Since its introduction in 1968, ERCP has become an essential tool for the diagnosis and treatment of numerous biliary and pancreatic diseases.1 In the hands of expert gastroenterologists, the rate of complications is low,2 although its incidence reaches 4%–10% and mortality 0.4%.3 In order of frequency, complications include pancreatitis (1.3%–5.4%), hemorrhage (0.76%–3%), cholangitis (0.78%–1%) and perforation (0.3%–2.1%).4 The risk of complications is statistically higher in therapeutic cases (5.4%) than in diagnostic cases (1.38%).4 Traditionally, surgical treatment was used for these complications; however, in the last decade, conservative management has provided increasingly better results.5
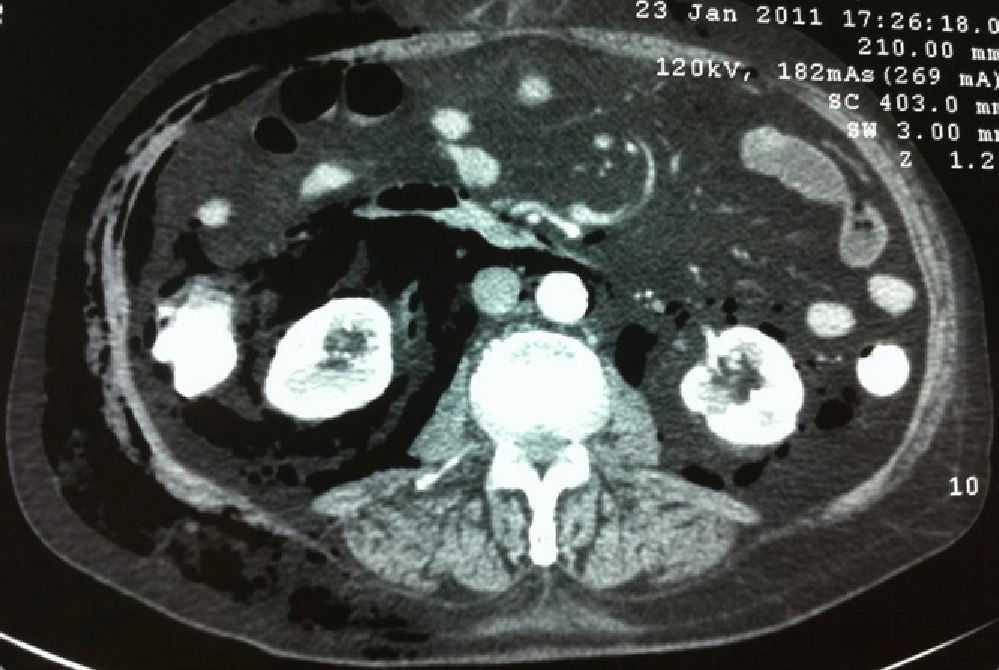
The patient is an 85-year-old male with a prior history of atrial fibrillation, glaucoma, vertigo and laparoscopic cholecystectomy for acute calculous cholecystitis in 2009, which was complicated by postoperative bile leakage that was treated with the insertion of a plastic biliary stent. Two years later, ERCP was carried out due to obstructive jaundice and previous acute cholangitis. The stent was removed with some degree of difficulty and the patient was discharged from hospital the day after the procedure. He returned to our Emergency Department 48h later due to general malaise and fever. He was hemodynamically stable and presented jaundice, generalized subcutaneous crepitation and tenderness in the epigastrium and right hypochondrium. Blood tests showed: leukocytes 9020, 87.5% PMN, total bilirubin 8.18g/dl, direct bilirubin 7.62g/dl, CRP 19.90mg/dl. Abdominal CT demonstrated dilated intra- and extrahepatic bile duct, and abundant free air distributed in the retroperitoneal/intraperitoneal spaces and subcutaneous tissue. No collections or free fluid were observed (Figs. 1 and 2). After assessing the patient and considering the hemodynamic stability and improvement after antibiotic therapy, we decided on conservative management and the patient was transferred to intensive care. Symptoms improved and the patient was moved to the hospital ward, where he eventually died after suffering kidney failure.
Perforation after ERCP usually occurs in the retroperitoneal portion of the duodenum6 and air diffuses through the perineural and perivascular sheaths, which are damaged by the pressure that the endoscope exerts on the wall of the duodenum.7 Risk factors include older age, difficulty and duration of the procedure, the presence of diverticula in the periampullary area, anatomical abnormalities (Billroth II), dilatation or stenosis of the bile duct and sphincter of Oddi dysfunction.8
According to Stapfer, these lesions are classified as type I (perforation in the medial or lateral duodenal wall), type II (periampullary), type III (bile duct or pancreatic injury) and type IV (retroperitoneal air).5 79% of perforations are suspected at the time of ERCP.5 Early diagnosis increases the chances of successful conservative treatment.8 Clinical manifestations are nonspecific, but a perforation should be suspected in any patient with abdominal or respiratory symptoms or crepitations after ERCP.4 A plain abdominal radiograph should be taken, which will show retroperitoneal air lines that increase on deep expiration.9 Abdominal CT without contrast is the test of choice to confirm the diagnosis2,4; and will show air in the intra- and retroperitoneal spaces along the inferior vena cava up to the mediastinum and pleura.4 It is important to mention that the amount of air does not correlate with the severity of the symptoms.10 Treatment of the perforation should be initially conservative4,5 and should include bowel rest, a nasogastric tube, hydration and antibiotics. Surgery is indicated for patients with persistent biliary obstruction, cholangitis, sepsis or non-response to conservative treatment.4 The type of surgery depends on the findings and can include perforation repair, drainage of abscesses, choledochojejunostomy or even pancreatoduodenectomy.5
Please cite this article as: Maturana Ibáñez V, Ferrer Márquez M, Moreno Serrano A, Rodríguez Morillas D, Belda Lozano R. Manejo del retroneumoperitoneo tras CPRE. Cir Esp. 2013;91:608–609.