Artículo
Comprando el artículo el PDF del mismo podrá ser descargado
Precio 19,34 €
Comprar ahora
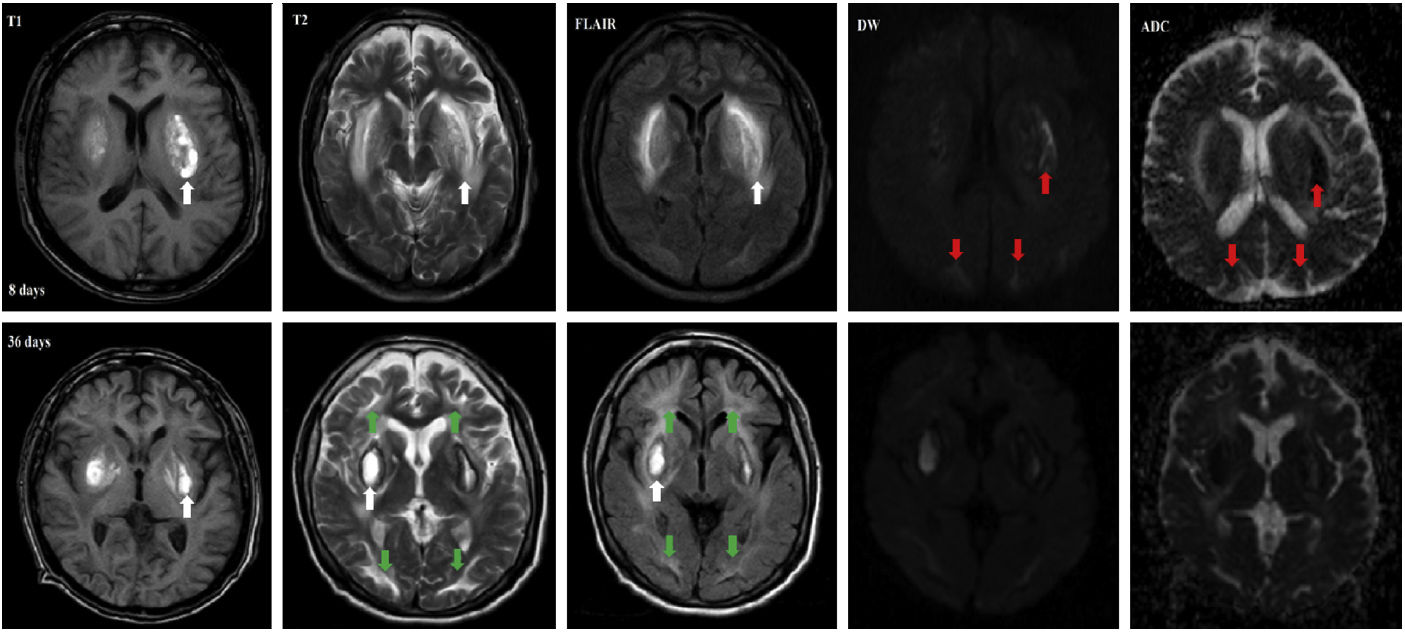
array:23 [ "pii" => "S0025775319306189" "issn" => "00257753" "doi" => "10.1016/j.medcli.2019.09.016" "estado" => "S300" "fechaPublicacion" => "2020-12-24" "aid" => "5019" "copyright" => "Elsevier España, S.L.U.. All rights reserved" "copyrightAnyo" => "2019" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Med Clin. 2020;155:557-8" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "itemSiguiente" => array:19 [ "pii" => "S0025775319306177" "issn" => "00257753" "doi" => "10.1016/j.medcli.2019.09.015" "estado" => "S300" "fechaPublicacion" => "2020-12-24" "aid" => "5018" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "crp" "cita" => "Med Clin. 2020;155:558-9" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "es" => array:10 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Carta científica</span>" "titulo" => "La albúmina como marcador pronóstico en el implante de válvula aórtica percutánea" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "558" "paginaFinal" => "559" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Albumin as a prognostic marker in the percutaneous aortic valve replacement" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Luisa Salido Tahoces, Ana Pardo Sanz, José Luis Zamorano-Gómez" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Luisa" "apellidos" => "Salido Tahoces" ] 1 => array:2 [ "nombre" => "Ana" "apellidos" => "Pardo Sanz" ] 2 => array:2 [ "nombre" => "José Luis" "apellidos" => "Zamorano-Gómez" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2387020620305374" "doi" => "10.1016/j.medcle.2019.09.013" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020620305374?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775319306177?idApp=UINPBA00004N" "url" => "/00257753/0000015500000012/v1_202012131718/S0025775319306177/v1_202012131718/es/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S0025775320304498" "issn" => "00257753" "doi" => "10.1016/j.medcli.2020.07.002" "estado" => "S300" "fechaPublicacion" => "2020-12-24" "aid" => "5289" "copyright" => "Elsevier España, S.L.U." "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Med Clin. 2020;155:548-56" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Special article</span>" "titulo" => "Anti-IL-6 receptor antibody treatment for severe COVID-19 and the potential implication of <span class="elsevierStyleItalic">IL-6</span> gene polymorphisms in novel coronavirus pneumonia" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "548" "paginaFinal" => "556" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Tratamiento con anticuerpos anti-receptor de IL-6 para COVID-19 grave y la posible implicación de polimorfismos del gen IL-6 en la nueva neumonía por coronavirus" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 3440 "Ancho" => 3167 "Tamanyo" => 649602 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">(A) Forest plot of studies reporting hazard ratio (HR) that investigates the mortality rate between Tocilizumab (TCZ) group and standard treatment (STD) group. (B–E) Forest plot of pooled studies evaluating mortality rate, invasive mechanical ventilation (IMV) requirement, ICU admissions, and the number of discharged patients between Tocilizumab (TCZ) group and standard treatment (STD) group, respectively.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Zulvikar Syambani Ulhaq, Gita Vita Soraya" "autores" => array:2 [ 0 => array:2 [ "nombre" => "Zulvikar Syambani" "apellidos" => "Ulhaq" ] 1 => array:2 [ "nombre" => "Gita Vita" "apellidos" => "Soraya" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2387020620305519" "doi" => "10.1016/j.medcle.2020.07.014" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020620305519?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775320304498?idApp=UINPBA00004N" "url" => "/00257753/0000015500000012/v1_202012131718/S0025775320304498/v1_202012131718/en/main.assets" ] "en" => array:15 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Cartas científicas</span>" "titulo" => "Late leukoencephalopathy in patients with methanol intoxication" "tieneTextoCompleto" => true "saludo" => "Dear Editor:" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "557" "paginaFinal" => "558" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Dannys Rivero Rodriguez, Kimberly Sam, Michelle Bravo" "autores" => array:3 [ 0 => array:4 [ "nombre" => "Dannys" "apellidos" => "Rivero Rodriguez" "email" => array:1 [ 0 => "dannyriverorodriguez@gmail.com" ] "referencia" => array:3 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] 2 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Kimberly" "apellidos" => "Sam" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 2 => array:3 [ "nombre" => "Michelle" "apellidos" => "Bravo" "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">c</span>" "identificador" => "aff0015" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">d</span>" "identificador" => "aff0020" ] ] ] ] "afiliaciones" => array:4 [ 0 => array:3 [ "entidad" => "San Francisco University of Quito USFQ, Ecuador" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Neurology Department, Eugenio Espejo Hospital, Quito, Ecuador" "etiqueta" => "b" "identificador" => "aff0010" ] 2 => array:3 [ "entidad" => "Neurology Department, Donald, United States" "etiqueta" => "c" "identificador" => "aff0015" ] 3 => array:3 [ "entidad" => "Barbara Zucker School of Medicine at Hofstra/Northwell, United States" "etiqueta" => "d" "identificador" => "aff0020" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Leucoencefalopatía tardía posterior a intoxicación por metanol" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 633 "Ancho" => 1405 "Tamanyo" => 119048 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Patient 1. (P<span class="elsevierStyleInf">1</span>) MRI Scan | MRI demonstrates bilateral hemorrhagic necrosis (white arrows) of the putamen, displaying the T1WI, T2WI, FLAIR, DWI, and ADC images. On day 8, the DWI is positive in the putamen and occipital lobe (red arrows), suggesting evidence of cytotoxic edema with acute leukoencephalopathy. At 36 days (B), signal hyperintensity in the subcortical/occipital and frontal white matter shows progression towards chronic leukoencephalopathy (green arrows) (high signal intensity on T2WI, FLAIR, DWI and ADC, T2 shine-through effect).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">Methanol is a clear substance with pronounced similarities in flavor and aroma to ethanol. It is highly toxic to the CNS and damage to the optic nerve and basal ganglia, accompanied by severe metabolic acidosis, have been observed within hours following ingestion. Common clinical manifestations of methanol intoxication (MI) include blindness, headache, abdominal pain, drowsiness, seizures, coma, and death.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a></p><p id="par0010" class="elsevierStylePara elsevierViewall">The most recurrent neuroradiological finding demonstrated by CT and MR imaging (MRI) is putaminal necrosis, with varying degrees of putaminal hemorrhage; however, optic nerve damage and white and grey matter lesions in various locations have also been reported, though less frequently.</p><p id="par0015" class="elsevierStylePara elsevierViewall">In this study, we report two patients (P<span class="elsevierStyleInf">1, 2</span>) with accidental methanol ingestion who developed late toxic leukoencephalopathy. The symptoms most frequently reported during the first medical evaluation (6-h after ingestion) were abdominal pain, headache, diaphoresis, and declined visual acuity. The progressive decrease in Glasgow coma score (GCS) during the initial 24<span class="elsevierStyleHsp" style=""></span>h (P<span class="elsevierStyleInf">1</span>, 13-9/15-GCS. P<span class="elsevierStyleInf">2</span>, 15-12/15-GCS) of hospitalization, coupled with metabolic acidosis (P<span class="elsevierStyleInf">1</span>, PH-6.80, PCO<span class="elsevierStyleInf">2</span>-25.7, HCO<span class="elsevierStyleInf">3</span>-3.90, Lactic acid-12.1<span class="elsevierStyleHsp" style=""></span>mmol/L. P<span class="elsevierStyleInf">2</span>, PH-7.13, PCO<span class="elsevierStyleInf">2</span>-12.0, HCO<span class="elsevierStyleInf">3</span>-4.0, Lactic acid-1.9<span class="elsevierStyleHsp" style=""></span>mmol/L) and a notably high anion gap (P<span class="elsevierStyleInf">1</span>-41.8<span class="elsevierStyleHsp" style=""></span>mEq/l. P<span class="elsevierStyleInf">2</span>-39.0<span class="elsevierStyleHsp" style=""></span>mEq/l), suggested the diagnosis of MI. The diagnosis was confirmed after methanol levels in the blood were tested and exceeded 20<span class="elsevierStyleHsp" style=""></span>mg/dL (P<span class="elsevierStyleInf">1</span>-43<span class="elsevierStyleHsp" style=""></span>mg/l. P<span class="elsevierStyleInf">2</span>-28<span class="elsevierStyleHsp" style=""></span>mg/l).</p><p id="par0020" class="elsevierStylePara elsevierViewall">In the both cases (P<span class="elsevierStyleInf">1</span>, P<span class="elsevierStyleInf">2</span>) was it possible to perform an initial MRI scan, allowed by their stable clinical status; more than 30 days later, follow-up MRI was performed, demonstrating the progression of active toxic leukoencephalopathy (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>). In all patients, putaminal hemorrhagic necrosis was observed, with subcortical and deep white matter damage.</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0025" class="elsevierStylePara elsevierViewall">MI causes severe damage to the CNS. Putaminal hemorrhagic necrosis has been described as the most frequent radiological and clinical-pathological finding in these patients. White matter (WM) lesions are another finding seen in MI; they have been observed to be bilateral, deep, or subcortical, although occasionally the subcortical fibers have been preserved.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> There are few case studies in the literature investigating DWI findings that use follow-up MRI evaluation after MI.<a class="elsevierStyleCrossRefs" href="#bib0015"><span class="elsevierStyleSup">3,4</span></a> It is probable that the prominent obstacles leading to difficulties in studying the severity of illness is the high level of morbidity and mortality associated with MI, which can cause difficulties in performing follow-up MRI studies, and the unstable initial state of the patient upon admission.</p><p id="par0030" class="elsevierStylePara elsevierViewall">One of the few descriptions of serial MRI studies in MI patients was described in a 2006 case study. Takao et al.<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a> reported restricted diffusion in the putamen and subcortical fibers, with a putaminal lesion in the initial MRI scan. Following three days, MRI revealed a new lesion in the subcortical fibers, leading the authors to hypothesize that the new lesion was related to the cytotoxic edema observed in the first MRI scan. On the 19th day, MRI revealed progressed, hemorrhagic damage to the subcortical fibers.</p><p id="par0035" class="elsevierStylePara elsevierViewall">In our two patients, we were able to demonstrate how relatively symmetric leukoencephalopathy in the frontal and/or occipital lobes continued to worsen more than 30 days after MI. We hypothesize that the initial restricted diffusion in the subcortical fibers in the DWI, indicative of cytotoxic edema, represents an early marker of potential WM damage seen in later imaging. In the patient with more extensive leukoencephalopathy detected in the later stages of MI (P<span class="elsevierStyleInf">1</span>), we observed worsened morbidity at three months following hospital discharge, leading us to suspect that WM lesions predict poor outcome following MI. From our patients’ imaging studies, we suspect that progressive WM lesions may be a significant finding in these patients, highlighting the severity over time following MI.</p><p id="par0040" class="elsevierStylePara elsevierViewall">Further investigation of the relationship between the development of chronic leukoencephalopathy and the quantity of methanol ingested provides additional insight that can be used as a valuable predictive tool for prognostics.</p><p id="par0045" class="elsevierStylePara elsevierViewall">Due to the few studies that have conducted follow-up MRI studies during the later stages of MI, and with our sample size being small, we cannot conclude that leukoencephalopathy is a long-term finding associated with MI. Nevertheless, it is worth exploring whether there is a relationship between worsened neuronal damage on serial MRI and patient outcomes.</p><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Funding</span><p id="par0050" class="elsevierStylePara elsevierViewall">This research received no external funding.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:2 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Funding" ] 1 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "multimedia" => array:1 [ 0 => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 633 "Ancho" => 1405 "Tamanyo" => 119048 ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Patient 1. (P<span class="elsevierStyleInf">1</span>) MRI Scan | MRI demonstrates bilateral hemorrhagic necrosis (white arrows) of the putamen, displaying the T1WI, T2WI, FLAIR, DWI, and ADC images. On day 8, the DWI is positive in the putamen and occipital lobe (red arrows), suggesting evidence of cytotoxic edema with acute leukoencephalopathy. At 36 days (B), signal hyperintensity in the subcortical/occipital and frontal white matter shows progression towards chronic leukoencephalopathy (green arrows) (high signal intensity on T2WI, FLAIR, DWI and ADC, T2 shine-through effect).</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0015" "bibliografiaReferencia" => array:5 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "MRI findings in methanol intoxication: a report of two cases" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "V. Arora" 1 => "I.B. Nijjar" 2 => "A.S. Multani" 3 => "J.P. Singh" 4 => "R. Abrol" 5 => "R. Chopra" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1259/bjr/40137535" "Revista" => array:6 [ "tituloSerie" => "Br J Radiol" "fecha" => "2007" "volumen" => "80" "paginaInicial" => "e243" "paginaFinal" => "e246" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/17959915" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "CT and MR imaging findings in methanol intoxication" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "M. Blanco" 1 => "R. Casado" 2 => "F. Vázquez" 3 => "J.M. Pumar" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "AJNR Am J Neuroradiol" "fecha" => "2006" "volumen" => "27" "paginaInicial" => "452" "paginaFinal" => "454" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/16484428" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Diffusion-weighted magnetic resonance imaging in a case of methanol intoxication" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "S. Deniz" 1 => "C. Oppenheim" 2 => "S. Lehéricy" 3 => "T. Sharshar" 4 => "T.F. Lalam" 5 => "D. Dormont" ] ] ] ] ] "host" => array:1 [ 0 => array:1 [ "Revista" => array:6 [ "tituloSerie" => "Neurotoxicology" "fecha" => "2000" "volumen" => "21" "paginaInicial" => "405" "paginaFinal" => "408" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/10894130" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Conventional and diffusion-weighted MR IMAGING in the evaluation of methanol poisoning" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "A. Server" 1 => "K.E. Hovda" 2 => "P.H. Nakstad" 3 => "D. Jacobsen" 4 => "R. Dullerud" 5 => "M. Haakonsen" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1046/j.1600-0455.2003.00138.x" "Revista" => array:6 [ "tituloSerie" => "Acta Radiol" "fecha" => "2003" "volumen" => "44" "paginaInicial" => "691" "paginaFinal" => "695" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/14616218" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Serial diffusion-weighted magnetic resonance imaging in methanol intoxication" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:3 [ 0 => "H. Takao" 1 => "I. Doi" 2 => "T. Watanabe" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1097/01.rct.0000228165.16592.0d" "Revista" => array:7 [ "tituloSerie" => "J Comput Assist Tomogr" "fecha" => "2006" "volumen" => "30" "paginaInicial" => "742" "paginaFinal" => "744" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/16954921" "web" => "Medline" ] ] "itemHostRev" => array:3 [ "pii" => "S1542356518301137" "estado" => "S300" "issn" => "15423565" ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/00257753/0000015500000012/v1_202012131718/S0025775319306189/v1_202012131718/en/main.assets" "Apartado" => array:4 [ "identificador" => "66447" "tipo" => "SECCION" "es" => array:2 [ "titulo" => "Cartas científicas" "idiomaDefecto" => true ] "idiomaDefecto" => "es" ] "PDF" => "https://static.elsevier.es/multimedia/00257753/0000015500000012/v1_202012131718/S0025775319306189/v1_202012131718/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775319306189?idApp=UINPBA00004N" ]
Consulte los artículos y contenidos publicados en este medio, además de los e-sumarios de las revistas científicas en el mismo momento de publicación
Esté informado en todo momento gracias a las alertas y novedades
Acceda a promociones exclusivas en suscripciones, lanzamientos y cursos acreditados
Medicina Clínica, fundada en 1943, es la única publicación semanal de contenido clínico que se edita en España y constituye el máximo exponente de la calidad y pujanza de la medicina española. Son características fundamentales de esta publicación el rigor científico y metodológico de sus artículos, la actualidad de los temas y, sobre todo, su sentido práctico, buscando siempre que la información sea de la mayor utilidad en la práctica clínica. Los contenidos de Medicina Clínica abarcan dos frentes: trabajos de investigación original rigurosamente seleccionados atendiendo a su calidad, originalidad e interés, y trabajos orientados a la formación continuada, encomendados por la revista a autores relevantes (Editoriales, Revisiones, Conferencias clínicas y clínico-patológicas, Diagnóstico y Tratamiento). En estos artículos se ponen al día aspectos de destacado interés clínico o conceptual en la medicina actual. Medicina Clínica es un vehículo de información científica de reconocida calidad, como demuestra su inclusión en los más prestigiosos y selectivos índices bibliográficos del mundo.
Current Contents/Clinical Medicine, Journal Citation Reports, SCI-Expanded, Index Medicus/Medline, Excerpta Medica/EMBASE, IBECS, IME, MEDES, PASCAL, SCOPUS, ScienceDirect
Ver másEl factor de impacto mide la media del número de citaciones recibidas en un año por trabajos publicados en la publicación durante los dos años anteriores.
© Clarivate Analytics, Journal Citation Reports 2022
SJR es una prestigiosa métrica basada en la idea de que todas las citaciones no son iguales. SJR usa un algoritmo similar al page rank de Google; es una medida cuantitativa y cualitativa al impacto de una publicación.
Ver másSNIP permite comparar el impacto de revistas de diferentes campos temáticos, corrigiendo las diferencias en la probabilidad de ser citado que existe entre revistas de distintas materias.
Ver más¿Es usted profesional sanitario apto para prescribir o dispensar medicamentos?
Are you a health professional able to prescribe or dispense drugs?
Você é um profissional de saúde habilitado a prescrever ou dispensar medicamentos