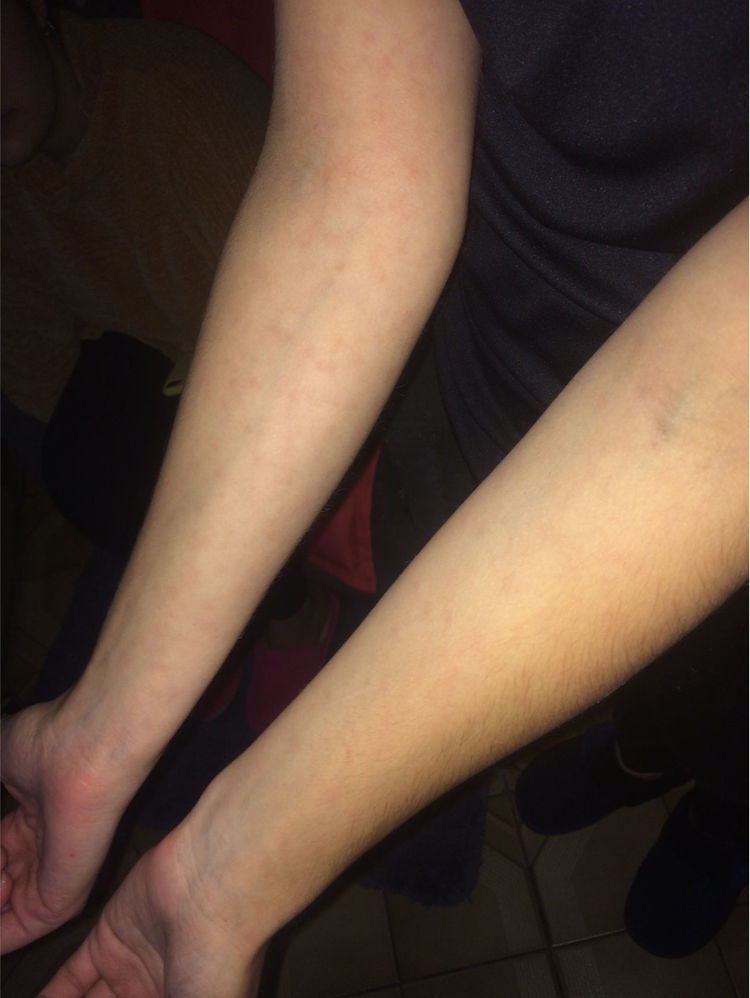Syphilis is an infectious disease caused by Treponema pallidum (T. pallidum). It has historically been seen as one of the great simulators in medicine, particularly in its secondary stage1. This disease remains a public health challenge, with 6.3 million new cases diagnosed each year worldwide2. As such, it should always be considered in the differential diagnosis of a multitude of clinical conditions, including some nephropathies.
We report the case of a 24-year-old woman who presented with a four-day history of facial oedema, nausea and decreased urine output. She was afebrile and had bipalpebral oedema without limb involvement. Laboratory testing revealed a creatinine level of 2.5 mg/dl, a normal complete blood count and an erythrocyte sedimentation rate (ESR) of 87 mm/h. C-reactive protein was 9 mg/l (normal <5 mg/l) and urinalysis showed proteinuria without haematuria, with a microalbuminuria level of 30 mg/dl. A phenomenon of autoimmune aetiology was suspected. The patient was prescribed prednisone 5 mg/day. Facial oedema abated and creatinine level fell to 1.9 mg/dl, while proteinuria persisted. Her ESR increased to 104 mm/h and non-confluent erythematous macules appeared on her trunk and upper limbs (Fig. 1), with no palmoplantar involvement. She was prescribed prednisone 20 mg/day and progressed without oedema. The skin lesions present became hyperpigmented, haemoglobin fell to 9.9 g/dl and creatinine dropped to 1.5 mg/dl, with a normal complete urinalysis and a 24-h urine protein of 1.5 g. A kidney ultrasound was normal. Rheumatological tests were negative for rheumatoid factor, antinuclear antibodies and antineutrophil cytoplasmic antibodies, and normal for complement C3 and C4, while a direct Coombs test was negative. The infectious diseases study was negative for human immunodeficiency virus (HIV) and hepatitis B virus (HBV), with a positive Venereal Disease Research Laboratory (VDRL) test at a titre of 1:64 and a positive microhaemagglutination assay for Treponema pallidum antibodies (MHA-TP). The patient's results for these exams had been negative one year prior and she denied high-risk behaviour. Secondary syphilis with kidney disease was diagnosed, and benzathine penicillin 2.4 million IU for three weeks was prescribed. A post-treatment check-up no signs or symptoms, a creatinine level of 1.0 mg/dl, a microalbuminuria level of 2.6 mg/dl, a normal complete urinalysis, an ESR of 50 mm/h and a haemoglobin level of 11.5 g/dl. VDRL titres fell to 1:16 five weeks after starting treatment.
Secondary signs in a context of haematogenous dissemination of T. pallidum appear six to eight weeks after the primary syphilitic lesion (chancre). These secondary signs may include fever, maculopapular rash with characteristic palmoplantar involvement, lymphadenopathy, hepatosplenomegaly and kidney disease, among many others. Renal involvement has been reported in secondary, latent and tertiary syphilis3. In 1935, in a series of more than 1000 patients with syphilis, Herman and Marr found that 7.1% of patients had proteinuria and 0.28% had nephropathy4. Over the last 25 years, fewer than 20 cases of renal involvement have been reported. The most common presentation consists of non-nephrotic proteinuria with normal kidney function. Today, the most common glomerulopathy is membranous nephropathy. An immunohistochemical study may reveal a “full-house” pattern, i.e. a pattern with deposition of a broad spectrum of components, including IgA, IgG, IgM, C3 and C1q5. Mesangioproliferative glomerulonephritis, rapidly progressive crescentic glomerulonephritis and minimal change disease have also been reported. The initial event is believed to be the glomerular deposition of immune complexes consisting of anti-treponemal antibodies and treponemal antigens6. Non-glomerular involvement has been observed as a sign of interstitial nephritis7. In addition, some cases of associated vasculopathy have been reported, and some cases have presented as a renal mass, known as a renal gumma8. The diagnostic criteria to determine whether or not a glomerulopathy is syphilitic are: positive treponemal serology in a patient with nephrotic syndrome and complete remission after penicillin therapy, or a finding of anti-treponemal antibodies or antigens in glomerular deposits in a histological study9. In terms of treatment, although there are differences in the various cases reported, with benzathine penicillin regimens of 2.4 million IU ranging from one to three doses, the single-dose regimen is the most widely accepted10.
In conclusion, although kidney disease in syphilis is uncommon, it should be taken into consideration when examining patients with glomerulopathy, particularly those who are sexually active and have membranous nephropathy. Antibiotic therapy remains highly effective, generally resulting in complete remission of renal impairment.
Please cite this article as: Erlij D, Sepúlveda P. Compromiso renal en sífilis secundaria: a propósito de un caso. Enferm Infecc Microbiol Clin. 2021;39:416–417.