvico-Facial" "documento" => "simple-article" "subdocumento" => "crp" "cita" => "Acta Otorrinolaringol Esp. 2015;66:49-51" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:2 [ "total" => 1955 "formatos" => array:3 [ "EPUB" => 39 "HTML" => 1206 "PDF" => 710 ] ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case study</span>" "titulo" => "Nasolabial Fold Lymphadenopathy Secondary to Fungal Rhinosinusitis" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "49" "paginaFinal" => "51" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Adenopatía nasogeniana secundaria a rinosinusitis fúngica" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 694 "Ancho" => 1904 "Tamanyo" => 151587 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">CAT scan of paranasal sinuses with intravenous contrast. Expansive hypodense lesion in right maxillary antrum with peripheral localised calcification (red arrow) that extends in an anterior direction (yellow arrow), conditioning thinning of the anterior inferior osseous wall (blue arrow).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Juan A. Pasamontes, Felicia Marginean, Gloria Torralbo, Jesús M. Martínez" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Juan A." "apellidos" => "Pasamontes" ] 1 => array:2 [ "nombre" => "Felicia" "apellidos" => "Marginean" ] 2 => array:2 [ "nombre" => "Gloria" "apellidos" => "Torralbo" ] 3 => array:2 [ "nombre" => "Jesús M." "apellidos" => "Martínez" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S000165191300126X" "doi" => "10.1016/j.otorri.2013.07.002" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => true "ES2" => true "LATM" => true ] "gratuito" => true "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S000165191300126X?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573515000034?idApp=UINPBA00004N" "url" => "/21735735/0000006600000001/v2_201503020128/S2173573515000034/v2_201503020128/en/main.assets" ] "en" => array:17 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Case study</span>" "titulo" => "Papillary Endolymphatic Sac Tumor: Catastrophic Presentation in a Child" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "52" "paginaFinal" => "55" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Martha C. Tuñón-Pitalúa, Leonardo Domínguez-de la Ossa, Gabriel Alcalá-Cerra, Javier Baena-del Valle" "autores" => array:4 [ 0 => array:3 [ "nombre" => "Martha C." "apellidos" => "Tuñón-Pitalúa" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 1 => array:3 [ "nombre" => "Leonardo" "apellidos" => "Domínguez-de la Ossa" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 2 => array:4 [ "nombre" => "Gabriel" "apellidos" => "Alcalá-Cerra" "email" => array:2 [ 0 => "alcalagabriel@gmail.com" 1 => "cisneuro.investigacion@gmail.com" ] "referencia" => array:3 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">c</span>" "identificador" => "aff0015" ] 2 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 3 => array:3 [ "nombre" => "Javier" "apellidos" => "Baena-del Valle" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] ] "afiliaciones" => array:3 [ 0 => array:3 [ "entidad" => "Sección de Patología, Facultad de Medicina, Universidad de Cartagena, Cartagena de Indias, Colombia" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Sección de Neurocirugía, Facultad de Medicina, Universidad de Cartagena, Cartagena de Indias, Colombia" "etiqueta" => "b" "identificador" => "aff0010" ] 2 => array:3 [ "entidad" => "Grupo de Investigación en Ciencias de la Salud y Neurociencias (CISNEURO), Cartagena de Indias, Colombia" "etiqueta" => "c" "identificador" => "aff0015" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Tumor papilar del saco endolinfático: presentación catastrófica en un escolar" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 582 "Ancho" => 1300 "Tamanyo" => 108468 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">(A) Magnetic resonance axial image (T1 with gadolinium). The tumour can be seen occupying the right cerebellopontine angle. Extrinsic compression of the brainstem and 4th ventricle can also be seen, associated with dilation of the temporal horn of the left lateral ventricle (white arrow). (B) Axial slice of computed axial tomography of the temporal bone, where extensive destruction of the right temporal bone is shown (red asterisk).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Clinical Case</span><p id="par0005" class="elsevierStylePara elsevierViewall">This was a 9-year-old female patient from a rural area, admitted to emergency service due to rapidly progressing deterioration of the state of consciousness. In the clinical examination, she was comatose, with bilateral non-reflective mydriasis, grade IV (House-Brackmann scale) right facial paralysis, absence of right corneal reflex and bilateral extensor motor responses to pain. When asked, the relatives did not report the presence of symptoms before her admission; in fact, they denied that the patient has any symptoms referring to the vestibular-cochlear system, such as vertigo, hypoacusis, hyperacusis, weakness of the facial muscles or instability in walking.