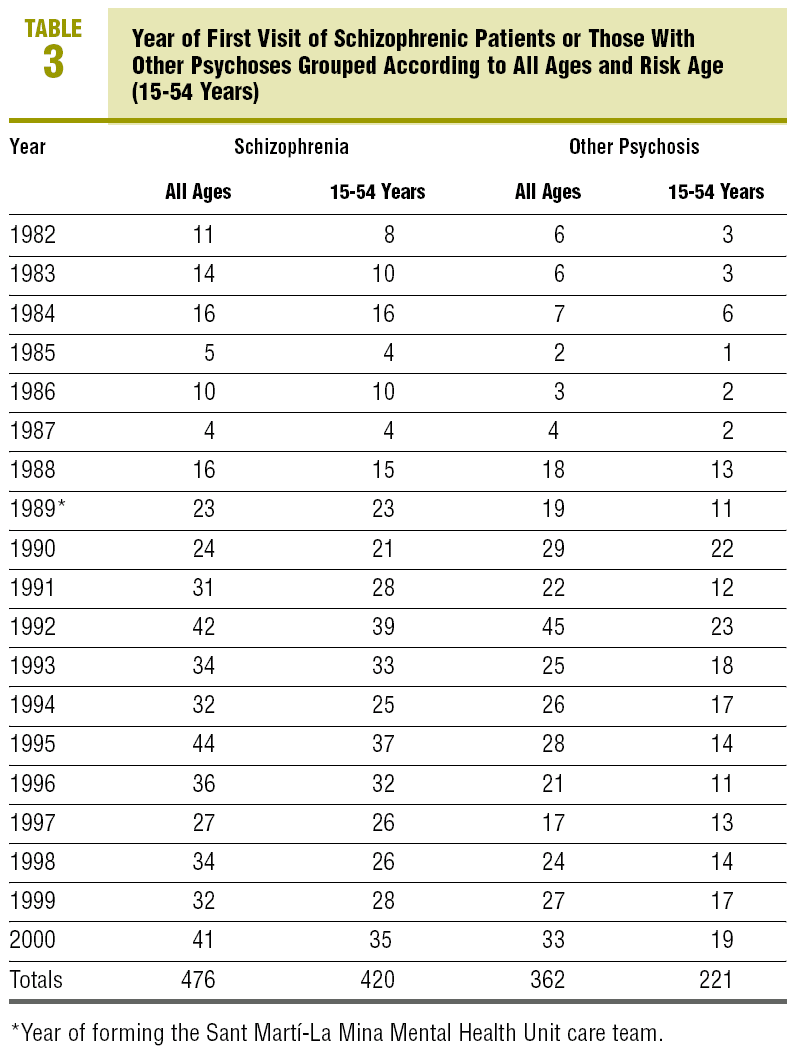Introduction
The epidemiological study of psychosis in general and schizophrenic syndromes in particular is almost a century old. Since the first studies by Faris and Dunham, Roger Bastide, or Raymond Cochrane, works in this field are usually grouped according to whether they have been carried out directly on the general population or by using "psychiatric case registers."1 The scientific literature and the abstracts on the problems of each of these type of studies is very extensive.2-11
Firstly, among the theoretical problems, is that the definition and specifications have to be considered for the syndrome, the group, or the schizophrenic disorder. Another problem is how to detect the patients affected in the community when, as a rule, they tend to avoid contact and therefore, diagnosis. The tendency to under-diagnose10 can lead to researchers taking pragmatic decisions such as, substituting the use of standardised and semi-standardised interviews for a check-list based on the clinical information obtained from clinical histories taken at hospital admissions and/or discharges, which may not be so reliable. It can also lead to grouping patients with different diagnoses, by including or excluding doubtful cases, or to considering the incidence and prevalence data obtained in hospitals or psychiatric services without taking into account the prevalence and incidence latent in the population for years, due to the characteristics of the disorder.3,4
That is why to collect data directly from primary health care (PHC) and mental health units (MHU) closely linked to PHC could be a way of complementing and, perhaps qualifying the data provided by other types of studies.12-15
The objective of this study was to determine the prevalence and incidence of schizophrenia and other psychoses in a MHU with close links to PHC centres.
Methods
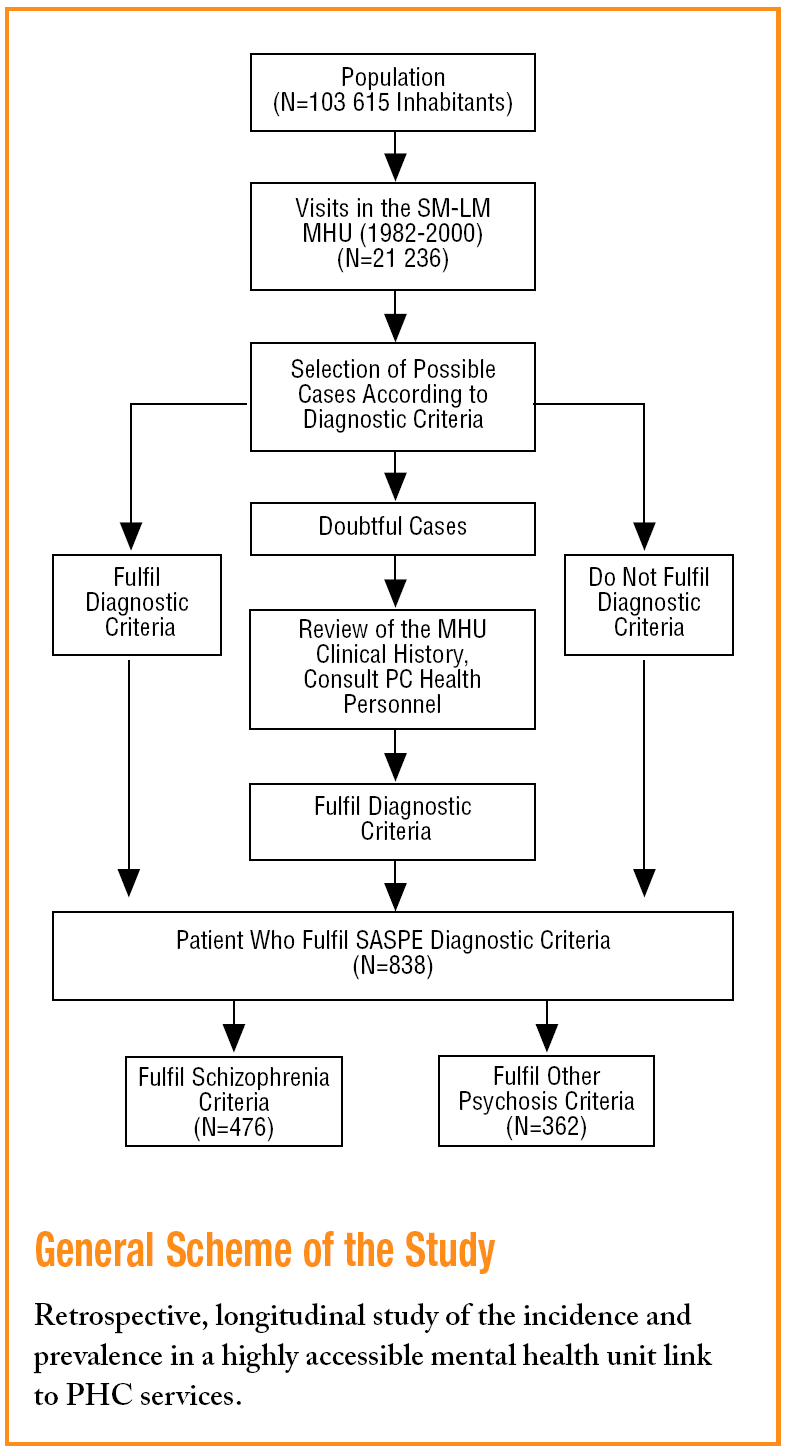
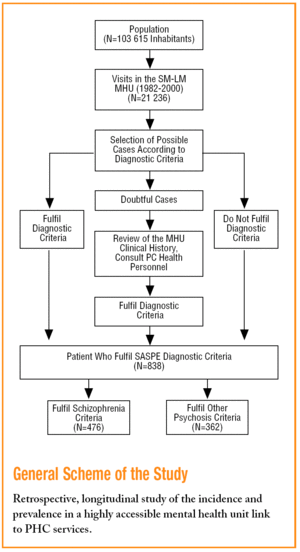
It is a retrospective longitudinal study of a population being treated in the Sant Martí-La Mina MHU (SM-LM-MHU) of the Catalonian Health Institute. This MHU, given its links with PHC and reference teams at secondary and tertiary level, as well as its strict boundaries, can rely on the collaboration of PHC in the detection and validation of cases. This study forms part of a much wider research projects called the SASPE Project (Schizophrenia Alert Signals and Prodromic Signs).13
The population in which the study was carried out is organised into 5 basic health areas which, together, have a total population of 103 615 inhabitants, and have used the SM-LM MHU as a referral centre for all types of mental health disorders, both for treatment and prevention, for more than 20 years. For the type of study proposed, it was necessary to rely on an easily accessible MHU with close links to the PCH centres. The SM-LM MHU appeared to fulfil these requirements, since it functioned within health centres and seemed to be one of the easiest to access in Europe: at the end of 2001, 22 846 people from the registered population (103 615 inhabitants) had visited this MHU at some time, which corresponds to 22.5% of the population in its area.
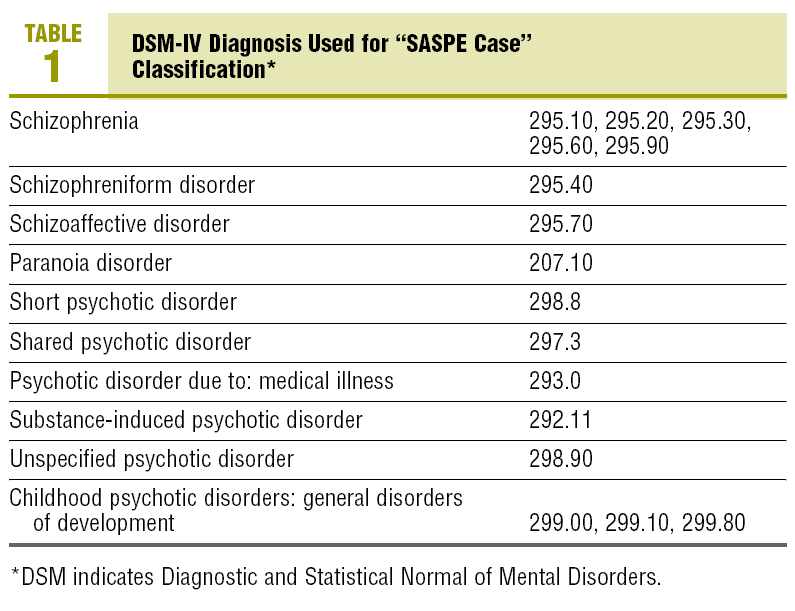
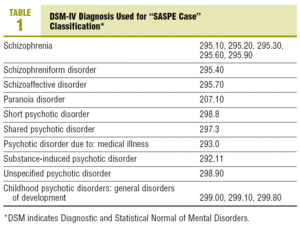
The criteria by which the patients included in Case Register of the MHU were diagnosed as a "SASPE case" are summarised in Tables 1 and 2. All the patients who have visited the MHU at any time can be found in this Register, although later on the treatment may be joint or, in a small percentage of cases, the treatment might have been entrusted to the PCH centre with the collaboration of the specialist team.
The computerised clinical records of all the patients were used to determine the prevalence and incidence of schizophrenia and other psychoses in the reference population. From these patients, those who fulfilled the criteria of a definition of a working case were selected so as not to "over-include" cases. Each record was validated with demographic information, after eliminating the deaths and those who had moved, and where necessary, by consulting their family doctors, nurses or paediatricians, until deciding whether they fulfilled the criteria to be defined as a "SASPE case."
The incidence of schizophrenia and other psychoses, in the general population as well as population age at risk (15-54 years), has been calculated for the period 1998-2000. The prevalence of schizophrenia and other psychoses has been calculated for the whole of the study period (1982-2000). The population denominators of the La Verneda district come from the year 2000 census update and those of La Mina (a municipality of Sant Adrià del Besós), from the 1996 electoral register.
Results
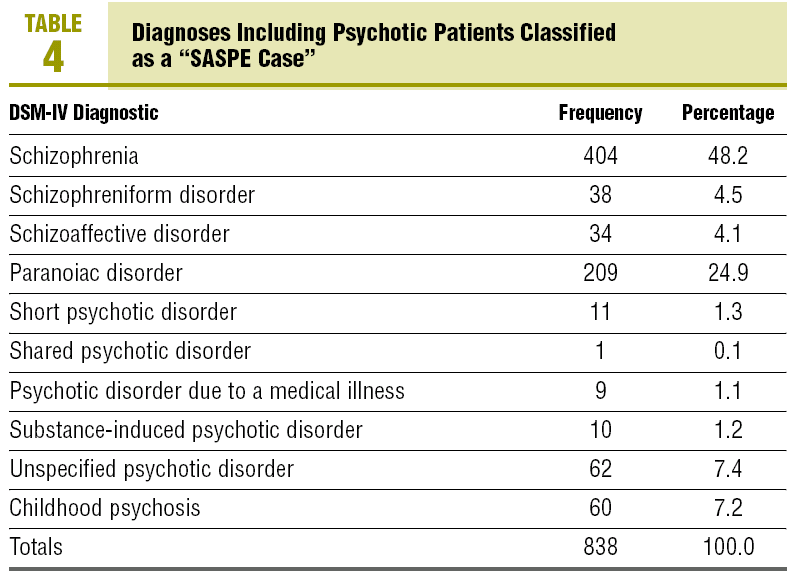
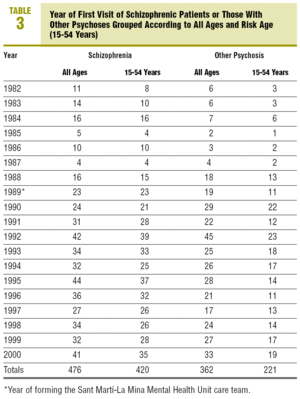
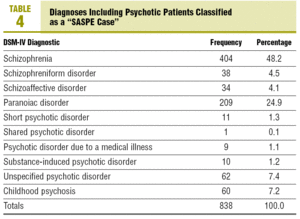
Detection was fairly stable in the team. Since it was formed (in 1989), between 42 and 87 new cases per year have been detected (Table 3). Their diagnoses are summarised in Table 4.
The mean incidence of schizophrenia in the general population in the last 3 years was 3.47 cases per 10 000 inhabitants (95% confidence interval [CI], 2.3-4.6), while in the population at risk (15-54 years), it was 5.09 cases per 10 000 inhabitants (95% CI, 3.2-6.9).
If the cases with psychosis in the general population are taken together, the mean incidence in the last 3 years was 6.17 cases per 10 000 inhabitants (95% CI, 4.6-7.6).
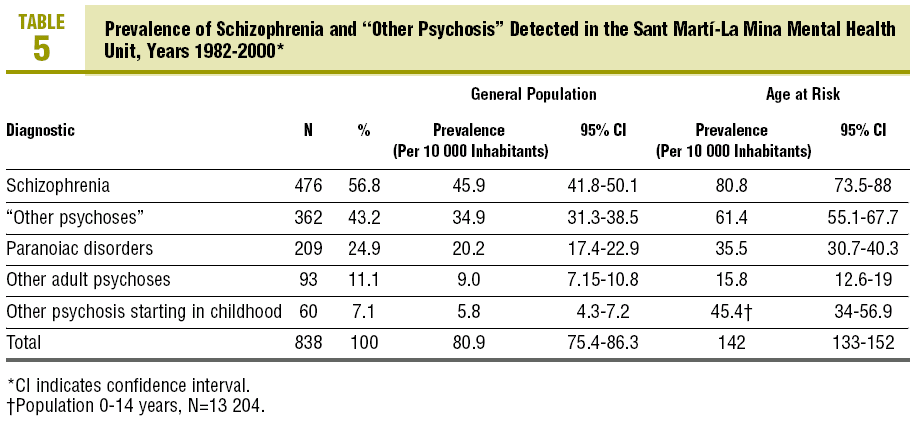
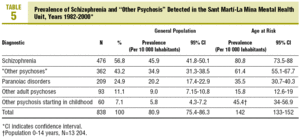
The schizophrenic syndromes, even with these strict criteria, were the most prevalent psychoses in our population: 45.9 per 10 000 inhabitants (95% CI, 41.8-50), in the general population, and 80.8 per 10 000 inhabitants (95% CI, 73.5-88) in the population at risk (Table 5). Its detected prevalence is greater than the rest of the psychoses together and more than twice as high as the paranoid disorders.
Discussion
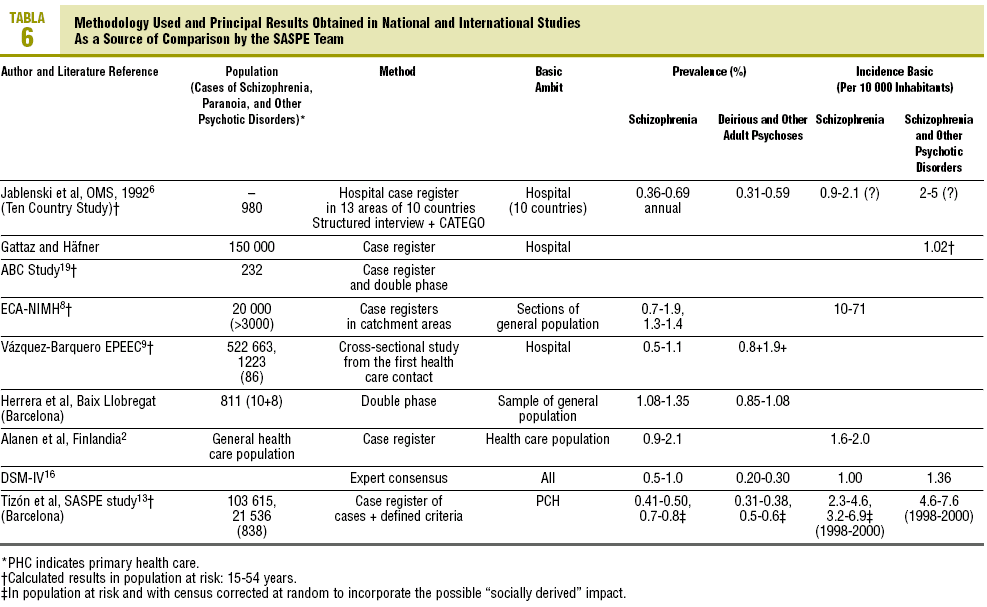
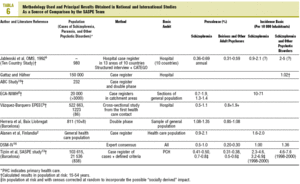
According to the North American National Institute of Mental Health, the annual incidence of schizophrenia varies between 0.9 and 1.3/10 000 in the Epidemiological Catchment Area study.16-20 The German ABC study,4,18,19 had an incidence of 1.02/10 000 in the population at risk (15-54 years). The Spanish study by Vázquez-Barquero in Cantabria9 showed an incidence of 0.80/10 000 and 1.90/10 000 in the population age at risk (15-54 years). The variations in the differences in incidence and prevalence between the different studies can be seen in Table 6.
This disparity has been attributed to the different study populations, to different information sources consulted, as well as the different diagnostic criteria used.
Our intention was to carry out a study not so much on the general population, but on the population "actually cared for" at some time in their history.
For this reason, it seemed ideal to investigate the incidence and prevalence in this health care service in PHC centres and/or MHUs.
Unfortunately, the psychiatric case records are systems that are limited to patients who contact the health care services: if only the hospital services are taken into account, even in the case of schizophrenia, this can lead to a significant bias, by leaving out an important proportion of people affected.
The problem is also observed even if the "psychiatric" case registers are extra-hospital, outpatient or community, which is why it is advisable to carry out studies in the general population such as in PHC: it is a health care service that, if it is sufficiently developed in the country, receives a large amount of all types of illnesses, including mental ones.1,5,12-28
As can be seen, for the group of studies with populations on treatment, the indices provided by the SASPE Project are higher, even after discounting patients who have died or moved, which indicates that there is greater access to this service.
From the results of the present research, it seems that PHC centres and the mental health teams linked to them are good places to detect mental disorders, particularly when it is combined with the stability of the MHU in the same area and with the same population. Studies with a treated population can provide more realistic figures of psychiatric disease in the population and of course, the different characteristics of different types of syndromes and psychopathological problems.
It is traditionally considered that studies in the general population, in double phase, are better to estimate the real incidence and prevalence of psychosis of this population. However, with the results of the present study, that consideration would have to be qualified.
This may offer a new contribution for studies based on psychiatric or PHC centre case records and, in general, on the case records linked with the community clinic and PHC1: with suitably supported PHC doctors it is likely that they could detect more cases than they used to. A relationship with a highly accessible MHU can improve detection (and care) of these types of patients in the health system in general.
Our prevalence results as regards the general population, are somewhat lower than those reported in some international population based studies, probably due to our strict criteria, but it is possible that they are more realistic: all correspond to real cases, continually or repeatedly treated as schizophrenics or psychotics. On the other hand, there is a similarity between our data and the prevalence in the age at risk normally reported for schizophrenia: although it is 1% in American Psychiatric Association estimates,16 these figures are tending to be corrected downwards7,20,22,23 and would be nearer our 0.8% in the at risk age group.
Likewise, we believe that our data are fairly close to the real incidence and prevalence of schizophrenia in a particular population for another reason: because our methodology has allowed us not to mix the schizophrenia diagnosis or other psychosis diagnoses in the same group as often happens. These diagnoses can include the "schizophrenic spectrum" (which can include personality disorders, such as schizotypy or schizoid), and bipolar or depressive psychosis, as in the ABC studies.19
On the other hand, population studies, and more so those of the ECA and the like, as pointed out some time ago,7 create problems of over-dimensionalisation. If, despite everything, our incidence and prevalence data continues to be comparable with them, it is most likely due to either the particular characteristics of the population studied or to a greater ability to pick up "cases" owing to the method used: collection of data of those actually treated in highly accessible mental health services included in the PHC services.
Even taking the results of the German ABC study and the Cantabrian studies into account, it still seems that, in our population, one can be sure there is a number of schizophrenics and patients with other psychoses who have still not been detected. If the first symptoms phase started an average of 5 years before,2,3,9-12,22 the prodromic or pre-psychotic phase was present at least 1 year before.4,19,28 These patients still go undetected by all the studies, even, to a greater extent, by community and PHC studies.
As limitations of our study, our definition of a case has to be mentioned, perhaps excessively restricted: it may have given rise to false negatives on including strict time criteria. Despite this, we could say that our results are comparable to those of the majority of methodologically reliable studies, and thus provide supplementary support to our results.
In any case, repeat studies like ours are required: on carrying them out in extra-hospital MHUs with other health, population, or technical-scientific characteristics, perhaps they may provide different data. Likewise, this type of study would need to be extended to the international setting and, particularly, to urban environments. Also, it would be advisable to take advantage of these types of estimations based on PHC to investigate and define risk factors, accessible from this health care service: perhaps they could provide knowledge for the early detection and primary and secondary prevention of schizophrenia and the rest of the psychotic disorders, in the adult, as well as in children and adolescents. And we must not forget that these patients, as well as their families, are suffering, and are likely deteriorating more severely than almost any other contemporary health care clinical problem.
Acknowledgements
We are grateful for the assistance of Eva Cirera (Municipal Health Institute), Enriqueta Pujol (Catalonian Health Institute), and Marta Goma and Laia Català, grant holders of the SASPE Research Project.
What Is Known About the Subject
• It is usually said that schizophrenic disorders have a prevalence of around 1% in the general population and an annual incidence of 1-2 per 100 000 inhabitants.
• There is a significant variation between different studies. The prevalence data is being revised "downwards" and each particular psychotic disorder according to dispersion is still higher.
• However, in the health system clinics, these patients and their families are among the most suffering they support, as well being among those which take up a larger economic share of the social and health budgets.
What This Study Contributes
• The SASPE project tries to contribute a direct perspective of the incidence, prevalence and the characteristics of schizophrenia and other psychoses based on cases actually treated in PHC and in MHUs linked to PHC, and not only in hospitals or by population surveys.
• It confirms that the majority of psychotic patients are seen in PHC or in the PCH-MHU interface (the type of work that we have called "Primary Care to Mental Health").
• The data contributed by this type of study, the incidence and the prevalence, can be more useful and realistic for PHC than those coming from studies based in the hospital setting, in the sense that they correlate more directly with their clinical and health care needs.
This study has been supported by the grant for the SASPE 02E/99 project by the Seny Foundation, after an evaluation carried out by the Catalonian Evaluation of Research and Medical Technologies Agency.
Correspondence: Dr. J.L. Tizón.
Institut Català de la Salut.
Roger de Llùria, 130, 1.º, 3.ª. 08037 Barcelona. España.
E-mail: jtizong@meditex.es
Manuscript received November 30, 2005.
Manuscript accepted for publication April 5, 2006.
Spanish version available at www.doyma.es/145.497
A commentary follow this article(page 125)