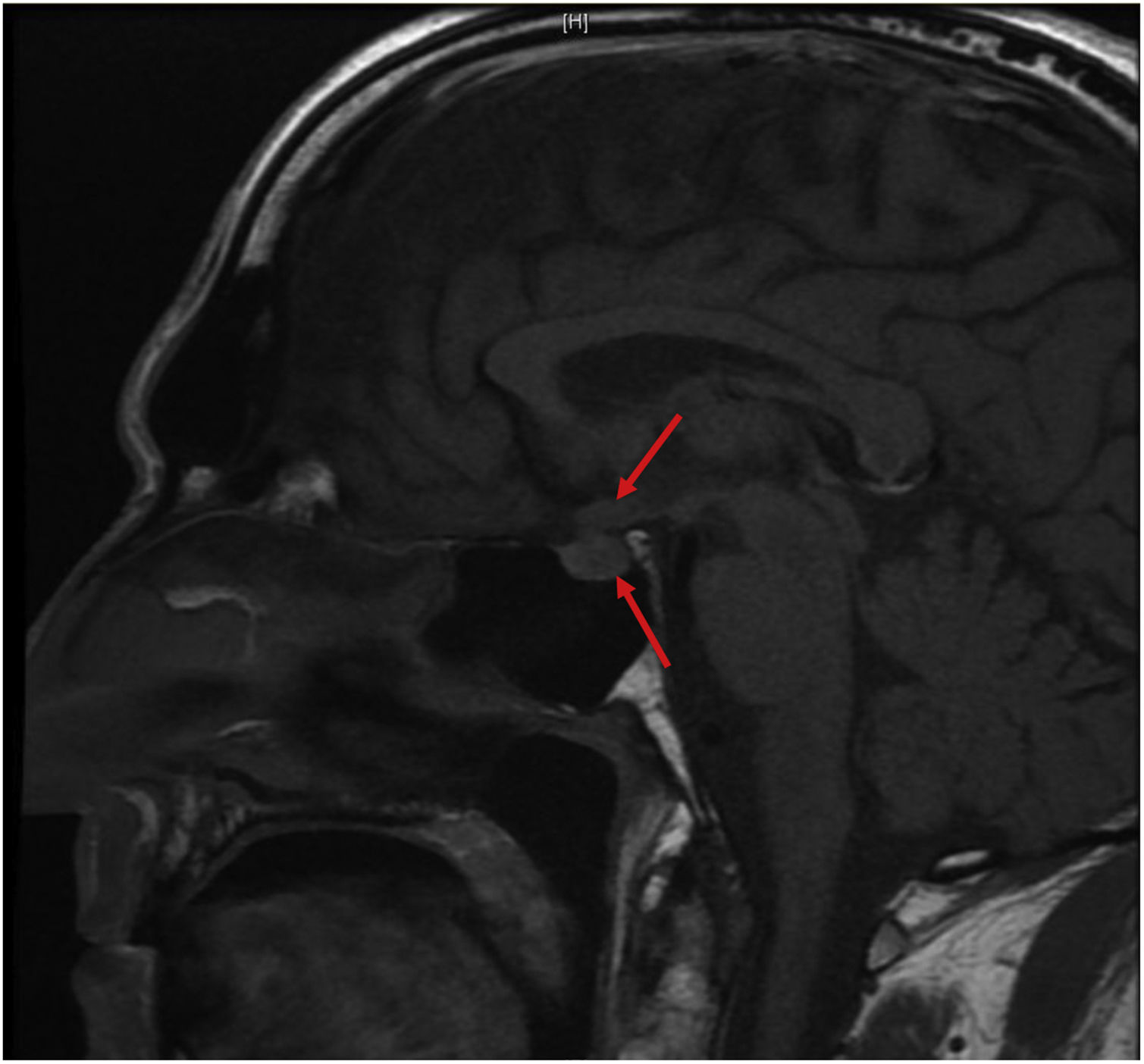
array:24 [ "pii" => "S2387020621003624" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.04.065" "estado" => "S300" "fechaPublicacion" => "2021-08-13" "aid" => "5253" "copyright" => "Elsevier España, S.L.U.. All rights reserved" "copyrightAnyo" => "2020" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:152-3" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S0025775320303717" "issn" => "00257753" "doi" => "10.1016/j.medcli.2020.04.034" "estado" => "S300" "fechaPublicacion" => "2021-08-13" "aid" => "5253" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:152-3" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Carta al Editor</span>" "titulo" => "Diabetes insípida y diabetes mellitus diagnosticadas al mismo tiempo en un varón con histiocitosis de células de Langerhans" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "152" "paginaFinal" => "153" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Diabetes insipidus and diabetes mellitus diagnosed at the same time in a male with Langerhans cell histiocytosis" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figura 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1123 "Ancho" => 1207 "Tamanyo" => 99120 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Imagen sagital de la RMN hipofisaria en secuencia T1 donde se observa el tallo engrosado (flecha superior) y la «falta de brillo» de la neurohipófisis (flecha inferior).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Guillermo Serra Soler, Carlos Antich Barceló, Honorato García Fernández" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Guillermo" "apellidos" => "Serra Soler" ] 1 => array:2 [ "nombre" => "Carlos" "apellidos" => "Antich Barceló" ] 2 => array:2 [ "nombre" => "Honorato" "apellidos" => "García Fernández" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2387020621003624" "doi" => "10.1016/j.medcle.2020.04.065" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621003624?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775320303717?idApp=UINPBA00004N" "url" => "/00257753/0000015700000003/v3_202112201214/S0025775320303717/v3_202112201214/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2387020621003491" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.05.053" "estado" => "S300" "fechaPublicacion" => "2021-08-13" "aid" => "5299" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:153-4" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Intrapancreatic accessory spleen" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "153" "paginaFinal" => "154" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Bazo accesorio intrapancreático" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 868 "Ancho" => 3333 "Tamanyo" => 312001 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Abdominal computed tomography scan depicting (white arrow) round homogeneous contrast-enhancing lesion in the pancreatic tail well-delineated from the pancreas parenchyma (A) and macroscopic appearance of the intrapancreatic splenule (white arrows) (B and C).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Milan Radojkovic, Danijela Radojkovic, Natalija Premovic" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Milan" "apellidos" => "Radojkovic" ] 1 => array:2 [ "nombre" => "Danijela" "apellidos" => "Radojkovic" ] 2 => array:2 [ "nombre" => "Natalija" "apellidos" => "Premovic" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S0025775320304668" "doi" => "10.1016/j.medcli.2020.05.031" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775320304668?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621003491?idApp=UINPBA00004N" "url" => "/23870206/0000015700000003/v3_202201060717/S2387020621003491/v3_202201060717/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2387020621003363" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.04.062" "estado" => "S300" "fechaPublicacion" => "2021-08-13" "aid" => "5298" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:151-2" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:10 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Unexpected finding of intravascular large B-cell lymphoma by a skin biopsy" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "151" "paginaFinal" => "152" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Hallazgo casual de un linfoma de células grandes B intravascular tras una biopsia cutánea a ciegas" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Santiago Guillen-Climent, Alejandro García-Vázquez, Carolina Martínez-Ciarpaglini" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Santiago" "apellidos" => "Guillen-Climent" ] 1 => array:2 [ "nombre" => "Alejandro" "apellidos" => "García-Vázquez" ] 2 => array:2 [ "nombre" => "Carolina" "apellidos" => "Martínez-Ciarpaglini" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0025775320304656" "doi" => "10.1016/j.medcli.2020.04.051" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775320304656?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621003363?idApp=UINPBA00004N" "url" => "/23870206/0000015700000003/v3_202201060717/S2387020621003363/v3_202201060717/en/main.assets" ] "en" => array:15 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Diabetes insipidus and diabetes mellitus diagnosed at the same time in a male with Langerhans cell histiocytosis" "tieneTextoCompleto" => true "saludo" => "Dear Editor:" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "152" "paginaFinal" => "153" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Guillermo Serra Soler, Carlos Antich Barceló, Honorato García Fernández" "autores" => array:3 [ 0 => array:4 [ "nombre" => "Guillermo" "apellidos" => "Serra Soler" "email" => array:1 [ 0 => "gserseol@hotmail.com" ] "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "*" "identificador" => "cor0005" ] ] ] 1 => array:2 [ "nombre" => "Carlos" "apellidos" => "Antich Barceló" ] 2 => array:2 [ "nombre" => "Honorato" "apellidos" => "García Fernández" ] ] "afiliaciones" => array:1 [ 0 => array:2 [ "entidad" => "Departamento de Endocrinología, Hospital Universitari Son Espases. Palma de Mallorca, Balearic Islands, Spain" "identificador" => "aff0005" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Diabetes insípida y diabetes mellitus diagnosticadas al mismo tiempo en un varón con histiocitosis de células de Langerhans" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1404 "Ancho" => 1509 "Tamanyo" => 119004 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Sagittal image of the pituitary T1-weighted sequence MRI showing the thickened infundibulum (upper arrow) and the posterior pituitary “bright spot absence” (lower arrow).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">Langerhans cell histiocytosis (LCH) is a rare disease characterized by the proliferation and infiltration of Langerhans cells in one or more organs. The most common endocrine disorders are diabetes insipidus (DI) and anterior pituitary deficiency (APD). Diabetes mellitus (DM) and thyroid involvement are less common. MD and DI present with polyuria and polydipsia, but with distinct biochemical parameters in blood and urine. Although DM is the most common in the population, we should not ignore the possibility that a patient with LCH may have DI or both at the same time, delaying the diagnosis of DI. We report the case of a 61-year-old man with LCH diagnosed with DI and DM at the same time. He was a smoker, had dyslipidaemia, was overweight with a body mass index (BMI) of 25.5 kg/m<span class="elsevierStyleSup">2</span> and LCH diagnosed 8 years earlier, with lung and liver involvement. The patient had not received systemic treatment. No family history of DM. He reported intense polyuria, polydipsia, and weight loss for 15 days, prompting a visit to the health centre. Lab tests showed hyperglycaemia: 121 mg/dl (70–100), HbA<span class="elsevierStyleInf">1 C</span>: 6.6% (< 6.1%) and hypernatremia: 152 mg/dl (136–145) and was diagnosed with DM2, initiating treatment with metformin. Despite treatment, his polyuria did not improve, and he went to the hospital. Physical examination revealed mucosal dehydration. A polyuria of 9 l/day was observed. Laboratory tests showed hypernatremia: 152 mEq/l; hyperosmolarity: 298 mosm/kg (275–295); urinary hypoosmolarity: 133 mosm/kg (50–1,400), diagnosing DI. He also had hyperglycaemia: 137 mg/dl (70-110); HbA<span class="elsevierStyleInf">1 C</span>: 6.5% (3.8–6.2%) and normal C-peptide. The liver profile showed anomalies, except for bilirubin, which was normal. Pituitary hormones were normal, except for an undetectable vasopressin. Pituitary T1-weighted sequence MRI showed a thickened 4.5 mm infundibulum and posterior pituitary “bright spot absence” (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>). The thoraco-abdominal CT showed a reticular pattern in the upper lung fields and hepatomegaly with several solid lesions. Thyroid ultrasound revealed a 1 cm right thyroid lobe nodule. PET/CT showed active pituitary disease. Treatment with desmopressin and metformin was initiated. He did not receive chemotherapy (CT) or radiotherapy (RT). Desmopressin 240 µg and metformin 1,275 mg/day were prescribed at discharge and outpatient follow-up was arranged. After 10 months, the patient reported sexual anaesthesia, showing hypogonadotropic hypogonadism on laboratory tests. He had euglycemia: 108 mg/dl; HbA<span class="elsevierStyleInf">1 C</span>: 6%; natremia: 137 mg/dl and LDLc 217 mg/dl. Treatment with 50 mg testosterone gel and atorvastatin 20 mg/day was started.</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0010" class="elsevierStylePara elsevierViewall">DI is the most common endocrinological disorder in LCH (30%), which can increase to 40% when there is multisystem involvement. It can be the first manifestation or develop years after diagnosis and is usually permanent.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> In our case, 8 years had passed. APD occurs in 20% of cases, usually accompanied by DI. GH and gonadotropin deficiency are the most common (50–67%).<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1,2</span></a> Although some studies have suggested that these deficiencies are caused by the CT and/or RT received, it seems that they are due to the natural course of the disease,<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> and occur over time, such as the hypogonadotropic hypogonadism observed in our case which occurred 10 months after DI. Posterior pituitary bright spot absence in the t1-weighted pituitary MRI is present in almost all cases with DI, together with a thickening of the infundibulum (71–78%), hypothalamic lesions (8–18%) and enlargement of the pituitary gland (16%).<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1,2</span></a> Hormone deficiency will be treated by replacement therapy. Once established, they usually do not respond to any systemic treatment. Thyroid involvement may occur in isolation or in the context of systemic LCH and present as a multinodular or single nodule goiter.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> In our case there was a 1 cm nodule with benign characteristics. LCH has been associated with metabolic disturbances such as impaired fasting glucose, glucose intolerance (21–28%), DM (5–7%) and, occasionally, hypercholesterolemia (17%), hypertriglyceridemia (28 %) and hypertension (17%), which increase cardiovascular risk.<a class="elsevierStyleCrossRefs" href="#bib0015"><span class="elsevierStyleSup">3,4</span></a> These glucose impairments may be due to insulin resistance caused by the disease itself, which is considered an inflammatory neoplasm, especially in multisystemic forms, liver infiltration, overweight, obesity (central in cases with hypothalamic involvement) and treatments such as corticosteroids; and to insulin deficiency caused by pancreatic islet infiltration.<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">4</span></a> Sollier et al. describe a patient with LCH, DI and type B insulin resistance positive for anti-insulin receptor antibodies as a cause of DM.<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a> Our case presented with multisystem LCH with liver involvement and mild overweight. Sometimes DI and DM can occur simultaneously, delaying the diagnosis of DI if it is not suspected, as in our case, since the patient had significant polyuria and hypernatremia from the outset. Regular screening for DI and APD is recommended in systemic forms. Thyroid assessment is also recommended, as well as screening and treatment of cardiovascular risk factors.</p></span>" "pdfFichero" => "main.pdf" "tienePdf" => true "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Serra Soler G, Antich Barceló C, García Fernández H. Diabetes insípida y diabetes mellitus diagnosticadas al mismo tiempo en un varón con histiocitosis de células de Langerhans. Med Clin (Barc). 2021;157:58–59.</p>" ] ] "multimedia" => array:1 [ 0 => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1404 "Ancho" => 1509 "Tamanyo" => 119004 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Sagittal image of the pituitary T1-weighted sequence MRI showing the thickened infundibulum (upper arrow) and the posterior pituitary “bright spot absence” (lower arrow).</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:5 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "The pituitary gland in patients with Langerhans cell histiocytosis: a clinical and radiological evaluation" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "N. Kurtulmus" 1 => "M. Mert" 2 => "R. Tanakol" 3 => "S. Yarman" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s12020-014-0408-6" "Revista" => array:6 [ "tituloSerie" => "Endocrine" "fecha" => "2015" "volumen" => "48" "paginaInicial" => "949" "paginaFinal" => "956" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/25209890" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endocrine changes in histiocytosis of the hypothalamic-pituitary axis" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "S. Toro Galván" 1 => "A. Planas Vilaseca" 2 => "T. Michalopoulou Alevras" 3 => "A. Torres Díaz" 4 => "J. Suárez Balaguer" 5 => "C. Villabona Artero" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.endonu.2014.10.004" "Revista" => array:6 [ "tituloSerie" => "Endocrinol Nutr" "fecha" => "2015" "volumen" => "62" "paginaInicial" => "72" "paginaFinal" => "79" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/25434508" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Endocrine and metabolic assessment in adults with Langerhans cell histiocytosis" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "L. Montefusco" 1 => "S. Harari" 2 => "D. Elia" 3 => "A. Rossi" 4 => "C. Specchia" 5 => "O. Torre" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.ejim.2017.11.011" "Revista" => array:6 [ "tituloSerie" => "Eur J Intern Med" "fecha" => "2018" "volumen" => "51" "paginaInicial" => "61" "paginaFinal" => "67" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29198444" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Cardiovascular risk factors in adult patients with multisystem Langerhans-cell histiocytosis: evidence of glucose metabolism abnormalities" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "K.I. Alexandraki" 1 => "P. Makras" 2 => "A.D. Protogerou" 3 => "K. Dimitriou" 4 => "A. Stathopoulou" 5 => "D.S. Papadogias" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1093/qjmed/hcm118" "Revista" => array:6 [ "tituloSerie" => "QJM" "fecha" => "2008" "volumen" => "101" "paginaInicial" => "31" "paginaFinal" => "40" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/18160417" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Diabetes Mellitus, extreme insulin resistance, and hypothalamic-pituitary langerhans cells histiocytosis" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "M. Sollier" 1 => "M. Halbron" 2 => "J. Donadieu" 3 => "A. Idbaih" 4 => "F. Cohen Aubart" 5 => "C. Vigouroux" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:5 [ "tituloSerie" => "Case Rep Endocrinol" "fecha" => "2019" "volumen" => "23" "paginaInicial" => "1" "paginaFinal" => "8" ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/23870206/0000015700000003/v3_202201060717/S2387020621003624/v3_202201060717/en/main.assets" "Apartado" => array:4 [ "identificador" => "43309" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Letters to the Editor" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/23870206/0000015700000003/v3_202201060717/S2387020621003624/v3_202201060717/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621003624?idApp=UINPBA00004N" ]
Journal Information
Vol. 157. Issue 3.
Pages 152-153 (August 2021)
Share
Download PDF
More article options
Vol. 157. Issue 3.
Pages 152-153 (August 2021)
Letter to the Editor
Diabetes insipidus and diabetes mellitus diagnosed at the same time in a male with Langerhans cell histiocytosis
Diabetes insípida y diabetes mellitus diagnosticadas al mismo tiempo en un varón con histiocitosis de células de Langerhans
Guillermo Serra Soler
, Carlos Antich Barceló, Honorato García Fernández
Corresponding author
Departamento de Endocrinología, Hospital Universitari Son Espases. Palma de Mallorca, Balearic Islands, Spain
Article information
These are the options to access the full texts of the publication Medicina Clínica (English Edition)
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail