Introduction
In Spain, smoking is beginning to be considered a socially unacceptable behavior,1 and its prevalence is decreasing in older age groups, although not in women. However, the decreases are smaller than in other European countries.2 The benefits of quitting are evident:3 quitting is the most important step smokers can take to improve their health, therefore patients should be informed about the risks of smoking, the benefits of quitting, and the options available to quit successfully. Given that the effectiveness of these measures is beyond question,7-9 anti-smoking advice should be provided systematically, as should advice about the most suitable treatment to help smokers quit.4-6 Because of its coverage and accessibility, primary care is the ideal setting for these interventions.10-12 In recent years general practitioners have developed programs of systematic intervention aimed at dealing with smoking as a risk factor in public health,4,13,14 but these programs should be more widely used.
To facilitate the timely contact and interaction with smokers and provide personalized advice and follow-up to the more highly motivated among them,15,16 the Support Program for Smokers (SPS) was implemented in Health Area VIII of Asturias, Spain.17 This article reports on the effectiveness of the program in helping smokers to quit. A secondary goal was to determine the mean time to relapse in order to evaluate the need to intensify follow-up measures for smokers who wish to quit.
Methods
Design
The participants were patients older than 14 years who took part in the SPS between 1 July 1998 and 30 September 2001. They were chosen from among a total of 987 patients who had been seen for any reason at primary care centers in Health Area VIII, Asturias. We excluded patients who did not live in Health Area VIII at the time of the study, or who had died. We considered as participants smokers who, having agreed to take part in the program, were given appointments for a number of scheduled activities which consisted of at least Richmond and Fagerström tests. These patients received systematic minimal intervention and if their degree of dependence was high nicotine replacement therapy (NRT). A sample size of 400 persons was calculated on the basis of the total number of patients who took part in the SPS, with an expected prevalence of 50%, a precision of 5% and a drop-out rate of 35%. To ensure that part of the sample was followed for more than 24 months, the participants were distributed in two equal groups on the basis of date of entry in the SPS. In both groups the sample was chosen randomly from a list of patients included in the SPS and a table of random numbers.
Main outcome variables
Smoker/nonsmoker status, relapses, mean duration of abstention and number of attempts to quit after the study period were noted. This information was obtained by health care staff who surveyed participants by telephone.
Independent variables
Information obtained from the patient´s medical record and noted on the data sheets used in the SPS included age, sex, duration of smoking habit in years, number of cigarettes smoked per day at the time of enrolment, chronic illnesses, previous attempts to quit, score on the Richmond and Fagerström tests, use of NRT, previous telephone reinforcement, and number and mean duration of follow-up visits.
Statistical analysis
Quantitative variables are reported as the mean, standard deviation and median; qualitative variables are reported as absolute and relative frequency distributions. Survival analysis is used to describe the findings for relapses, and 95% confidence intervals are reported for each estimator. Differences for each item in comparison to the control variables are evaluated with the chi-squared or Student´s t test. The differences were considered statistically significant when P was less than 0.05. All analyses were done with SPSS software.
Results
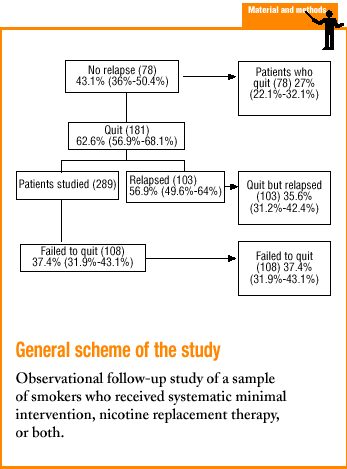
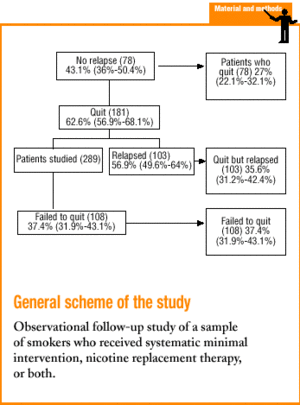
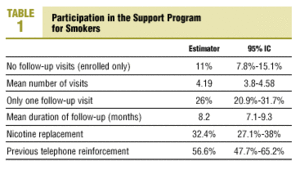
Of the 400 patients initially included in the study, we were able to contact 289 (72.3%). There was no statistically significant difference in response rates between observers. For the group of patients who could not be reached, we recorded all available data from the data sheet and found no statistically significant differences in the distribution of values for any variable. Of the final sample, 143 patients (49.5%) had been included in the SPS before the year 2000. Mean age was 44 years, 75% of the participants were younger than 50 years, and 177 participants (58.9%) were men. Mean duration of the smoking habit was 24 years, with a mean daily consumption of 26 cigarettes. Mean scores on the tests for dependence and motivation to quit were 5.3 and 7.8, respectively. Of all participants, 83.4% had at least one chronic illness, and 67% had tried to quit before. The data sheet was available for 281 patients (97%), 31 (11%) of whom did not attend any of the follow-up visits after initial enrollment («enrolled only»). Mean number of visits, duration of follow-up, use of NRT and previous reinforcement are shown in Table 1. Of the 289 smokers, 181 quit initially, and at the end of the study 78 continued to abstain from smoking.
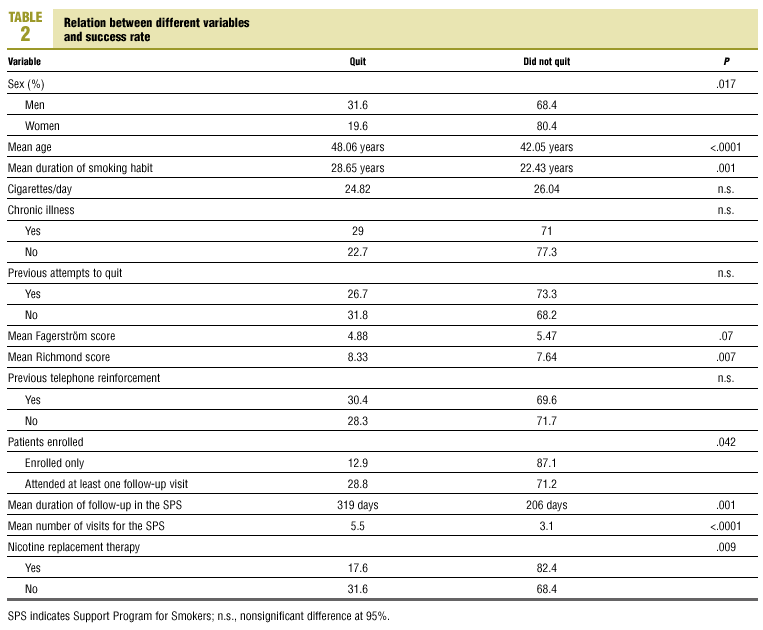
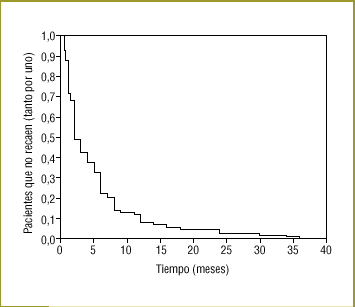
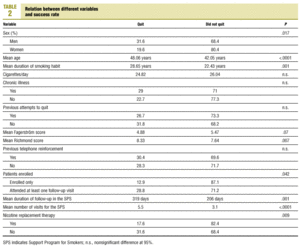
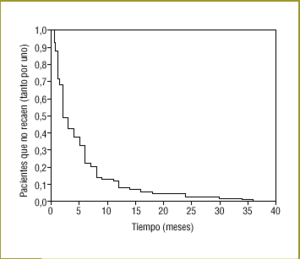
There were no statistically significant differences in success rates (proportion of patients who said they had quit) between observers, although we did find significant differences in some variables between patients who quit and those who did not (Table 2). Of the 108 patients who failed to quit, 71.1% (64.7%-76.9%) made no further attempt, and among those who did try again, 58.1% (45.5%-69.8%) tried only once more. Of the 103 patients who relapsed, only 98 recalled how long they had refrained from smoking: the mean was 5.25 months (3.9-6.6 months). Figure 1 shows the survival curves; 50% relapsed within the first 2 months (1.4-2.6 months), and 75% within the first 6 months (4.6-7.4 months).
Figure 1. Percentage of patients who had still not relapsed (referred to unity) at different points in time (only patients who relapsed).
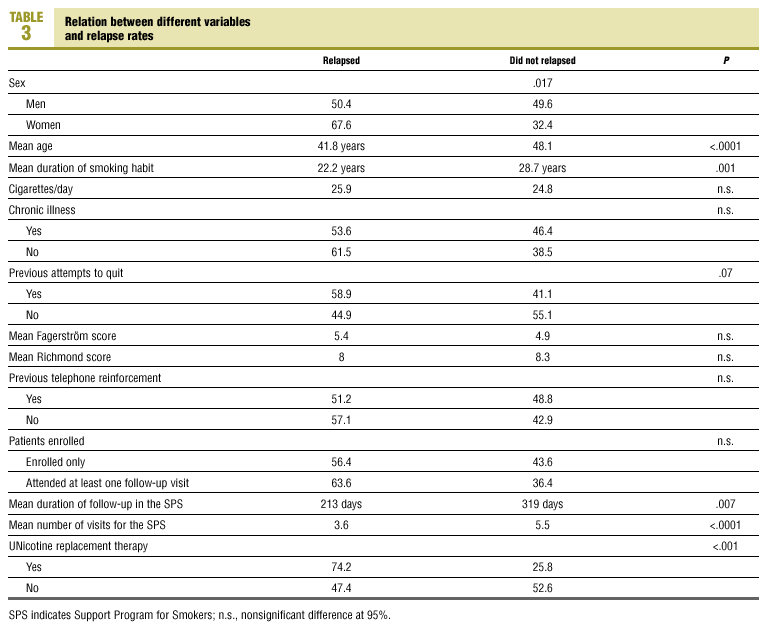
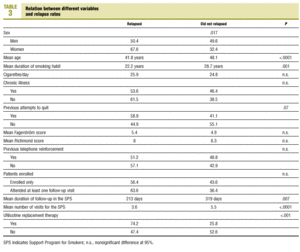
We found a statistically significant relationship between relapse rates and certain variables (Table 3). Patients who had not resumed smoking at the end of the study had abstained for a mean of 23.19 months (95% CI, 20.8-25.6 months), hence 80% had not smoked for 1 year, and 50% had not smoked for more than 23 months. Considering only smokers who joined the program more than 12 months previously and those who had abstained for at least 1 year, the overall success rate was 27.2% (21.8%-33.1%, ie, 65 of 239 patients).
Discussion
The relatively high drop-out rate (27.7%) may have skewed the results; however, we believe the patients who could not be contacted for follow-up did not differ significantly in the main outcome variables from those who completed the study program. Comparison of the information obtained about the independent variables from the data sheet failed to reveal any significant differences between the two groups in the distribution of values for these variables, or in the results obtained by different observers.
As in other studies,18,19 most patients who took part in the SPS were men; mean age was higher than in earlier surveys, as there as no age limit for enrollment. Eleven percent of the participants did not attend any of the follow-up appointments, and we assumed they had dropped out of the program or that their participation had not been recorded. However, this figure was clearly lower than that reported in an earlier study,19 in which 32.8% of those initially enrolled did not participate in any further interventions. The SPS was evaluated yearly when the center´s regular services were reviewed; this may have contributed to the better rate of participation.
In contrast with at least one earlier study,19 56.6% of the participants had received previous reinforcement. In our health area, the SPS is implemented jointly by physicians and nurses, and involvement of the nursing staff is fundamental in this type of program. Success was greatest in smokers who were more highly motivated and who participated in the program for longer, but, in contrast to other studies,11,20 the program was less successful when NRT was used. We have no explanation for this finding; although patients treated with NRT smoked more and were more dependent on nicotine, they were also more highly motivated.
We did not evaluate adverse effects. The percentage of ex-smokers was greater than in an earlier report18 on a systematic, opportunistic intervention in a nonselected population, but these participants did not use NRT and their initial level of motivation was clearly lower than in our patients. The percent success rate in the present study was also higher than that found in another study4 with NRT. However, our results were worse than those obtained by Torrecilla et al.11 with systematic minimal intervention and NRT. One of the most noteworthy biases in our study arises from the fact that our main outcome variable was evaluated with information obtained by telephone survey, with no further analysis to corroborate the patients´ responses, despite the fact that Bedfont breath CO monitors are available at the health centers in our area for use at follow-up appointments. The administration of the study was centralized, and we realized that giving appointments for follow-up visits might have increased the number of drop-outs. This bias may have led us to overestimate the effectiveness of the intervention as a result of underreporting of smoker status. Some have estimated underreporting at 2%-4%,1 whereas others21,22 have reported a deception rate of 15% or 17.6%, although we note that these latter surveys were done by staff members of the health center. Our survey was run by four family physicians at different health centers and by a health care technician, hence false positives were unlikely to be due to the patient´s desire to please the physician. Moreover, the survey was done outside the health center setting, and no observer-dependent differences were found in drop-out rates. As an added measure, responses were checked against the information entered in the data sheet.
Another limitation arises from the characteristics of the study: because no control group was used, we cannot determine whether the success rates were the result of the intervention we set out to evaluate, or of other factors. Among the earlier studies we reviewed, the program most similar to ours was that described by Martín Cantera et al.,19 which achieved an 18% success rate. Although this figure is lower than our success rate, no mention of the use of NRT was made in this study. We achieved an initial success rate of 62.6%, although of those who quit at the start of the program, 56.9% resumed smoking, half within the first 2 months and one-fourth after the first 6 months.
It would seem reasonable to follow participants more closely during the first months of the program, and to use telephone reinforcement (especially for participants who skip scheduled appointments), to instill in participants the idea that relapses are part of the quitting process, and to support subsequent attempts to quit.
The effectiveness of the SPS appears to have been acceptable. Coverage was low: we estimate a target population of 25 109 patients,15 of whom 987 4% of all smokers in the area served by our health centers were enrolled in the program. Other programs have been implemented individually by physicians interested in smoking prevention and cessation,5,23 whereas our program forms part of an institutional policy aimed at gradually involving all primary care professionals in attempts to deal with this health problem. Raising their awareness of the problem takes time, and we did not set highly ambitious goals for the primary care teams in this initial study. Despite the low coverage, it should be recalled that smokers who enrolled in the program agreed to take part and attended at least one appointment. However, the SPS aims to identify smokers, inform them about their habit, advise them and offer help. Thus, in addition to the patients initially enrolled, others received advice, and we expect at least 5% of this latter group to quit smoking.24
In the light of evidence that the program is effective, more ambitious goals should be considered, and coverage should be extended to make the program available to the large percentage of smokers who intend to quit.25
Acknowledgments
We thank doctors Carlos Fernández Benítez and José Fuentes for their help with the telephone surveys.