INTRODUCTION
A significant number of workers is employed in the production and processing of tobacco. They are exposed therefore to hazards related to the structural elements of tobacco plant and the processing method of its dried leaves. There are two factors associated with the work environment and thus possibly related to health problems of tobacco industry workers: 1) the tobacco dust present in the work site and 2) the alterations of tobacco leaves after dampening and heating. There are very few studies about the effect of occupational exposure of tobacco workers. Respiratory disorders and more specifically dyspnea, emphysema and chronic bronchitis have been reported in the past1. Today, the sensitization to substances of the occupational environment and the occurrence of bronchial asthma2-4 are thought to be the main occupational effects. Extrinsic allergic alveolitis5 and increased incidence of allergic rhinitis6 have also been reported. At the antipodes, other researchers argue against occupational effects of tobacco processing on the respiratory system7.
In Greece, one of the largest tobacco producing countries worldwide, such epidemiological studies have not been conducted yet. Aim of this study was to examine the pollution level of the occupational environment and to investigate the effects of the occupational exposure to tobacco dust on the respiratory system of tobacco workers, during the processing of dried tobacco leaves.
MATERIALS AND METHODS
Subjects
Tobacco workers and controls
The research was conducted during 1996-99, in a tobacco factory in the region of Thessaloniki. The whole number of 1,020 seasonal and non-seasonal tobacco workers, were examined (188 men and 832 women aged 19-71, mean age 45.9 ± 9.8 years). The seasonal workers were occupied at an average of 4 months per year, starting from the last month of the spring until the first month of the autumn, i.e. during the processing period of tobacco. The total employment time was measured in months.
The research was conducted with the consent of the Labor Union and the Administration of the factory.
Among the 1618 persons employed in a hospital of Thessaloniki, 469 were selected to participate as controls according to their gender and age, i.e. 87 men and 382 women aged 19-67 (mean age 46.0 ± 13.2 years). Subjects with a history of chest injuries or operations, cardiac disease, pulmonary neoplasm or tuberculosis were excluded. All persons gave their informed consent prior to their inclusion in the study.
Description of the factory
The factory is divided in two areas: 1) Ground floor and first floor. They are large flat areas, with parallel wooden structures with racks. They are used as storage areas for both unprocessed and processed tobacco bundles. 2) The upper floor. It is a large area with several external openings in order to ensure its lighting. This area is indented for the processing of tobacco leaves, feeding, sorting, mixing and redrying as well as their bundling. There exist benches, conveyors, stirring and pressing machines for bundling.
The personnel is classified according to its qualification: 5 carriers, 142 stackers, 569 feeders, 132 sorting workers, 5 craftsmen, 68 sewers, 38 cleaning workers, 37 technicians and 24 administrative workers. Four groups (feeders, sorting workers, sewers, cleaning workers) were working under extremely dusty conditions. Therefore in certain cases they were examined separately. The other 5 groups were considered as one single group.
Research methods
History and respiratory function testing
1. Filling of the questionnaire of the Committee for the Environmental and Occupational Hygiene of the British Medical Research Council-MRC 19868, intended for epidemiological investigations concerning the respiratory system. History was taken in an office provided by the factory administration, where workers filled in the questionnaire after entering separately. The prevalence of chronic bronchitis and rhinitis9 was calculated according to the analysis of the answers.
2. Spirometry was conducted with a dry spirometer Vitalograph Ltd, Buckingham, England, according to the guidelines of the American Thoracic Society10. The spirometer was being calibrated every day before spirometry tests. The Forced Expiratory Volume in one second-FEV1 and the Forced Vital Capacity-FVC were measured. Then the FEV1/FVC ratio and the Forced Expiratory Flow 25-75 %-FEF25-75 % were calculated. The predicted values of the European Respiratory Society11 were used. The chronic obstructive pulmonary disease (COPD) was characterized by the symptoms included in the MRC8 questionnaire and by FEV1 < 80 % pred. and FEV1/FVC < 70 %, according to the guidelines of the British Thoracic Society12.
3. Rhinomanometry was performed with a Rhinotest mP500 rhinomanometer of Allergopharma Joachin Ganzer KG Germany. The nasal flows and subsequently the nasal resistances13 were determined by the method of anterior rhinomanometry. Measurements were conducted in 150 Pa (Pascal) and flows were measured in ml/sec. The severity of nasal obstruction was estimated according to rhinomanometry values14,15.
Environmental study
The study of the environment in the tobacco factory was conducted with the use of a 13040/1 sampling device CF Casella & Co Ltd, London England, suitable for measurements of the total suspended dust in the work place16. After mapping of the work place with the use of a portable ausJENA dust meter samples were obtained from twelve sites of the processing area (static samplings). The air flow of the suction pump was set in 1.9 lit/min, as specified in the operating instructions. The dust particles were retained by a filter. An AA filter of Millipore Corporation, Bedford MA USA, was used with 0.8 mm porous diameter. The filter and the cartridge were weighted before and after preset collection time (4 hours), in an electronic balance (with 105 gr error), after they had been demoisturized in a drying unit. Dust concentration was calculated (in mg/m3 of air) by reduction of the dust volume retained in the filter to the totally suctioned air volume.
Special examinations
A tobacco dust sample from the work site was sent to the laboratories of Allergopharma Joachin Ganzer KG Germany for the preparation, by order, of a specific antigen solution suitable for: 1) prick tests and 2) provocation test.
Workers who reported nasal symptoms in the questionnaire and did not demonstrate apparent nasal anatomy disorders neither had they excised nasal conchie underwent voluntarily further examination: 1) Provocation test with the use of a tobacco dust antigen, after local spraying with normal saline. Test was considered as positive when the flow reduction was greater than 40 % of the reference value15. 2) Prick test with the antigen solution of tobacco dust17. 3) Blood sampling for the measurement of total IgE and specific IgE and IgG antibodies against the tobacco dust antigen. The determination of total serum IgE was conducted by the micro-particle enzyme immunoassay method (MEIA), with the use of Abbott Laboratories reagents, in an IMx system analyzer of the same manufacturer. Specific serum IgE against tobacco dust antigen concentration was conducted by enzyme immunoassay method RAST, with the use of cellulose plates, where tobacco proteins from the tobacco factory had been adsorbed. The plates were manufactured in the laboratories of Allergopharma Joachim Ganzer KG Germany. The detection of specific IgG (precipitins) in the serum against the tobacco dust antigen, which was prepared as described above, was conducted by double immunodiffusion method (DID) in agarose18. Tests were conducted in the Immunology Laboratory of the Pulmonary Clinic of the Aristotle' s University of Thessaloniki. The results were compared to the respective ones of administrative employees of the factory without symptoms of rhinitis.
Any worker with dyspnea complaints or wheezing or with bronchial asthma history was submitted to: 1) Reversibility test (spirometry before and 30 minutes after bronchodilatation with inhalation of 400 mg salbutamol) and 2) Systematic measurement of the maximum expiratory flow (PEFR), which is assumed the most reliable test for diagnosis of occupational asthma19, before and by the end of their work and before bedtime as well for two weeks, with a mini-Wright flow meter of Clement Clarke International Ltd. Results were compared to the respective ones of administrative employees of the factory without symptoms of asthma.
Statistical analysis
For the statistical analysis of the quantitative variables' results, under normal data distribution, the student's t-test was used, whereas for the comparison of the qualitative variables the x2 was used. For the comparison of quantitative data among several subgroups the ANOVA analysis was used. For the examination of linear trends the x2 test as modified by Mantel-Haenszel20 was used. Biostatistical analysis was performed using the statistical packet SPSS (Statistical Package for the Social Sciences, 10.1 for Windows, SPPS Inc., Chicago, IC, USA).
RESULTS
Environmental measurements
Twelve dust measurements, each of 4 hours duration, were performed in the processing area, in different sites of the factory. The values of the total suspended dust ranged between 45.3-54.4 mg/m3 of air in the work area. In contrast, values between 0.3-0.9 mg/m3 of air were found out of the work area.
Subjects
A total of 1,020 tobacco workers and 469 controls were examined. The mean age of the workers and controls was not statistically different. As for the smoking habits: a) 34 % of the workers were smokers, whereas 2.8 % were ex smokers and b) 35.8 % of the controls were smokers, whereas 10.9 % were ex smokers. There were statistical differences (r < 0.001) due to the large number of ex smokers among the controls.
Effects on the lower respiratory system
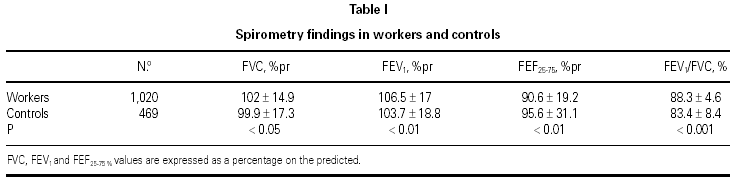
The spirometry findings (m ± SD) as well as the level of statistical differences between workers and controls are listed in table I.
FVC % pred., FEV1 % pred. and FEV1/FVC % ratio were lower in controls, at a statistically significant level. FEF25-75 % % pred. was lower in workers (p < 0.01).
The prevalence of chronic bronchitis was found by the MRC8 questionnaire analysis. According to the analysis, the prevalence of chronic bronchitis was found as follows: a) Workers 8.7 % and b) Controls 20.6 %. The observed differences were statistically significant, p < 0.001.
According to the spirometry values (in compliance with the BTS12 guidelines), chronic obstructive pulmonary disease was found in 13 workers (1.3 %) and 16 controls (3.4 %), p < 0.01. A greater prevalence of chronic bronchitis and chronic obstructive bronchitis was found in controls, probably because there were more smokers among them.
In table II the age, the work site, the employment period, the smoking habits and the respiratory function test results according to the work site of tobacco workers are presented. The statistical error possibility, in the right column of the table at the end, has been calculated with the ANOVA method. Lower FEV1 (p < 0.001) is observed among other workers (stackers, administrative employees etc) who were mostly men smokers and worked for a longer period.
With the use of the multiple regression model FEV1 measurements were found to be affected by the duration of employment (p < 0.001). FEV1 and employment period are better correlated in non smokers (p < 0.01) than in smokers (p < 0.05, fig. 1).
Figure 1.--Effect of the employment time on FEV1.
Both the twenty-seven workers who reported wheezing or dyspnea attacks or chronic asthma history in the questionnaire and the other fourteen who did not present similar symptoms and were used as controls, were not found to have bronchial asthma after the examination.
Effects on the upper respiratory system
The prevalence of rhinitis, the flow sum from both nostrils (Flow Sum in ml/sec, m ± SD) and the prevalence of severe nasal obstruction (Flow Sum < 500 ml/sec) are presented in table III. There were statistically significant differences between workers and controls.
The estimated odds ratio for the occurrence of severe nasal obstruction was found, taking 1 as the basis for the cleaning stuff and with downward trend, 0.64 for the sorting stuff, 0.59 for the feeding stuff, 0.58 for the sewers and 0.22 for the rest of the workers (p < 0.001, fig. 2).
Figure 2.--Odds ratio for the occurrence of severe nasal obstruction according to the work site (1 = cleaners).
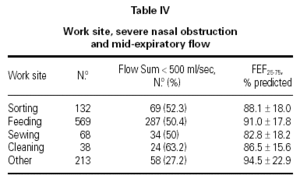
Table IV shows the relation between the work site, the severe nasal obstruction and the mid expiratory flow. It seems that subjects with severe nasal obstruction had also low mid expiratory flow in the spirometry.
When filling out the MRC questionnaire, 279 (27.3 %) workers stated rhinitis. Seventy-six of them accepted to undergo further examination, whereas 35 administrative employees of the tobacco factory, without rhinitis symptoms according to the questionnaire, were used as controls. All the above subjects underwent a nasal provocation test with tobacco dust antigen, prick tests to tobacco dust and measurement of the total IgE, specific IgE and IgG against tobacco dust antigen. Results are listed in table V.
According to the results, there was only a small number of subjects (six) who were sensitized to dried tobacco leaves' dust. Four of them presented also a positive specific IgE.
DISCUSSION
The measured values of the total suspended dust in the work site ranged between 45.3-54.4 mg/m3 of air. The above values were extremely high in comparison with the respective ones reported in other studies: Valic et al2 0.9-27.5 mg/m3, Lander and Gravesen4 0.27-0.89 mg/m3, Viegi et al6 0.7-24.9 mg/m3, Kjaergaard et al7 0.02-5.69 mg/m3 and Ghosh et al21 29.37 mg/m3. We should note that no permitted exposure levels to tobacco dust were specified.
According to the MRC questionnaire analysis, it was found out that 8.6 % of the workers and 20,9 % of the controls were suffering from chronic bronchitis. Chronic bronchitis prevalence was higher in controls, since they presented a higher level of smoking addiction (active smokers 35.8 % against 34 % in workers and 10.9 % ex smokers against 2.8 % respectively). Valic et al2 studied 318 female non smoker workers in a tobacco factory using the MRC questionnaire and found a chronic bronchitis prevalence of 7.5 %, a percentage comparable to this of the present study. Kjaergaard et al studied 75 workers in a cigar manufacturing unit; no increased prevalence of chronic bronchitis7 was detected. However, Huuskonen et al5 in a study of 57 workers in a tobacco factory detected a high percentage of chronic bronchitis (22.2 %). Due to the limited number of the examined workers in the above studies, the comparison to the present study can be considered as uncertain.
The prevalence of chronic obstructive pulmonary disease was 1.3 % in workers, considerably lower than the expected for their age, and 3.4 % in controls (p < 0.01). According to Sichletidis et al22 a low prevalence of chronic obstructive pulmonary disease was found in Northern Greece which ranged between 2.4 % and 4 % in specific population groups.
The predicted FVC %, FEV1 % and FEV1/FVC % values were lower in controls, apart from that of predicted FEF25-75 % % which was lower in workers. It seems that the total employment time in the tobacco factory had a significant effect on the respiratory function of the workers. With the use of the multiple correlation analysis model, it was found that FEV1 was mainly dependent on the employment time and at a minor degree on the smoking habits of the workers. This finding, that the respiratory function and especially the small airways are affected by employment, in general, is in-line with the findings of other authors6,7,23,24.
No bronchial asthma was detected in workers, which may be due to the "healthy worker effect", i.e. early removal of unhealthy persons from the work force, whereas healthy persons continue working, leading to the underestimation of the problem. Wheeze and/or dyspnea attacks in most of the 27 interviewed workers may be due to an exacerbation of chronic bronchitis. Contrary to the findings of this study, 69 % of the workers in a cigar industry studied by Lander and Gravesen reported symptoms related to asthma in comparison with only 6 % of the controls. This fact was attributed to the antigen components of the tobacco dust4. According to Viegi et al in a study of 223 workers in a cigar and tobacco industry, the frequency of asthma symptoms in workers was higher than this of the general population of the same region6. Kjaergaard et al studied 75 workers of a cigar industry and compared them with 50 controls. According to the sensitization test of the workers to the tobacco dust through prick tests, despite more reactions compared to controls, they were mild and without clinical importance7. The incompatibility of the findings between the above and this study could be interpreted through the probable differences in the origin and type of the tobacco leaves. It is well known that the responsible antigens for the antibodies development are contained in tobacco leaves' extracts25. Moreover, it is important to note that there is no standardized tobacco antigen solution in the market, so as to obtain comparable results.
None of the studied workers presented symptoms of extrinsic allergic alveolitis.
It was found that the prevalence of rhinitis was 27.3 % in workers and 17.9 % in controls. The wording of an accurate definition of rhinitis is a very complicated issue for the planning of epidemiological surveys to detect its prevalence. In a way, everybody has "rhinitis", since the nasal mucosa is constantly irritated by various environmental pollutants, viruses and bacteria, and in fact there is no "normal" nasal mucosa26. According to Sibbald and Rink27, in a sample of 5349 examined subjects in London, the prevalence of rhinitis was 24 %. Studies about the incidence of occupational rhinitis are very rare. Hytonen et al during a 5-year observation period registered 1244 new cases of occupational rhinitis in Finland28.
Through correlation of the nasal symptoms and rhinomanometry findings according to the work site, it was concluded that the work site and thus the concentration of tobacco dust in the air played an important role for the occurrence of rhinitis in workers. Chronic dust inhalation is the most common factor responsible for the irritation of nasal mucosa. It is mainly due to its chemical action and bacterial content and less to the mechanical properties of the dust. It has been found that the occupational exposure in a wood processing plant to dust causes severe disorder of the nasal mucociliary clearance29. On the other hand, the inhalation of inert dust at levels up to 25 mg/m3 does not cause alterations of the nasal mucociliary clearance or nasal resistance30.
As concluded by the study concerning the relationship between work sites, mid-expiratory flow and severity of the nasal obstruction, it can be assumed that the damage of the upper respiratory airways, presented as nasal dysfunction, is related to the occurrence of the lower respiratory system impairment. The decrease of the mid-expiratory flow may be due to activation of neural reflexive mechanisms linking the nose to the bronchi31.
After allergic tests, only six workers were found to have been sensitized and presented allergic rhinitis to the dried tobacco leaves dust. The other workers were not sensitized, nor can they be considered as desensitized, given that there was no specific IgG against tobacco dust antigen detected. Positive nasal provocation to the 53 workers with symptomatology in the nose, who apparently were not sensitized to the tobacco dust antigen, indicates the presence of idiopathic rhinitis. The fact that nasal provocation was positive only in 3 out of 35 controls shows that the density of the tobacco dust antigen solution used was not irritant to the normal nasal mucosa. According to the study of Valic et al2, a number of 318 female non smokers in a tobacco factory were found with nasal catarrh 11 %, a percentage no different from that of the control group. On the other hand, Viegi et al6 found that rhinitis prevalence in workers was higher compared to that in the general population. Gleich et al3 reported a case of allergic rhinitis and asthma developed after three years of work in a tobacco processing factory. It is known that the cigarette smoke or other mechanical or chemical stimuli causes inflammation of the respiratory mucosa due to the release of the substance P of unmyelinated C-nerve fibers32. The inflammation of airways' epithelium and the development of nasal hyper-reactivity are closely related33, leading to a permanent nasal mucosa dysfunction. However, an eventual local production and secretion of IgE without systematic sensitization cannot be excluded. This is suggested as for the explanation of allergic rhinitis in patients with negative prick tests34.
This paper was financially supported by the Central Health Council of the Greek Ministry of Health-Welfare and Social Security.