</p><p id="par0010" class="elsevierStylePara elsevierViewall">The patient presented no other clinical signs that would suggest von Hippel–Lindau (VHL) disease.</p><p id="par0015" class="elsevierStylePara elsevierViewall">A contrast-free cerebral computed tomography revealed a tumoral lesion of heterogeneous density with areas of calcification, which deformed and perforated the right temporal bone; the lesion extended from the temporal bone towards the cerebellopontine angle, compressing the brainstem. In addition, partial occlusion of the 4th ventricle could be seen, causing obstructive hydrocephaly. A contrasting cerebral magnetic resonance (MR) helped to define lesion borders; the MR image presented heterogeneous intensity in the T1- and T2-weighted sequences, due to the presence of solid cystic components, indicating subtle gadolinium uptake. Because of the patient's clinical condition, she was given immediate surgical treatment (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>A and B).</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0020" class="elsevierStylePara elsevierViewall">To handle the hydrocephaly, an endoscopic 3rd ventriclocisternostomy was performed, with a later partial resection of the tumour using retrosigmoid approach, to decompress the brainstem and cerebellum. During this procedure, a large, pale brown encapsulated lesion of very firm consistency was identified; this lesion emerged from the temporal bone, firmly attached to the surrounding dura mater. Almost the entire lesion perforated the dura mater, compressing the cerebellum on the petrous face and displacing it posteriorly, while the protuberance and the brainstem were displaced in the anterior direction. During the procedure it was impossible to identify the entrance site of the <span class="elsevierStyleSmallCaps">vii</span> and <span class="elsevierStyleSmallCaps">viii</span> cranial nerves by the internal auditory canal. Likewise, it was impossible to visualise their apparent origins at the level of the brainstem. During the resection, elevated tumour vascularisation was notable, with this being reflected in intraoperative haematic losses that prevented a more radical resection.</p><p id="par0025" class="elsevierStylePara elsevierViewall">During the postoperative period the patient did not improve in clinical condition. She remained in a profound coma for 18 days, with persistence of bilateral mydriasis and decerebrate motor responses. The patient died as a result of septic shock secondary to a nosocomial infection of the urinary tract.</p><p id="par0030" class="elsevierStylePara elsevierViewall">Pathological and immunohistochemical studies confirmed the diagnosis of papillary endolymphatic sac tumour (PELST) (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>A–H).</p><elsevierMultimedia ident="fig0010"></elsevierMultimedia></span><span id="sec0010" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0010">Discussion</span><p id="par0035" class="elsevierStylePara elsevierViewall">Originating in the vestibular aqueduct, a PELST is a low-grade adenocarcinoma. It can present sporadically or, as one of the manifestations, within the neoplastic spectrum that affects patients with VHL disease.<a class="elsevierStyleCrossRef" href="#bib0070"><span class="elsevierStyleSup">1</span></a></p><p id="par0040" class="elsevierStylePara elsevierViewall">These lesions mainly affect the young adult population. In patients with VHL disease, the average age at on-set is from 31 to 38 years; in individuals that do not suffer the mutation, it is diagnosed at the age of approximately 52 years; and it is only found in paediatric patients rarely.<a class="elsevierStyleCrossRef" href="#bib0075"><span class="elsevierStyleSup">2</span></a></p><p id="par0045" class="elsevierStylePara elsevierViewall">We reviewed the articles published between January 1984 and January 2013, using PubMed, EMBASE, LILACS, Science Direct, OVID, SCIELO and Google Scholar; in this review we found only 10 cases in patients younger than 20 years of age.<a class="elsevierStyleCrossRefs" href="#bib0080"><span class="elsevierStyleSup">3–11</span></a> In these cases, the average age at diagnosis was 13.6 years, while the distribution by sex was practically the same. This differs from the predilection for females observed in adults (female ratio of 3:2) (<a class="elsevierStyleCrossRef" href="#tbl0005">Table 1</a>).<a class="elsevierStyleCrossRef" href="#bib0075"><span class="elsevierStyleSup">2</span></a></p><elsevierMultimedia ident="tbl0005"></elsevierMultimedia><p id="par0050" class="elsevierStylePara elsevierViewall">Nearly 20% of adults that have a PELST suffer from VHL disease.