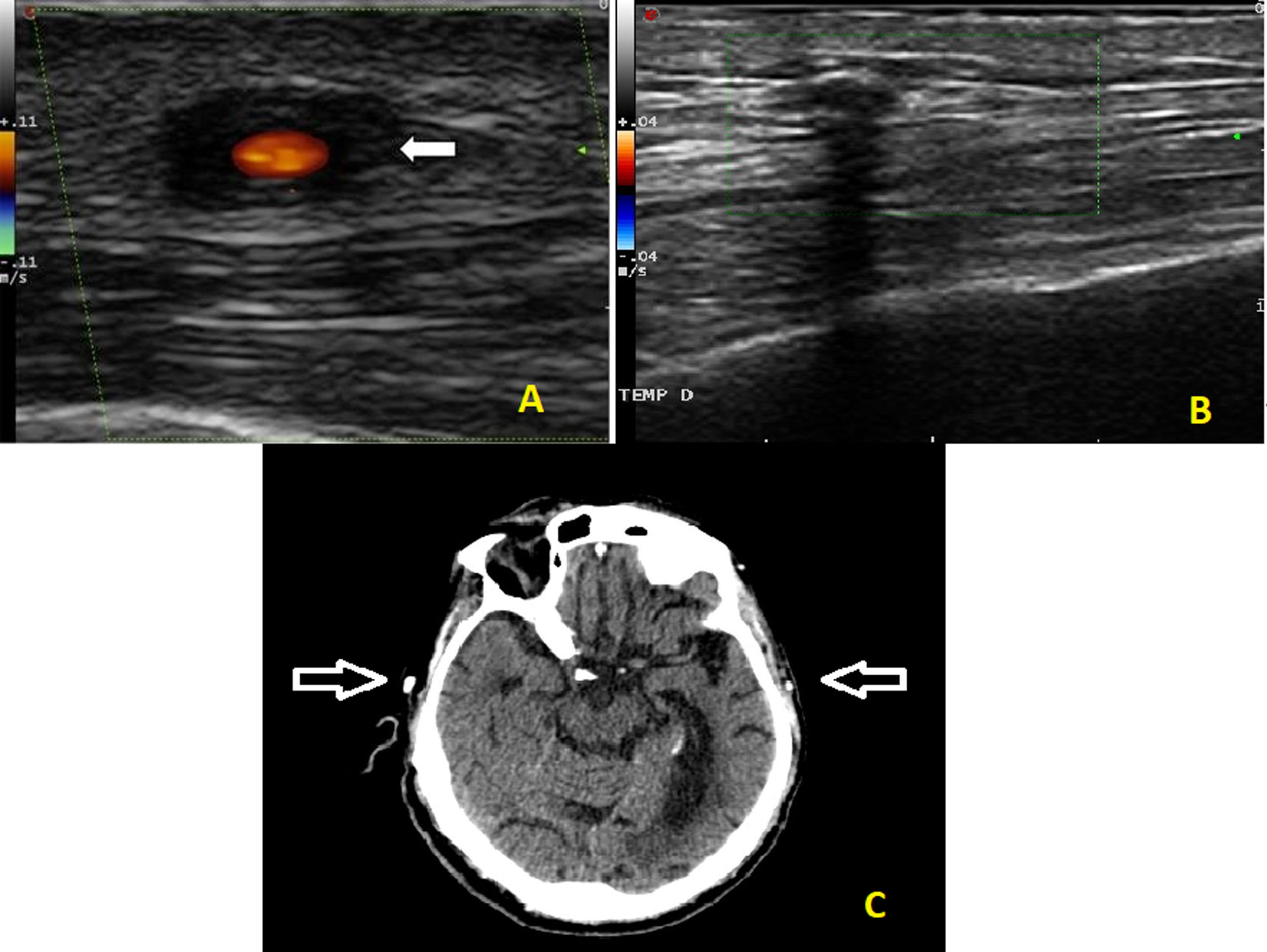
array:24 [ "pii" => "S2387020621004587" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.07.036" "estado" => "S300" "fechaPublicacion" => "2021-10-08" "aid" => "5361" "copyright" => "Elsevier España, S.L.U.. All rights reserved" "copyrightAnyo" => "2020" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:352-3" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S0025775320305285" "issn" => "00257753" "doi" => "10.1016/j.medcli.2020.07.012" "estado" => "S300" "fechaPublicacion" => "2021-10-08" "aid" => "5361" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:352-3" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Carta al Editor</span>" "titulo" => "Falso signo del halo secundario a calcificación en la arteria temporal" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "352" "paginaFinal" => "353" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "False halo sign secondary to calcification of temporal artery" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figura 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1878 "Ancho" => 2500 "Tamanyo" => 323767 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">a) Ejemplo de halo anecoico en arteria temporal en un paciente con arteritis de células gigantes diferente al descrito en el caso clínico. b) Ecografía de arterias temporales en el paciente del caso actual. La caja muestra el área en modo color. La imagen muestra la arteria temporal como una estructura ovoidea en la que destaca la ausencia de señal color de flujo que, <span class="elsevierStyleItalic">a priori</span>, sugiere oclusión del vaso. La presencia de un reborde superficial hiperecoico y la sombra acústica demuestra que corresponde con un vaso calcificado en el que no se puede visualizar en su contenido la estructura (modo B) ni la presencia de flujo (modo color). c) TC de cráneo sin contraste que muestra la calcificación de la arteria temporal (flechas).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Luis Marhuenda-Bermejo, Óscar Ayo-Martín, Jorge García-García" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Luis" "apellidos" => "Marhuenda-Bermejo" ] 1 => array:2 [ "nombre" => "Óscar" "apellidos" => "Ayo-Martín" ] 2 => array:2 [ "nombre" => "Jorge" "apellidos" => "García-García" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2387020621004587" "doi" => "10.1016/j.medcle.2020.07.036" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621004587?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775320305285?idApp=UINPBA00004N" "url" => "/00257753/0000015700000007/v1_202109300523/S0025775320305285/v1_202109300523/es/main.assets" ] ] "itemSiguiente" => array:18 [ "pii" => "S2387020621004575" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.07.035" "estado" => "S300" "fechaPublicacion" => "2021-10-08" "aid" => "5360" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:353-5" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "AV block in a young patient secondary to cystic tumor of the auriculoventricular node" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "353" "paginaFinal" => "355" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Bloqueo AV en un paciente joven secundario a tumor quístico del nodo auriculoventricular" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 2891 "Ancho" => 3167 "Tamanyo" => 1091873 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">A) Electrocardiogram of the patient on admission, showing a first-degree AVB. B1 and B2) Transesophageal echocardiogram images revealing anechoic lesions in the interatrial septum (arrows).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Luis Cabezón-Gutiérrez, Laura Espinosa-Pinzón, Eduardo Alegría-Barrero" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Luis" "apellidos" => "Cabezón-Gutiérrez" ] 1 => array:2 [ "nombre" => "Laura" "apellidos" => "Espinosa-Pinzón" ] 2 => array:2 [ "nombre" => "Eduardo" "apellidos" => "Alegría-Barrero" ] ] ] ] ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621004575?idApp=UINPBA00004N" "url" => "/23870206/0000015700000007/v1_202110050801/S2387020621004575/v1_202110050801/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2387020621004599" "issn" => "23870206" "doi" => "10.1016/j.medcle.2020.07.037" "estado" => "S300" "fechaPublicacion" => "2021-10-08" "aid" => "5366" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2021;157:350-2" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Interstitial pneumonia as the first manifestation of lupus in a pregnant woman in the early stages of the disease" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "350" "paginaFinal" => "352" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Neumonía intersticial como primera manifestación de un lupus en una gestante en etapas tempranas de la enfermedad" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 3173 "Ancho" => 3174 "Tamanyo" => 1263664 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Chest HRCT. Signs of diffuse interstitial lung disease with fibrosis, with a non-UIP pattern, which may be compatible with NSIP in the context of a systemic autoimmune disease.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Ángela López-Bauzá, Santiago Rodríguez Suárez, Jose Antonio Rodríguez Portal" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Ángela" "apellidos" => "López-Bauzá" ] 1 => array:2 [ "nombre" => "Santiago" "apellidos" => "Rodríguez Suárez" ] 2 => array:2 [ "nombre" => "Jose Antonio" "apellidos" => "Rodríguez Portal" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0025775320305339" "doi" => "10.1016/j.medcli.2020.07.017" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775320305339?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621004599?idApp=UINPBA00004N" "url" => "/23870206/0000015700000007/v1_202110050801/S2387020621004599/v1_202110050801/en/main.assets" ] "en" => array:17 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "False halo sign secondary to calcification of temporal artery" "tieneTextoCompleto" => true "saludo" => "Dear Editor:" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "352" "paginaFinal" => "353" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Luis Marhuenda-Bermejo, Óscar Ayo-Martín, Jorge García-García" "autores" => array:3 [ 0 => array:4 [ "nombre" => "Luis" "apellidos" => "Marhuenda-Bermejo" "email" => array:1 [ 0 => "l.marhuenda@hotmail.com" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "*" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Óscar" "apellidos" => "Ayo-Martín" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 2 => array:3 [ "nombre" => "Jorge" "apellidos" => "García-García" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] ] "afiliaciones" => array:2 [ 0 => array:3 [ "entidad" => "Hospital General Universitario de Elche, Departamento de Neurología, Alicante, Spain" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Hospital General Universitario de Albacete, Departamento de Neurología, Albacete, Spain" "etiqueta" => "b" "identificador" => "aff0010" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Falso signo del halo secundario a calcificación en la arteria temporal" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1878 "Ancho" => 2500 "Tamanyo" => 323767 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">a) Example of an anechoic halo in the temporal artery of a patient with giant cell arteritis different from that described in the clinical case. b) Ultrasound of the temporal arteries of the patient whose clinical case is described in this paper. The box displays the area in color mode. The image shows the temporal artery as an ovoid structure in which the absence of color flow signal stands out, a finding that tends to be suggestive of vessel occlusion. The presence of a superficial, hyperechoic rim and the acoustic shadow demonstrate that it corresponds to a calcified vessel within which neither the structure (B-mode) nor the presence of flow (color mode) can be visualized. c) Cranial CT scan without contrast showing calcification of the temporal artery (arrows).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">Giant cell arteritis (GCA) is a vasculitis of the medium and large arteries, with a particularly high involvement of the temporal artery (TA). This disease requires an early diagnosis to avoid serious complications such as optic neuropathy or ischemic stroke. In this context, ultrasonography is progressively gaining prominence due to its quick availability and having demonstrated both adequate sensitivity and specificity for the diagnosis of GCA. The most characteristic ultrasonographic sign of this condition is the so-called halo sign, which consists in a concentric, hypoechoic area surrounding the lumen of the temporal artery (temporal halo; <a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>a) that translates into the existence of arterial wall edema. The detection of this halo sign in the TA is highly specific and practically confirms the diagnosis of GCA. There are only sporadic reports on other pathological processes that may cause a false positive sign.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a></p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0010" class="elsevierStylePara elsevierViewall">In this paper we present the case of a patient in whom an ultrasonographic study showed a false halo sign in the TA due to the acoustic shadow caused by the calcification of this artery.</p><p id="par0015" class="elsevierStylePara elsevierViewall">The patient was an 86-year-old man with a history of arterial hypertension, type-2 diabetes mellitus, colon carcinoma, and mild chronic renal failure. He was initially admitted to the hospital due to presenting with a low level of consciousness and left, hemispheric focal deficits secondary to an acute traumatic subdural hematoma. Surgical treatment was ruled out and conservative management was chosen in his particular case. During his stay at the hospital, the patient experienced an illdefined holocranial headache; fever spikes without a clear infectious focus, although with circadian predominance and a poor response to broad-spectrum antibiotic therapy; and had increased levels of acute phase reactants, such as C-reactive protein (CRP) levels of up to 40 mg/ml and an erythrocyte sedimentation rate (ESR) of up to 20 mm/h. These findings, together with the presence of a very indurated TA on physical examination, prompted his referral to the Neurology Department with a suspected diagnosis of GCA. An ultrasound study of the TAs was performed (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>b), observing patchy segments with anechoic images across the entire section of the arteries examined and no color flow signal within them (video). This finding mimicked a temporal halo at its maximum degree of intensity (arterial occlusion). However, closer observation showed a hyperechoic rim in the most superficial margin and a posterior acoustic shadow in these segments, which are characteristic findings of calcic structures. The remaining segments of both temporal arteries had a normal morphology and hemodynamics. No vasculitic abnormalities were observed in the rest of the cervical and cranial arteries examined. A cranial computed tomography (CT) revealed calcification of both regions of the temporal arteries that had been examined through ultrasonography (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>c). Both the fever and analytical alterations described resolved without the need for corticosteroid treatment. Based on the above findings, a diagnosis of GCA was finally not established at discharge, and the clinical picture was attributed to an infection of undetermined focus.</p><p id="par0020" class="elsevierStylePara elsevierViewall">Ultrasonography can significantly contribute to the diagnosis of GCA, especially by allowing visualization of the inflammation on the walls of the aforementioned blood vessels, which manifests as a predominantly hypoechoic concentric mural thickening, known as the halo sign.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> It is estimated that the halo sign in patients with GCA has a sensitivity of 77% and a specificity of 96%.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> Therefore, although there are patients with GCA in whom temporal arterial anomalies are not identified, the presence of false positives is very infrequent. The available literature describes some pathologies that can sporadically also cause a false halo sign, such as stenosis or arteriosclerotic occlusion of the TA, as well as infectious or malignant diseases.<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">4</span></a></p><p id="par0025" class="elsevierStylePara elsevierViewall">Calcifications of the TA mimicking GCA have previously been described<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a>; however, according to our knowledge of the existing literature on the subject, this is the first described case of TA calcification as a cause of a false ultrasonographic halo sign. In this context, in order to avoid diagnostic errors, it is important to rule out that the anechoic image of the artery is accompanied by a superficial, hyperechoic rim and a posterior acoustic shadow, as these findings are suggestive of being caused by structures containing calcium. Occluded temporal arteries (with no color signal within the “halo”) due to vasculitis are rare, but possible, and involve the highest degree of inflammation of the vessel. In these cases, there is no such hyperechoic rim and the deep structures are visualized normally.</p><p id="par0030" class="elsevierStylePara elsevierViewall">In summary, we present a new ultrasonographic finding whose awareness will help improve the reliability of ultrasonography in the study of patients with suspected GCA. We believe that it is interesting because of the frequent presence of calcifications in any artery, particularly among elderly subjects. Hence, being aware of this finding will make it easier to recognize it and avoid confusions in this type of studies.</p><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Funding</span><p id="par0035" class="elsevierStylePara elsevierViewall">We have not received any funding for the conduct of this study.</p></span><span id="sec0010" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0010">Conflicts of interest</span><p id="par0040" class="elsevierStylePara elsevierViewall">The authors declare no conflicts of interest.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:3 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Funding" ] 1 => array:2 [ "identificador" => "sec0010" "titulo" => "Conflicts of interest" ] 2 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "⋆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Marhuenda-Bermejo L, Ayo-Martín Ó, García-García J. Falso signo del halo secundario a calcificación en la arteria temporal. Med Clin (Barc). 2021;157:352–353.</p>" ] ] "apendice" => array:1 [ 0 => array:1 [ "seccion" => array:1 [ 0 => array:4 [ "apendice" => "<p id="par0050" class="elsevierStylePara elsevierViewall">The following is Supplementary data to this article:<elsevierMultimedia ident="upi0005"></elsevierMultimedia></p>" "etiqueta" => "Appendix A" "titulo" => "Supplementary data" "identificador" => "sec0020" ] ] ] ] "multimedia" => array:2 [ 0 => array:8 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1878 "Ancho" => 2500 "Tamanyo" => 323767 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">a) Example of an anechoic halo in the temporal artery of a patient with giant cell arteritis different from that described in the clinical case. b) Ultrasound of the temporal arteries of the patient whose clinical case is described in this paper. The box displays the area in color mode. The image shows the temporal artery as an ovoid structure in which the absence of color flow signal stands out, a finding that tends to be suggestive of vessel occlusion. The presence of a superficial, hyperechoic rim and the acoustic shadow demonstrate that it corresponds to a calcified vessel within which neither the structure (B-mode) nor the presence of flow (color mode) can be visualized. c) Cranial CT scan without contrast showing calcification of the temporal artery (arrows).</p>" ] ] 1 => array:5 [ "identificador" => "upi0005" "tipo" => "MULTIMEDIAECOMPONENTE" "mostrarFloat" => false "mostrarDisplay" => true "Ecomponente" => array:3 [ "fichero" => "mmc1.mp4" "ficheroTamanyo" => 914474 "Video" => array:2 [ "flv" => array:5 [ "fichero" => "mmc1.flv" "poster" => "mmc1.jpg" "tiempo" => 0 "alto" => 0 "ancho" => 0 ] "mp4" => array:5 [ "fichero" => "mmc1.m4v" "poster" => "mmc1.jpg" "tiempo" => 0 "alto" => 0 "ancho" => 0 ] ] ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:5 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "The ultrasound halo sign in angiolymphoid hyperplasia of the temporal artery" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "M.W.T. Arnander" 1 => "M.W. Arnander" 2 => "N.G. Anderson" 3 => "F. Schönauer" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1259/bjr/81338007" "Revista" => array:6 [ "tituloSerie" => "Br J Radiol" "fecha" => "2006" "volumen" => "79" "paginaInicial" => "e184" "paginaFinal" => "e186" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/17065284" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Color duplex ultrasonography in the diagnosis of temporal arteritis" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:4 [ 0 => "W.A. Schmidt" 1 => "H.E. Kraft" 2 => "K. Vorpahl" 3 => "E.J. Gromnica-Ihle" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1056/NEJM199711063371902" "Revista" => array:6 [ "tituloSerie" => "N Engl J Med" "fecha" => "1997" "volumen" => "337" "paginaInicial" => "1336" "paginaFinal" => "1342" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/9358127" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Imaging in diagnosis, outcome prediction and monitoring of large vessel vasculitis: a systematic literature review and meta-analysis informing the EULAR recommendations" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "C. Duftner" 1 => "C. Dejaco" 2 => "A. Sepriano" 3 => "L. Falzon" 4 => "W.A. Schmidt" 5 => "S. Ramiro" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1136/rmdopen-2017-000612" "Revista" => array:5 [ "tituloSerie" => "RMD Open" "fecha" => "2018" "volumen" => "4" "paginaInicial" => "e000612" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29531788" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Meta-analysis: test performance of ultrasonography for giant-cell arteritis" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "F.B. Karassa" 1 => "M.I. Matsagas" 2 => "W.A. Schmidt" 3 => "J.P.A. Ioannidis" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.7326/0003-4819-142-5-200503010-00011" "Revista" => array:6 [ "tituloSerie" => "Ann Intern Med" "fecha" => "2005" "volumen" => "142" "paginaInicial" => "359" "paginaFinal" => "369" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/15738455" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Mönckeberg medial calcific sclerosis mimicking giant cell arteritis clinically" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "M.J. Belliveau" 1 => "D. Almeida" 2 => "A. Eneh" 3 => "J. Farmer" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.jcjo.2012.09.013" "Revista" => array:6 [ "tituloSerie" => "Can J Ophthalmol" "fecha" => "2013" "volumen" => "48" "paginaInicial" => "71" "paginaFinal" => "72" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/23419302" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/23870206/0000015700000007/v1_202110050801/S2387020621004587/v1_202110050801/en/main.assets" "Apartado" => array:4 [ "identificador" => "43309" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Letters to the Editor" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/23870206/0000015700000007/v1_202110050801/S2387020621004587/v1_202110050801/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020621004587?idApp=UINPBA00004N" ]
Journal Information
Vol. 157. Issue 7.
Pages 352-353 (October 2021)
Share
Download PDF
More article options
Vol. 157. Issue 7.
Pages 352-353 (October 2021)
Letter to the Editor
False halo sign secondary to calcification of temporal artery
Falso signo del halo secundario a calcificación en la arteria temporal
Visits
4
This item has received
Article information
These are the options to access the full texts of the publication Medicina Clínica (English Edition)
Subscriber
Subscribe
Purchase
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail