array:24 [ "pii" => "S2387020620300036" "issn" => "23870206" "doi" => "10.1016/j.medcle.2019.02.041" "estado" => "S300" "fechaPublicacion" => "2020-03-13" "aid" => "4790" "copyright" => "Elsevier España, S.L.U.. All rights reserved" "copyrightAnyo" => "2019" "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2020;154:195-6" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S002577531930140X" "issn" => "00257753" "doi" => "10.1016/j.medcli.2019.02.008" "estado" => "S300" "fechaPublicacion" => "2020-03-13" "aid" => "4790" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2020;154:195-6" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Carta al Editor</span>" "titulo" => "Disección de arteria vertebral secundaria a fractura tipo <span class="elsevierStyleItalic">hangman</span>" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "195" "paginaFinal" => "196" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Vertebral artery dissection secondary to hangman's fracture" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figura 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 864 "Ancho" => 750 "Tamanyo" => 58921 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Imagen axial de resonancia magnética de columna cervical en secuencia potenciada en T2 TSE. Se aprecia un aumento de la señal de la arteria vertebral derecha (flecha roja) respecto a la contralateral (flecha amarilla), lo que apunta a una posible disección de la primera.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Antonio Jesús Láinez Ramos-Bossini, Regina Gálvez López, Jorge Pastor Rull" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Antonio Jesús" "apellidos" => "Láinez Ramos-Bossini" ] 1 => array:2 [ "nombre" => "Regina" "apellidos" => "Gálvez López" ] 2 => array:2 [ "nombre" => "Jorge" "apellidos" => "Pastor Rull" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2387020620300036" "doi" => "10.1016/j.medcle.2019.02.041" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020620300036?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S002577531930140X?idApp=UINPBA00004N" "url" => "/00257753/0000015400000005/v2_202004200610/S002577531930140X/v2_202004200610/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2387020620300061" "issn" => "23870206" "doi" => "10.1016/j.medcle.2019.05.013" "estado" => "S300" "fechaPublicacion" => "2020-03-13" "aid" => "4912" "copyright" => "Elsevier España, S.L.U." "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Med Clin. 2020;154:197" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Image in medicine</span>" "titulo" => "Vestibular schwannoma and normal pressure hydrocephalus: An infrequent association as a cause of dementia" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:1 [ "paginaInicial" => "197" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Schwannoma vestibular e hidrocefalia crónica del adulto: una asociación infrecuente como causa de demencia" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:6 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 956 "Ancho" => 1074 "Tamanyo" => 123954 ] ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Jose Manuel Felices-Farias, Pilar Rey-Segovia, Francisco Barqueros-Escuer, Victoria Vázquez-Sáez, Ana Pérez-Ballesta" "autores" => array:5 [ 0 => array:2 [ "nombre" => "Jose Manuel" "apellidos" => "Felices-Farias" ] 1 => array:2 [ "nombre" => "Pilar" "apellidos" => "Rey-Segovia" ] 2 => array:2 [ "nombre" => "Francisco" "apellidos" => "Barqueros-Escuer" ] 3 => array:2 [ "nombre" => "Victoria" "apellidos" => "Vázquez-Sáez" ] 4 => array:2 [ "nombre" => "Ana" "apellidos" => "Pérez-Ballesta" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0025775319304300" "doi" => "10.1016/j.medcli.2019.05.021" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775319304300?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020620300061?idApp=UINPBA00004N" "url" => "/23870206/0000015400000005/v2_202004200617/S2387020620300061/v2_202004200617/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2387020620300048" "issn" => "23870206" "doi" => "10.1016/j.medcle.2019.02.042" "estado" => "S300" "fechaPublicacion" => "2020-03-13" "aid" => "4792" "copyright" => "Elsevier España, S.L.U." "documento" => "simple-article" "crossmark" => 1 "subdocumento" => "cor" "cita" => "Med Clin. 2020;154:194" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:10 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Schwannoma of the cervical plexus in a 76-year-old woman" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:1 [ "paginaInicial" => "194" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Schwannoma del plexo cervical en una mujer de 76 años" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Irene Vacas Muñoz, Inmaculada Ruiz Molina, Antonio Gallardo Ávila" "autores" => array:3 [ 0 => array:2 [ "nombre" => "Irene" "apellidos" => "Vacas Muñoz" ] 1 => array:2 [ "nombre" => "Inmaculada" "apellidos" => "Ruiz Molina" ] 2 => array:2 [ "nombre" => "Antonio" "apellidos" => "Gallardo Ávila" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S0025775319301423" "doi" => "10.1016/j.medcli.2019.02.010" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S0025775319301423?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020620300048?idApp=UINPBA00004N" "url" => "/23870206/0000015400000005/v2_202004200617/S2387020620300048/v2_202004200617/en/main.assets" ] "en" => array:15 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Letter to the Editor</span>" "titulo" => "Vertebral artery dissection secondary to hangman's fracture" "tieneTextoCompleto" => true "saludo" => "To the Editor:" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "195" "paginaFinal" => "196" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Antonio Jesús Láinez Ramos-Bossini, Regina Gálvez López, Jorge Pastor Rull" "autores" => array:3 [ 0 => array:4 [ "nombre" => "Antonio Jesús" "apellidos" => "Láinez Ramos-Bossini" "email" => array:1 [ 0 => "ajbossini@ugr.es" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 1 => array:3 [ "nombre" => "Regina" "apellidos" => "Gálvez López" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 2 => array:3 [ "nombre" => "Jorge" "apellidos" => "Pastor Rull" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] ] "afiliaciones" => array:2 [ 0 => array:3 [ "entidad" => "Servicio de Radiodiagnóstico, Hospital Virgen de las Nieves, Granada, Spain" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Servicio de Urgencias, Hospital Virgen de las Nieves, Granada, Spain" "etiqueta" => "b" "identificador" => "aff0010" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Disección de arteria vertebral secundaria a fractura tipo" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1237 "Ancho" => 1074 "Tamanyo" => 103695 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Axial magnetic resonance imaging of the cervical spine in T2-weighted TSE sequence. There is an increase in the signal of the right vertebral artery (red arrow) with respect to the contralateral one (yellow arrow), which points to a possible dissection of the first.</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">Vertebral artery dissection (VAD) is a rare entity,<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> with an estimated annual incidence of one case per 100,000 inhabitants, although it is considered underdiagnosed.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> It affects all age groups, with a peak incidence in the fifth decade of life,<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> and accounts for up to 25 % of strokes (CVA) in young and middle-aged patients.<a class="elsevierStyleCrossRefs" href="#bib0005"><span class="elsevierStyleSup">1,3</span></a> We report the case of a patient who came to the Emergency Department for cervical pain after an accidental fall at home, with diagnosis of <span class="elsevierStyleItalic">hangman's</span> cervical fracture and post-trauma VAD.</p><p id="par0010" class="elsevierStylePara elsevierViewall">A 67-year-old male patient, with a history of COPD grade 2 and lumbar canal stenosis, who came to the Emergency Department after suffering an accidental fall at home, without loss of consciousness. The physical examination was normal, and the patient was clinically and hemodynamically stable, but had intense cervical pain. A cervical radiography was requested, and intravenous analgesic treatment was prescribed.</p><p id="par0015" class="elsevierStylePara elsevierViewall">Spondylolisthesis of C2 on C3 was observed on the lateral cervical radiograph, so a cervical spine CT scan was requested, which showed a type <span class="elsevierStyleSmallCaps">II</span> fracture of the axis vertebra (<span class="elsevierStyleItalic">hangman's fracture</span>).</p><p id="par0020" class="elsevierStylePara elsevierViewall">Given this finding, cervical immobilization with a collar and admission to the Neurosurgery ward was decided. MRI of the cervical spine was requested, ruling out any spinal trauma or rupture of the transverse ligament of the atlas. However, hyperintensity of the right vertebral artery (RVA) signal was observed in sequences T1 and T2 in segments V2, V3 and V4, which evidenced an occlusion or a very slow flow of the signal (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>).</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0025" class="elsevierStylePara elsevierViewall">Given the high suspicion of traumatic dissection in the RVA, it was decided to perform a CT angiography, in which occlusion of said artery was confirmed from the distal portion of V2 to the middle portion of V3. Treatment with low molecular weight heparin and oral acenocoumarol was subsequently prescribed after the diagnosis of VAD. The patient's progression was favourable and was discharged.</p><p id="par0030" class="elsevierStylePara elsevierViewall">Classically, VAD has been considered associated with high-energy trauma, but is increasingly found after minor trauma.<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">4</span></a> Fractures of the upper cervical spine and those that affect the transverse foramen are specifically associated with VAD, but VAD associated with minimal fractures have also been described.<a class="elsevierStyleCrossRef" href="#bib0020"><span class="elsevierStyleSup">4</span></a> Up to half of post-trauma VADs have an associated cervical fracture.<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a></p><p id="par0035" class="elsevierStylePara elsevierViewall">The main problem with VAD is that they usually manifest with little specific symptoms, mainly cervical or headache pain, and they are often masked by cervical trauma itself.<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> However, secondary strokes can occur during their development. A symptom-free interval is common, which is explained by the compensation of flow through the contralateral artery.</p><p id="par0040" class="elsevierStylePara elsevierViewall">Most dissections resolve spontaneously, and long-term outcomes are favourable. More than two thirds of occlusions and up to 90 % of stenosis end up rechanneling.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> However, prognosis is variable. Chronic headache, recurrent dissection and stroke sequela are among the medium- and long-term complications of VAD.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> Mortality attributed to carotid and vertebral dissections is less than 5 % and patients who experience a stroke secondary to this condition have a good functional recovery in 75 %.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a></p><p id="par0045" class="elsevierStylePara elsevierViewall">VAD screening is recommended in patients after a serious traffic accident even if they are asymptomatic, since the administration of anticoagulation has proven effective in preventing ischemic stroke due to embolization of thrombotic fragments from the affected artery.<a class="elsevierStyleCrossRef" href="#bib0025"><span class="elsevierStyleSup">5</span></a></p><p id="par0050" class="elsevierStylePara elsevierViewall">The authors want to highlight the diagnostic difficulty of VAD, since it can be masked by the trauma symptoms themselves, and the importance of keeping a suspicious approach even in the face of minimal trauma. In addition, there is a need to adequately assess the possible existence of cervical fractures in patients of a certain age, even in cases of low-energy trauma. The establishment of early anticoagulant treatment has demonstrated a significant decrease in the risk of stroke due to cervical arterial dissection.</p></span>" "pdfFichero" => "main.pdf" "tienePdf" => true "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Láinez Ramos-Bossini AJ, Gálvez López R, Pastor Rull J. Disección de arteria vertebral secundaria a fractura tipo <span class="elsevierStyleItalic">Hangman</span>. Med Clin (Barc). 2020;15:195–196.</p>" ] ] "multimedia" => array:1 [ 0 => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1237 "Ancho" => 1074 "Tamanyo" => 103695 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Axial magnetic resonance imaging of the cervical spine in T2-weighted TSE sequence. There is an increase in the signal of the right vertebral artery (red arrow) with respect to the contralateral one (yellow arrow), which points to a possible dissection of the first.</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:5 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Prognosis of spontaneous cervical artery dissection and transcranial Doppler findings associated with clinical outcomes" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "W.J. Lee" 1 => "K.H. Jung" 2 => "J. Moon" 3 => "S.T. Lee" 4 => "K. Chu" 5 => "S.K. Lee" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s00330-015-3944-4" "Revista" => array:7 [ "tituloSerie" => "Eur Radiol" "fecha" => "2016" "volumen" => "26" "numero" => "5" "paginaInicial" => "1284" "paginaFinal" => "1291" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/26265371" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Masking of vertebral artery dissection by severe trauma to the cervical spine" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "P.D. Schellinger" 1 => "S. Schwab" 2 => "D. Krieger" 3 => "J.B. Fiebach" 4 => "T. Steiner" 5 => "E.F. Hund" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1097/00007632-200102010-00019" "Revista" => array:7 [ "tituloSerie" => "Spine" "fecha" => "2001" "volumen" => "26" "numero" => "3" "paginaInicial" => "314" "paginaFinal" => "319" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/11224870" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Spontaneous dissection of the carotid and vertebral arteries" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:1 [ 0 => "W.I. Schievink" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1056/NEJM200103223441206" "Revista" => array:7 [ "tituloSerie" => "N Engl J Med" "fecha" => "2001" "volumen" => "344" "numero" => "12" "paginaInicial" => "898" "paginaFinal" => "906" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/11259724" "web" => "Medline" ] ] ] ] ] ] ] ] 3 => array:3 [ "identificador" => "bib0020" "etiqueta" => "4" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Traumatic vertebral artery dissection and cerebral infarction following head and neck injury with a lucid interval" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:2 [ 0 => "S. Tabuchi" 1 => "H. Nakayasu" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1002/ams2.75" "Revista" => array:7 [ "tituloSerie" => "Acute Med Surg" "fecha" => "2015" "volumen" => "2" "numero" => "2" "paginaInicial" => "127" "paginaFinal" => "130" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/29123707" "web" => "Medline" ] ] ] ] ] ] ] ] 4 => array:3 [ "identificador" => "bib0025" "etiqueta" => "5" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Imaging of spontaneous and traumatic cervical artery dissection" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "P.B. Sporns" 1 => "T. Niederstadt" 2 => "W. Heindel" 3 => "M.J. Raschke" 4 => "R. Hartensuer" 5 => "R. Dittrich" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1007/s00062-018-0666-4" "Revista" => array:2 [ "tituloSerie" => "Clin Neuroradiol" "fecha" => "2018" ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/23870206/0000015400000005/v2_202004200617/S2387020620300036/v2_202004200617/en/main.assets" "Apartado" => array:4 [ "identificador" => "43309" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Letters to the Editor" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/23870206/0000015400000005/v2_202004200617/S2387020620300036/v2_202004200617/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2387020620300036?idApp=UINPBA00004N" ]
Journal Information
Vol. 154. Issue 5.
Pages 195-196 (March 2020)
Share
Download PDF
More article options
Vol. 154. Issue 5.
Pages 195-196 (March 2020)
Letter to the Editor
Vertebral artery dissection secondary to hangman's fracture
Disección de arteria vertebral secundaria a fractura tipo
Visits
2
This item has received
Article information
These are the options to access the full texts of the publication Medicina Clínica (English Edition)
Subscriber
Subscribe
Purchase
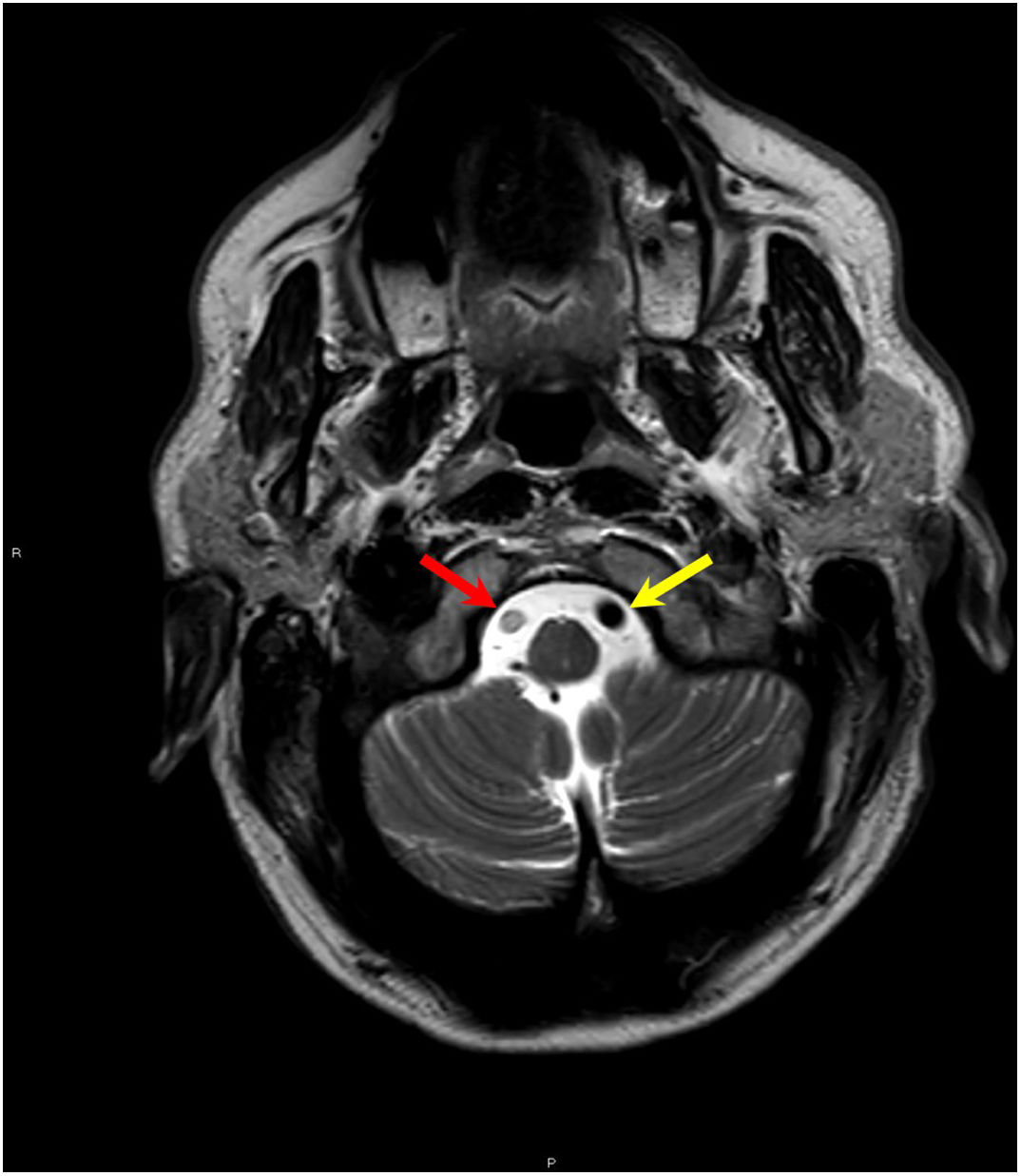
Contact
Phone for subscriptions and reporting of errors
From Monday to Friday from 9 a.m. to 6 p.m. (GMT + 1) except for the months of July and August which will be from 9 a.m. to 3 p.m.
Calls from Spain
932 415 960
Calls from outside Spain
+34 932 415 960
E-mail