<a class="elsevierStyleCrossRefs" href="#bib0070"><span class="elsevierStyleSup">1,2</span></a> Nevertheless, the literature review demonstrated that VHL prevalence in paediatric patients reaches 54.5%. This suggests that, in these patients, the development of the neoplasia could be earlier or more accelerated than in sporadic cases. This hypothesis is also backed by the observations of Lonser et al, who noted that the average age in sporadic cases is 20 years higher than that of the tumours associated with the mutation.<a class="elsevierStyleCrossRef" href="#bib0070"><span class="elsevierStyleSup">1</span></a></p><p id="par0055" class="elsevierStylePara elsevierViewall">The PELST are found in Trautmann's triangle, in an intraosseous area located at the half-way point between the internal auditory canal and the sigmoid sinus.<a class="elsevierStyleCrossRef" href="#bib0075"><span class="elsevierStyleSup">2</span></a> Due to its limited capacity, this confined space can tolerate only very small tumour volumes before producing symptoms. In the largest series published to date, Kim et al. reported an average tumour size of only 1.3<span class="elsevierStyleHsp" style=""></span>cm at diagnosis, so most of the symptoms produced are audiovestibular.<a class="elsevierStyleCrossRef" href="#bib0125"><span class="elsevierStyleSup">12</span></a> Reduced auditory acuity is found in 94% of the cases, followed by tinnitus (55%), vertigo (47%), facial paralysis (32.7%), paralysis of lower cranial nerves (5%) and facial paresthesias (5%).<a class="elsevierStyleCrossRefs" href="#bib0075"><span class="elsevierStyleSup">2,12</span></a></p><p id="par0060" class="elsevierStylePara elsevierViewall">Serious symptoms such as acute obstructive hydrocephaly are extremely rare, although they can appear in presence of very large tumours. There was only 1 other similar case, which also began with obstructive hydrocephaly, reported by Joseph et al., who described favourable evolution in an adult who had a giant tumour that obliterated the 4th ventricle once drainage of cerebrospinal fluid was re-established with a ventricle-peritoneal derivation and the lesion was partially resected.<a class="elsevierStyleCrossRef" href="#bib0130"><span class="elsevierStyleSup">13</span></a> In contrast to that case, our final result was caused by the rostrocaudal deterioration that the patient presented upon admission. This was corroborated by the clinical findings of profound coma, bilateral mydriasis and abnormal decerebrate postures, suggesting an extensive brainstem compromise, which was irreversible in spite of surgical treatment.</p></span><span id="sec0015" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0015">Funding</span><p id="par0065" class="elsevierStylePara elsevierViewall">Funding was provided by the Health Sciences and Neurosciences Research Group (CISNEURO), Cartagena de Indias, Colombia.</p></span><span id="sec0020" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0020">Conflict of Interest</span><p id="par0070" class="elsevierStylePara elsevierViewall">The authors have no conflicts of interest to declare.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:5 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Clinical Case" ] 1 => array:2 [ "identificador" => "sec0010" "titulo" => "Discussion" ] 2 => array:2 [ "identificador" => "sec0015" "titulo" => "Funding" ] 3 => array:2 [ "identificador" => "sec0020" "titulo" => "Conflict of Interest" ] 4 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "fechaRecibido" => "2013-03-19" "fechaAceptado" => "2013-06-13" "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Tuñón-Pitalúa MC, Domínguez-de la Ossa L, Alcalá-Cerra G, Baena-del Valle J. Tumor papilar del saco endolinfático: presentación catastrófica en un escolar. Acta Otorrinolaringol Esp. 2015;66:52–5.</p>" ] ] "multimedia" => array:3 [ 0 => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 582 "Ancho" => 1300 "Tamanyo" => 108468 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">(A) Magnetic resonance axial image (T1 with gadolinium). The tumour can be seen occupying the right cerebellopontine angle. Extrinsic compression of the brainstem and 4th ventricle can also be seen, associated with dilation of the temporal horn of the left lateral ventricle (white arrow). (B) Axial slice of computed axial tomography of the temporal bone, where extensive destruction of the right temporal bone is shown (red asterisk).</p>" ] ] 1 => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figure 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 1098 "Ancho" => 1500 "Tamanyo" => 531252 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Histopathological findings of the papillary endolymphatic sac tumour. (A–C) H&E: tumour consisting of glandular acini with eosinophilic cytoplasm and other areas with clear cytoplasm. Dilated structures of cystic appearance can also be seen (A and C). (D) Immunolabeling for vimentin (+); (E) EMA (+); (F) S-100 (+ focal); (G) CD56 (+ focal), and (H) cytokeratin (+). GFAP and TTF-1 were negative.</p>" ] ] 2 => array:7 [ "identificador" => "tbl0005" "etiqueta" => "Table 1" "tipo" => "MULTIMEDIATABLA" "mostrarFloat" => true "mostrarDisplay" => false "tabla" => array:2 [ "leyenda" => "<p id="spar0020" class="elsevierStyleSimplePara elsevierViewall">NR: not reported; PELST: papillary endolymphatic sac tumour; VHL: von Hippel–Lindau disease.</p>" "tablatextoimagen" => array:1 [ 0 => array:2 [ "tabla" => array:1 [ 0 => """ <table border="0" frame="\n \t\t\t\t\tvoid\n \t\t\t\t" class=""><thead title="thead"><tr title="table-row"><th class="td" title="table-head " align="" valign="top" scope="col" style="border-bottom: 2px solid black"> \t\t\t\t\t\t\n \t\t\t\t</th><th class="td" title="table-head " align="left" valign="top" scope="col" style="border-bottom: 2px solid black">Author \t\t\t\t\t\t\n \t\t\t\t</th><th class="td" title="table-head " align="left" valign="top" scope="col" style="border-bottom: 2px solid black">Age \t\t\t\t\t\t\n \t\t\t\t</th><th class="td" title="table-head " align="left" valign="top" scope="col" style="border-bottom: 2px solid black">Sex \t\t\t\t\t\t\n \t\t\t\t</th><th class="td" title="table-head " align="left" valign="top" scope="col" style="border-bottom: 2px solid black">VHL \t\t\t\t\t\t\n \t\t\t\t</th></tr></thead><tbody title="tbody"><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">1 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Ferreira et al., 2002<a class="elsevierStyleCrossRef" href="#bib0110"><span class="elsevierStyleSup">9</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">11 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Female \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">No \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">2 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Kupferman et al., 2004<a class="elsevierStyleCrossRef" href="#bib0120"><span class="elsevierStyleSup">11</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">4 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Male \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">No \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">3 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Díaz et al., 2007<a class="elsevierStyleCrossRef" href="#bib0100"><span class="elsevierStyleSup">7</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">17 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Male \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">No \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">4 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Bae et al., 2008<a class="elsevierStyleCrossRef" href="#bib0105"><span class="elsevierStyleSup">8</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">15 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Female \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">NR \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">5 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Ni et al., 2008<a class="elsevierStyleCrossRef" href="#bib0115"><span class="elsevierStyleSup">10</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">14 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">NR \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">NR \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">6 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Safatle et al., 2009<a class="elsevierStyleCrossRef" href="#bib0090"><span class="elsevierStyleSup">5</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">15 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Female \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Yes \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">7 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Safatle et al., 2009<a class="elsevierStyleCrossRef" href="#bib0090"><span class="elsevierStyleSup">5</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">17 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Male \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Yes \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">8 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Codreanu et al., 2010<a class="elsevierStyleCrossRef" href="#bib0095"><span class="elsevierStyleSup">6</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">16 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Female \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Yes \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">9 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Vielsmeier et al., 2011<a class="elsevierStyleCrossRef" href="#bib0085"><span class="elsevierStyleSup">4</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">12 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Male \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">No \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">10 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Honeder et al., 2012<a class="elsevierStyleCrossRef" href="#bib0080"><span class="elsevierStyleSup">3</span></a> \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">15 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Male \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Yes \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td" title="table-entry " align="char" valign="top">11 \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Current case \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="char" valign="top">9 years \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">Female \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="table-entry " align="left" valign="top">No \t\t\t\t\t\t\n \t\t\t\t</td></tr></tbody></table> """ ] "imagenFichero" => array:1 [ 0 => "xTab689589.png" ] ] ] ] "descripcion" => array:1 [ "en" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall">Characteristics of PELST cases reported in paediatric patients.