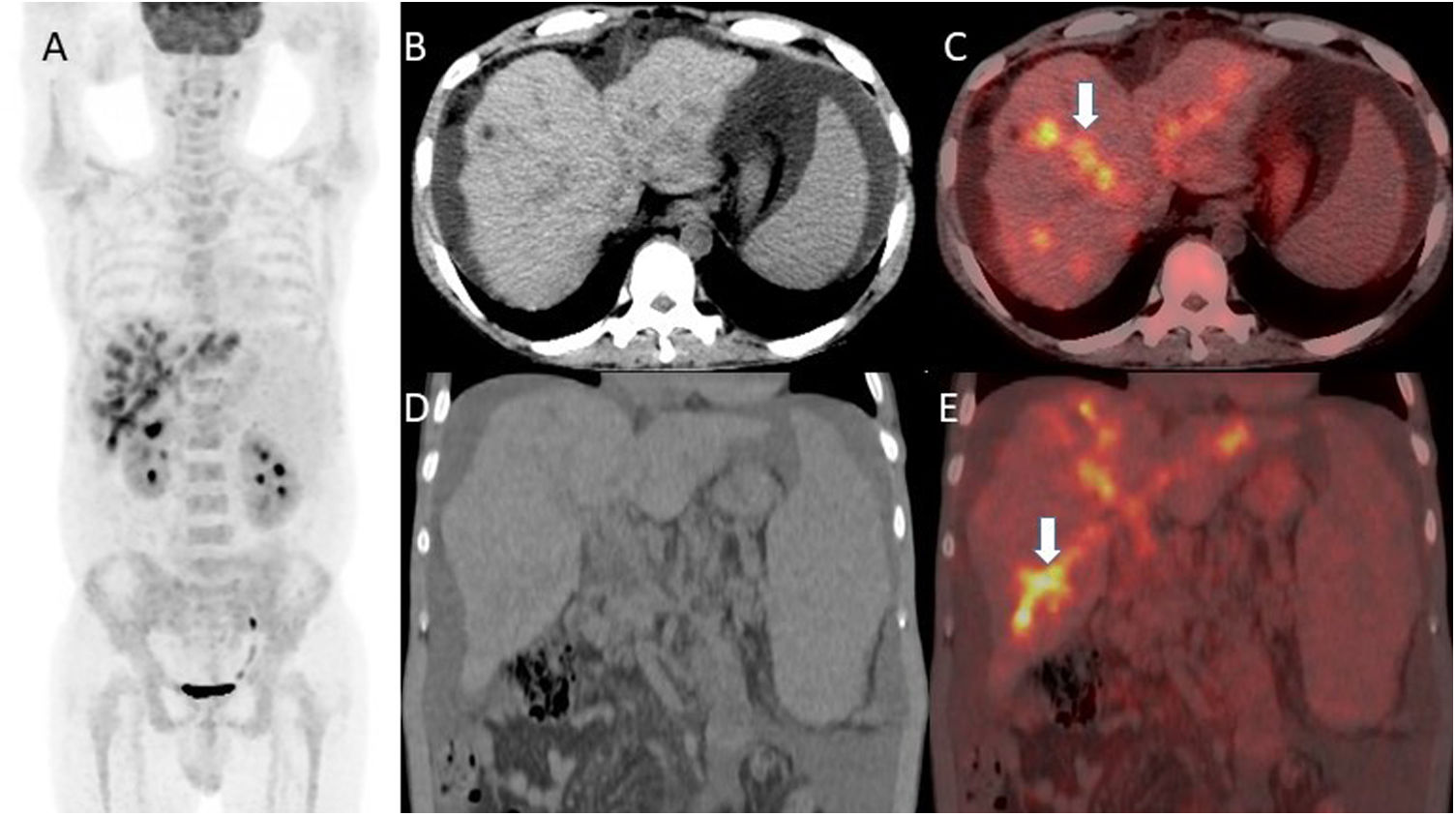
Interesting Images: Surprising and didactic findings from clinical practice
More infoArticle

Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)
array:24 [ "pii" => "S2253808920301634" "issn" => "22538089" "doi" => "10.1016/j.remnie.2020.12.005" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1233" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "copyrightAnyo" => "2020" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S4-S5" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S2253654X20301943" "issn" => "2253654X" "doi" => "10.1016/j.remn.2020.09.004" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1233" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S4-S5" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Imágenes de interés</span>" "titulo" => "Aumento difuso de la captación en los conductos biliares intrahepáticos en<span class="elsevierStyleSup">18</span>F-FDG-PET/TC en un caso de colangitis esclerosante primaria" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S4" "paginaFinal" => "S5" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Diffuse increased uptake in intrahepatic biliary ducts on <span class="elsevierStyleSup">18</span>F-FDG PET/CT in a case with primary sclerosing cholangitis" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Figura 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 838 "Ancho" => 1500 "Tamanyo" => 140412 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Proyección de máxima intensidad de cuerpo entero (MIP) (A), imágenes de tomografía computarizada axial (TC) (B), fusión axial (C) y TC coronal (D) y de fusión coronal (E) del hígado. La captación difusa lineal aumentada de [<span class="elsevierStyleSup">18</span>F]FDG se observó a lo largo de los conductos biliares intrahepáticos (SUVmáx: 8,0), probablemente debido al proceso inflamatorio, junto con una captación leve de radiotrazador en los ganglios linfáticos periportales (SUVmáx: 4,6).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "M. Araz, P. Akkuş, M.H. Baltacioglu, C. Soydal, K.M. Kır" "autores" => array:5 [ 0 => array:2 [ "nombre" => "M." "apellidos" => "Araz" ] 1 => array:2 [ "nombre" => "P." "apellidos" => "Akkuş" ] 2 => array:2 [ "nombre" => "M.H." "apellidos" => "Baltacioglu" ] 3 => array:2 [ "nombre" => "C." "apellidos" => "Soydal" ] 4 => array:2 [ "nombre" => "K.M." "apellidos" => "Kır" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2253808920301634" "doi" => "10.1016/j.remnie.2020.12.005" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808920301634?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X20301943?idApp=UINPBA00004N" "url" => "/2253654X/00000041000000S1/v1_202207160644/S2253654X20301943/v1_202207160644/es/main.assets" ] ] "itemSiguiente" => array:19 [ "pii" => "S2253808921000082" "issn" => "22538089" "doi" => "10.1016/j.remnie.2020.11.001" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1244" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S6-S7" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Unusual location of sentinel node in the inferior gluteal region in a patient with ovarian tumor" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S6" "paginaFinal" => "S7" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Localización inusual del ganglio centinela en la región glútea inferior en una paciente con tumor de ovario" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 688 "Ancho" => 2917 "Tamanyo" => 170331 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0010" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">SPECT/CT images of the patient. Arrows show the para-aortic sentinel nodes.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Marjaneh Farazestanian, Saeedeh Ataei Nakhaei, Afrooz Azad, Najmeh Jahani, Ramin Sadeghi" "autores" => array:5 [ 0 => array:2 [ "nombre" => "Marjaneh" "apellidos" => "Farazestanian" ] 1 => array:2 [ "nombre" => "Saeedeh" "apellidos" => "Ataei Nakhaei" ] 2 => array:2 [ "nombre" => "Afrooz" "apellidos" => "Azad" ] 3 => array:2 [ "nombre" => "Najmeh" "apellidos" => "Jahani" ] 4 => array:2 [ "nombre" => "Ramin" "apellidos" => "Sadeghi" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S2253654X20302079" "doi" => "10.1016/j.remn.2020.11.002" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X20302079?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808921000082?idApp=UINPBA00004N" "url" => "/22538089/00000041000000S1/v1_202207210552/S2253808921000082/v1_202207210552/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S225380892030121X" "issn" => "22538089" "doi" => "10.1016/j.remnie.2020.09.016" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1213" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S2-S3" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting image</span>" "titulo" => "Repeated treatment with low dose of <span class="elsevierStyleSup">131</span>I-MIBG with good response and without toxicity" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S2" "paginaFinal" => "S3" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Tratamiento repetido con una dosis baja de <span class="elsevierStyleSup">131</span>I-MIBG con buena respuesta y sin toxicidad" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 1675 "Ancho" => 2583 "Tamanyo" => 217653 ] ] "descripcion" => array:1 [ "en" => "<p id="spar1010" class="elsevierStyleSimplePara elsevierViewall">positive 123I-MIBG manifestations of the left axilla (A black arrow) and of the mediastinum (A and B red arrow), confirmed by SPECT/CT (B), including malign bone infiltration of the left humerus (A) confirmed by SPECT/CT (B). The following 123I-MIBG imaging after 131I-MIBG therapy clearly depicted the decline of 123I-MIBG accumulation of the lymph nodes along the left axilla (C) and the mediastinum (C and D). A diffuse 123I-MIBG infiltration of the left humerus (A–D) remained stable after 131I-MIBG therapy.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Lisa-Maria Rossetti, Alexander Stephan Kroiss, Christian Uprimny, Sabine Buxbaum, Irene Johanna Virgolini" "autores" => array:5 [ 0 => array:2 [ "nombre" => "Lisa-Maria" "apellidos" => "Rossetti" ] 1 => array:2 [ "nombre" => "Alexander Stephan" "apellidos" => "Kroiss" ] 2 => array:2 [ "nombre" => "Christian" "apellidos" => "Uprimny" ] 3 => array:2 [ "nombre" => "Sabine" "apellidos" => "Buxbaum" ] 4 => array:2 [ "nombre" => "Irene Johanna" "apellidos" => "Virgolini" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S2253654X20301402" "doi" => "10.1016/j.remn.2020.08.003" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X20301402?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S225380892030121X?idApp=UINPBA00004N" "url" => "/22538089/00000041000000S1/v1_202207210552/S225380892030121X/v1_202207210552/en/main.assets" ] "en" => array:15 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Diffuse increased uptake in intrahepatic biliary ducts on <span class="elsevierStyleSup">18</span>F-FDG PET/CT in a case with primary sclerosing cholangitis" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S4" "paginaFinal" => "S5" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Mine Araz, Pınar Akkuş, Muhammet Halil Baltacioglu, Cigdem Soydal, K. Metin Kır" "autores" => array:5 [ 0 => array:4 [ "nombre" => "Mine" "apellidos" => "Araz" "email" => array:1 [ 0 => "minesoylu@yahoo.com" ] "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] 1 => array:2 [ "nombre" => "Pınar" "apellidos" => "Akkuş" ] 2 => array:2 [ "nombre" => "Muhammet Halil" "apellidos" => "Baltacioglu" ] 3 => array:2 [ "nombre" => "Cigdem" "apellidos" => "Soydal" ] 4 => array:2 [ "nombre" => "K. Metin" "apellidos" => "Kır" ] ] "afiliaciones" => array:1 [ 0 => array:2 [ "entidad" => "Ankara University, Medical School Nuclear Medicine Department, Turkey" "identificador" => "aff0005" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Aumento difuso de la captación en los conductos biliares intrahepáticos en <span class="elsevierStyleSup">18</span>F-FDGPET/TC en un caso de colangitis esclerosante primaria" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 843 "Ancho" => 1505 "Tamanyo" => 141949 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0025" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Whole body maximum intensity projection (MIP) (A), axial computerized tomography (CT) (B), axial fusion (C) coronal CT (D) and coronal fusion (E) images of liver Diffuse linear increased <span class="elsevierStyleSup">18</span>F-FDG uptake was seen throughout the intrahepatic bile ducts (SUVmax:8.0), probably due to inflammatory process, together with mild radiotracer uptake in the periportal lymph nodes (SUVmax:4.6).</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">We represent a 46 years old female candidate for liver transplantation with primary sclerosing cholangitis. On preoperative diagnostic contrast enhanced abdominal CT, multiple lymphadenopathies in the portal area were detected. <span class="elsevierStyleSup">18</span>F-FDG PET/CT was ordered to rule out malignant disease. No focal area of a significantly increased metabolic activity suggestive of malignant disease was detected. Diffuse increased <span class="elsevierStyleSup">18</span>F-FDG uptake was seen along the intrahepatic bile ducts, demonstrating the disseminated inflammatory process (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>).</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0010" class="elsevierStylePara elsevierViewall">Primary sclerosing cholangitis is a progressive cholestatic disease and frequently ends up with liver failure. It is characterized by inflammation, fibrosis and strictures of intra-extrahepatic biliary ducts. Although etiology is still not exactly known, the most accepted theory is the autoimmune mechanism and inflammatory response to accumulated bacteria and bile salts precipitating due to cholestasis.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a><span class="elsevierStyleSup">18</span>F-FDG is the most commonly used radiopharmaceutical in nuclear oncology. Nonspecific uptake mechanism of <span class="elsevierStyleSup">18</span>F-FDG by tumor cells is also possible by inflammatory cells with increased metabolic activity. Thus, its role in detection, follow up and therapy response assessment of benign conditions like systemic inflammatory diseases has also been reported. Radiological imaging modalities like USG, CT and MRI are most frequently used in follow up of PSC. Secondary malignancies like hepatobiliary cancer and colon cancer may develop in advanced disease. <span class="elsevierStyleSup">18</span>F-FDG PET/CT is indicated to rule out secondary malignancies and for screening before transplantation. Some authors have also reported that it can be beneficial in follow up of strictures in PSC.<a class="elsevierStyleCrossRefs" href="#bib0010"><span class="elsevierStyleSup">2,3</span></a> However, these studies are focused on the intensity of the tracer uptake (mostly represented with SUV) in order to detect carcinoma. However, the distribution pattern has not been considered before.</p><p id="par0015" class="elsevierStylePara elsevierViewall">In this case, supporting previous publications, we presented the visualisation of diffuse <span class="elsevierStyleSup">18</span>F-FDG uptake of intrahepatic bile ducts, almost mapping the inflammatory process of the whole biliary tree in advanced stage PSC, which is to the best of our knowledge, the most striking image of PSC detected by <span class="elsevierStyleSup">18</span>F-FDG PET/CT. Diffuse linear uptake should be indicative of benign process anyway, even if a high value of uptake is calculated.</p></span>" "pdfFichero" => "main.pdf" "tienePdf" => true "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Araz M, Akkuş P, Baltacioglu MH, Soydal C, Kır KM. Aumento de la captación difusa en los conductos biliares intrahepáticos en la PET/TC con <span class="elsevierStyleSup">18</span>F-FDG en un caso con colangitis esclerosante primaria. Rev Esp Med Nucl Imagen Mol. 2022;41:S4–S5.</p>" ] ] "multimedia" => array:1 [ 0 => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 843 "Ancho" => 1505 "Tamanyo" => 141949 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0025" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Whole body maximum intensity projection (MIP) (A), axial computerized tomography (CT) (B), axial fusion (C) coronal CT (D) and coronal fusion (E) images of liver Diffuse linear increased <span class="elsevierStyleSup">18</span>F-FDG uptake was seen throughout the intrahepatic bile ducts (SUVmax:8.0), probably due to inflammatory process, together with mild radiotracer uptake in the periportal lymph nodes (SUVmax:4.6).</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:3 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Primary sclerosing cholangitis" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:2 [ 0 => "Y.M. Lee" 1 => "M.M. Kaplan" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1056/NEJM199504063321406" "Revista" => array:5 [ "tituloSerie" => "N Engl J Med" "fecha" => "1995" "volumen" => "332" "paginaInicial" => "924" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/7877651" "web" => "Medline" ] ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "The values of F-8 FDG PET in patients with primary sclerosing cholangitis and cholangiocarcinoma using visual and semiquantitative analysis" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "K. Alkhawaldeh" 1 => "S. Faltten" 2 => "H.J. Biersack" 3 => "S. Ezziddin" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1097/RLU.0b013e3182291a64" "Revista" => array:6 [ "tituloSerie" => "Clin Nucl Med" "fecha" => "2011" "volumen" => "36" "paginaInicial" => "879" "paginaFinal" => "883" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/21892037" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Monitoring dominant strictures in primary sclerosing cholangitis with brush cytology and FDG-PET" "autores" => array:1 [ 0 => array:2 [ "etal" => true "autores" => array:6 [ 0 => "P. Sangfelt" 1 => "A. Sundin" 2 => "A. Wanders" 3 => "I. Rasmussen" 4 => "B.M. Karlson" 5 => "A. Bergquist" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1016/j.jhep.2014.07.032" "Revista" => array:6 [ "tituloSerie" => "J Hepatol" "fecha" => "2014" "volumen" => "61" "paginaInicial" => "1352" "paginaFinal" => "1357" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/25111173" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] "agradecimientos" => array:1 [ 0 => array:4 [ "identificador" => "xack617732" "titulo" => "Acknowledgements" "texto" => "<p id="par0020" class="elsevierStylePara elsevierViewall">None to declare.</p>" "vista" => "all" ] ] ] "idiomaDefecto" => "en" "url" => "/22538089/00000041000000S1/v1_202207210552/S2253808920301634/v1_202207210552/en/main.assets" "Apartado" => array:4 [ "identificador" => "7927" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Interesting images" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/22538089/00000041000000S1/v1_202207210552/S2253808920301634/v1_202207210552/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808920301634?idApp=UINPBA00004N" ]
Consulte los artículos y contenidos publicados en éste medio, además de los e-sumarios de las revistas científicas en el mismo momento de publicación
Esté informado en todo momento gracias a las alertas y novedades
Acceda a promociones exclusivas en suscripciones, lanzamientos y cursos acreditados
The Revista Española de Medicina Nuclear e Imagen Molecular (Spanish Journal of Nuclear Medicine and Molecular Imaging), was founded in 1982, and is the official journal of the Spanish Society of Nuclear Medicine and Molecular Imaging, which has more than 700 members. The Journal, which publishes 6 regular issues per year, has the promotion of research and continuing education in all fields of Nuclear Medicine as its main aim. For this, its principal sections are Originals, Clinical Notes, Images of Interest, and Special Collaboration articles. The works may be submitted in Spanish or English and are subjected to a peer review process. In 2009, it became the leading Spanish journal in the field of Medical Imaging on having an Impact Factor , awarded by the Journal Citation Reports.
Science Citation Index Expander, Medline, IME, Bibliomed, EMBASE/Excerpta Medica, Healthstar, Cancerlit, Toxine, Inside Conferences, Scopus
See moreThe Impact Factor measures the average number of citations received in a particular year by papers published in the journal during the two preceding years.
© Clarivate Analytics, Journal Citation Reports 2022
SRJ is a prestige metric based on the idea that not all citations are the same. SJR uses a similar algorithm as the Google page rank; it provides a quantitative and qualitative measure of the journal's impact.
See moreSNIP measures contextual citation impact by wighting citations based on the total number of citations in a subject field.
See more
Interesting Images: Surprising and didactic findings from clinical practice
More info
Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)

¿Es usted profesional sanitario apto para prescribir o dispensar medicamentos?
Are you a health professional able to prescribe or dispense drugs?
Você é um profissional de saúde habilitado a prescrever ou dispensar medicamentos