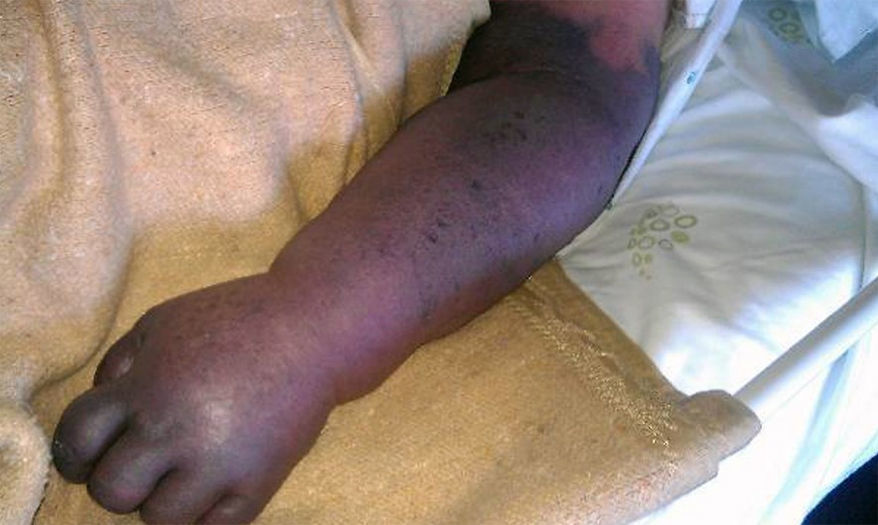
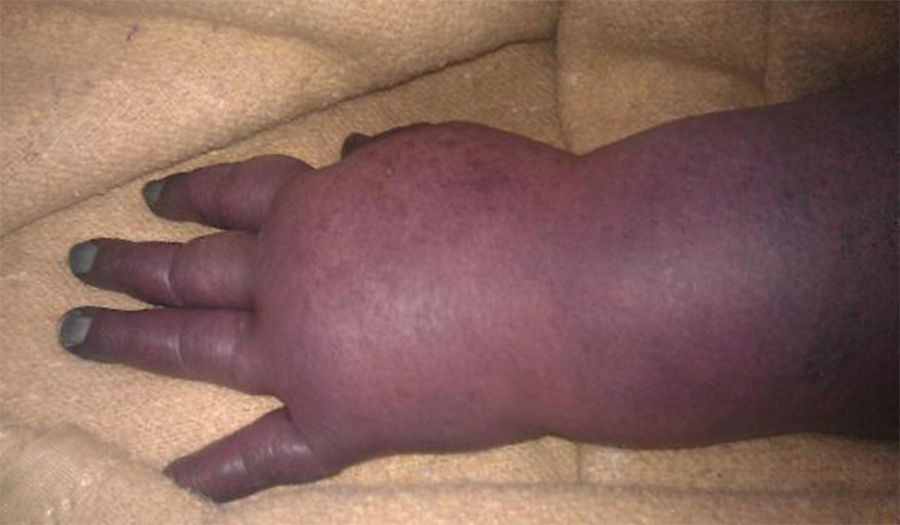
A 90-year-old female with history of atrial fibrillation (treated with a beta-blocker), right breast carcinoma diagnosed few years previously (not treated) and a 1-month history of left upperextremity deep vein thrombosis (anticoagulated with warfarin) presented to the emergency department after having had fever, dyspnoea and productive cough for two days. Physical examination revealed crackles on pulmonary auscultation and mild peripheral cyanosis of the nail beds of the left hand fingers only. Both radial pulses were present. Laboratory investigations revealed mild respiratory failure (pO2/FiO2 ratio: 268), anaemia (haemoglobin 10.4g/dL), leucocytosis with neutrophilia (WBC 15.85×109L−1, neutrophils 86%) and elevated C-reactive protein (195.6mg/L, reference value: <3.0mg/L); her INR was in the therapeutic range (2.35, reference value: 2–3). A chest radiograph showed bilateral interstitial pulmonary infiltrates. These findings were consistent with a community-acquired pneumonia, it was started amoxicillin-clavulanate and azithromycin, and the patient admitted in the internal medicine ward. After two days, the left upper-extremity was cold and markedly oedematous, the cyanosis had progressed proximally and the distal pulses were no longer palpable (Figs. 1 and 2). Laboratory examination showed a marked rhabdomyolysis (creatine kinase 3470U/L, reference value: 10–37U/L; myoglobin 2549.2ng/mL, reference value: <146.9ng/mL) and a very high D-dimer value (24.5μg/mL, reference value: < 0.50μg/mL).
An echo-doppler was performed and confirmed a left brachial-axillary-subclavian massive deep vein thrombosis (even with effective anticoagulation) and absence of distal arterial flow. The patient had a venous gangrene and an urgent surgical amputation was proposed. However she presented with circulatory collapse and shock, and died the following day.
Phlegmasia alba dolens and phlegmasia cerulea dolens predominantly affect the lower extremities, involving the upper extremities in less than 5% of the cases. The first one is known by the triad of oedema, pain and blanching (alba) without cyanosis. The onset of symptoms may be gradual or fulminant, preceding phlegmasia cerulea dolens in 50–60% of cases. With increasing cyanosis and progression, patients may develop a compartment syndrome precipitated by venous congestion. Venous gangrene and shock are the ultimate killers, so it is vital that patients be treated before reaching that stage.1–3 Malignancy is the most common triggering factor and is also associated with higher mortality.4 Phlegmasia and venous gangrene are life-threatening conditions, although rare. It is crucial for nonvascular specialists to be able to recognize this condition promptly and accurately because treatment is time-dependent.
Conflicts of interestThe authors declare no conflicts of interest.