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:13 [ 0 => array:3 [ "identificador" => "bib0070" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "The vestibular aqueduct: site of origin of endolymphatic sac tumors" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:5 [ 0 => "R.R. Lonser" 1 => "M. Baggenstos" 2 => "H.J. Kim" 3 => "J.A. Butman" 4 => "A.O. Vortmeyer" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.3171/JNS/2008/108/4/0751" "Revista" => array:6 [ "tituloSerie" => "J Neurosurg" "fecha" => "2008" "volumen" => "108" "paginaInicial" => "751" "paginaFinal" => "756" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/18377255" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0075" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "The Gruppo Otologico experience of endolymphatic sac tumor" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "S.T. Husseini" 1 => "E. Piccirillo" 2 => "A. Taibah" 3 => "C.T. Paties" 4 => "T. Almutair" 5 => "M. Sanna" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.anl.2012.01.009" "Revista" => array:6 [ "tituloSerie" => "Auris Nasus Larynx" "fecha" => "2013" "volumen" => "40" "paginaInicial" => "25" "paginaFinal" => "31" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/22326122" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0080" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endolymphatic sac tumor and angiomatous lesions of the nasal and pharyngeal mucosa as a first manifestation of von Hippel–Lindau disease" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "C. Honeder" 1 => "W. Gstoettner" 2 => "C. Matula" 3 => "C. Czerny" 4 => "A. Gruber" 5 => "R. Ramsebner" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1002/lary.23438" "Revista" => array:6 [ "tituloSerie" => "Laryngoscope" "fecha" => "2012" "volumen" => "122" "paginaInicial" => "2300" "paginaFinal" => "2303" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/22777797" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0085" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Tumour of the endolymphatic sac in a 12-year-old child" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "V. Vielsmeier" 1 => "P. Kwok" 2 => "M. Jakob" 3 => "C. Vogel" 4 => "J. Strutz" 5 => "M. Huber" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s00106-010-2228-1" "Revista" => array:6 [ "tituloSerie" => "HNO" "fecha" => "2011" "volumen" => "59" "paginaInicial" => "529" "paginaFinal" => "532" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/21181388" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0090" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endolymphatic sac tumor and von Hippel–Lindau disease in a single family" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "P.P. Safatle" 1 => "L. Farage" 2 => "A. Sampaio" 3 => "F.A. Ferreira" 4 => "H.P. Safatle" 5 => "C.A. Oliveira" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Arq Neuropsiquiatr" "fecha" => "2009" "volumen" => "67" "paginaInicial" => "1097" "paginaFinal" => "1099" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/20069227" "web" => "Medline" ] ] ] ] ] ] ] ] 5 => array:3 [ "identificador" => "bib0095" "etiqueta" => "6" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endolymphatic sac tumors in von Hippel–Lindau disease: report of three cases" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "C.M. Codreanu" 1 => "M. Duet" 2 => "C. Hautefort" 3 => "M. Wassef" 4 => "J.P. Guichard" 5 => "S. Giraud" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1097/MAO.0b013e3181d8d863" "Revista" => array:6 [ "tituloSerie" => "Otol Neurotol" "fecha" => "2010" "volumen" => "31" "paginaInicial" => "660" "paginaFinal" => "664" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/20351605" "web" => "Medline" ] ] ] ] ] ] ] ] 6 => array:3 [ "identificador" => "bib0100" "etiqueta" => "7" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Tumors and pseudotumors of the endolymphatic sac" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:5 [ 0 => "R.C. Díaz" 1 => "E.H. Amjad" 2 => "E.W. Sargent" 3 => "M.J. Larouere" 4 => "W.T. Shaia" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1055/s-2007-991116" "Revista" => array:6 [ "tituloSerie" => "Skull Base" "fecha" => "2007" "volumen" => "17" "paginaInicial" => "379" "paginaFinal" => "393" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/18449331" "web" => "Medline" ] ] ] ] ] ] ] ] 7 => array:3 [ "identificador" => "bib0105" "etiqueta" => "8" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endolymphatic sac tumors: report of four cases" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "C.W. Bae" 1 => "Y.H. Cho" 2 => "J.W. Chung" 3 => "C.J. Kim" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.3340/jkns.2008.44.4.268" "Revista" => array:6 [ "tituloSerie" => "J Korean Neurosurg Soc" "fecha" => "2008" "volumen" => "44" "paginaInicial" => "268" "paginaFinal" => "272" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/19096691" "web" => "Medline" ] ] ] ] ] ] ] ] 8 => array:3 [ "identificador" => "bib0110" "etiqueta" => "9" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endolymphatic sac tumor: unique features of two cases and review of the literature" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "M.A. Ferreira" 1 => "I. Feiz-Erfan" 2 => "J.M. Zabramski" 3 => "R.F. Spetzler" 4 => "S.W. Coons" 5 => "M.C. Preul" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Acta Neurochir (Wien)" "fecha" => "2002" "volumen" => "144" "paginaInicial" => "1047" "paginaFinal" => "1053" ] ] ] ] ] ] 9 => array:3 [ "identificador" => "bib0115" "etiqueta" => "10" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Surgery for endolymphatic sac tumor: whether and when to keep hearing" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "Y. Ni" 1 => "S. Wang" 2 => "W. Huang" 3 => "H. Jiang" 4 => "T. Zhang" 5 => "Y. Wang" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1080/00016480701808996" "Revista" => array:6 [ "tituloSerie" => "Acta Otolaryngol" "fecha" => "2008" "volumen" => "128" "paginaInicial" => "976" "paginaFinal" => "983" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/19086306" "web" => "Medline" ] ] ] ] ] ] ] ] 10 => array:3 [ "identificador" => "bib0120" "etiqueta" => "11" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endolymphatic sac tumor in a 4-year-old boy" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:5 [ 0 => "M.E. Kupferman" 1 => "D.C. Bigelow" 2 => "D.F. Carpentieri" 3 => "L.T. Bilaniuk" 4 => "K. Kazahaya" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Otol Neurotol" "fecha" => "2004" "volumen" => "25" "paginaInicial" => "782" "paginaFinal" => "786" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/15354011" "web" => "Medline" ] ] ] ] ] ] ] ] 11 => array:3 [ "identificador" => "bib0125" "etiqueta" => "12" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Surgical resection of endolymphatic sac tumors in von Hippel–Lindau disease: findings, results, and indications" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "H.J. Kim" 1 => "M. Hagan" 2 => "J.A. Butman" 3 => "M. Baggenstos" 4 => "C. Brewer" 5 => "C. Zalewski" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1002/lary.23646" "Revista" => array:6 [ "tituloSerie" => "Laryngoscope" "fecha" => "2013" "volumen" => "123" "paginaInicial" => "477" "paginaFinal" => "483" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/23070752" "web" => "Medline" ] ] ] ] ] ] ] ] 12 => array:3 [ "identificador" => "bib0130" "etiqueta" => "13" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endolymphatic sac tumor: a rare cerebellopontine angle tumor" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "B.V. Joseph" 1 => "G. Chacko" 2 => "L. Raghuram" 3 => "V. Rajshekhar" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Neurol India" "fecha" => "2002" "volumen" => "50" "paginaInicial" => "476" "paginaFinal" => "479" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/12577100" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/21735735/0000006600000001/v2_201503020128/S2173573515000058/v2_201503020128/en/main.assets" "Apartado" => array:4 [ "identificador" => "5881" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Case Studies" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/21735735/0000006600000001/v2_201503020128/S2173573515000058/v2_201503020128/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173573515000058?idApp=UINPBA00004N" ]
Journal Information
Vol. 66. Issue 1.
Pages 52-55 (January - February 2015)
Share
Download PDF
More article options
Vol. 66. Issue 1.
Pages 52-55 (January - February 2015)
Case study
Papillary Endolymphatic Sac Tumor: Catastrophic Presentation in a Child
Tumor papilar del saco endolinfático: presentación catastrófica en un escolar
Visits
1620
Martha C. Tuñón-Pitalúaa, Leonardo Domínguez-de la Ossab, Gabriel Alcalá-Cerrab,c,
, Javier Baena-del Vallea
Corresponding author
a Sección de Patología, Facultad de Medicina, Universidad de Cartagena, Cartagena de Indias, Colombia
b Sección de Neurocirugía, Facultad de Medicina, Universidad de Cartagena, Cartagena de Indias, Colombia
c Grupo de Investigación en Ciencias de la Salud y Neurociencias (CISNEURO), Cartagena de Indias, Colombia
This item has received
Article information
These are the options to access the full texts of the publication Acta Otorrinolaringológica Española
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail