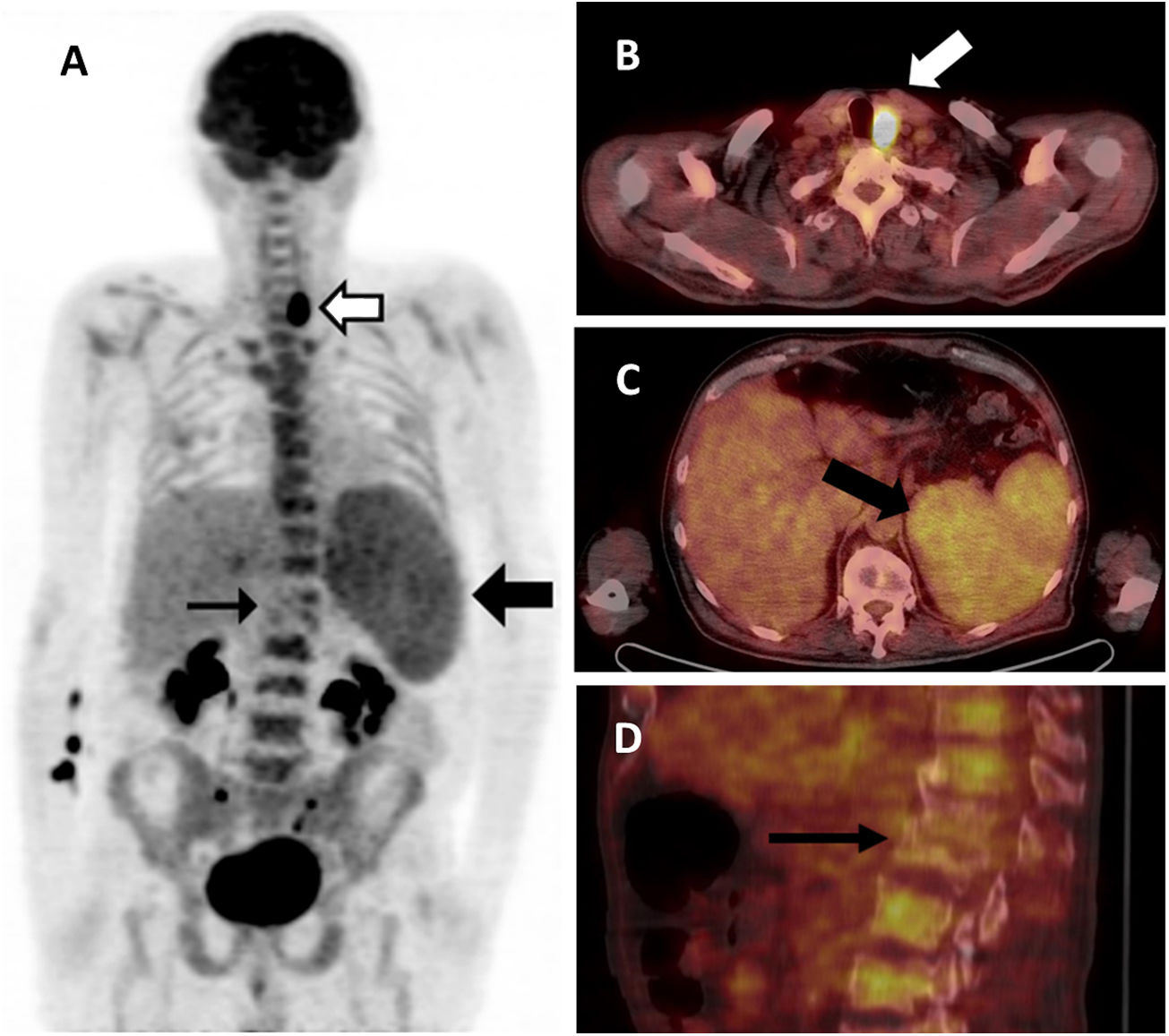
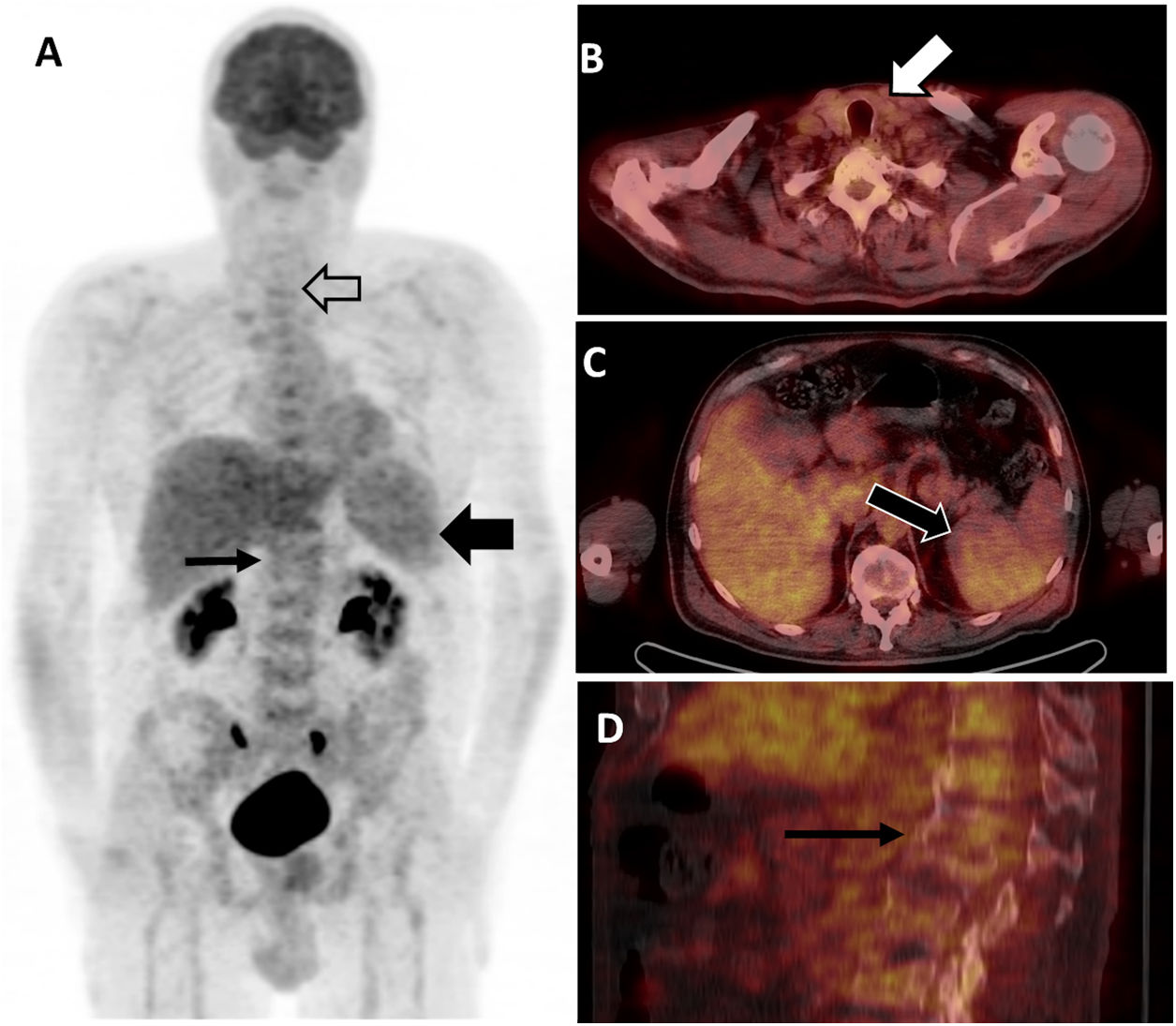
Interesting Images: Surprising and didactic findings from clinical practice
More infoArticle

Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)
array:24 [ "pii" => "S2253808922000350" "issn" => "22538089" "doi" => "10.1016/j.remnie.2022.04.003" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1363" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "copyrightAnyo" => "2022" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S64-S65" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S2253654X22000026" "issn" => "2253654X" "doi" => "10.1016/j.remn.2021.12.006" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1363" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S64-S65" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Imágenes de interés</span>" "titulo" => "Leishmaniasis visceral versus recidiva de mieloma múltiple: El bazo como pista principal" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S64" "paginaFinal" => "S65" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Visceral leishmaniasis versus treated multiple myeloma relapse: Spleen as the main clue" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figura 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 1095 "Ancho" => 1255 "Tamanyo" => 135688 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">MIP (A), cortes de fusión axiales (B y C) y sagital (D) de la PET-CT con 18F-FDG del estudio de control, con normalización de las alteraciones descritas en el estudio inicial, tras hemitiroidectomía izquierda por carcinoma folicular de tiroides y tratamiento de la Leishmaniasis.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "X. Boulvard-Chollet, F.M. Cañete-Sánchez, P.M. Hernández-Pérez, L.G. Romero-Robles, P. Garrastachu-Zumarán" "autores" => array:5 [ 0 => array:2 [ "nombre" => "X." "apellidos" => "Boulvard-Chollet" ] 1 => array:2 [ "nombre" => "F.M." "apellidos" => "Cañete-Sánchez" ] 2 => array:2 [ "nombre" => "P.M." "apellidos" => "Hernández-Pérez" ] 3 => array:2 [ "nombre" => "L.G." "apellidos" => "Romero-Robles" ] 4 => array:2 [ "nombre" => "P." "apellidos" => "Garrastachu-Zumarán" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2253808922000350" "doi" => "10.1016/j.remnie.2022.04.003" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808922000350?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X22000026?idApp=UINPBA00004N" "url" => "/2253654X/00000041000000S1/v1_202207160644/S2253654X22000026/v1_202207160644/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2253808922000362" "issn" => "22538089" "doi" => "10.1016/j.remnie.2022.04.004" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1364" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S66-S68" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "[<span class="elsevierStyleSup">68</span>Ga] Ga-DOTA-TOC PET/CT uptake by parathyroid adenoma in the context of multiple endocrine neoplasia type 1 (MEN1)" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S66" "paginaFinal" => "S68" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Captación en [<span class="elsevierStyleSup">68</span>Ga]Ga-DOTA-TOC PET/TC de adenoma paratiroideo en el contexto de neoplasia endocrina múltiple tipo 1 (MEN1)" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0015" "etiqueta" => "Figure 3" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr3.jpeg" "Alto" => 869 "Ancho" => 1500 "Tamanyo" => 96302 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0015" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall"><span class="elsevierStyleBold"><span class="elsevierStyleItalic">[<span class="elsevierStyleSup">68</span>Ga]Ga-DOTA-TOC PET/CT. MIP: maximum intensity projection (A). PET and PET/CT fusion in axial projection (A). PET/CT fusion in the coronal (C) and sagittal (D) projections:</span></span> an area of ​​moderate radiopharmaceutical uptake is observed (blue arrow), which sits on the already known parathyroid adenoma (Krenning score 2). Likewise, other foci of hyperuptake of the radiopharmaceutical are observed in the already known metastases in left interlobar adenopathy (Krenning score 2) and segment V of the liver (Krenning score 4). Activity in the right forearm corresponds to the injection site. Rest of the study with a radiopharmaceutical physiological distribution.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "V. Carrero-Vásquez, S. Prado-Wohlwend" "autores" => array:2 [ 0 => array:2 [ "nombre" => "V." "apellidos" => "Carrero-Vásquez" ] 1 => array:2 [ "nombre" => "S." "apellidos" => "Prado-Wohlwend" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S2253654X22000038" "doi" => "10.1016/j.remn.2021.12.007" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X22000038?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808922000362?idApp=UINPBA00004N" "url" => "/22538089/00000041000000S1/v1_202207210552/S2253808922000362/v1_202207210552/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S225380892100166X" "issn" => "22538089" "doi" => "10.1016/j.remnie.2021.12.001" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1344" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S62-S63" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Brain perfusion SPECT in Alice in Wonderland syndrome" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S62" "paginaFinal" => "S63" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "SPECT de perfusión cerebral en el síndrome de Alicia en el país de las Maravillas" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1359 "Ancho" => 3333 "Tamanyo" => 470380 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">(A) Brain perfusion study performed after the administration of 370 MBq (10 mCi) of <span class="elsevierStyleSup">99m</span>Tc-ECD, where a perfusion defect is observed in the right occipito-temporal territory (white arrow). (B) Brain perfusion control study performed after the administration of 481 MBq (13 mCi) of <span class="elsevierStyleSup">99m</span>Tc-HMPAO, in which resolution of the occipital perfusion defect is observed (yellow arrow). The technical parameters selected for SPECT studies were a 128 × 128 matrix, 128 rotation angles and an acquisition of 20 s per angle. SPECT attenuation correction was performed and it was applied while processing Butterworth filter.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "P. Oliván-Sasot, C. Ipiens-Escuer, A.C. Orozco-Molano, H. Azzi, L. Camacho-Berne, A. Tembl-Ferrairo" "autores" => array:6 [ 0 => array:2 [ "nombre" => "P." "apellidos" => "Oliván-Sasot" ] 1 => array:2 [ "nombre" => "C." "apellidos" => "Ipiens-Escuer" ] 2 => array:2 [ "nombre" => "A.C." "apellidos" => "Orozco-Molano" ] 3 => array:2 [ "nombre" => "H." "apellidos" => "Azzi" ] 4 => array:2 [ "nombre" => "L." "apellidos" => "Camacho-Berne" ] 5 => array:2 [ "nombre" => "A." "apellidos" => "Tembl-Ferrairo" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S2253654X21001773" "doi" => "10.1016/j.remn.2021.09.010" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X21001773?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S225380892100166X?idApp=UINPBA00004N" "url" => "/22538089/00000041000000S1/v1_202207210552/S225380892100166X/v1_202207210552/en/main.assets" ] "en" => array:17 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Visceral leishmaniasis versus multiple myeloma relapse: Spleen as the main clue" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S64" "paginaFinal" => "S65" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "X. Boulvard-Chollet, F.M. Cañete-Sánchez, P.M. Hernández-Pérez, L.G. Romero-Robles, P. Garrastachu-Zumarán" "autores" => array:5 [ 0 => array:4 [ "nombre" => "X." "apellidos" => "Boulvard-Chollet" "email" => array:1 [ 0 => "xleboulvard@riojasalud.es" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "F.M." "apellidos" => "Cañete-Sánchez" "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 2 => array:3 [ "nombre" => "P.M." "apellidos" => "Hernández-Pérez" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">c</span>" "identificador" => "aff0015" ] ] ] 3 => array:3 [ "nombre" => "L.G." "apellidos" => "Romero-Robles" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 4 => array:3 [ "nombre" => "P." "apellidos" => "Garrastachu-Zumarán" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] ] "afiliaciones" => array:3 [ 0 => array:3 [ "entidad" => "Departments of Nuclear Medicine, University Hospital San Pedro and Centre for Biomedical Research of La Rioja (CIBIR), Logroño, Spain" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Departments of Nuclear Medicine, University Hospital Puerta del Mar, Cádiz, Spain" "etiqueta" => "b" "identificador" => "aff0010" ] 2 => array:3 [ "entidad" => "Departments of Hematology and Hemotherapy, University Hospital San Pedro, Logroño, Spain" "etiqueta" => "c" "identificador" => "aff0015" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Leishmaniasis visceral versus recidiva de mieloma múltiple: El bazo como pista principal" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1157 "Ancho" => 1305 "Tamanyo" => 152111 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">MIP (A), axial (B and C) and sagittal (D) fusion sections of the PET/CT with <span class="elsevierStyleSup">18</span>F-FDG of the initial study. Diffuse hypermetabolism is observed in the bone marrow except for an uptake defect in D12 and L1. Splenomegaly with moderate diffuse hypermetabolism. Intense focal uptake in the left thyroid nodule.</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">A 62-year-old male with multiple myeloma (MM) in lenalidomide treatment after an autologous bone marrow (BM) transplant two years ago, was hospitalized for fever and pancytopenia. An F-18 FDG PET/CT was done to rule out MM relapse. Maximum intensity projection ([MIP], A), axial (B, C) and sagittal (D) fusion images showed moderate diffuse uptake in enlarged spleen (bold black arrow, maximum standardized uptake value [SUV<span class="elsevierStyleInf">max</span>] = 6,7) and BM (SUV<span class="elsevierStyleInf">max</span> = 6, higher than the liver) excepting an uptake defect in 12th thoracic and 1st lumbar vertebral bodies secondary to old compression fractures (thin black arrow) (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>). Additionally, we observed intense focal uptake of the radiotracer in a nodule situated in the left thyroid lobe (white arrow, SUV<span class="elsevierStyleInf">max</span> = 22,2). After this exploration, BM biopsy was taken, being negative for MM. However, images in some histiocytes suggesting Leishmania parasites were found, so PCR determination of Leishmania DNA was done, giving a final diagnosis of visceral leishmaniasis (VL). Subsequently, the patient received antibiotherapy amphotericin B during a month, and fine needle aspiration (FNA) followed by thyroid left lobectomy were performed, with the anatomopathological result of follicular thyroid cancer.</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0010" class="elsevierStylePara elsevierViewall">One month after surgery, subsequent F-18 FDG PET/CT revealed normalization of the pathological uptake in the spleen (bold black arrow in A and C) and BM (A, D) and no uptake in the left thyroid bed (white arrow in A and B) (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>).</p><elsevierMultimedia ident="fig0010"></elsevierMultimedia><p id="par0015" class="elsevierStylePara elsevierViewall">The leishmaniases are a group of diseases caused by the protozoa parasite Leishmania, transmitted by the bite of infected female phlebotomine sandflies. It can be cutaneous (the most common form), mucocutaneus or VL (the most serious form, also known as kala-azar) and is endemic in the mediterranean countries. It is associated with malnutrition, population displacement, poor housing, weak immune system and lack of resources.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> Since parasites replicate in the reticuloendothelial system, very high parasite loads accumulate in the spleen, liver, and BM in the visceral form, leading to an increased F-18 FDG uptake in those locations. Recommended treatment is liposomal amphotericin B intravenously. MM is an haematologic cancer associated with the presence of malignant plasma cells that usually reside in the BM and the F-18 FDG PET/CT shows diffuse increased BM uptake higher than that of liver in case of multiple myeloma infiltration which is also a very frequent finding in VL. MM extramedullary disease is increasingly seen in the clinic as a result of sensitive imaging studies and extended survival but spleen is not a common site of infiltration in this setting which, on the other hand, is the most frequent pattern in VL.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> Therefore, it is important to have in mind this entity, especially when observing high diffuse BM and spleen uptake, in those MM patients with weakened immune systems who are living in endemic area of VL or reporting to travel to endemic areas. Other causes of splenic FDG uptake on PET imaging reported in the literature include lymphoma, granulocyte colony stimulating factor treatment, beta-thalassemia, and infections. Diffuse increased FDG uptake in the bone marrow on PET scan is frequently observed due to hematopoietic stimulation after chemotherapy but can also be noted in a variety of pathologic conditions, including leukemia and lymphoma.</p><p id="par0020" class="elsevierStylePara elsevierViewall">Also, this case highlights the importance of histopathological correlation of PET findings, in bone marrow and studying focal F-18 FDG uptake in the thyroid, which is incidentally detected in 1-2% of patients. When it corresponds to a thyroid nodule conveys an increased risk of thyroid cancer of approximately one in three, so FNA is recommended if ≥1 cm.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a></p><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Conflict of interest</span><p id="par0025" class="elsevierStylePara elsevierViewall">All authors declare that they have no potential conflicts of interest to disclose.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:2 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Conflict of interest" ] 1 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "fechaRecibido" => "2021-09-28" "fechaAceptado" => "2021-12-22" "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Boulvard-Chollet X, Cañete-Sánchez FM, Hernández-Pérez PM, Romero-Robles LG, Garrastachu-Zumarán P. Leishmaniasis visceral ver-sus recidiva de mieloma múltiple: El bazo como pista principal. Rev Esp Med Nucl Imagen Mol. 2022;41:S64–S65.</p>" ] ] "multimedia" => array:2 [ 0 => array:8 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1157 "Ancho" => 1305 "Tamanyo" => 152111 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">MIP (A), axial (B and C) and sagittal (D) fusion sections of the PET/CT with <span class="elsevierStyleSup">18</span>F-FDG of the initial study. Diffuse hypermetabolism is observed in the bone marrow except for an uptake defect in D12 and L1. Splenomegaly with moderate diffuse hypermetabolism. Intense focal uptake in the left thyroid nodule.</p>" ] ] 1 => array:8 [ "identificador" => "fig0010" "etiqueta" => "Figure 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 1095 "Ancho" => 1255 "Tamanyo" => 143818 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0010" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar1005" class="elsevierStyleSimplePara elsevierViewall">MIP (A), axial (B and C) and sagittal (D) fusion slices of the PET-CT with 18F-FDG of the control study, with normalization of the alterations described in the initial study, after left hemithyroidectomy for follicular carcinoma of thyroid and treatment of Leishmaniasis.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:3 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Leishmaniasis" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "World Health Organization" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "WWW" => array:2 [ "link" => "https://www.who.int/gho/neglected_diseases/leishmaniasis/en/" "fecha" => "2018" ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "18F FDG PET/CT in visceral leishmaniasis: uptake patterns in the context of a multiannual outbreak in Northern Italy" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "L. Zanoni" 1 => "S. Varani" 2 => "L. Attard" 3 => "JJ Morigi" 4 => "E Vanino" 5 => "M Ortalli" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s12149-019-01381-6" "Revista" => array:6 [ "tituloSerie" => "Ann Nucl Med" "fecha" => "2019" "volumen" => "33" "paginaInicial" => "716" "paginaFinal" => "723" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/31254270" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "B.R. Haugen" 1 => "E.K. Alexander" 2 => "K.C. Bible" 3 => "GM Doherty" 4 => "SJ Mandel" 5 => "Y.E. NikiforovF" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1089/thy.2015.0020" "Revista" => array:6 [ "tituloSerie" => "Thyroid" "fecha" => "2016" "volumen" => "26" "paginaInicial" => "1" "paginaFinal" => "133" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/26462967" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/22538089/00000041000000S1/v1_202207210552/S2253808922000350/v1_202207210552/en/main.assets" "Apartado" => array:4 [ "identificador" => "7927" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Interesting images" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/22538089/00000041000000S1/v1_202207210552/S2253808922000350/v1_202207210552/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808922000350?idApp=UINPBA00004N" ]
Consulte los artículos y contenidos publicados en éste medio, además de los e-sumarios de las revistas científicas en el mismo momento de publicación
Esté informado en todo momento gracias a las alertas y novedades
Acceda a promociones exclusivas en suscripciones, lanzamientos y cursos acreditados
The Revista Española de Medicina Nuclear e Imagen Molecular (Spanish Journal of Nuclear Medicine and Molecular Imaging), was founded in 1982, and is the official journal of the Spanish Society of Nuclear Medicine and Molecular Imaging, which has more than 700 members. The Journal, which publishes 6 regular issues per year, has the promotion of research and continuing education in all fields of Nuclear Medicine as its main aim. For this, its principal sections are Originals, Clinical Notes, Images of Interest, and Special Collaboration articles. The works may be submitted in Spanish or English and are subjected to a peer review process. In 2009, it became the leading Spanish journal in the field of Medical Imaging on having an Impact Factor , awarded by the Journal Citation Reports.
Science Citation Index Expander, Medline, IME, Bibliomed, EMBASE/Excerpta Medica, Healthstar, Cancerlit, Toxine, Inside Conferences, Scopus
See moreThe Impact Factor measures the average number of citations received in a particular year by papers published in the journal during the two preceding years.
© Clarivate Analytics, Journal Citation Reports 2022
SRJ is a prestige metric based on the idea that not all citations are the same. SJR uses a similar algorithm as the Google page rank; it provides a quantitative and qualitative measure of the journal's impact.
See moreSNIP measures contextual citation impact by wighting citations based on the total number of citations in a subject field.
See more
Interesting Images: Surprising and didactic findings from clinical practice
More info
Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)

¿Es usted profesional sanitario apto para prescribir o dispensar medicamentos?
Are you a health professional able to prescribe or dispense drugs?
Você é um profissional de saúde habilitado a prescrever ou dispensar medicamentos