Primary hyperparathyroidism is a disease characterised by the autonomous production of parathyroid hormone. The most common cause is an adenoma, followed by hyperplasia, and rarely carcinoma.
Clinical casesThree cases are presented. The first case is associated with a brown tumour that was diagnosed as hyperplasia after study and surgery. The second case was related to pathological fractures, and a lower right adenoma 236 times bigger than a normal parathyroid was excised. The last case presented with abdominal pain and heartburn. Histopathology reported a carcinoma, which was removed using surgery en bloc. All patients have improved.
ConclusionHyperparathyroidism symptoms are very difficult to identify and diagnose, thus a detailed and broad approach is needed when hyperparathyroidism is suspected.
El hiperparatiroidismo primario es una enfermedad caracterizada por la producción autónoma de hormona paratiroidea. La causa más común es un adenoma, seguido de hiperplasia y más raro por carcinoma.
Casos clínicosPresentamos 3 casos, el primero está asociado a un tumor pardo de paratiroides, que posterior al estudio y cirugía se determinó hiperplasia paratiroidea. El segundo caso, está relacionado con fracturas patológicas, se resecó un adenoma paratiroideo inferior derecho 236 veces el tamaño de una glándula normal. El último caso se presentó con dolor abdominal y pirosis, se realizó resección en bloque y patología determinó carcinoma de glándula paratiroides. Todos los pacientes presentaron mejoría.
ConclusionesLa sintomatología del hiperparatiroidismo representan un gran reto para su identificación y diagnóstico, por lo cual debemos hacer un abordaje integral del paciente y, muy importante también, una historia clínica detallada.
Hyperparathyroidism was first described in 1920 in the context of severe bone disease. Primary hyperparathyroidism is a disease that is characterised by autonomous parathyroid hormone production. The most common cause of the condition is adenoma (80%), followed by parathyroid hyperplasia (19%) and, much less frequently, parathyroid carcinoma (<1%).1–3
We present 3 cases in this article, where we found different causes of hyperparathyroidism.
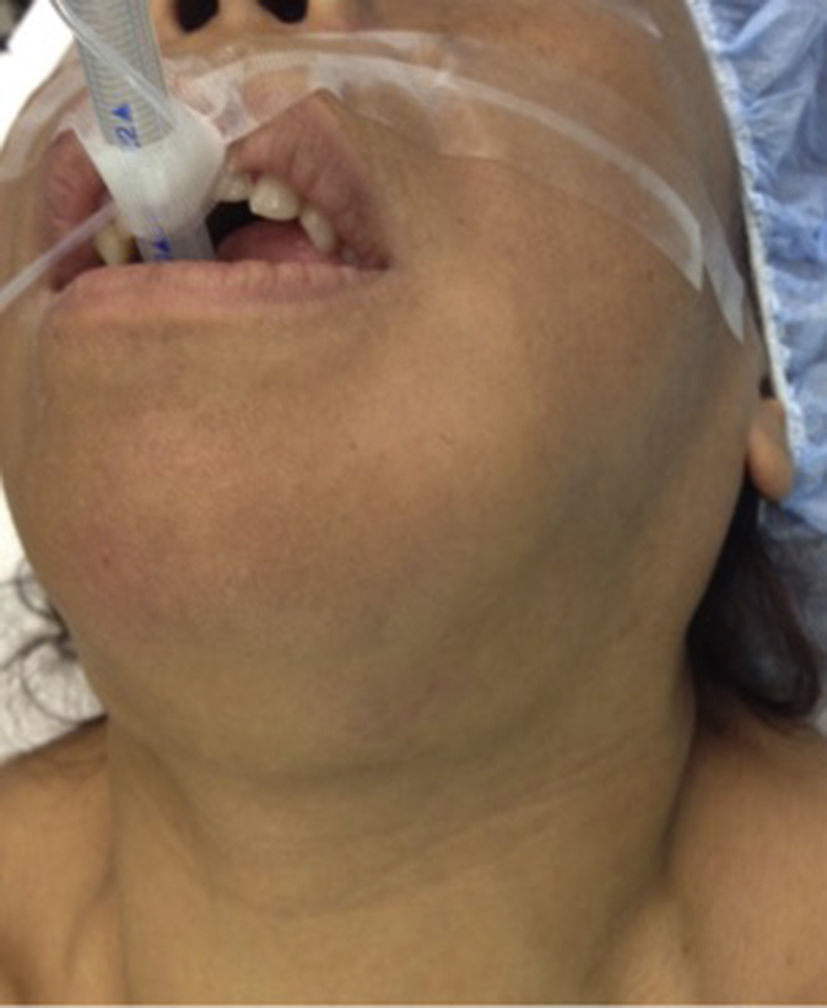
Case 1The first case was a 24-year-old woman, with a history of 2 years’ hair loss, bone growth, deformity and pain in the facial region and a history of renal failure, 9 years with a diagnosis of uncertain aetiology (Fig. 1). Levels of parathyroid hormone 1789.4pg/ml, calcium 9.9mg/dl and phosphorus of 4.6mg/dl were established during the study protocol. A parathyroid scintigraphy was undertaken, from which a possible right inferior adenoma was concluded. The patient was taken for surgery with levels of parathyroid hormone of 1954pg/ml, calcium 8.8mg/dl and phosphorus 4.5mg/dl. During the operation we decided to resect the 4 glands due to their macroscopic appearance and size. Post-resection measurement of parathyroid hormone was 837mg/dl. The pathology department reported parathyroid glands of 1–1.5g, with a diagnosis of parathyroid hyperplasia. The patient has been symptom-free for a year, her renal failure improved and regression in bone growth has been reported.
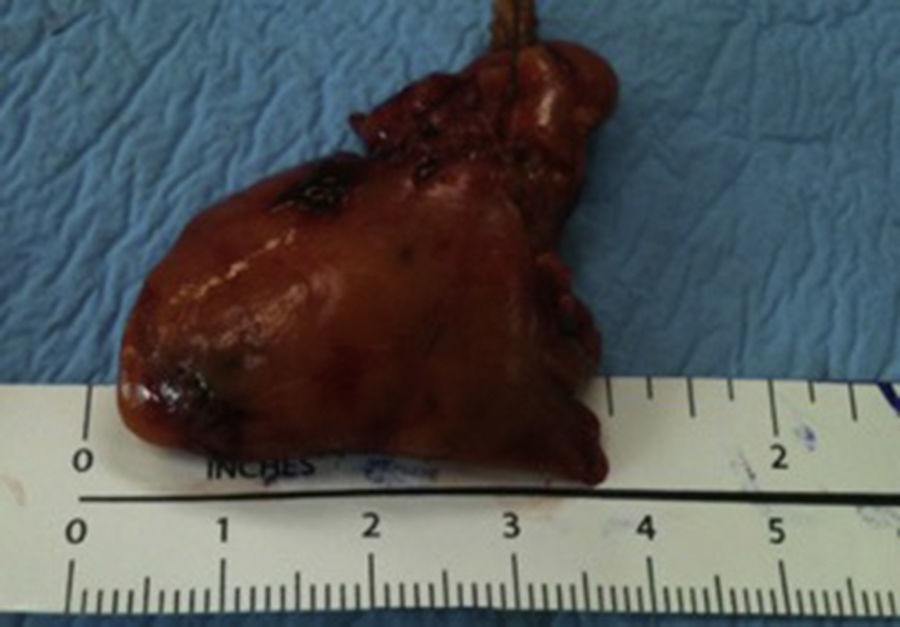
Case 2The second case is a 73-year-old woman with a history of pathological fractures over the 6 previous months, including the femur, clavicle and ribs. The study protocol was started, which found levels of parathyroid hormone 1400pg/ml and calcium 13.3mg/dl. Scintigraphy revealed a probable right inferior adenoma. The patient underwent surgery and we found a parathyroid gland of 4cm and 7.1g (Fig. 2) after resection, parathyroid hormone levels lowered to 274pg/ml, and normalised one day later (27.4pg/ml), with calcium 10.5mg/dl. The pathology report revealed a parathyroid adenoma 236 times the gland's normal size. The patient has been asymptomatic for 4 months.
Case 3The final case is a 46-year-old male with a 6-month history of abdominal pain and pyrosis, referred to us because, in the approach for the abdominal pain, levels of calcium were found of 12.9mg/dl and of parathyroid hormone of 1205pg/ml. Scintigraphy showed an image suggestive of right inferior adenoma. During the surgical procedure, we resected the right inferior parathyroid gland of 2.2g, with post resection parathyroid hormone level of 147pg/ml. One week later the pathology department reported parathyroid carcinoma with capsular and vascular invasion. Therefore we decided to reoperate the patient, to complete an en bloc resection with ipsilateral hemithyroidectomy and central compartment lymph node dissection. The patient has been asymptomatic for one month.
DiscussionPrimary hyperparathyroidism is the presence of hypercalcaemia with elevated or inappropriately normal parathyroid hormone levels.1,3 It has an incidence of 1% of the population and is more common in females.1 It is usually caused by a benign tumour of the parathyroid gland, termed adenoma (85%), or multiglandular hyperplasia (10–15%).1
Completely asymptomatic hyperparathyroidism is rare. The clinical manifestations can be skeletal (bone pain, fractures and abnormal growth), renal (nephrolithiasis and renal lesions) neuromuscular, cardiovascular and digestive.1,4 It is more common for these patients to have hypercalcaemia, than parathyroid hormone alterations.5
Bone manifestations generally present late in the progress of hyperparathyroidism and fractures of the long bone, clavicle, ribs and pelvis are common.
Brown tumour is a bone lesion that occurs in patients with primary or secondary hyperparathyroidism, and is a component of metabolic bone disease called “generalised osteitis fibrosis cystica”.6 It is more common in primary hyperparathyroidism (3%) and usually presents as a lytic lesion, well defined on X-ray, with important enhancement on scintigraphy.5 The most common sites are the clavicles, ribs, pelvis, femur and, less commonly, the facial bones; surgical treatment is indicated for symptomatic, large and deforming lesions.6,7 Our case had regression of their bone deformity with after parathyroid resection.
The gastrointestinal manifestations of hyperparathyroidism range from constipation (33%), pyrosis (24%), nausea (24%), loss of appetite (15%) and vague abdominal pain, which can occur in up to 29% of cases.4 The measurement of serum calcium levels should be considered in approaching patients with vague or non-specific abdominal pain.
Parathyroid carcinoma is a rare cancer, and is also a rare cause of primary hyperparathyroidism with an incidence of 0.005% of all cancers, with equal frequency in males and females.2 It is difficult to diagnose the malignancy of these tumours preoperatively, therefore, in the absence of obvious metastasis, diagnosis is made from the histopathological study.2
The best therapeutic option is complete resection of the tumour, since these tumours do not respond to radiotherapy. The appropriate surgical procedure includes ipsilateral hemithyroidectomy with thyroid isthmusectomy, and central compartment dissection.
ConclusionsHyperparathyroidism symptoms pose a great challenge clinically; the gastrointestinal symptoms are generally overlooked. Therefore serum calcium levels should be measured as part of the routine studies for patients with abdominal pain. Similarly, it is very important to undertake a detailed and complete preoperative study to determine the location of the diseased gland in order to offer the patient the best treatment.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of interestThe authors have no conflict of interests to declare.
Please cite this article as: Stoopen-Margain E, Valanci-Aroesty S, Castañeda-Martínez L, Baquera-Heredia J, Sainz-Hernández JC. Enfermedad paratiroidea: el espectro completo, de adenoma a carcinoma. Reporte de 3 casos. Cir Cir. 2017;85:549–551.