In a recent article in your journal, Colsa Gutiérrez et al.1 reviewed intraoperative injuries to peripheral nerves in colorectal surgery. As in abdominal surgery, breast surgery can lead to neurological injuries during the immediate postoperative period that are not related with the surgical technique but instead with the positioning of the patient on the operating table. Therefore, a critical analysis of each case is necessary for the prevention of these adverse effects and to improve patient safety, which are the responsibility of medical professionals. In this Letter to the Editor, we will describe our experience in neurological lesions after breast surgery in order to discuss possible causes and, above all, recommendations to avoid them.
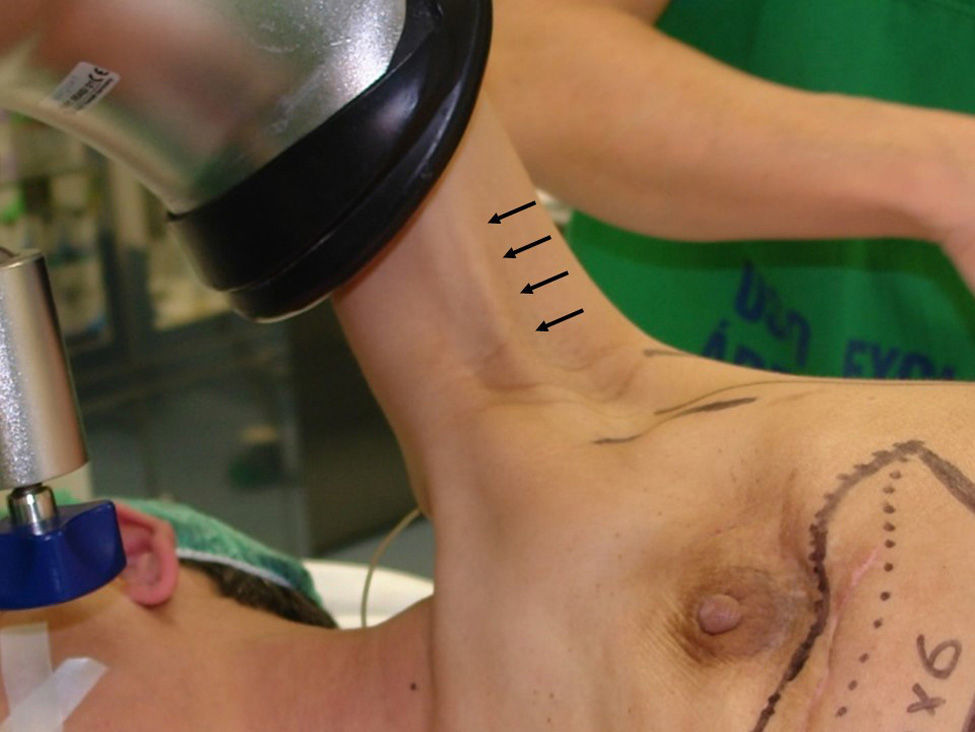
Between January 2000 and June 2015, 1501 surgical procedures were performed in women with breast cancer. During the immediate postoperative period, 4 neurological deficits were observed secondary to injury to the brachial plexus, which was an incidence of 0.002% (Table 1). The surgical techniques performed were mastectomy with axillary lymph node dissection, bilateral vertical mammaplasty, latissimus dorsi flap reconstruction and replacement of breast expander with definitive prosthesis. The mechanisms related with neurological injury were diverse and included the use of retractors on the brachial plexus, hyperabduction of the upper extremity and its elongation in lateral decubitus (Fig. 1). In one case, axillary fibrosis secondary to radiotherapy predisposed the patient to functional limitation prior to surgery, which conditioned the appearance of postoperative paralysis in spite of the correct placement of the limbs during the intervention. The neurological deficits affected the sensitivity and mobility of the upper limb, and recovery was variable (between 6 and 28 weeks). The patients were evaluated by the rehabilitation unit, and all were diagnosed with injury to the brachial plexus (neurapraxia), with no evidence of distal nerve injury in any of the cases. The 4 patients recovered their neurological function, although one presented chronic sensory neuropathy in the proximal region of the upper extremity.
Clinical Characteristics of the Patients With Neurological Injury After Breast Surgery.
| Age | Sex | Appearance of symptoms | Surgery | Surgery duration | Precipitating factors | Neurological deficit | Type of neurological injury | Time until stabilisation | Sequelae |
|---|---|---|---|---|---|---|---|---|---|
| 55 | Female | Immediate | Mastectomy and axillary lymphadenectomy | 150min | Placement of separator over brachial plexus | Sensory and motor | Neurapraxia of the brachial plexus | 10 weeks | None |
| 50 | Female | Immediate | Latissimus dorsi flap | 300min | Stretching of the upper extremity | Sensory and motor | Neurapraxia of the brachial plexus | 28 weeks | Sensory deficit in the proximal upper limb |
| 36 | Female | Immediate | Mammoplasty vertical | 140min | Hyperabduction of upper extremity | Sensory and motor | Neurapraxia of the brachial plexus | 6 weeks | None |
| 47 | Female | Immediate | Replacement of breast expander | 100min | Axillary and supraclavicular radiotherapy | Sensory and motor | Neurapraxia of the brachial plexus | 7 weeks | None |
Iatrogenic injury to the brachial plexus is an uncommon occurrence in breast surgery, and its exact incidence is unknown because most authors have published isolated cases of neurological injury.2 Breast surgery presents factors for the appearance of paralysis of the brachial plexus; oncoplastic and reconstructive procedures are characteristically long in duration and involve postural changes as well as the need for positioning the upper limbs in abduction.2–4 This predisposition affects not only oncological procedures but also later reconstructive surgeries, where manipulation of patient position is also required.5 The explanation of this predisposition lies in the vulnerability of the brachial plexus due to its anatomical factors: its attachment between fixed points (foramen and axillary fascia), its passage through a narrow canal between the clavicle and first rib, its relationship with bony protuberances (head of the humerus and ulna),2–4 and the fibrosis of the axillary canal after radiation.6
Surgeons are responsible for preventing neurological injuries, and they should therefore ensure correct placement of these patients during surgery. There are 4 basic recommendations for the prevention of these injuries. The first is to avoid direct injury with surgical instruments, especially during manipulation in axillary lymph node dissection,7 using separators that are not in contact with the brachial plexus or limiting thermocoagulation during lymph node dissection. A second recommendation is to limit the abduction of the upper limb to 90°, and in this situation to maintain the head in a neutral position, with no lateral displacement, since cadaveric studies have demonstrated a greater tension of the brachial plexus when the head is turned.3 We should also take greater care during limb abduction in patients with prior radiation of the lymph node chains, because in these cases the local fibrosis and direct toxicity on the nerve entail a greater risk of appearance of neurapraxia, as we observed in one of our patients. The third recommendation is related with the traction of the shoulder in the position of lateral decubitus during the dissection of a latissimus dorsi muscle flap. In these cases, we should take care that the shoulder traction is not excessive or creates elongation of the nerve structures. Finally, we should use cushioned arm supports to prevent injury to the peripheral nerves.
In conclusion, the presence of a lesion to the brachial plexus during the postoperative period of breast surgery is caused by the concomitance of several factors, including hyperabduction of the upper extremity, hyperextension/external rotation of the upper extremity, rotation of the head or the presence of axillary fibrosis secondary to radiotherapy. The identification of these risk factors by medical professionals is necessary to prevent this complication during the postoperative period.
Conflict of InterestsThe authors declare that there were no conflicts of interest in the elaboration or publication of this manuscript.
Please cite this article as: Acea Nebril B, Domenech Pina E, Díaz Carballada C, García Novoa A. Lesiones del plexo braquial en la cirugía mamaria. Recomendaciones para su prevención. Cir Esp. 2016;94:251–253.