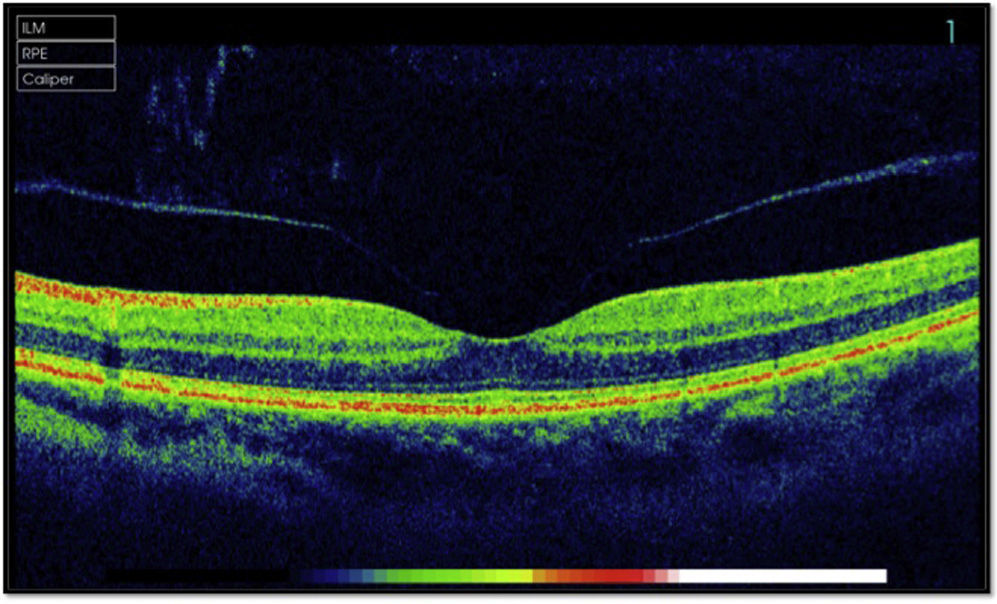
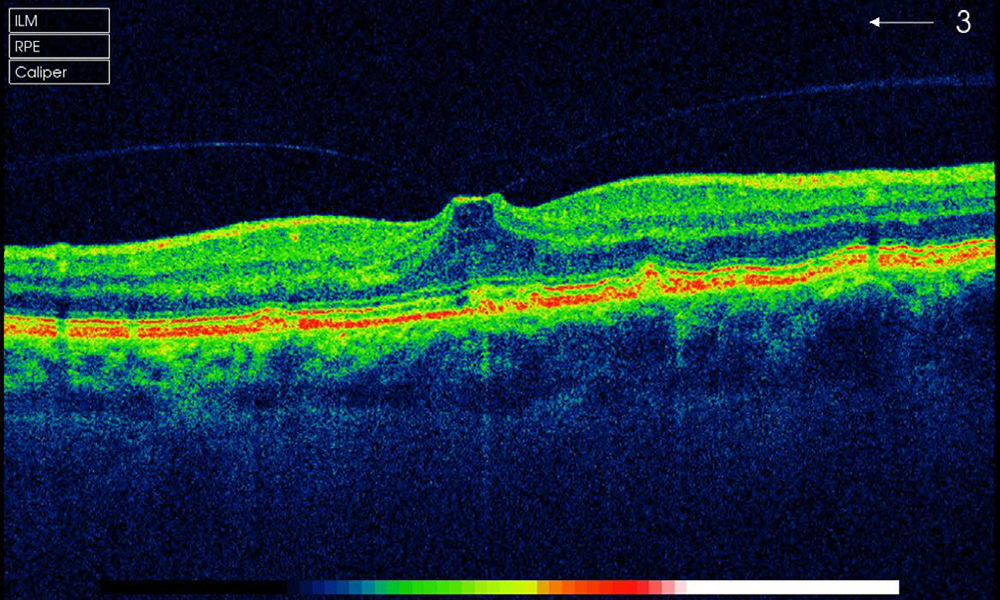
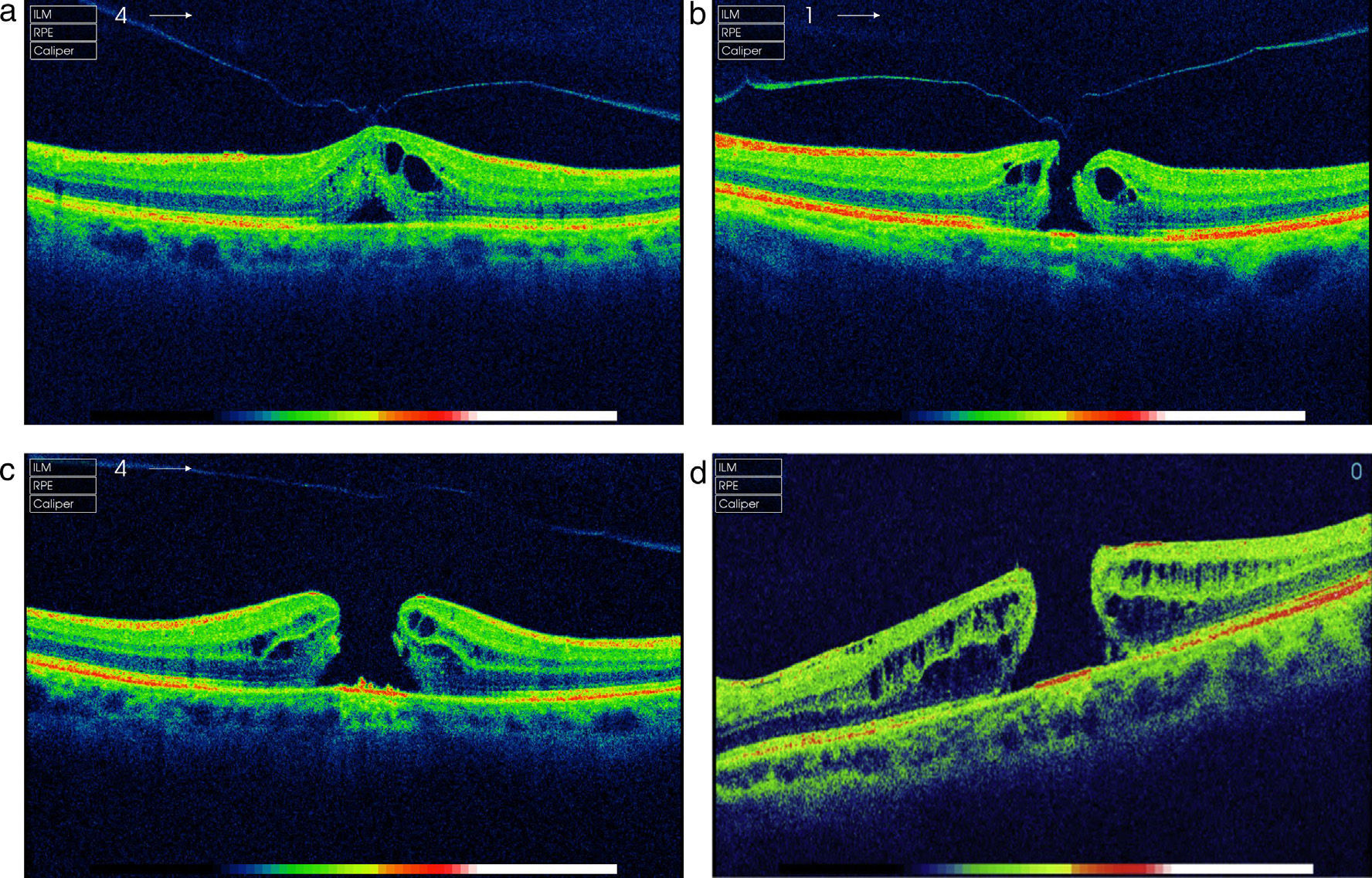
array:23 [ "pii" => "S2173579414000061" "issn" => "21735794" "doi" => "10.1016/j.oftale.2014.01.005" "estado" => "S300" "fechaPublicacion" => "2013-12-01" "aid" => "528" "copyright" => "Sociedad Española de Oftalmología" "copyrightAnyo" => "2013" "documento" => "article" "crossmark" => 0 "subdocumento" => "sco" "cita" => "Arch Soc Esp Oftalmol. 2013;88:455-7" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 1927 "formatos" => array:3 [ "EPUB" => 10 "HTML" => 1548 "PDF" => 369 ] ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S0365669113001342" "issn" => "03656691" "doi" => "10.1016/j.oftal.2013.03.007" "estado" => "S300" "fechaPublicacion" => "2013-12-01" "aid" => "528" "copyright" => "Sociedad Española de Oftalmología" "documento" => "article" "crossmark" => 0 "subdocumento" => "sco" "cita" => "Arch Soc Esp Oftalmol. 2013;88:455-7" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 4318 "formatos" => array:3 [ "EPUB" => 10 "HTML" => 3722 "PDF" => 586 ] ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Editorial</span>" "titulo" => "Tratamiento no quirúrgico de la tracción vitreomacular y del agujero macular" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "455" "paginaFinal" => "457" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Non-surgical treatment of vitreomacular traction and macular hole" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0015" "etiqueta" => "Figura 3" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr3.jpeg" "Alto" => 1895 "Ancho" => 2960 "Tamanyo" => 1459672 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall">Agujero macular. A) Estadio <span class="elsevierStyleSmallCaps">i.</span> B) Estadio <span class="elsevierStyleSmallCaps">ii.</span> C) Estadio <span class="elsevierStyleSmallCaps">iii</span>. D) Estadio <span class="elsevierStyleSmallCaps">iv</span>.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "L. Arias Barquet" "autores" => array:1 [ 0 => array:2 [ "nombre" => "L." "apellidos" => "Arias Barquet" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2173579414000061" "doi" => "10.1016/j.oftale.2014.01.005" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173579414000061?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0365669113001342?idApp=UINPBA00004N" "url" => "/03656691/0000008800000012/v2_201311281008/S0365669113001342/v2_201311281008/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2173579414000085" "issn" => "21735794" "doi" => "10.1016/j.oftale.2014.01.007" "estado" => "S300" "fechaPublicacion" => "2013-12-01" "aid" => "563" "copyright" => "Sociedad Española de Oftalmología" "documento" => "article" "crossmark" => 0 "subdocumento" => "fla" "cita" => "Arch Soc Esp Oftalmol. 