To analyze the outcomes of distal tibia fractures with or without extension into the ankle joint, treated by percutaneous cannulated screws or locking plates.
Materials and methodsA retrospective study was conducted on 107 patients treated between 2001 and 2012. Inclusion criteria: fractures 43-A and 43-C1 and C2 according to the AO/OTA system, treated with percutaneous osteosynthesis by locking plate or two cannulated screws in X-letter setting. A total of 33 patients were evaluated: 16 tibial fractures were performed with locking plate (G1) and 17 with cannulated screws (G2). Mean time to surgery was 8.31 days (0–14) in G1, and 2 days (0–7) in G2. The mean follow-up was 72 months (12–132). Mean time to healing: 17.08 weeks (8–48) in G1, and 14.56 weeks (8–24) in G2. The results were evaluated according to the AOFAS scale, with plain X-rays, and complications during follow-up.
ResultsThe mean evaluation according to the AOFAS score was 78.62 in G1 (22–93), and 90.63 in G2 (70–100), and this was statistically significant. In G1, 61.4% (8) of the results were excellent or good, while in G2 it was 76% (13). There were no axial deformity cases or shortenings. There were four superficial infections and one broken device recorded in G1.
DiscussionThe percutaneous cannulated screw fixation is a suitable alternative for the management of fractures without significant joint involvement, and seems to offer better functional results than plates. The shortest time from injury to intervention in this group improves the progress of the soft tissues, and can improve the final result.
Analizar los resultados del tratamiento de las fracturas de tibia distal con o sin afectación intraarticular, tratadas con osteosíntesis percutánea mediante placas o tornillos canulados.
Material y métodoEstudio retrospectivo de 107 pacientes intervenidos entre 2001 y 2012. Criterios de inclusión: fracturas 43-A y 43-C1 y C2 según la clasificación AO, tratadas con osteosíntesis percutánea mediante placa bloqueada o 2 tornillos canulados en aspa. Se evaluaron 33 pacientes: 16 casos fueron sintetizados con placa bloqueada (G1) y 17 con tornillos canulados (G2). El tiempo medio hasta cirugía fue de 8,31 días (0-14) en G1 y de 2 días (0-7) en G2. La media de seguimiento fue de 72 meses (12-132). Tiempo medio hasta consolidación: 17,08 semanas (8-48) en G1 y 14,56 semanas (8-24) en G2. Los resultados se evaluaron según la escala AOFAS, radiografías simples y complicaciones durante el seguimiento.
ResultadosLa valoración media según la AOFAS fue de 78,62 en G1 (22-93) y 90,63 en G2 (70-100), siendo esta diferencia estadísticamente significativa. En G1 el 61,4% (8) de los resultados fueron excelentes o buenos, mientras que en G2 lo fueron el 76% (13). Ausencia de casos con deformidad axial y acortamientos. Se registraron 4 infecciones superficiales y una rotura de material en G1.
DiscusiónLa osteosíntesis percutánea con tornillos canulados supone una alternativa adecuada para el manejo de fracturas tibiales sin gran componente articular con mejores resultados que la síntesis con placas. El menor tiempo desde el traumatismo hasta la intervención en este grupo mejora la evolución de partes blandas, siendo significativo en el resultado final.
The management of complex, distal tibial fractures represents a challenge for orthopedic surgeons and their treatment is the subject of active debate.1
In the 60s and 70s, the most widely accepted treatment for intraarticular fractures of the distal tibia was open reduction and external fixation of the bone fragments through a correct joint reconstruction, according to the general principles advocated by the AO/OTA working group.2 However, this required extensive approaches which could cause devitalization of adjacent soft tissues, infection, scarring problems in the surgical wound and joint rigidity, especially in those fractures caused by high-energy trauma.3 The high rate of complications of this treatment, which included consolidation delays, pseudoarthrosis and infection,4–6 highlighted the need to develop new therapeutic patterns toward the end of the 80s.
The introduction of percutaneous treatment for these lesions allowed the use of closed, indirect reduction techniques, which enabled an internal fixation of the tibia along with correction of rotational and axial malalignment.7,8 The most commonly used devices for this purpose have been intramedullary nails,9 locking plates10 and, to a lesser extent, percutaneous screws inserted by compression.11 Previous studies have observed that percutaneous fixation in fractures lacking a significant joint component are satisfactory, with a low complication rate.12,13
The objective of our study was to carry out a comparative analysis of the clinical and functional results of two types of percutaneous techniques, employed for the management of metaphyseal fractures of the distal tibia, with or without intraarticular involvement.
Materials and methodsThis was a retrospective study of a consecutive series of 107 patients who were treated at our center with a diagnosis of metaphyseal fractures of the distal tibia between 2001 and 2012. Patient data were gathered through a review of medical histories.
The inclusion criteria were simple extraarticular or intraarticular fractures of the tibial metaphysis (43-A and C1-2 according to the AO classification system), which had been treated by closed reduction and percutaneous synthesis with locking plates or cannulated screws, and with a follow-up period of at least 1 year. We excluded fractures classified as types B and C3 according to the AO system, those treated by open reduction with extensive approaches and those synthesized using other percutaneous methods, as well as fractures with a follow-up period of less than 1 year.
Applying these criteria, we included 33 patients in the study, who were divided into two groups. The first group (G1) was composed of 16 patients and corresponded to those treated with plates locked in a medial disposition (LCP Synthes®). The group included eight males and eight females, with a mean age of 49.9 years (range: 25–79 years) and six patients presented associated lesions (two distal radius fractures, two tibial plateau fractures and two multiple trauma patients). The second group (G2) consisted of 17 patients intervened with cannulated AO 7.3mm screws in a cross or X shape. It included 11 males and 6 females with a mean age of 49.6 years (range: 28–84 years) and six patients presented associated lesions (three distal radius fractures, two proximal humerus fractures and one talar fracture). The most common mechanism of injury in both groups was an accidental fall (G1: 56%; G2: 53%).
Each fracture was classified retrospectively according to the AO classification system, and soft tissue lesions were assessed according to the classification by Tscherne and Oestern. We did not use preoperative computed tomography (CT) scans routinely for the assessment of fractures.
According to the AO system, in G1 there were three fractures graded as 43-A1, four as 43-A2, three as 43-A3, two as 43-C1 and four as 43-C2. Meanwhile, in G2 there were five fractures graded as 43-A1, five as 43-A2, three as 43-A3, three as 43-C1 and one as 43-C2. According to the classification by Tscherne and Oestern, the majority of closed fractures in both groups presented ample edema and contusion of the soft tissues (G1: 2 T1, 6 T2, 6 T3; G2: 2 T1, 6 T2, 6 T3). There were two open fractures in G1 (Gustilo I) and three open fractures in G2 (1 Gustilo I, 2 Gustilo II).
The mean time elapsed from the trauma until surgery was of 8.2 days (range: 2–14 days) in group 1 and 4.75 days (range: 2–7 days) in group 2. In the emergency room, all fractures were immobilized using a long leg cast, maintaining elevation of the affected lower limb. In total, five patients underwent a sequential treatment, with application of external fixation on the day of admission.
Surgical techniqueThe type of anesthesia employed varied between general and subarachnoid. Patients were placed in the supine position on a radiotransparent table, where ischemia of the intervened limb was conducted in all cases. Preoperative antibiotic prophylaxis was applied in all patients.
All fractures were treated through reduction techniques by traction or using percutaneous reduction forceps. A fluoroscope was used to assess the quality of the reduction.
In G1, the fractures were synthesized with a 3.5mm blocked plate (LCP, Synthes®) which was inserted percutaneously through an incision of approximately 3cm on the medial malleolus. The device produced a bridge effect on the metaphyseal fracture. At least three or four screws were placed, locked in a juxtaarticular and diaphyseal position, using the fluoroscope to ensure a correct placement of the plate and screws. When necessary, compression screws were also used, independently from the plate.
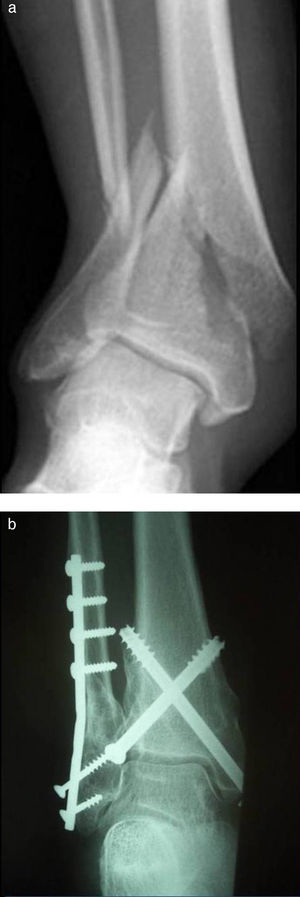
In G2, the fractures were synthesized using two cannulated AO screws inserted percutaneously (Fig. 1). The screws were placed in a cross or X shape, from distal to proximal (from medial-posterior to lateral-anterior and from lateral-posterior to medial-anterior). A fluoroscope was used to assess the correct placement of the screws.
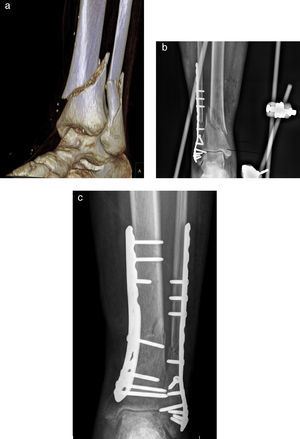
There were 11 fibular fractures in G1 and 8 in G2. The fibula was stabilized in the case of displaced or distal third shortened fractures, and in cases of fractures located between 40 and 50mm from the ankle joint (G1: 9; G2: 8). In all cases, the synthesis of the fibula was carried out ahead of the tibial fracture. Five patients in G1 underwent sequential treatment, including application of an external fixator in the emergency room, and were subsequently intervened for the definitive synthesis after a mean period of 9.8 days (range: 6–14 days) (Fig. 2).
(a) 3D CT scan of the AO type A3 distal tibial fracture and transsyndesmotic fibular fracture. (b) Synthesis of transsyndesmotic fibular fracture with a PERI-LOC VLP plate (Smith and Nephew®) and Hoffmann II external fixator (Stryker®) with emergency bridging of the ankle. (c) Definitive synthesis of the tibial fracture with a locking compression plate (LCP Synthes®) (3 months after the intervention).
Patients in G1 with extraarticular metaphyseal fractures or absence of synthesized fibular fractures were immobilized using a compressive bandage after the intervention, enabling passive exercises from the first postoperative day. In patients with intraarticular fractures we applied a postoperative plaster cast. All patients started progressive load without a cast between 6 and 8 weeks after surgery. Patients in G2 were immobilized with a long leg cast after the intervention and load was permitted with a short leg cast after the 2–3 weeks in extraarticular cases and after 4–6 weeks in intraarticular cases.
All patients were monitored at least until clinical and radiological consolidation took place, with a mean follow-up period of 17.4 months (range: 12–60 months) in G1 and 28.5 months (range: 12–60 months) in G2. There were three losses during the follow-up period in G1 and one in G2.
The assessment of results was based on the AOFAS ankle scale,14 which establishes a clinical and functional evaluation of the ankle, subtalar joint and calcaneal-cuboid joint, according to the range of pain, function and alignment.
We obtained simple radiographs during monitoring (antero-posterior and lateral). Consolidation of the fracture within the first 6 months was defined as normal, between 6 and 9 months as a delayed consolidation and over 9 months as pseudoarthrosis. We considered the fracture to be consolidated upon the appearance of a callus in at least one cortical in the AP and lateral projections and if the patient could apply load without pain.
Statistical analysisThe statistical analysis of the results was conducted using the following tests: Chi-squared test and Fisher's exact test for categorical variables, and Wilcoxon test for quantitative variables. We considered as significant those results with values of P equal to or below 0.05.
ResultsBoth groups were comparable in terms of epidemiological characteristics (Table 1), without significant differences between them (P>.05). Although in G2 there were more comminuted fractures with simple intraarticular outlines (C2), the retrospective classification according to the AO systems and the assessment of soft tissues according to the classification by Tscherne and Oestern did not show significant differences (P>.05).
The period elapsed between the trauma and surgery was significantly lower in the group of patients synthesized with cannulated screws (4.75 days compared to 8.2 days in G1, P<.001). The number of fibular fractures synthesized and the time of their stabilization did not show significant differences between groups (P>.05). This was also true regarding the application of a treatment in two stages among patients in G1 (P>.05).
The clinical and functional assessment of patients according to the AOFAS scale for the ankle and hindfoot had 61.5% of excellent or good results in G1 (seven excellent results, one good, three average and two poor). This percentage was significantly lower than the 76% of excellent or good results reported by patients in G2 (nine excellent results, four good, three average), with P<.05. There were no cases of rotational or angular deformities >5° or shortenings >1cm in any of the groups.
The mean period elapsed until consolidation among patients in G1 was 17.08 weeks, compared to 14.56 weeks in G2, with no significant differences between groups (P>.05). There were no cases of pseudoarthrosis, but there was one instance of consolidation delay in G1, which achieved fracture union 10 months after the first intervention and without requiring a second intervention.
Regarding complications, we recorded four superficial infections in G1 (Table 2). A second intervention was necessary in all cases to remove the material or debride the affected area. Two patients in G1suffered loosening or breakage of screws, but neither required a second intervention to achieve consolidation of the fracture. There were no cases of soft tissue or deep infections in G2.
Patients with superficial soft tissue infection following the surgical intervention.
| Case | Age (years) | Gender | Mechanism of injury | AO type | Tscherne/Gustilo | Fibular fracture | Treatment | Associated lesions/comorbidities | EOM |
| 1 | 30 | F | Sport | A2 | Tscherne1 | Suprasyndesmotic | LCP | DM | Yes |
| 2 | 75 | F | Accidental fall | A3 | Tscherne1 | No | LCP | NO | Yes |
| 3 | 56 | M | Traffic accident | C1 | Gustilo I | No | EF+LCP | Wrist fracture | Yes |
| 4 | 77 | M | Traffic accident | A2 | Gustilo I | Suprasyndesmotic | EF+LCP | Chest trauma+mild TBI | Yes |
EF: external fixator; EOM: extraction of osteosynthesis material; F: female; LCP: locking compression plate; M: male; TBI: traumatic brain injury.
Most patients in G2 (15/16) required a new manipulation to extract the cannulated screws approximately 1 year after the surgery and once the fracture had become consolidated. The size of the screws and their percutaneous juxtamalleolar disposition could lead to discomfort related to the material. In G1, four patients required a second intervention to remove the material, in all cases due to superficial infections in the region of the surgical scar.
DiscussionOver the past 15 years, the surgical treatment of fractures according to AO principles has undergone an evolution. The initial objective of treatment was to achieve a consolidation which allowed adequate function without pain. A precise reduction and absolute stability with interfragmentary compression were conceived to provide a final, asymptomatic function of the affected joints.15
Borrelli et al.16 proved how the risk of altering the vascular supply in the metaphyseal region of the tibia was increased by conventional approaches. This led to the development of minimally invasive stabilization techniques. The first description of the development of percutaneous techniques through the application of a plate fixed to the bone in the superior and inferior parts of the fracture was carried out by Krettek et al.7 The objective of minimally invasive plate osteosynthesis (MIPO) techniques is to minimize the biological risk to soft tissues and decrease the rate of infection and pseudoarthrosis, offering a good functional result.13,17
The time until consolidation in our series was similar to that reported in published series of fractures synthesized using plates blocked by MIPO.13,17–19 The mean time was of 17.08 weeks for the group of the plates and 14.56 weeks for the group of the screws which, although it did not represent a significant difference between groups (P>.05), did seem to indicate that the reduced aggression on soft tissues and preservation of bone vascularization could be favorable during the consolidation process. In our study of percutaneous techniques there were no cases of pseudoarthrosis and only 1 case of consolidation delay which achieved the union of fragments 10 months after the initial intervention. The fracture in this patient was initially synthesized with a medial plate, which requires a greater dissection of soft tissues than cannulated screws. The fracture finally became consolidated without requiring a second intervention. Neither did we register angular and rotational deformities over 5° nor shortening of limbs over 1cm. This type of rotational or axial malalignments are more frequent with the use of other percutaneous techniques, like intramedullary screws.9 The clinical and functional results of our study were excellent or good in over half the cases in both groups, according to the AOFAS scale for the ankle and hindfoot (61.5% versus 76%). This agrees with the results of previous studies which reviewed the percutaneous treatment of this type of fractures with locked plates.19–22
There were no cases of deep infections in either group, however, the development of soft tissue complications was more frequent in the group using plates. We registered four cases of superficial infections in G1, and all of them required a second intervention for debriding of the wound and in three of them final healing was achieved after the extraction of the osteosynthesis material, once the clinical and radiological consolidation of the fracture had been verified. Failure of the material occurred in two patients with fractures synthesized using locked plates. In both cases, the screw which broke was that closest to the focus of the fracture, in the union between the head and neck; however, both fractures achieved consolidation without problems within a mean period of 12 weeks. This higher frequency of soft tissue complications in the group with plates could be explained by a greater surgical aggression, the use of more rigid devices and a longer period elapsed until surgery.
The time of evolution from the trauma until surgery also seems to be linked to the final result. In G2, the patients were intervened after a mean period of 4.75 days since the aggression, compared to 8.2 days waited on average by patients in G1, with this difference being statistically significant (P<.001). Sirkin et al.23 analyzed the results of the previous series by Wyrsch,24 who randomly compared external fixation versus plate osteosynthesis in distal tibial fractures, and found a high rate of complications among the second group. Sirkin defended that patients treated with external fixation in the study by Wyrsch suffered less soft tissue complications because they were intervened before edema and tumefaction developed or after this tumefaction was resolved. In contrast, the majority of patients treated with open reduction and internal fixation were intervened between 3 and 5 days after the trauma, when the soft tissue edema was still considerable. This led to the procedure being developed in stages, with the application of an external fixator within the first 24h after the aggression, to carry out the definitive reconstruction of the tibial joint surface once the soft tissues allowed it. In our study, synthesis of the fracture within the first 24h after the trauma, through the use of percutaneous devices with minimal periosteal and soft tissue aggression, like that represented by the use of cannulated screws, led to a better final functional result than the use of plates, with a lower rate of complications.
To the best of our knowledge, there are no published studies of the results of synthesis with cannulated screws placed in an X-shape, with this being an interesting alternative to consider in extraarticular fractures of the distal tibia and in fractures with a minimal joint component, in which restoration of the tibial joint surface can be achieved through closed or percutaneous methods.
Although the cost of cannulated screws is lower than that of blocked plates, we must also consider that the need to extract material took place significantly among the majority of patients (15/16). In all cases it was carried out once the fracture had become consolidated, or in a prophylactic manner to avoid discomfort, or once this had appeared, but there were no cases of failure of the material or soft tissue problems related to the device. We have related the need for a second intervention in these patients to the use of large caliber screws in very subcutaneous, juxtamalleolar areas.
The main limitations of our study are the absence of a retrospective study, the low number of patients, the participation of several surgeons, the lack of stratification into open and closed fractures and the absence of a control group. Nevertheless, we can conclude that percutaneous techniques offer satisfactory clinical and functional results and that, most likely, the initial aggression on the soft tissues and subsequent evolution thereof determines the final result.
In spite of our limited series, the technique of closed reduction and fixation with cannulated screws placed in an X-shape offers promising results in types 43-A, 43-C1 and C2 fractures, in which an adequate joint reduction can be achieved without the need for extensive approaches. This technique offers the possibility of achieving an adequate bone alignment with minimal damage to the surrounding soft tissues whilst also achieving adequate stability without the use of an external fixator. Long term studies and the analysis of devices which prevent discomfort related to the material in subcutaneous areas are required to improve and extend the use of this technique.
Level of evidenceLevel of evidence IV.
Ethical responsibilitiesProtection of people and animalsThe authors declare that this investigation did not require experiments on humans or animals.
Confidentiality of dataThe authors declare that they have followed the protocols of their workplace on the publication of patient data and that all patients included in the study received sufficient information and gave their written informed consent to participate in the study.
Right to privacy and informed consentThe authors declare having obtained written informed consent from patients and/or subjects referred to in the work. This document is held by the corresponding author.
Conflict of interestThe authors have not received any grant or economic aid from any institution to carry out this work.
Please cite this article as: Martín Fuentes A, Sánchez Morata E, Mellado Romero M, Bravo Giménez B, Vilà y Rico J. Osteosíntesis percutánea en fracturas de pilón tibial, ¿condiciona la técnica quirúrgica el resultado final?. Rev Esp Cir Ortop Traumatol. 2014;58:290–296.