Interesting Images: Surprising and didactic findings from clinical practice
More infoArticle

Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)
array:24 [ "pii" => "S2253808921000082" "issn" => "22538089" "doi" => "10.1016/j.remnie.2020.11.001" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1244" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "copyrightAnyo" => "2021" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S6-S7" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "Traduccion" => array:1 [ "es" => array:19 [ "pii" => "S2253654X20302079" "issn" => "2253654X" "doi" => "10.1016/j.remn.2020.11.002" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1244" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S6-S7" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "es" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Imágenes de interés</span>" "titulo" => "Localización inusual del ganglio centinela en la región glútea inferior en una paciente con tumor de ovario" "tienePdf" => "es" "tieneTextoCompleto" => "es" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S6" "paginaFinal" => "S7" ] ] "titulosAlternativos" => array:1 [ "en" => array:1 [ "titulo" => "Unusual location of sentinel node in the inferior gluteal region in a patient with ovarian tumor" ] ] "contieneTextoCompleto" => array:1 [ "es" => true ] "contienePdf" => array:1 [ "es" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:7 [ "identificador" => "fig0010" "etiqueta" => "Figura 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 543 "Ancho" => 2335 "Tamanyo" => 119908 ] ] "descripcion" => array:1 [ "es" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">Imágenes SPECT/TC de la paciente. Las flechas muestran los ganglios centinelas paraaórticos.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "M. Farazestanian, S. Ataei Nakhaei, A. Azad, N. Jahani, R. Sadeghi" "autores" => array:5 [ 0 => array:2 [ "nombre" => "M." "apellidos" => "Farazestanian" ] 1 => array:2 [ "nombre" => "S." "apellidos" => "Ataei Nakhaei" ] 2 => array:2 [ "nombre" => "A." "apellidos" => "Azad" ] 3 => array:2 [ "nombre" => "N." "apellidos" => "Jahani" ] 4 => array:2 [ "nombre" => "R." "apellidos" => "Sadeghi" ] ] ] ] ] "idiomaDefecto" => "es" "Traduccion" => array:1 [ "en" => array:9 [ "pii" => "S2253808921000082" "doi" => "10.1016/j.remnie.2020.11.001" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808921000082?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X20302079?idApp=UINPBA00004N" "url" => "/2253654X/00000041000000S1/v1_202207160644/S2253654X20302079/v1_202207160644/es/main.assets" ] ] "itemSiguiente" => array:18 [ "pii" => "S2253808921000616" "issn" => "22538089" "doi" => "10.1016/j.remnie.2021.03.015" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1267" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S8-S9" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Detection of Parotid Metastasis from Retinoblastoma by <span class="elsevierStyleSup">18</span>F-FDG PET/CT scan" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S8" "paginaFinal" => "S9" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Detección de metástasis parotídeas de retinoblastoma mediante PET/TC con <span class="elsevierStyleSup">18</span>F-FDG" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Figure 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 2204 "Ancho" => 2500 "Tamanyo" => 320649 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Figure " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">The MIP image (A) showed elevated FDG activity in the right face region (A, solid arrows). No abnormal activity was noted on the axial images of the right orbit region (B, arrowheads). On the axial images of the face (C), the increased tracer activity (solid arrows) corresponded to a soft tissue mass (the size of 3.4 cm) in the right parotid with the SUVmax of 8.9.</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Huijuan Liu, Yuhong Liu, Yue Chen, Huipan Liu" "autores" => array:4 [ 0 => array:2 [ "nombre" => "Huijuan" "apellidos" => "Liu" ] 1 => array:2 [ "nombre" => "Yuhong" "apellidos" => "Liu" ] 2 => array:2 [ "nombre" => "Yue" "apellidos" => "Chen" ] 3 => array:2 [ "nombre" => "Huipan" "apellidos" => "Liu" ] ] ] ] ] "idiomaDefecto" => "en" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808921000616?idApp=UINPBA00004N" "url" => "/22538089/00000041000000S1/v1_202207210552/S2253808921000616/v1_202207210552/en/main.assets" ] "itemAnterior" => array:19 [ "pii" => "S2253808920301634" "issn" => "22538089" "doi" => "10.1016/j.remnie.2020.12.005" "estado" => "S300" "fechaPublicacion" => "2022-01-01" "aid" => "1233" "copyright" => "Sociedad Española de Medicina Nuclear e Imagen Molecular" "documento" => "article" "crossmark" => 1 "subdocumento" => "sco" "cita" => "Rev Esp Med Nucl Imagen Mol. 2022;41 Supl 1:S4-S5" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "en" => array:11 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Diffuse increased uptake in intrahepatic biliary ducts on <span class="elsevierStyleSup">18</span>F-FDG PET/CT in a case with primary sclerosing cholangitis" "tienePdf" => "en" "tieneTextoCompleto" => "en" "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S4" "paginaFinal" => "S5" ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Aumento difuso de la captación en los conductos biliares intrahepáticos en <span class="elsevierStyleSup">18</span>F-FDGPET/TC en un caso de colangitis esclerosante primaria" ] ] "contieneTextoCompleto" => array:1 [ "en" => true ] "contienePdf" => array:1 [ "en" => true ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 843 "Ancho" => 1505 "Tamanyo" => 141949 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0025" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Whole body maximum intensity projection (MIP) (A), axial computerized tomography (CT) (B), axial fusion (C) coronal CT (D) and coronal fusion (E) images of liver Diffuse linear increased <span class="elsevierStyleSup">18</span>F-FDG uptake was seen throughout the intrahepatic bile ducts (SUVmax:8.0), probably due to inflammatory process, together with mild radiotracer uptake in the periportal lymph nodes (SUVmax:4.6).</p>" ] ] ] "autores" => array:1 [ 0 => array:2 [ "autoresLista" => "Mine Araz, Pınar Akkuş, Muhammet Halil Baltacioglu, Cigdem Soydal, K. Metin Kır" "autores" => array:5 [ 0 => array:2 [ "nombre" => "Mine" "apellidos" => "Araz" ] 1 => array:2 [ "nombre" => "Pınar" "apellidos" => "Akkuş" ] 2 => array:2 [ "nombre" => "Muhammet Halil" "apellidos" => "Baltacioglu" ] 3 => array:2 [ "nombre" => "Cigdem" "apellidos" => "Soydal" ] 4 => array:2 [ "nombre" => "K. Metin" "apellidos" => "Kır" ] ] ] ] ] "idiomaDefecto" => "en" "Traduccion" => array:1 [ "es" => array:9 [ "pii" => "S2253654X20301943" "doi" => "10.1016/j.remn.2020.09.004" "estado" => "S300" "subdocumento" => "" "abierto" => array:3 [ "ES" => false "ES2" => false "LATM" => false ] "gratuito" => false "lecturas" => array:1 [ "total" => 0 ] "idiomaDefecto" => "es" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253654X20301943?idApp=UINPBA00004N" ] ] "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808920301634?idApp=UINPBA00004N" "url" => "/22538089/00000041000000S1/v1_202207210552/S2253808920301634/v1_202207210552/en/main.assets" ] "en" => array:17 [ "idiomaDefecto" => true "cabecera" => "<span class="elsevierStyleTextfn">Interesting images</span>" "titulo" => "Unusual location of sentinel node in the inferior gluteal region in a patient with ovarian tumor" "tieneTextoCompleto" => true "paginas" => array:1 [ 0 => array:2 [ "paginaInicial" => "S6" "paginaFinal" => "S7" ] ] "autores" => array:1 [ 0 => array:4 [ "autoresLista" => "Marjaneh Farazestanian, Saeedeh Ataei Nakhaei, Afrooz Azad, Najmeh Jahani, Ramin Sadeghi" "autores" => array:5 [ 0 => array:3 [ "nombre" => "Marjaneh" "apellidos" => "Farazestanian" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 1 => array:3 [ "nombre" => "Saeedeh" "apellidos" => "Ataei Nakhaei" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] ] ] 2 => array:3 [ "nombre" => "Afrooz" "apellidos" => "Azad" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 3 => array:3 [ "nombre" => "Najmeh" "apellidos" => "Jahani" "referencia" => array:1 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">a</span>" "identificador" => "aff0005" ] ] ] 4 => array:4 [ "nombre" => "Ramin" "apellidos" => "Sadeghi" "email" => array:1 [ 0 => "Sadeghir@mums.ac.ir" ] "referencia" => array:2 [ 0 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">b</span>" "identificador" => "aff0010" ] 1 => array:2 [ "etiqueta" => "<span class="elsevierStyleSup">*</span>" "identificador" => "cor0005" ] ] ] ] "afiliaciones" => array:2 [ 0 => array:3 [ "entidad" => "Women's Health Research Center, Mashhad University of Medical Sciences, Mashhad, Iran" "etiqueta" => "a" "identificador" => "aff0005" ] 1 => array:3 [ "entidad" => "Nuclear Medicine Research Center, Mashhad University of Medical Sciences, Mashhad, Iran" "etiqueta" => "b" "identificador" => "aff0010" ] ] "correspondencia" => array:1 [ 0 => array:3 [ "identificador" => "cor0005" "etiqueta" => "⁎" "correspondencia" => "Corresponding author." ] ] ] ] "titulosAlternativos" => array:1 [ "es" => array:1 [ "titulo" => "Localización inusual del ganglio centinela en la región glútea inferior en una paciente con tumor de ovario" ] ] "resumenGrafico" => array:2 [ "original" => 0 "multimedia" => array:8 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 688 "Ancho" => 2917 "Tamanyo" => 170331 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0010" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">SPECT/CT images of the patient. Arrows show the para-aortic sentinel nodes.</p>" ] ] ] "textoCompleto" => "<span class="elsevierStyleSections"><p id="par0005" class="elsevierStylePara elsevierViewall">A 45-year-old female patient with a right side ovarian pelvic mass suspicious for an ovarian malignancy (8 cm tumor with moderately high CEA = 6 ng/mL and CA-125 = 45 U/mL) was scheduled for surgical removal of the tumor. The day of surgery; after exposing the ovarian tumor, two 37 MBq/0.2 mL injections of Tc-99 m Phytate was done in the utero-ovarian and suspensory ligaments of the involved ovary beneath the peritoneum. The surgeon waited for 10 min and then oophorectomy was carried out. Frozen section showed a benign ovarian pathology (benign cystadenoma) and no lymphadenectomy was done. Our case is a patient of an ongoing study on feasibility of sentinel node biopsy and lymphatic mapping in patients with ovarian mass with high probability of malignancy and the patient gave an informed consent before surgery. According to our protocol patients with benign frozen section pathology undergo lymphoscintigraphy of abdominopelvic area the day after surgery (<a class="elsevierStyleCrossRef" href="#fig0005">Fig. 1</a>).</p><elsevierMultimedia ident="fig0005"></elsevierMultimedia><p id="par0010" class="elsevierStylePara elsevierViewall">The location of the para-aortic sentinel nodes was shown in better detail on SPECT/CT images (<a class="elsevierStyleCrossRef" href="#fig0010">Fig. 2</a>). In addition to the para-aortic sentinel nodes, a sentinel node was noted in the left inferior gluteal region (<a class="elsevierStyleCrossRef" href="#fig0015">Fig. 3</a>) which was not visible on the planar images most likely due to deep location of the node.</p><elsevierMultimedia ident="fig0010"></elsevierMultimedia><elsevierMultimedia ident="fig0015"></elsevierMultimedia><p id="par0015" class="elsevierStylePara elsevierViewall">Sentinel node mapping in ovarian tumors is feasible and several groups worldwide reported excellent results for this procedure.<a class="elsevierStyleCrossRef" href="#bib0005"><span class="elsevierStyleSup">1</span></a> The lymphatic drainage of ovaries is to the para-aortic and pelvic regions which mandates pelvic and para-aortic lymph node dissection in ovarian malignancies. Although lymphatic drainage of skin tumors of the pelvic areas has been reported rarely to be in the gluteal lymph nodes,<a class="elsevierStyleCrossRef" href="#bib0010"><span class="elsevierStyleSup">2</span></a> to the extent of our knowledge, lymphatic drainage of ovaries to the gluteal lymph nodes has not been reported before in the literature. Gluteal lymph nodes are the extension of internal iliac lymph nodes and according to the accompanying vessels, gluteal lymph nodes are divided to superior and inferior gluteal lymph nodes.<a class="elsevierStyleCrossRef" href="#bib0015"><span class="elsevierStyleSup">3</span></a> Our case showed an unusual location of lymphatic drainage in an ovarian tumor (crossed drainage from a right side tumor to the left gluteal region). In addition our case shows the importance of SPECT/CT in sentinel node mapping to explore the unexpected locations of sentinel nodes.</p><span id="sec0005" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0005">Funding source</span><p id="par0020" class="elsevierStylePara elsevierViewall">This study was supported by vice chancellery of research of <span class="elsevierStyleGrantSponsor" id="gs0005">Mashhad University of Medical Sciences</span> with the approval number of <span class="elsevierStyleGrantNumber" refid="gs0005">981455</span>.</p></span><span id="sec0010" class="elsevierStyleSection elsevierViewall"><span class="elsevierStyleSectionTitle" id="sect0010">Conflict of interest</span><p id="par0025" class="elsevierStylePara elsevierViewall">All authors declare no conflict of interest.</p></span></span>" "textoCompletoSecciones" => array:1 [ "secciones" => array:3 [ 0 => array:2 [ "identificador" => "sec0005" "titulo" => "Funding source" ] 1 => array:2 [ "identificador" => "sec0010" "titulo" => "Conflict of interest" ] 2 => array:1 [ "titulo" => "References" ] ] ] "pdfFichero" => "main.pdf" "tienePdf" => true "fechaRecibido" => "2020-11-02" "fechaAceptado" => "2020-11-19" "NotaPie" => array:1 [ 0 => array:2 [ "etiqueta" => "☆" "nota" => "<p class="elsevierStyleNotepara" id="npar0005">Please cite this article as: Farazestanian M, Ataei Nakhaei S, Azad A, Jahani N, Sadeghi R. Ubicación inusual del ganglio centinela en la región glútea inferior en una paciente con tumor de ovario. Rev Esp Med Nucl Imagen Mol. 2022;41:S6–S7.</p>" ] ] "multimedia" => array:3 [ 0 => array:8 [ "identificador" => "fig0005" "etiqueta" => "Fig. 1" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr1.jpeg" "Alto" => 864 "Ancho" => 2500 "Tamanyo" => 174767 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0005" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0005" class="elsevierStyleSimplePara elsevierViewall">Planar anterior/posterior images of the patient showed remaining activities of the injection sites (narrow arrows) as well as para-aortic sentinel nodes (bold arrows).</p>" ] ] 1 => array:8 [ "identificador" => "fig0010" "etiqueta" => "Fig. 2" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr2.jpeg" "Alto" => 688 "Ancho" => 2917 "Tamanyo" => 170331 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0010" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0010" class="elsevierStyleSimplePara elsevierViewall">SPECT/CT images of the patient. Arrows show the para-aortic sentinel nodes.</p>" ] ] 2 => array:8 [ "identificador" => "fig0015" "etiqueta" => "Fig. 3" "tipo" => "MULTIMEDIAFIGURA" "mostrarFloat" => true "mostrarDisplay" => false "figura" => array:1 [ 0 => array:4 [ "imagen" => "gr3.jpeg" "Alto" => 705 "Ancho" => 3000 "Tamanyo" => 164849 ] ] "detalles" => array:1 [ 0 => array:3 [ "identificador" => "at0015" "detalle" => "Fig. " "rol" => "short" ] ] "descripcion" => array:1 [ "en" => "<p id="spar0015" class="elsevierStyleSimplePara elsevierViewall">SPECT/CT images of the patient which show a sentinel node in the left inferior gluteal area (arrow).</p>" ] ] ] "bibliografia" => array:2 [ "titulo" => "References" "seccion" => array:1 [ 0 => array:2 [ "identificador" => "bibs0005" "bibliografiaReferencia" => array:3 [ 0 => array:3 [ "identificador" => "bib0005" "etiqueta" => "1" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Lymphatic mapping and sentinel node biopsy in ovarian tumors: a study using intra-operative Tc-99m-phytate and lymphoscintigraphy imaging" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:6 [ 0 => "M. Hassanzadeh" 1 => "E. Hosseini Farahabadi" 2 => "Z. Yousefi" 3 => "S. Kadkhodayan" 4 => "L. Zarifmahmoudi" 5 => "R. Sadeghi" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1186/s13048-016-0265-4" "Revista" => array:6 [ "tituloSerie" => "J Ovarian Res." "fecha" => "2016" "volumen" => "9" "paginaInicial" => "55" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/27604260" "web" => "Medline" ] ] "itemHostRev" => array:3 [ "pii" => "S0003999315014768" "estado" => "S300" "issn" => "00039993" ] ] ] ] ] ] ] 1 => array:3 [ "identificador" => "bib0010" "etiqueta" => "2" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Superior gluteal lymph node metastasis of melanoma" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "M. Fujiwara" 1 => "T. Nagata" 2 => "Y. Matsushita" 3 => "H. Fukamizu" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.1111/1346-8138.12257" "Revista" => array:6 [ "tituloSerie" => "J Dermatol." "fecha" => "2013" "volumen" => "40" "paginaInicial" => "852" "paginaFinal" => "853" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/23962005" "web" => "Medline" ] ] ] ] ] ] ] ] 2 => array:3 [ "identificador" => "bib0015" "etiqueta" => "3" "referencia" => array:1 [ 0 => array:2 [ "contribucion" => array:1 [ 0 => array:2 [ "titulo" => "Use of MRI to identify enlarged inferior gluteal and ischioanal lymph nodes and associated findings related to the primary disease" "autores" => array:1 [ 0 => array:2 [ "etal" => false "autores" => array:4 [ 0 => "C. Uzun" 1 => "A. Erden" 2 => "E. Dusunceli Atman" 3 => "E. Ustuner" ] ] ] ] ] "host" => array:1 [ 0 => array:2 [ "doi" => "10.5152/dir.2016.15478" "Revista" => array:6 [ "tituloSerie" => "Diagn Interv Radiol." "fecha" => "2016" "volumen" => "22" "paginaInicial" => "314" "paginaFinal" => "318" "link" => array:1 [ 0 => array:2 [ "url" => "https://www.ncbi.nlm.nih.gov/pubmed/27113423" "web" => "Medline" ] ] ] ] ] ] ] ] ] ] ] ] ] "idiomaDefecto" => "en" "url" => "/22538089/00000041000000S1/v1_202207210552/S2253808921000082/v1_202207210552/en/main.assets" "Apartado" => array:4 [ "identificador" => "7927" "tipo" => "SECCION" "en" => array:2 [ "titulo" => "Interesting images" "idiomaDefecto" => true ] "idiomaDefecto" => "en" ] "PDF" => "https://static.elsevier.es/multimedia/22538089/00000041000000S1/v1_202207210552/S2253808921000082/v1_202207210552/en/main.pdf?idApp=UINPBA00004N&text.app=https://www.elsevier.es/" "EPUB" => "https://multimedia.elsevier.es/PublicationsMultimediaV1/item/epub/S2253808921000082?idApp=UINPBA00004N" ]
Consulte los artículos y contenidos publicados en éste medio, además de los e-sumarios de las revistas científicas en el mismo momento de publicación
Esté informado en todo momento gracias a las alertas y novedades
Acceda a promociones exclusivas en suscripciones, lanzamientos y cursos acreditados
The Revista Española de Medicina Nuclear e Imagen Molecular (Spanish Journal of Nuclear Medicine and Molecular Imaging), was founded in 1982, and is the official journal of the Spanish Society of Nuclear Medicine and Molecular Imaging, which has more than 700 members. The Journal, which publishes 6 regular issues per year, has the promotion of research and continuing education in all fields of Nuclear Medicine as its main aim. For this, its principal sections are Originals, Clinical Notes, Images of Interest, and Special Collaboration articles. The works may be submitted in Spanish or English and are subjected to a peer review process. In 2009, it became the leading Spanish journal in the field of Medical Imaging on having an Impact Factor , awarded by the Journal Citation Reports.
Science Citation Index Expander, Medline, IME, Bibliomed, EMBASE/Excerpta Medica, Healthstar, Cancerlit, Toxine, Inside Conferences, Scopus
See moreThe Impact Factor measures the average number of citations received in a particular year by papers published in the journal during the two preceding years.