2013;88:458-65" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 1168 "formatos" => array:3 [ "EPUB" => 15 "HTML" => 915 "PDF" => 238 ] ] "en" => array:12 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Original article</span>" "titulo" => "Spectrum and susceptibility of preoperative conjunctival bacteria" "tienePdf" => "en" "tieneTextoCompleto" => "en" "tieneResumen" => array:2 [ 0 => "en" 1 => "es" ] "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "458" "paginaFinal" => "465" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Espectro y susceptibilidad de las bacterias conjuntivales preoperatorias" ] ] "contieneResumen" => array:2 [ "en" => true "es" => true ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "M.E. Fernández-Rubio, T. Cuesta-Rodríguez, J.L. Urcelay-Segura, C. Cortés-Valdés" "autores" => array:4 [ 0 => array:2 [ "nombre" => "M.E." "apellidos" => "Fernández-Rubio" ] 1 => array:2 [ "nombre" => "T." "apellidos" => "Cuesta-Rodríguez" ] 2 => array:2 [ "nombre" => "J.L." "apellidos" => "Urcelay-Segura" ] 3 => array:2 [ "nombre" => "C." "apellidos" => "Cortés-Valdés" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0365669113002311" "doi" => "10.1016/j.oftal.2013.06.007" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0365669113002311?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173579414000085?idApp=UINPBA00004N" "url" => "/21735794/0000008800000012/v1_201402160014/S2173579414000085/v1_201402160014/en/main.assets" ] "en" => array:14 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Editorial</span>" "titulo" => "Non-surgical treatment of vitreomacular traction and macular hole" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "455" "paginaFinal" => "457" ] ] "autores" => array:1 [ 0 => array:3 [ "autoresLista" => "L. Arias Barquet" "autores" => array:1 [ 0 => array:3 [ "nombre" => "L." "apellidos" => "Arias Barquet" "email" => array:1 [ 0 => "luisariasbarquet@gmail.com" ] ] ] "afiliaciones" => array:1 [ 0 => array:2 [ "entidad" => "Sección de Retina Médico-Quirúrgica, Servicio de Oftalmología, Hospital Universitario de Bellvitge, Bellvitge, Barcelona, Spain" "identificador" => "aff0005" ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Tratamiento no quirúrgico de la tracción vitreomacular y del agujero macular" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 600 "Ancho" => 1000 "Tamanyo" => 225317 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Vitreomacular traction.</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">Macular hole (MA) is a significant cause of visual acuity (VA) loss in patients over 50 years in our environment. The traction by the vitreous, particularly the posterior hyaloids, on the retina surface plays a leading role in the etiopathogeny of MA.</p><p id="par0010" class="elsevierStylePara elsevierViewall">The collagen fibers that comprise the posterior vitreous are firmly joined to the macula and connecting to the internal limiting membrane by means of a sort of biological adhesive made up by proteoglycans, laminin and fibronectin.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> With aging, the vitreous gel becomes progressively liquid and vitreoretinal adherence weakens to the point that the vitreous detaches from the retina, known as posterior vitreous detachment (PVD). However, PVD may not be complete: a portion of the vitreous may remain adhered to the macular surface, which is known as vitreomacular adhesion (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>). When the traction increases due to anteroposterior or tangential stress, vitreomacular traction (VMT) takes place. VMT can be asymptomatic in the form of metamorphopsia and loss of central VA (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>). In addition, VMT can produce cystic spaces in the retina and involve the formation of MA.