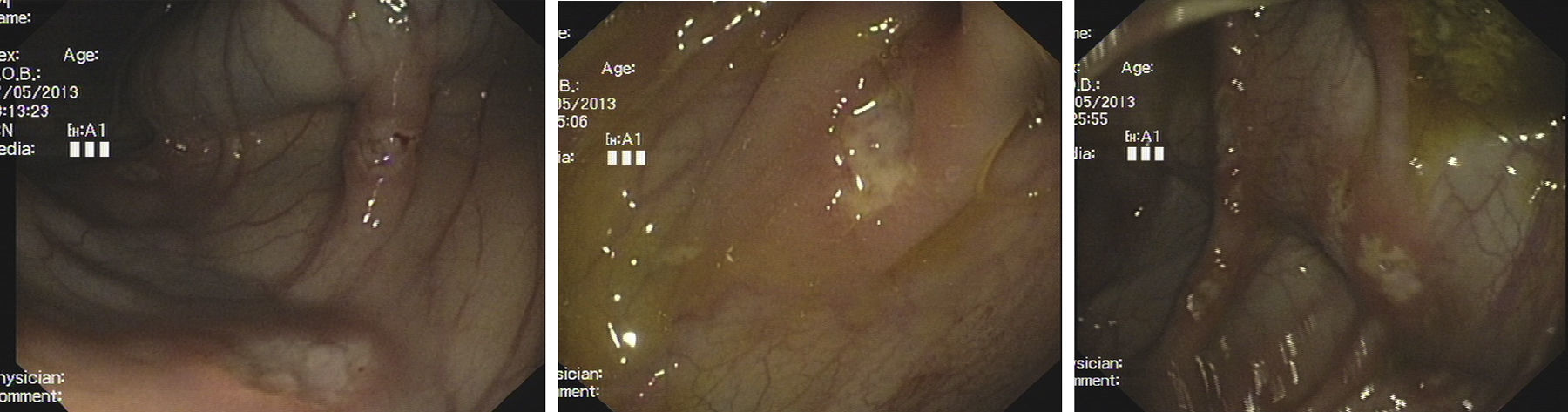
Caucasian 7-year-old boy of Spanish origin admitted due to abdominal pain and mucus and blood in the stool for 3 months, sporadic arthralgia, and asthenia and low-grade fever in the last 12 days, with no other prior history. Physical examination: asthenia and pallor with no other findings. Weight 22.3kg (−0.94 SD), height 124cm (−1.10 SD) and body mass index (BMI) 14.5kg/m2 (−0.84 SD). Leukocytosis 24,400cell/μl (17,700neutrophils/μl), haemoglobin 9.3g/dl (MCV 65.1fl, MCH 20.2pg), platelets 762,000μl and CRP 129.7mg/l, normal transaminases, serum albumin 2.7g/dl, serum iron 10.5μg/dl (50–170); negative antigliadin and IgA anti-transglutaminase antibodies, elevated faecal calprotectin (929μg/g). Negative HIV and HBV serology. Negative coproculture and parasites. The abdominal ultrasound revealed ileal loop wall thickening (7mm). No gastroduodenal or intestinal transit abnormalities found. The colonoscopy revealed pale mucosa with punched-out ulcers, particularly in the caecum and ascending colon, and the oedematous and stenotic ileocaecal valve with fibrin-covered superficial circumferential ulcers (Figs. 1–3).
Clinical courseGiven that Crohn's disease (CD) was initially suspected, induction treatment was started with exclusive polymeric enteral nutrition. Before initiating treatment with immunomodulators, a tuberculin skin test was performed, with a 12mm induration at 72h and a diagnosis of tuberculosis infection. The chest X-ray showed upper left lobe condensation. Positive gastric aspirate smear microscopy, Xpert MTB PCR positive for Mycobacterium tuberculosis (M. tuberculosis) and Lowenstein culture with Mycobacterium tuberculosis growth in fewer than 7 days and sensitive to first-line drugs. Intestinal histology showed ulcerative and granulomatous colitis in the caecum, with minor involvement of the ascending and descending colon, sigmoid and rectum. In the biopsy samples, the Ziehl-Neelsen stain, PCR and Lowenstein culture were all positive. Conventional treatment was started (induction: 2 HRZ, maintenance: 7 HR); triple therapy against pan-susceptible bacteria was prescribed for 9 months due to the extrapulmonary location and severity of clinical symptoms. Exclusive polymeric enteral nutrition formula was added for 8 weeks as coadjuvant therapy. Upon completion of treatment, the child was asymptomatic with recovered anthropometric parameters: weight: 28.3kg (−0.38 SD), height: 129.5cm (−0.96 SD) and BMI: 16.88kg/m2 (−0.38 SD). Follow-up gastroscopy and colonoscopy without findings and with normal histology.
Final commentIn 2013, the incidence of childhood tuberculosis in Spain was 5.4/100,000 population, with intestinal tuberculosis (IT) accounting for 0.5% of all cases.1 It is primarily caused by the bacteria M. tuberculosis and the ileocaecal region is most commonly affected.2
The clinical manifestations of IT are nonspecific and develop slowly,3–5 resulting in a delayed diagnosis.2 Abdominal pain and fever are the most common symptoms, together with weight loss, asthenia and episodes of diarrhoea or constipation. Intestinal obstruction is the most common complication.3 Laboratory tests are nonspecific, with elevated reactants, anaemia and lymphocytopaenia or leukocytosis4 all manifesting in our patient. The tuberculin skin test and interferon-gamma release assays offer limited sensitivity in IT diagnosis owing to the functional immunodeficiency caused by malnutrition that many of these patients suffer.2
Abdominal ultrasound and computed tomography may be useful in diagnosing the extent of the disease, although findings tend to be largely nonspecific.4
Colonoscopy shows the most commonly affected region to be the ileocaecal valve. Intestinal lesions usually manifest in the form of multiple superficial and circumferential ulcers with normal surrounding mucosa, instead of linear ulcers surrounded by inflamed and nodular mucosa typical of Crohn's disease.6,7
The differential diagnosis with CD poses a real challenge. The histology is similar in both conditions, although deep ulcers, lymphoid aggregates, transmural inflammation and non-caseating granuloma are more typical of CD, whereas large caseating and coalescent granuloma are suggestive of IT.8
IT diagnosis is confirmed by detecting the bacteria in the histological sample. However, the low sensitivity and specificity of traditional microbiological techniques, coupled with slow bacterial growth, limit the usefulness of these techniques.9 PCR to detect M. tuberculosis is a rapid and useful method of diagnosing pulmonary and extrapulmonary tuberculosis.10
Subacute tuberculous enteritis is treated using classic regimens. Clinical response is apparent less than 2 weeks after treatment initiation, and patients should be reassessed in the event of a lack of response.4
We have presented this case due to its epidemiological and clinical interest, and due to the diagnostic difficulties encountered. High clinical suspicion in this field is essential to ensure early diagnosis and treatment.
Conflicts of interestThe authors declare that they have no conflicts of interest concerning the preparation and publication of this article.
Please cite this article as: Plácido Paias R, Rodríguez Martínez A, Falcón Neyra MD. Dolor abdominal y astenia en niño de 7 años. Enferm Infecc Microbiol Clin. 2017;35:260–261.