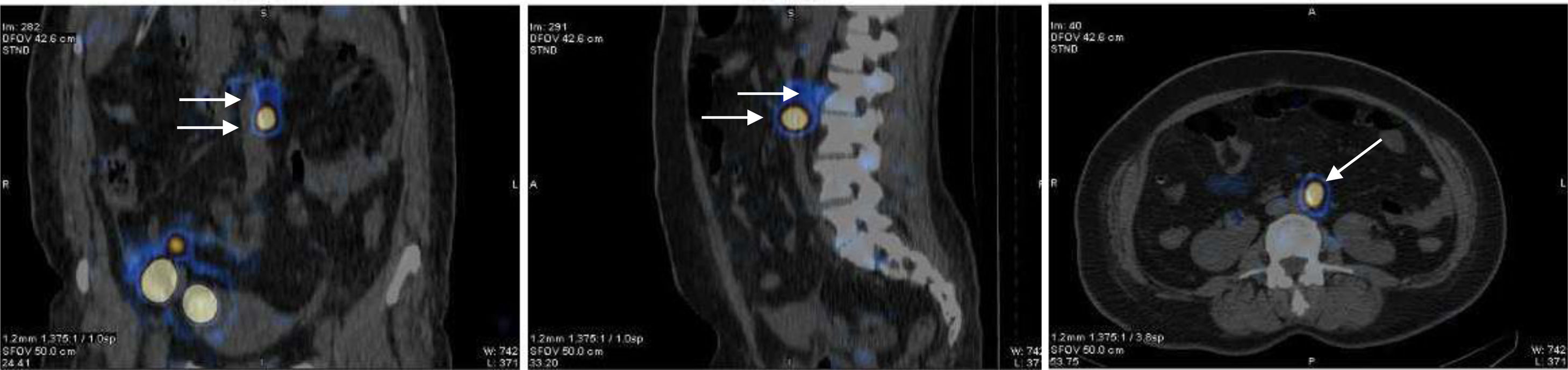
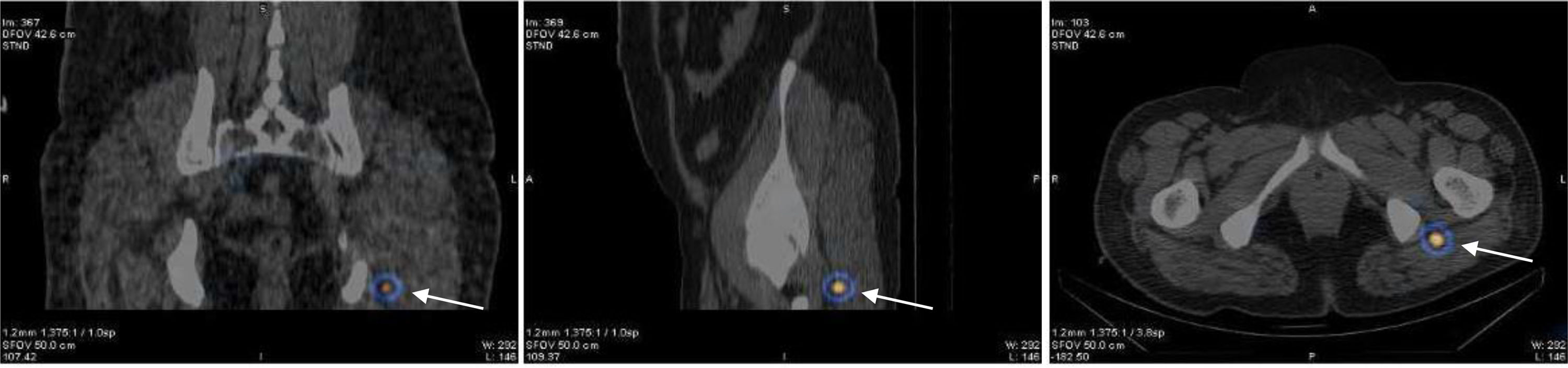
© Clarivate Analytics, Journal Citation Reports 2022
SRJ is a prestige metric based on the idea that not all citations are the same. SJR uses a similar algorithm as the Google page rank; it provides a quantitative and qualitative measure of the journal's impact.
See moreSNIP measures contextual citation impact by wighting citations based on the total number of citations in a subject field.
See more
Interesting Images: Surprising and didactic findings from clinical practice
More info
Revista Española de Medicina Nuclear e Imagen Molecular (English Edition)

¿Es usted profesional sanitario apto para prescribir o dispensar medicamentos?
Are you a health professional able to prescribe or dispense drugs?
Você é um profissional de saúde habilitado a prescrever ou dispensar medicamentos