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a></p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><elsevierMultimedia ident="fig0010"></elsevierMultimedia><p id="par0015" class="elsevierStylePara elsevierViewall">Typically, MA is classified in 4 stages depending on partial thickness without involving the external layers (<span class="elsevierStyleSmallCaps">i</span>), full thickness with VMT (<span class="elsevierStyleSmallCaps">ii</span>), full thickness without VMT and without PVD (<span class="elsevierStyleSmallCaps">iii</span>) and full thickness without VMT and with PVD (<span class="elsevierStyleSmallCaps">iv</span>) (<a class="elsevierStyleCrossRef" href="#fig0015">Fig. 3</a>).<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a></p><elsevierMultimedia ident="fig0015"></elsevierMultimedia><p id="par0020" class="elsevierStylePara elsevierViewall">In the treatment of MA, observation is recommended with frequent supervision for stage <span class="elsevierStyleSmallCaps">i</span>, while surgery is recommended for the remaining stages. At present, recommended surgical treatment consists of microincision 25 or 23<span class="elsevierStyleHsp" style=""></span>g posterior vitrectomy, posterior hyaloids dissection, internal limiting membrane peeling and short duration gas tamponade.<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">4</span></a> Most surgeons recommend post-surgery rest in prone position during 5–7 days, which is not comfortable and not easy to comply with for older patients. Similarly, this surgery is not technically simple and is not free of complications such as endophthalmitis, retina detachment and cataracts.</p><p id="par0025" class="elsevierStylePara elsevierViewall">In recent years, enzymatic vitriolysis with drugs capable of digesting the molecules which are responsible for VMT has been tested. Clinical trials with hyaluronidase dispase and chondroitinase have been discarded due to lack of efficacy or safety.<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a> Ocriplasmin (previously known as microplasmin) is a recombinant form of human plasmine serinprotease with proteolytic activity against laminin and fibronectin, two of the main components of the vitreoretinal interface. Preclinical and clinical trials have demonstrated that ocriplasmin can induce the formation of PVD with the ensuing resolution of TVM.<a class="elsevierStyleCrossRef" href="#bib0030"><span class="elsevierStyleSup">6</span></a></p><p id="par0030" class="elsevierStylePara elsevierViewall">Recently, the results of 2 multicenter phase 3 clinical trials comparing the results of a single 125<span class="elsevierStyleHsp" style=""></span>μg injection of ocriplasmin against placebo injections in patients with symptomatic VMT have been published. Said trials included 652 eyes, 464 treated with ocriplasmin and 198 with placebo. VMT was resolved in 26.5% of cases treated with ocriplasmin against 10.1% of those treated with placebo (<span class="elsevierStyleItalic">p</span><span class="elsevierStyleHsp" style=""></span><<span class="elsevierStyleHsp" style=""></span>0.001). It must be noted that 14.6% of the cases treated with ocriplasmin and 10.6% of cases treated with placebo injection (<span class="elsevierStyleItalic">p</span><span class="elsevierStyleHsp" style=""></span><<span class="elsevierStyleHsp" style=""></span>0.001) achieved nonsurgical closure of the MA. In addition, complete PVD was observed in 13.4% of patients treated with ocriplasmin and in 3.7% of those treated with placebo (<span class="elsevierStyleItalic">p</span><span class="elsevierStyleHsp" style=""></span><<span class="elsevierStyleHsp" style=""></span>0.001). The ocriplasmin injection was demonstrated to be safe, without significant adverse effects being observed.<a class="elsevierStyleCrossRef" href="#bib0035"><span class="elsevierStyleSup">7</span></a></p><p id="par0035" class="elsevierStylePara elsevierViewall">Said results open up new options in the treatment of symptomatic VMT and MA. For the first time a pharmacological treatment can make vitrectomy unnecessary. Even though said surgery has very good results for treating said macular disorder, the above commented complications are a cause of concern. In addition, the repercussions for patients and the health system of resolving a disease with a complex surgical procedure or an intravitreal injection, which can be carried out in a clean outpatient practice, are completely different. On the other hand, this will enable ophthalmologists with training in medical retina but with little experience in surgical retina to treat these patients who, until now, must be referred to a hospital with retina and vitreous surgery. It is clear that this will facilitate faster treatments after diagnosis, which would have a positive impact on the end results. As in other maculopathies, early diagnosis and treatment are crucial to obtain good results to preserve visual function as much as possible.</p><p id="par0040" class="elsevierStylePara elsevierViewall">Initially, intravitreal ocriplasmin (JETREA<span class="elsevierStyleSup">®</span>, Alcon Laboratories, Fort Worth, TX, USA) shall be used in a primary VMT cases, including small size macular holes (<400<span class="elsevierStyleHsp" style=""></span>μm). However, its application will also be researched for VMT cases that are concurrent with other diseases such as exudative age-related macular degeneration (ARMD), diabetic retinopathy and pathological myopia. It seems that, in what concerns exudative ARMD, there is evidence that in some cases VMT could prevent the resolution of the presence of intraretinal or subretinal fluid after the injection of anti-VEGF (vascular endothelial growth factor) drugs.<a class="elsevierStyleCrossRef" href="#bib0040"><span class="elsevierStyleSup">8</span></a></p><p id="par0045" class="elsevierStylePara elsevierViewall">Due to recent developments in research and the efforts of the pharmaceutical industry, ophthalmologists are able to increase the therapeutical range and accordingly the possibility of providing more and better services to our patients.</p></span>" "pdfFichero" => "main.pdf" "tienePdf" => true "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Arias Barquet L. Tratamiento no quirúrgico de la tracción vitreomacular y del agujero macular. Arch Soc Esp Oftalmol. 2013;88:455–457.</p>" ] ] "multimedia" => array:3 [ 0 => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 604 "Ancho" => 997 "Tamanyo" => 150101 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Vitreomacular adhesion.</p>" ] ] 1 => array:7 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 600 "Ancho" => 1000 "Tamanyo" => 225317 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Vitreomacular traction.</p>" ] ] 2 => array:7 [ "identificador" => "fig0015" "etiqueta" => "Fig. 3" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr3.jpeg" "Alto" => 1137 "Ancho" => 1776 "Tamanyo" => 672276 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall">Macular hole: (A) stage <span class="elsevierStyleSmallCaps">i,</span> (B) stage <span class="elsevierStyleSmallCaps">ii,</span> (C) stage <span class="elsevierStyleSmallCaps">iii</span> and (D) stage <span class="elsevierStyleSmallCaps">iv</span>.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:8 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Structural macromolecules and supramolecular organisation of the vitreous gel" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "P.N. Bishop" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Prog Retin Eye Res" "fecha" => "2000" "volumen" => "19" "paginaInicial" => "323" "paginaFinal" => "344" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/10749380" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Age-related differences in the human vitreoretinal interface" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "J. Sebag" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Arch Ophthalmol" "fecha" => "1991" "volumen" => "109" "paginaInicial" => "966" "paginaFinal" => "971" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/2064577" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Stereoscopic atlas of macular diseases: diagnosis and treatment" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "J.D. Gass" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Libro" => array:4 [ "edicion" => "4th ed." "fecha" => "1997" "editorial" => "Mosby" "editorialLocalizacion" => "St. Louis" ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:1 [ "titulo" => "Manejo del agujero, macular. Guías de práctica clínica de la Sociedad Española de Retina y Vítreo" ] ] "host" => array:1 [ 0 => array:1 [ "Libro" => array:3 [ "fecha" => "2011" "editorial" => "Sociedad Española de Retina y Vítreo" "editorialLocalizacion" => "Madrid" ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Enzymatic vitreolysis" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "F. López-López" 1 => "M. Rodríguez-Blanco" 2 => "F. Gómez-Ulla" 3 => "J. Marticorena" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Curr Diabetes Rev" "fecha" => "2009" "volumen" => "5" "paginaInicial" => "57" "paginaFinal" => "62" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/19199900" "web" => "Medline" ] ] ] ] ] ] ] ] 5 => array:3 [ "identificador" => "bib0030" "etiqueta" => "6" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Posterior vitreous detachment induced by microplasmin" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "A. Gandorfer" 1 => "M. Rohleder" 2 => "C. Sethi" 3 => "D. Eckle" 4 => "U. Welge-Lüssen" 5 => "A. Kampik" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Invest Ophthalmol Vis Sci" "fecha" => "2004" "volumen" => "45" "paginaInicial" => "641" "paginaFinal" => "647" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/14744909" "web" => "Medline" ] ] ] ] ] ] ] ] 6 => array:3 [ "identificador" => "bib0035" "etiqueta" => "7" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Enzymaticvitreolysis with ocriplasmin for vitreomacular traction and macular holes" "autores" => array:1 [ 0 => array:3 [ "colaboracion" => "for the MIVI-TRUST Study Group" "etal" => true "autores" => array:6 [ 0 => "P. Stalmans" 1 => "M.S. Benz" 2 => "A. Gandorfer" 3 => "A. Kampik" 4 => "A. Girach" 5 => "S. Pakola" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1056/NEJMoa1110823" "Revista" => array:6 [ "tituloSerie" => "N Engl J Med" "fecha" => "2012" "volumen" => "367" "paginaInicial" => "606" "paginaFinal" => "615" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/22894573" "web" => "Medline" ] ] ] ] ] ] ] ] 7 => array:3 [ "identificador" => "bib0040" "etiqueta" => "8" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Vitreomacular adhesion in active and end-stage age-related macular degeneration" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "C.D. Robison" 1 => "I. Krebs" 2 => "S. Binder" 3 => "I.A. Barbazetto" 4 => "A.I. Kotsolis" 5 => "L.A. Yannuzzi" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.ajo.2009.01.014" "Revista" => array:6 [ "tituloSerie" => "Am J Ophthalmol" "fecha" => "2009" "volumen" => "148" "paginaInicial" => "79" "paginaFinal" => "82" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/19327744" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/21735794/0000008800000012/v1_201402160014/S2173579414000061/v1_201402160014/en/main.assets" "Apartado" => array:4 [ "identificador" => "5814" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Editorial" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/21735794/0000008800000012/v1_201402160014/S2173579414000061/v1_201402160014/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2173579414000061?idApp=UINPBA00004N" ]
Journal Information
Vol. 88. Issue 12.
Pages 455-457 (December 2013)
Share
Download PDF
More article options
Vol. 88. Issue 12.
Pages 455-457 (December 2013)
Editorial
Non-surgical treatment of vitreomacular traction and macular hole
Tratamiento no quirúrgico de la tracción vitreomacular y del agujero macular
Visits
1918
L. Arias Barquet
Sección de Retina Médico-Quirúrgica, Servicio de Oftalmología, Hospital Universitario de Bellvitge, Bellvitge, Barcelona, Spain
This item has received
Article information
These are the options to access the full texts of the publication Archivos de la Sociedad Española de Oftalmología (English Edition)
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail