array:23 [ "pii" => "S2387020621005362" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.09.018" "estado" => "S300" "fechaPublicacion" => "2021-11-12" "aid" => "5466" "copyright" => "Elsevier España, S.L.U.. All rights reserved" "copyrightAnyo" => "2020" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:455-6" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "itemSiguiente" => array:19 [ "pii" => "S2387020621005386" "issn" => "23870206" "doi" => "10.1016/j.medcle.2021.10.001" "estado" => "S300" "fechaPublicacion" => "2021-11-12" "aid" => "5457" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:456-7" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:10 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "<span class="elsevierStyleItalic">KCNQ1</span> gene mutation and epilepsy in patient with long QT syndrome" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "456" "paginaFinal" => "457" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Mutación en el gen <span class="elsevierStyleItalic">KCNQ1</span> y epilepsia en paciente con síndrome de QT largo" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Macarena García Gozalo, Ignacio Bermejo Arnedo, Paula de Vera McMullan" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Macarena" "apellidos" => "García Gozalo" ] 1 => array:2 [ "nombre" => "Ignacio" "apellidos" => "Bermejo Arnedo" ] 2 => array:2 [ "nombre" => "Paula" "apellidos" => "de Vera McMullan" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0025775320307399" "doi" => "10.1016/j.medcli.2020.09.008" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775320307399?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621005386?idApp=UINPBA00004N" "url" => "/23870206/0000015700000009/v1_202111060623/S2387020621005386/v1_202111060623/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2387020621005349" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.09.016" "estado" => "S300" "fechaPublicacion" => "2021-11-12" "aid" => "5452" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:454-5" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:10 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Miliary tuberculosis complicated with acute respiratory distress syndrome and hemophagocytic lymphohistiocytosis syndrome in an immunocompetent patient" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "454" "paginaFinal" => "455" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Tuberculosis miliar complicada con síndrome de distrés respiratorio y linfohistiocitosis hemofagocítica en un paciente inmunocompetente" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Antonio Rosales-Castillo, Miguel Ángel López-Ruz" "autores" => array:2 [ 0 => array:2 [ "nombre" => "Antonio" "apellidos" => "Rosales-Castillo" ] 1 => array:2 [ "nombre" => "Miguel Ángel" "apellidos" => "López-Ruz" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S002577532030734X" "doi" => "10.1016/j.medcli.2020.09.007" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S002577532030734X?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621005349?idApp=UINPBA00004N" "url" => "/23870206/0000015700000009/v1_202111060623/S2387020621005349/v1_202111060623/en/main.assets" ] "en" => array:15 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Hereditary multiple paraganglioma" "tieneTextoCompleto" => true "saludo" => "Dear Editor:" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "455" "paginaFinal" => "456" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Antonio Rosales-Castillo, Antonio Bustos-Merlo, Laura Gallo Padilla" "autores" => array:3 [ 0 => array:4 [ "nombre" => "Antonio" "apellidos" => "Rosales-Castillo" "email" => array:1 [ 0 => "anrocas90@hotmail.com" ] "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "*" "identificador" => "cor0005" ] ] ] 1 => array:2 [ "nombre" => "Antonio" "apellidos" => "Bustos-Merlo" ] 2 => array:2 [ "nombre" => "Laura" "apellidos" => "Gallo Padilla" ] ] "afiliaciones" => array:1 [ 0 => array:2 [ "entidad" => "Servicio de Medicina Interna, Hospital Universitario Virgen de las Nieves, Granada, Spain" "identificador" => "aff0005" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Paraganglioma múltiple hereditario" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 823 "Ancho" => 1255 "Tamanyo" => 92619 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">PET-DOPA scan images revealing bilateral contrast uptake at the carotid and paraaortic levels.</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">Paragangliomas are highly vascularized neoplasms arising from sympathetic (such as the sympathetic chain) or parasympathetic (such as the carotid body, the glomus tympanicum, the glomus <span class="elsevierStyleItalic">jugulare</span>, or the glomus <span class="elsevierStyleItalic">intravagale</span>) tissue cells.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> Between 25% and 33% of cases are associated with hereditary multiple paragangliomatosis. This condition frequently lacks initial clinical manifestations, and the suspected diagnosis is reached based on the patient’s levels of catecholamines and metanephrines, as well as their radiological findings, and subsequently confirmed by means of a bone scintigraphy and a histopathology exam.</p><p id="par0010" class="elsevierStylePara elsevierViewall">In this paper we present the case of a young male with a diagnosis of multiple paragangliomas in which a genetic hereditary etiology was confirmed.</p><p id="par0015" class="elsevierStylePara elsevierViewall">The patient is a 28-year-old male, without a remarkable personal medical history, who presented with a two-week history of upper hemiabdominal pain associated with constipation and interrupted sleep, but not with intestinal rhythm disorders, pathological products, or food intake. He denied fever, hyporexia, or weight loss, although he did complain of persistent asthenia. He reported no respiratory, genitourinary, cutaneous, or articular symptoms either. A physical examination revealed a tendency toward arterial hypertension (143/97 mmHg) and a heart rate of 88 bpm. A 1 × 1-cm, rubbery adenopathy was detected in the left laterocervical region, without pain on palpation nor adhesion to the deep tissue planes. Both a cardiorespiratory auscultation and an abdominal examination revealed normal findings. His legs had palpable pedal pulses an no oedemas. A hematometry and blood biochemistry revealed no alterations, as did a systemic urinalysis. A chest X-ray showed a normal silhouette. However, an abdominal ultrasound revealed a solid, hypoechogenic, vascularized, 2-cm left paraaortic nodular image. Given this finding, the patient was admitted to the clinic in order to complete further screening tests.</p><p id="par0020" class="elsevierStylePara elsevierViewall">Ancillary tests were also performed, including serology tests (human immunodeficiency virus [HIV], hepatitis B virus [HBV], hepatitis C virus [HCV], <span class="elsevierStyleItalic">Coxiella</span> spp., <span class="elsevierStyleItalic">Mycoplasma</span> spp., and <span class="elsevierStyleItalic">Treponema pallidum</span>), a protein panel, and an immunoglobulins assay, all yielding normal results. A 24-h urinalysis revealed elevated noradrenaline (425 µg/24 h) and normetanephrine (1220 µg/24 h) levels. A subsequent abdominal and cervical computed tomography scan confirmed the ultrasound findings, also detecting a probable bilateral carotid paraganglioma. Given these radiological findings, a positron emission tomography scan with fluorodopa (PET-DOPA) was also requested (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>). The images of this study revealed bilateral homogenous contrast uptake both at a carotid and paraaortic level, which suggested the existence of multiple paragangliomas. Given the suspected diagnosis of multiple paraganglioma, the case was discussed with a multidisciplinary committee, who jointly agreed to initially excise the retroperitoneal tumor and request the conduct of genetic testing. A pathology study of the specimen obtained during the surgical procedure revealed positivity for neuron-specific enolase and chromogranin, both of which are findings compatible with paraganglioma. In addition, the genetic study of mutations related to familial paraganglioma yielded a positive result for variant <span class="elsevierStyleItalic">c.337_340delGACT (p.Asp113Mets*21)</span>, which is classified as pathogenic in heterozygosis in the <span class="elsevierStyleItalic">SDHD</span> gene and of autosomal dominant inheritance.</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0025" class="elsevierStylePara elsevierViewall">Paragangliomas are rare, neuroendocrine neoplasms derived from extra-adrenal autonomic ganglia and histologically indistinguishable from adrenal pheochromocytomas. Paragangliomas derived from sympathetic tissue are frequently catecholamine-secreting and located at a paravertebral level, whereas those derived from parasympathetic tissue are usually non-functional and located at the glossopharyngeal and vagal levels. The clinical manifestations of catecholamine-secreting paragangliomas are similar to those of pheochromocytomas; i.e., hypertension, headache, profuse sweating, and heart palpitations. Although most cases are sporadic, up to one-third of them are associated with an inherited syndrome. A familial association should be suspected in cases of early onset, a multiple or bilateral presentation, and sympathetic paragangliomas.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a></p><p id="par0030" class="elsevierStylePara elsevierViewall">In addition, there are four particular syndromes associated with an increased susceptibility to the onset of paragangliomas: multiple endocrine neoplasia (MEN) types 2A and 2B, neurofibromatosis type 1, the von Hippel-Lindau syndrome, and the Carney complex, all of which are linked to germline mutations in the genes classically recognized as associated with this condition ( i.e., <span class="elsevierStyleItalic">RET, VHL, NF1, SDHB, SDHC,</span> and <span class="elsevierStyleItalic">SDHD)</span><a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> or in newly identified ones ( i.e., <span class="elsevierStyleItalic">SDHA, SDHAF2, TMEM127, MAX, PDH1,</span> and <span class="elsevierStyleItalic">HIF1alpha</span>).<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">4</span></a> On average, 30% of head and neck paragangliomas are associated with germline mutations in one of the <span class="elsevierStyleItalic">SDH</span> subunit genes (most commonly <span class="elsevierStyleItalic">SDHD</span>). The PGL1 syndrome (<span class="elsevierStyleItalic">SDHD</span>), with an autosomal dominant inheritance pattern, is characterized by the presence of multifocal paragangliomas that do not release catecholamines into the bloodstream and have a very low risk of malignancy (approximately 4%).<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a></p></span>" "pdfFichero" => "main.pdf" "tienePdf" => true "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Rosales-Castillo A, Bustos-Merlo A, Gallo Padilla L. Paraganglioma múltiple hereditario. Med Clin (Barc). 2021;157:455–456.</p>" ] ] "multimedia" => array:1 [ 0 => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 823 "Ancho" => 1255 "Tamanyo" => 92619 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">PET-DOPA scan images revealing bilateral contrast uptake at the carotid and paraaortic levels.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:5 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Phaeochromocytomas and functional paragangliomas: Clinical management" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "P.F. Plouin" 1 => "L. Amar" 2 => "C. Lepoutre" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.beem.2010.10.002" "Revista" => array:6 [ "tituloSerie" => "Best Pract Res Clin Endocrinol Metab" "fecha" => "2010" "volumen" => "24" "paginaInicial" => "933" "paginaFinal" => "941" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/21115162" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Clinically guided genetic screening in a large cohort of italian patients with pheochromocytomas and/or functional or nonfunctional paragangliomas" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "M. Mannelli" 1 => "M. Castellano" 2 => "F. Schiavi" 3 => "S. Filetti" 4 => "M. Giacchè" 5 => "L. Mori" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1210/jc.2008-2419" "Revista" => array:6 [ "tituloSerie" => "J Clin Endocrinol Metab" "fecha" => "2009" "volumen" => "94" "paginaInicial" => "1541" "paginaFinal" => "1547" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/19223516" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Hereditary syndromes in neuroendocrine tumors" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "M.A. Lewis" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s11864-019-0692-8" "Revista" => array:6 [ "tituloSerie" => "Curr Treat Options Oncol" "fecha" => "2020" "volumen" => "21" "paginaInicial" => "1" "paginaFinal" => "8" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/31927649" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Malignant Intrarenal/renal pelvis paraganglioma with co-occurring SDHB and ATRX mutations" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "T. Irwin" 1 => "E.Q. Konnick" 2 => "M.S. Tretiakova" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s12022-019-09594-1" "Revista" => array:6 [ "tituloSerie" => "Endocr Pathol." "fecha" => "2019" "volumen" => "30" "paginaInicial" => "270" "paginaFinal" => "275" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/31705439" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "15 YEARS OF PARAGANGLIOMA: clinical manifestations of paraganglioma syndromes types 1-5" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "D.E. Benn" 1 => "B.G. Robinson" 2 => "R.J. Clifton-Bligh" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Endocr Relat Cancer" "fecha" => "2015" "volumen" => "22" "paginaInicial" => "91" "paginaFinal" => "103" ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/23870206/0000015700000009/v1_202111060623/S2387020621005362/v1_202111060623/en/main.assets" "Apartado" => array:4 [ "identificador" => "43309" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Letters to the Editor" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/23870206/0000015700000009/v1_202111060623/S2387020621005362/v1_202111060623/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621005362?idApp=UINPBA00004N" ]
Journal Information
Letter to the Editor
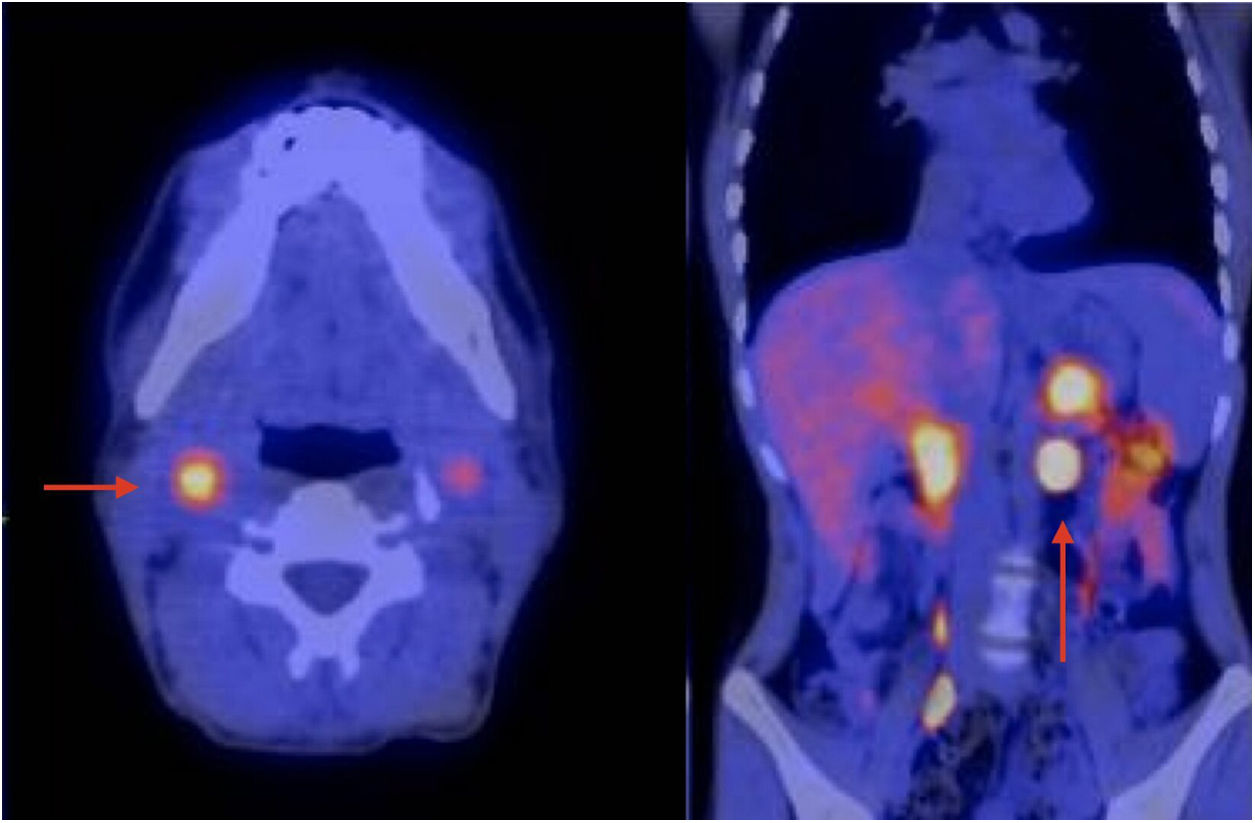
Hereditary multiple paraganglioma
Paraganglioma múltiple hereditario
Antonio Rosales-Castillo
, Antonio Bustos-Merlo, Laura Gallo Padilla
Corresponding author
Servicio de Medicina Interna, Hospital Universitario Virgen de las Nieves, Granada, Spain
Article information
These are the options to access the full texts of the publication Medicina Clínica (English Edition)
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail