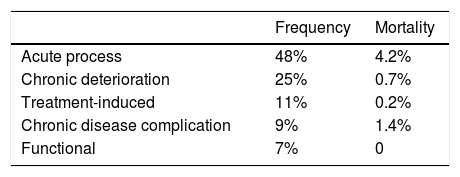
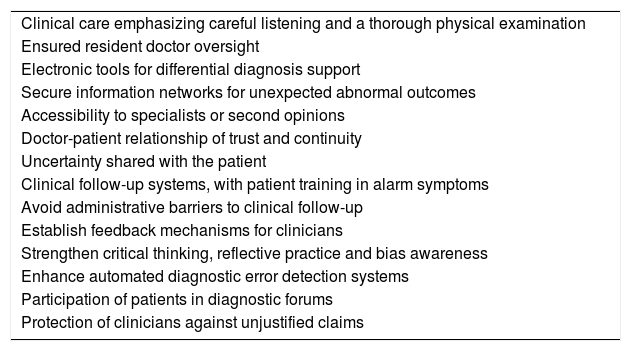
array:24 [ "pii" => "S2387020619303997" "issn" => "23870206" "doi" => "10.1016/j.medcle.2019.06.012" "estado" => "S300" "fechaPublicacion" => "2019-10-25" "aid" => "4915" "copyright" => "Elsevier España, S.L.U.. All rights reserved" "copyrightAnyo" => "2019" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Med Clin. 2019;153:332-5" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 2 "HTML" => 2 ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S0025775319304361" "issn" => "00257753" "doi" => "10.1016/j.medcli.2019.06.001" "estado" => "S300" "fechaPublicacion" => "2019-10-25" "aid" => "4915" "copyright" => "Elsevier España, S.L.U." "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Med Clin. 2019;153:332-5" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 14 "formatos" => array:2 [ "HTML" => 7 "PDF" => 7 ] ] "es" => array:10 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Artículo especial</span>" "titulo" => "Mejorar en seguridad diagnóstica: la asignatura pendiente" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "332" "paginaFinal" => "335" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "To improve in diagnostic safety: The pending subject" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Pere Tudela, Carme Forcada, Anna Carreres, Mònica Ballester" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Pere" "apellidos" => "Tudela" ] 1 => array:2 [ "nombre" => "Carme" "apellidos" => "Forcada" ] 2 => array:2 [ "nombre" => "Anna" "apellidos" => "Carreres" ] 3 => array:2 [ "nombre" => "Mònica" "apellidos" => "Ballester" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2387020619303997" "doi" => "10.1016/j.medcle.2019.06.012" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020619303997?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775319304361?idApp=UINPBA00004N" "url" => "/00257753/0000015300000008/v2_201911121014/S0025775319304361/v2_201911121014/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2387020619303742" "issn" => "23870206" "doi" => "10.1016/j.medcle.2018.08.019" "estado" => "S300" "fechaPublicacion" => "2019-10-25" "aid" => "4635" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Med Clin. 2019;153:336-7" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 2 "HTML" => 2 ] "en" => array:10 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Scientific letter</span>" "titulo" => "Osteogenesis imperfecta caused by <span class="elsevierStyleItalic">COL1A1</span>, <span class="elsevierStyleItalic">CRTAP</span> and <span class="elsevierStyleItalic">LEPRE1</span> mutations. Report of 2 cases" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "336" "paginaFinal" => "337" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Osteogénesis imperfecta causada por mutación en los genes <span class="elsevierStyleItalic">COL1A1, CRTAP</span> y <span class="elsevierStyleItalic">LEPRE1</span>. Estudio de 2 casos" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Pilar Caudevilla Lafuente, Silvia Izquierdo-Álvarez, José Ignacio Labarta Aizpún" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Pilar" "apellidos" => "Caudevilla Lafuente" ] 1 => array:2 [ "nombre" => "Silvia" "apellidos" => "Izquierdo-Álvarez" ] 2 => array:2 [ "nombre" => "José Ignacio" "apellidos" => "Labarta Aizpún" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0025775318305396" "doi" => "10.1016/j.medcli.2018.08.017" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775318305396?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020619303742?idApp=UINPBA00004N" "url" => "/23870206/0000015300000008/v1_201910190847/S2387020619303742/v1_201910190847/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2387020619304152" "issn" => "23870206" "doi" => "10.1016/j.medcle.2019.05.005" "estado" => "S300" "fechaPublicacion" => "2019-10-25" "aid" => "4918" "copyright" => "Elsevier España, S.L.U." "documento" => "article" "crossmark" => 1 "subdocumento" => "rev" "cita" => "Med Clin. 2019;153:326-31" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:2 [ "total" => 1 "HTML" => 1 ] "en" => array:12 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Review</span>" "titulo" => "The role of aspirin as antiaggregant therapy in primary prevention. An update" "tienePdf" => "en" "tieneTextoCompleto" => "en" "tieneResumen" => array:2 [ 0 => "en" 1 => "es" ] "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "326" "paginaFinal" => "331" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Papel de la Aspirina® como tratamiento antiagregante en prevención primaria. Puesta al día" ] ] "contieneResumen" => array:2 [ "en" => true "es" => true ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Nicolás Jiménez-García, Javier de la Torre Lima, Javier García Alegría" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Nicolás" "apellidos" => "Jiménez-García" ] 1 => array:2 [ "nombre" => "Javier" "apellidos" => "de la Torre Lima" ] 2 => array:2 [ "nombre" => "Javier" "apellidos" => "García Alegría" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0025775319304397" "doi" => "10.1016/j.medcli.2019.05.024" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775319304397?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020619304152?idApp=UINPBA00004N" "url" => "/23870206/0000015300000008/v1_201910190847/S2387020619304152/v1_201910190847/en/main.assets" ] "en" => array:16 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Special article</span>" "titulo" => "To improve in diagnostic safety: The pending subject" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "332" "paginaFinal" => "335" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Pere Tudela, Carme Forcada, Anna Carreres, Mònica Ballester" "autores" => array:4 [ 0 => array:4 [ "nombre" => "Pere" "apellidos" => "Tudela" "email" => array:1 [ 0 => "ptudela.germanstrias@gencat.cat" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "*" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Carme" "apellidos" => "Forcada" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 2 => array:3 [ "nombre" => "Anna" "apellidos" => "Carreres" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 3 => array:3 [ "nombre" => "Mònica" "apellidos" => "Ballester" "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] ] "afiliaciones" => array:2 [ 0 => array:3 [ "entidad" => "Unidad de Observación y Corta Estancia, Servicio de Urgencias, Dirección de Calidad, Hospital Universitario Germans Trias i Pujol, Badalona, Barcelona, Spain" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Centro de Atención Primaria, Vilassar de Dalt, Barcelona, Spain" "etiqueta" => "b" "identificador" => "aff0010" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Mejorar en seguridad diagnóstica: la asignatura pendiente" ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">In recent years, medical errors and their consequences have been widely acknowledged, prompting its study and the issuing of preventive recommendations. But this work has focused mainly on general aspects of care, such as patient identification or communication, technical clinical procedures or pharmacological and surgical treatments. Diagnostic errors (DE) have taken a back seat even though they were already evident from the first studies on adverse events, constantly appear in the media and the most recent estimates show that they are not rare or occasional. Quite the contrary, they can reach around 10% of cases, pose a high risk of harm to the patient and represent one of the first causes of medical-legal claims.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1–6</span></a> That is why improving diagnostic safety and minimizing the possibility of error in this regard is so important. This purpose is common to all healthcare settings, but it is especially important in hospital emergency departments (ED), where diagnostic guidance is essential to determine the need for complementary examinations, hospital admission and specific treatment, sometimes time-effective.<a class="elsevierStyleCrossRef" href="#bib0030"><span class="elsevierStyleSup">6</span></a></p><p id="par0010" class="elsevierStylePara elsevierViewall">On the other hand, trying to avoid the risk of DE, along with other different factors, a tendency has been developed to carry out numerous complementary examinations, which sometimes only result in overdiagnosis. It is necessary to balance and minimize these two risks, which could be likened to the two sides of the same coin. Recently, some essential recommendations have been defined in the field of diagnosis, which may mean a step forward in this regard and that may lay the foundations for a safer diagnostic process.</p><p id="par0015" class="elsevierStylePara elsevierViewall">Likewise, there is a specific problem, that of patients who seek medical care for poorly defined reasons, this entails a high-risk scenario for DE, especially in ED. Different studies dealing with this subject have contributed knowledge and have become an element of support for clinicians.</p><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Key elements in diagnostic improvement</span><p id="par0020" class="elsevierStylePara elsevierViewall">The experience accumulated in recent times has made it possible to draw some conclusions that allow us to indicate generic recommendations. The Harvard Medical School has recently standardized these concepts,<a class="elsevierStyleCrossRef" href="#bib0035"><span class="elsevierStyleSup">7</span></a> which should be a point of reference and always be considered by clinicians in their daily practice:<ul class="elsevierStyleList" id="lis0005"><li class="elsevierStyleListItem" id="lsti0005"><span class="elsevierStyleLabel">–</span><p id="par0025" class="elsevierStylePara elsevierViewall">Personalized clinical care, emphasizing careful listening and a thorough physical examination needs to be restored.<a class="elsevierStyleCrossRef" href="#bib0040"><span class="elsevierStyleSup">8</span></a> All this, together with a patient-shared reflection, should help decision making regarding complementary examinations. It is about avoiding the devaluation of clinical impression, overvaluing the results of lab or imaging data.</p></li><li class="elsevierStyleListItem" id="lsti0010"><span class="elsevierStyleLabel">–</span><p id="par0030" class="elsevierStylePara elsevierViewall">An open awareness of the existence of a certain degree of uncertainty should be established. In this sense, the complexity of the biological systems and the limitation of examination techniques should lead to a more modest and reflective clinical practice, expressed and shared with the patient.</p></li><li class="elsevierStyleListItem" id="lsti0015"><span class="elsevierStyleLabel">–</span><p id="par0035" class="elsevierStylePara elsevierViewall">In some situations, it may be necessary to reconsider the symptoms, given the possibility that some of them are transient or correspond more to the psychosomatic sphere of the patient. The two extremes, that is, over-examination and the stigmatization of the patient, should be avoided, in some cases raising personal support measures, which may be more effective.</p></li><li class="elsevierStyleListItem" id="lsti0020"><span class="elsevierStyleLabel">–</span><p id="par0040" class="elsevierStylePara elsevierViewall">In the doctor-patient relationship it is essential to establish a bond of trust and continuity, ensuring clinical information and avoiding defensive attitudes on the part of the clinician.</p></li><li class="elsevierStyleListItem" id="lsti0025"><span class="elsevierStyleLabel">–</span><p id="par0045" class="elsevierStylePara elsevierViewall">Dedication of sufficient time to the patient is a key aspect to consider. Quality clinical care requires time to listen, examine and inform, adapting to the psychosocial domain of the person.</p></li><li class="elsevierStyleListItem" id="lsti0030"><span class="elsevierStyleLabel">–</span><p id="par0050" class="elsevierStylePara elsevierViewall">Linking the diagnostic process with therapeutic options is essential. The need for an accurate diagnosis is unquestionable in situations with effective, specific or emergency treatments. In contrast, for conditions without effective treatment, the diagnostic search may be unjustified.</p></li><li class="elsevierStyleListItem" id="lsti0035"><span class="elsevierStyleLabel">–</span><p id="par0055" class="elsevierStylePara elsevierViewall">The indication of complementary examinations should be rationalized. In order to weigh their potential benefit, their usefulness should be analysed, selecting and sequencing them appropriately. In the same way, its risks and possible side effects should be considered, of which many of them are not exempt.</p></li><li class="elsevierStyleListItem" id="lsti0040"><span class="elsevierStyleLabel">–</span><p id="par0060" class="elsevierStylePara elsevierViewall">Collaborative work between ED, other specialists and Primary Care professionals can rationalize the indication of complementary examinations, while speeding up the preferred diagnostic processes.</p></li><li class="elsevierStyleListItem" id="lsti0045"><span class="elsevierStyleLabel">–</span><p id="par0065" class="elsevierStylePara elsevierViewall">From a more systemic point of view, the healthcare model, as well as the media, should contemplate a dissemination work regarding safety and limitations in diagnostic tests performance. What has come to be called <span class="elsevierStyleItalic">health literacy.</span><a class="elsevierStyleCrossRef" href="#bib0040"><span class="elsevierStyleSup">8</span></a> It is necessary to clarify concepts such as false positives and negatives, or doubtful benefits in some early diagnosis cases. This may be of special significance in the field of cancer diagnosis, such as prostate or thyroid cases.<a class="elsevierStyleCrossRef" href="#bib0045"><span class="elsevierStyleSup">9</span></a></p></li><li class="elsevierStyleListItem" id="lsti0050"><span class="elsevierStyleLabel">–</span><p id="par0070" class="elsevierStylePara elsevierViewall">incorporating the knowledge provided by the analysis of previous DE is increasingly being considered. In the near future this could mean designing safety systems for certain clinical situations of presumable risk.</p></li></ul></p></span><span id="sec0010" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0010">The problem of overdiagnosis</span><p id="par0075" class="elsevierStylePara elsevierViewall">The concept of overdiagnosis, although difficult to define, involves turning people into patients unnecessarily, identifying problems that probably would not cause harm. In short, causing more harm than benefit. It consists in carrying out an excess assessment of asymptomatic individuals or requesting a disproportionate number of examinations in patients with some symptoms. It can be determined by two mechanisms: over-detection or the extended definition of a disease.<a class="elsevierStyleCrossRefs" href="#bib0045"><span class="elsevierStyleSup">9,10</span></a></p><p id="par0080" class="elsevierStylePara elsevierViewall">Over-detection refers to the finding of abnormalities that, most probably, will not progress, will not cause damage or will resolve spontaneously. It is what has come to be called “incidentaloma”, typically in imaging scans, indicated for unrelated reasons. Adrenal, prostatic, thyroid, mammary or pulmonary nodes, as well as aortic aneurysms or meningiomas, are some of them. The problem lies in the eventual difficulty in distinguishing which of them are the ones that will really give clinical problems. In many cases it is not clear that their casual detection can improve the real prognosis of patients.</p><p id="par0085" class="elsevierStylePara elsevierViewall">An extended definition is established by modification of the normal thresholds. This is the case of vascular risk factors (blood pressure, blood glucose, lipids), which can be contemplated in a more or less interventionist manner depending on which are the limits of normality, or of negative psychological experiences (insomnia, sadness, difficulty of attention) that can be considered simply transitory in the course of life or debilitating and therefore candidates for specific treatment. These threshold modifications logically have a direct impact on the estimation of disease prevalence (which, in turn, can stimulate overdiagnosis) and the number of treatments indicated.</p><p id="par0090" class="elsevierStylePara elsevierViewall">The point is that all this entails zero or little benefit for the patient, while it can cause non-negligible medical complications, together with significant psychological, social or economic inconveniences.</p></span><span id="sec0015" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0015">The challenge of patients who seek medical attention for poorly defined reasons</span><p id="par0095" class="elsevierStylePara elsevierViewall">A particular situation is that of patients who seek medical attention for poorly defined reasons, without a predominant symptom that we can interpret as the “guiding symptom”. They usually present a general malaise, in which different combinations of some symptoms converge, such as a feeling of weakness or fatigue, instability, functional decline or poorly located erratic pain. The patient or family members fail to be more specific despite the clinician's efforts to enhance history-taking. The typical profile is that of an elderly patient with significant comorbidity and polypharmacy, sometimes with neurological impairments and often institutionalized. They can account for 5–20% of patients who seek medical attention in ED, usually with prolonged stays in them.<a class="elsevierStyleCrossRefs" href="#bib0055"><span class="elsevierStyleSup">11,12</span></a></p><p id="par0100" class="elsevierStylePara elsevierViewall">A very high DE index has been estimated in this group; in the study by Peng et al.<a class="elsevierStyleCrossRef" href="#bib0065"><span class="elsevierStyleSup">13</span></a> only 46% had a correct diagnosis. The most common diagnostic errors were functional decline, depression or anxiety, poisoning, heart failure and urinary tract infection. In the 30-day follow-up, a serious disease was observed in 59% and a mortality of 6–20%.<a class="elsevierStyleCrossRefs" href="#bib0055"><span class="elsevierStyleSup">11,12</span></a> Likewise, among hospital readmissions, it has been estimated that 12% corresponded to a first admission due to a poorly defined reason.<a class="elsevierStyleCrossRef" href="#bib0070"><span class="elsevierStyleSup">14</span></a> 65% of the cases had a more specific reason in the second episode. This suggests that they were not adequately evaluated in the first admission, that their high comorbidity made a successful diagnosis difficult or that progression clarified the symptomatology.</p><p id="par0105" class="elsevierStylePara elsevierViewall">Malinovska et al.<a class="elsevierStyleCrossRef" href="#bib0075"><span class="elsevierStyleSup">15</span></a> categorized these patients into 5 subgroups according to their frequency and mortality (<a class="elsevierStyleCrossRef" href="#tbl0005">Table 1</a>). The problem lies in the fact that, while in the ED, there are care protocols for specific consultation reasons (chest, abdominal pain, fever, headache, among others), there are generally no guidelines for patients with poorly defined reasons. The aim should be having the ability to discriminate, from <span class="elsevierStyleItalic">triage</span>, which of these patients could be serious and have a bad prognosis, to prioritize them and avoid the risk of a delay in care.</p><elsevierMultimedia ident="tbl0005"></elsevierMultimedia></span><span id="sec0020" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0020">Future expectations</span><p id="par0110" class="elsevierStylePara elsevierViewall">It is clear that improving diagnostic safety is not easy, among other reasons because the same diagnostic process is very complex; tt is dynamic over time, implies uncertainty, is conditioned by aspects of communication and by multiple health system factors. On the other hand, from a scientific point of view, there are also numerous difficulties, experts raise important doubts and controversies both in the definitions of DE, as in the measuring tools.<a class="elsevierStyleCrossRef" href="#bib0080"><span class="elsevierStyleSup">16</span></a></p><p id="par0115" class="elsevierStylePara elsevierViewall">However, we believe that some key recommendations should be contemplated and promoted by clinicians and health institutions. This could mean a substantial improvement and, although hardly quantifiable, certainly unquestionable. On the one hand, it is worth recalling some general clinical safety aspects; such as ensuring the oversight of resident doctors, improving referrals and communication, or avoiding interruptions and work overload.<a class="elsevierStyleCrossRef" href="#bib0030"><span class="elsevierStyleSup">6</span></a> And from the perspective of the recommendations of the Harvard Medical School,<a class="elsevierStyleCrossRef" href="#bib0035"><span class="elsevierStyleSup">7</span></a> added to those of other authors,<a class="elsevierStyleCrossRef" href="#bib0080"><span class="elsevierStyleSup">16</span></a> it is necessary to consider the incorporation of some strategies into daily clinical practice (<a class="elsevierStyleCrossRef" href="#tbl0010">Table 2</a>).</p><elsevierMultimedia ident="tbl0010"></elsevierMultimedia><p id="par0120" class="elsevierStylePara elsevierViewall">Likewise, some specific and innovative resources have been raised in recent years. One of them has been the incorporation of checklists in diagnostic processes, although, so far, the results have not been entirely conclusive.<a class="elsevierStyleCrossRef" href="#bib0085"><span class="elsevierStyleSup">17</span></a> Another line of research corresponds to what artificial intelligence can offer us, through the application of algorithms such as symptom assessment tools, which finally offer a list of possible diagnoses. Recent experience in our setting has shown promising results, which allow us to propose the incorporation of this resource into the initial evaluation process in ED. This could mean a dynamic process of care, advancing nursing performance or the request for diagnostic tests.<a class="elsevierStyleCrossRef" href="#bib0090"><span class="elsevierStyleSup">18</span></a> Some predictive models have been proposed specifically for patients with poorly defined reasons, which seem to surpass clinical intuition in the prediction of morbidity and mortality and may be a supportive element in clinical decisions.<a class="elsevierStyleCrossRef" href="#bib0095"><span class="elsevierStyleSup">19</span></a> D-dimer has also been proposed as a support element, since the values of this marker allow stratifying the risk of mortality at 30 days.<a class="elsevierStyleCrossRef" href="#bib0100"><span class="elsevierStyleSup">20</span></a></p><p id="par0125" class="elsevierStylePara elsevierViewall">However, most authors continue to emphasize the great significance of basic clinical aspects, such as knowledge updating, history-taking and physical examination, and always performing some differential diagnosis.<a class="elsevierStyleCrossRefs" href="#bib0105"><span class="elsevierStyleSup">21,22</span></a> Likewise, it is considered essential to maintain feedback programs that allow clinicians to learn through the analysis of their own mistakes.<a class="elsevierStyleCrossRefs" href="#bib0080"><span class="elsevierStyleSup">16,21,23</span></a> And from the point of view of medical training, the recommendation of: (a) reinforce critical thinking in clinical reasoning; (b) perform a more reflective practice, deliberative in some cases, and (c) become aware of possible cognitive biases (<a class="elsevierStyleCrossRef" href="#tbl0015">Table 3</a>) that can interfere and predispose DE.<a class="elsevierStyleCrossRefs" href="#bib0105"><span class="elsevierStyleSup">21,24,25</span></a></p><elsevierMultimedia ident="tbl0015"></elsevierMultimedia><p id="par0130" class="elsevierStylePara elsevierViewall">In conclusion, a comprehensive rethinking of the diagnostic processes is necessary, to avoid the risks of both DE and overdiagnosis, which should involve clinicians, patients and the health system as a whole.</p></span><span id="sec0025" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0025">Conflict of interest</span><p id="par0135" class="elsevierStylePara elsevierViewall">The authors declare that they have no conflict of interest.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:6 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Key elements in diagnostic improvement" ] 1 => array:2 [ "identificador" => "sec0010" "titulo" => "The problem of overdiagnosis" ] 2 => array:2 [ "identificador" => "sec0015" "titulo" => "The challenge of patients who seek medical attention for poorly defined reasons" ] 3 => array:2 [ "identificador" => "sec0020" "titulo" => "Future expectations" ] 4 => array:2 [ "identificador" => "sec0025" "titulo" => "Conflict of interest" ] 5 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "fechaRecibido" => "2019-05-30" "fechaAceptado" => "2019-06-23" "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Tudela P, Forcada C, Carreres A, Ballester M. Mejorar en seguridad diagnóstica: la asignatura pendiente. Med Clin (Barc). 2019;153:332–335.</p>" ] ] "multimedia" => array:3 [ 0 => array:8 [ "identificador" => "tbl0005" "etiqueta" => "Table 1" "tipo" => "MULTIMEDIATABLA" "mostrarFloat" => true "mostrarDisplay" => false "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Table " "rol" => "short" ] ] "tabla" => array:2 [ "leyenda" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Taken from Malinovska et al.<a class="elsevierStyleCrossRef" href="#bib0075"><span class="elsevierStyleSup">15</span></a></p>" "tablatextoimagen" => array:1 [ 0 => array:2 [ "tabla" => array:1 [ 0 => """ <table border="0" frame="\n \t\t\t\t\tvoid\n \t\t\t\t" class=""><thead title="thead"><tr title="table-row"><th class="td" title="\n \t\t\t\t\ttable-head\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t" scope="col" style="border-bottom: 2px solid black"> \t\t\t\t\t\t\n \t\t\t\t\t\t</th><th class="td" title="\n \t\t\t\t\ttable-head\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t" scope="col" style="border-bottom: 2px solid black">Frequency \t\t\t\t\t\t\n \t\t\t\t\t\t</th><th class="td" title="\n \t\t\t\t\ttable-head\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t" scope="col" style="border-bottom: 2px solid black">Mortality \t\t\t\t\t\t\n \t\t\t\t\t\t</th></tr></thead><tbody title="tbody"><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Acute process \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">48% \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">4.2% \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Chronic deterioration \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">25% \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">0.7% \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Treatment-induced \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">11% \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">0.2% \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Chronic disease complication \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">9% \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">1.4% \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Functional \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">7% \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">0 \t\t\t\t\t\t\n \t\t\t\t</td></tr></tbody></table> """ ] "imagenFichero" => array:1 [ 0 => "xTab2148580.png" ] ] ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Final categories of patients who seek medical attention for poorly defined reasons.</p>" ] ] 1 => array:8 [ "identificador" => "tbl0010" "etiqueta" => "Table 2" "tipo" => "MULTIMEDIATABLA" "mostrarFloat" => true "mostrarDisplay" => false "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0010" "detalle" => "Table " "rol" => "short" ] ] "tabla" => array:2 [ "leyenda" => "<p id="spar0020" class="elsevierStyleSimplePara elsevierViewall">Adapted from Schiff et al.<a class="elsevierStyleCrossRef" href="#bib0035"><span class="elsevierStyleSup">7</span></a> and Singh et al.<a class="elsevierStyleCrossRef" href="#bib0080"><span class="elsevierStyleSup">16</span></a></p>" "tablatextoimagen" => array:1 [ 0 => array:2 [ "tabla" => array:1 [ 0 => """ <table border="0" frame="\n \t\t\t\t\tvoid\n \t\t\t\t" class=""><tbody title="tbody"><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Clinical care emphasizing careful listening and a thorough physical examination \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Ensured resident doctor oversight \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Electronic tools for differential diagnosis support \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Secure information networks for unexpected abnormal outcomes \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Accessibility to specialists or second opinions \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Doctor-patient relationship of trust and continuity \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Uncertainty shared with the patient \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Clinical follow-up systems, with patient training in alarm symptoms \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Avoid administrative barriers to clinical follow-up \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Establish feedback mechanisms for clinicians \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Strengthen critical thinking, reflective practice and bias awareness \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Enhance automated diagnostic error detection systems \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Participation of patients in diagnostic forums \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Protection of clinicians against unjustified claims \t\t\t\t\t\t\n \t\t\t\t</td></tr></tbody></table> """ ] "imagenFichero" => array:1 [ 0 => "xTab2148582.png" ] ] ] ] "descripcion" => array:1 [ "en" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall">Specific strategies for diagnostic safety improvement.</p>" ] ] 2 => array:8 [ "identificador" => "tbl0015" "etiqueta" => "Table 3" "tipo" => "MULTIMEDIATABLA" "mostrarFloat" => true "mostrarDisplay" => false "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0015" "detalle" => "Table " "rol" => "short" ] ] "tabla" => array:2 [ "leyenda" => "<p id="spar0030" class="elsevierStyleSimplePara elsevierViewall">Adapted from Clark et al.<a class="elsevierStyleCrossRef" href="#bib0105"><span class="elsevierStyleSup">21</span></a> and Phua and Tan<a class="elsevierStyleCrossRef" href="#bib0120"><span class="elsevierStyleSup">24</span></a></p>" "tablatextoimagen" => array:1 [ 0 => array:2 [ "tabla" => array:1 [ 0 => """ <table border="0" frame="\n \t\t\t\t\tvoid\n \t\t\t\t" class=""><tbody title="tbody"><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Anchoring \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Be fixed in some initial outstanding sign, without adjustment with the subsequent information \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Premature closure \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Accepting an option before verifying it, on impulse, without raising differential diagnosis \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Overconfidence \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Acting with incomplete information, by intuition, without considering suggestions \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Confirmation bias \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Selecting the information that confirms the initial hypothesis \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Outcome bias \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Selecting the most favourable option to the initial approach \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Recent influence \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Acting conditioned by similar close in time experiences \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Availability bias \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Not considering what is not known \t\t\t\t\t\t\n \t\t\t\t</td></tr><tr title="table-row"><td class="td-with-role" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t ; entry_with_role_rowhead " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Bias of omission \t\t\t\t\t\t\n \t\t\t\t</td><td class="td" title="\n \t\t\t\t\ttable-entry\n \t\t\t\t " align="left" valign="\n \t\t\t\t\ttop\n \t\t\t\t">Not performing complementary actions (examinations, consultations) \t\t\t\t\t\t\n \t\t\t\t</td></tr></tbody></table> """ ] "imagenFichero" => array:1 [ 0 => "xTab2148581.png" ] ] ] ] "descripcion" => array:1 [ "en" => "<p id="spar0025" class="elsevierStyleSimplePara elsevierViewall">Main cognitive biases in the diagnostic process.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:25 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Bringing diagnosis into the quality and safety equations" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "M.L. Graber" 1 => "R.M. Wachter" 2 => "C.K. Cassel" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1001/2012.jama.11913" "Revista" => array:6 [ "tituloSerie" => "JAMA" "fecha" => "2012" "volumen" => "308" "paginaInicial" => "1211" "paginaFinal" => "1212" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/23011708" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Epidemiología de los eventos adversos hospitalarios en Catalunya: un primer paso para la mejora de la seguridad del paciente" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "J. Bañeres" 1 => "C. Orrego" 2 => "L. Navarro" 3 => "L. Casas" 4 => "M. Banqué" 5 => "R. Suñol" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Med Clin (Barc)" "fecha" => "2014" "volumen" => "143" "numero" => "Suppl 1" "paginaInicial" => "3" "paginaFinal" => "10" ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Improving diagnosis in health care – the next imperative for patient safety" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:2 [ 0 => "H. Singh" 1 => "M.L. Graber" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1056/NEJMp1512241" "Revista" => array:6 [ "tituloSerie" => "N Engl J Med" "fecha" => "2015" "volumen" => "373" "paginaInicial" => "2493" "paginaFinal" => "2495" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/26559457" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Reducing diagnostic errors – why now?" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "D. Khullar" 1 => "A.K. Jha" 2 => "A.B. Jena" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1056/NEJMp1508044" "Revista" => array:6 [ "tituloSerie" => "N Engl J Med" "fecha" => "2015" "volumen" => "373" "paginaInicial" => "2491" "paginaFinal" => "2493" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/26397948" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Eleven-year descriptive analysis of closed court verdicts on medical errors in Spain and Massachusetts" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "P. Giraldo" 1 => "L. Sato" 2 => "J.M. Martínez-Sánchez" 3 => "M. Comas" 4 => "K. Dwyer" 5 => "M. Sala" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1136/bmjopen-2016-011644" "Revista" => array:4 [ "tituloSerie" => "BMJ Open" "fecha" => "2016" "volumen" => "6" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/28186945" "web" => "Medline" ] ] ] ] ] ] ] ] 5 => array:3 [ "identificador" => "bib0030" "etiqueta" => "6" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Error diagnóstico en Urgencias" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "P. Tudela" 1 => "A. Carreres" 2 => "M. Ballester" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Med Clin (Barc)" "fecha" => "2017" "volumen" => "149" "paginaInicial" => "170" "paginaFinal" => "175" ] ] ] ] ] ] 6 => array:3 [ "identificador" => "bib0035" "etiqueta" => "7" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Ten Principles for more conservative, care-full diagnosis" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "G.D. Schiff" 1 => "S.A. Martin" 2 => "D.H. Eidelman" 3 => "L.A. Volk" 4 => "E. Ruan" 5 => "C. Cassel" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.7326/M18-1468" "Revista" => array:6 [ "tituloSerie" => "Ann Intern Med" "fecha" => "2018" "volumen" => "169" "paginaInicial" => "643" "paginaFinal" => "645" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/30285046" "web" => "Medline" ] ] ] ] ] ] ] ] 7 => array:3 [ "identificador" => "bib0040" "etiqueta" => "8" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Importancia de la semiología en la era tecnológica" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "F.J. Laso" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Med Clin (Barc)" "fecha" => "2017" "volumen" => "148" "paginaInicial" => "559" "paginaFinal" => "561" ] ] ] ] ] ] 8 => array:3 [ "identificador" => "bib0045" "etiqueta" => "9" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Sobrediagnóstico: realidades y perspectivas" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "J. Varela" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Med Clin (Barc)" "fecha" => "2017" "volumen" => "148" "paginaInicial" => "118" "paginaFinal" => "120" ] ] ] ] ] ] 9 => array:3 [ "identificador" => "bib0050" "etiqueta" => "10" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Overdiagnosis: what it is and what it isn’t" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "J. Brodersen" 1 => "L.M. Schwartz" 2 => "C. Heneghan" 3 => "J.W. O’Sullivan" 4 => "J.K. Aronson" 5 => "S. Woloshin" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1136/ebmed-2017-110886" "Revista" => array:6 [ "tituloSerie" => "BMJ Evid Based Med" "fecha" => "2018" "volumen" => "23" "paginaInicial" => "1" "paginaFinal" => "3" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29367314" "web" => "Medline" ] ] ] ] ] ] ] ] 10 => array:3 [ "identificador" => "bib0055" "etiqueta" => "11" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Patients presenting to the emergency department with non-specific complaints: the Basel Non-specific Complaints (BANC) study" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "M. Nemec" 1 => "M.T. Koller" 2 => "C.H. Nickel" 3 => "S. Maile" 4 => "C. Winterhalder" 5 => "C. Karrer" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1111/j.1553-2712.2009.00658.x" "Revista" => array:6 [ "tituloSerie" => "Acad Emerg Med" "fecha" => "2010" "volumen" => "17" "paginaInicial" => "284" "paginaFinal" => "292" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/20370761" "web" => "Medline" ] ] ] ] ] ] ] ] 11 => array:3 [ "identificador" => "bib0060" "etiqueta" => "12" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Elderly emergency patients presenting with non-specific complaints: characteristics and outcomes" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "J.J.H. Wachelder" 1 => "P.M. Stassen" 2 => "L.P.A.M. Hubens" 3 => "S.H.A. Brouns" 4 => "S.L.E. Lambooij" 5 => "J.P. Dieleman" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1371/journal.pone.0189910" "Revista" => array:4 [ "tituloSerie" => "PLoS One" "fecha" => "2017" "volumen" => "12" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29287100" "web" => "Medline" ] ] ] ] ] ] ] ] 12 => array:3 [ "identificador" => "bib0065" "etiqueta" => "13" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "The proportion of correct diagnoses is low in emergency patients with nonspecific complaints presenting to the emergency department" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "A. Peng" 1 => "M. Rohacek" 2 => "S. Ackermann" 3 => "J. Ilsemann-Karakoumis" 4 => "L. Ghanim" 5 => "A.S. Messmer" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:3 [ "tituloSerie" => "Swiss Med Wkly" "fecha" => "2015" "volumen" => "145" ] ] ] ] ] ] 13 => array:3 [ "identificador" => "bib0070" "etiqueta" => "14" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Unplanned readmissions among patients presenting with nonspecific complaints" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "J.J.H. Wachelder" 1 => "L.S. van Galen" 2 => "J. Kellett" 3 => "C.H. Nickel" 4 => "H.R. Haak" 5 => "safer@home consortium" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.ejim.2018.05.020" "Revista" => array:6 [ "tituloSerie" => "Eur J Intern Med" "fecha" => "2018" "volumen" => "54" "paginaInicial" => "e36" "paginaFinal" => "e37" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29885755" "web" => "Medline" ] ] ] ] ] ] ] ] 14 => array:3 [ "identificador" => "bib0075" "etiqueta" => "15" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Trajectories of survival in patients with nonspecific complaints" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "A. Malinovska" 1 => "C.H. Nickel" 2 => "R. Bingisser" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.ejim.2018.06.020" "Revista" => array:6 [ "tituloSerie" => "Eur J Intern Med" "fecha" => "2018" "volumen" => "55" "paginaInicial" => "e17" "paginaFinal" => "e18" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/30006032" "web" => "Medline" ] ] ] ] ] ] ] ] 15 => array:3 [ "identificador" => "bib0080" "etiqueta" => "16" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Measures to Improve Diagnostic Safety in Clinical Practice" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "H. Singh" 1 => "M.L. Graber" 2 => "T.P. Hofer" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:2 [ "tituloSerie" => "J Patient Saf" "fecha" => "2016" ] ] ] ] ] ] 16 => array:3 [ "identificador" => "bib0085" "etiqueta" => "17" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Checklists to prevent diagnostic errors: a pilot randomized controlled trial" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:2 [ 0 => "J.W. Ely" 1 => "M.A. Graber" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Diagnosis (Berl)" "fecha" => "2015" "volumen" => "2" "paginaInicial" => "163" "paginaFinal" => "169" ] ] ] ] ] ] 17 => array:3 [ "identificador" => "bib0090" "etiqueta" => "18" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Experiencia de Mediktor®: un nuevo evaluador de síntomas basado en inteligencia artificial para pacientes atendidos en el servicio de urgencias" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:5 [ 0 => "E. Moreno" 1 => "I. Pueyo" 2 => "M. Sánchez" 3 => "M. Martín" 4 => "J. Masip" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Emergencias" "fecha" => "2017" "volumen" => "29" "paginaInicial" => "391" "paginaFinal" => "396" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29188913" "web" => "Medline" ] ] ] ] ] ] ] ] 18 => array:3 [ "identificador" => "bib0095" "etiqueta" => "19" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Are mortality and acute morbidity in patients presenting with nonspecific complaints predictable using routine variables?" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "M.A. Jenny" 1 => "R. Hertwig" 2 => "S. Ackermann" 3 => "A.S. Messmer" 4 => "J. Karakoumis" 5 => "C.H. Nickel" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1111/acem.12755" "Revista" => array:6 [ "tituloSerie" => "Acad Emerg Med" "fecha" => "2015" "volumen" => "22" "paginaInicial" => "1155" "paginaFinal" => "1163" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/26375290" "web" => "Medline" ] ] ] ] ] ] ] ] 19 => array:3 [ "identificador" => "bib0100" "etiqueta" => "20" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Risk stratification using D-dimers in patients presenting to the emergency department with nonspecific complaints" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "C.H. Nickel" 1 => "T. Kuster" 2 => "C. Keil" 3 => "A.S. Messmer" 4 => "N. Geigy" 5 => "R. Bingisser" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.ejim.2016.03.006" "Revista" => array:6 [ "tituloSerie" => "Eur J Intern Med" "fecha" => "2016" "volumen" => "31" "paginaInicial" => "20" "paginaFinal" => "24" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/27053291" "web" => "Medline" ] ] ] ] ] ] ] ] 20 => array:3 [ "identificador" => "bib0105" "etiqueta" => "21" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Diagnostic errors and the bedside clinical examination" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "B.W. Clark" 1 => "A. Derakhshan" 2 => "S.V. Desai" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.mcna.2017.12.007" "Revista" => array:6 [ "tituloSerie" => "Med Clin North Am" "fecha" => "2018" "volumen" => "102" "paginaInicial" => "453" "paginaFinal" => "464" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29650067" "web" => "Medline" ] ] ] ] ] ] ] ] 21 => array:3 [ "identificador" => "bib0110" "etiqueta" => "22" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "The key role of differential diagnosis in diagnosis" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "B. Jain" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Diagnosis (Berl)" "fecha" => "2017" "volumen" => "4" "paginaInicial" => "239" "paginaFinal" => "240" ] ] ] ] ] ] 22 => array:3 [ "identificador" => "bib0115" "etiqueta" => "23" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Audit and feedback: effects on professional practice and healthcare outcomes" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "N. Ivers" 1 => "G. Jamtvedt" 2 => "S. Flottorp" 3 => "J.M. Young" 4 => "J. Odgaard-Jensen" 5 => "S.D. French" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1002/14651858.CD000259.pub3" "Revista" => array:3 [ "tituloSerie" => "Cochrane Database of Syst Rev" "fecha" => "2012" "volumen" => "6" ] ] ] ] ] ] 23 => array:3 [ "identificador" => "bib0120" "etiqueta" => "24" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Cognitive aspect of diagnostic errors" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:2 [ 0 => "D.H. Phua" 1 => "N.C. Tan" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Ann Acad Med Singapore" "fecha" => "2013" "volumen" => "42" "paginaInicial" => "33" "paginaFinal" => "41" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/23417589" "web" => "Medline" ] ] ] ] ] ] ] ] 24 => array:3 [ "identificador" => "bib0125" "etiqueta" => "25" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Teaching critical thinking: a case for instruction in cognitive biases to reduce diagnostic errors and improve patient safety" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "C.S. Royce" 1 => "M.M. Hayes" 2 => "R.M. Schwartzstein" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1097/ACM.0000000000002518" "Revista" => array:6 [ "tituloSerie" => "Acad Med" "fecha" => "2019" "volumen" => "94" "paginaInicial" => "187" "paginaFinal" => "194" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/30398993" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/23870206/0000015300000008/v1_201910190847/S2387020619303997/v1_201910190847/en/main.assets" "Apartado" => array:4 [ "identificador" => "44145" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Special article" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/23870206/0000015300000008/v1_201910190847/S2387020619303997/v1_201910190847/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020619303997?idApp=UINPBA00004N" ]
Journal Information
Share
Download PDF
More article options
Received 30 May 2019. Accepted 23 June 2019
Article information
These are the options to access the full texts of the publication Medicina Clínica (English Edition)
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail