Flood syndrome, caused by spontaneous rupture of an umbilical hernia, is a rare but potentially fatal complication that occurs in patients with advanced liver disease and long-term refractory ascites, in whom the prevalence of umbilical hernias can be greater than 20%.1–3 The treatment of choice is conservative given the high perioperative risk and the high rate of surgical complications.3
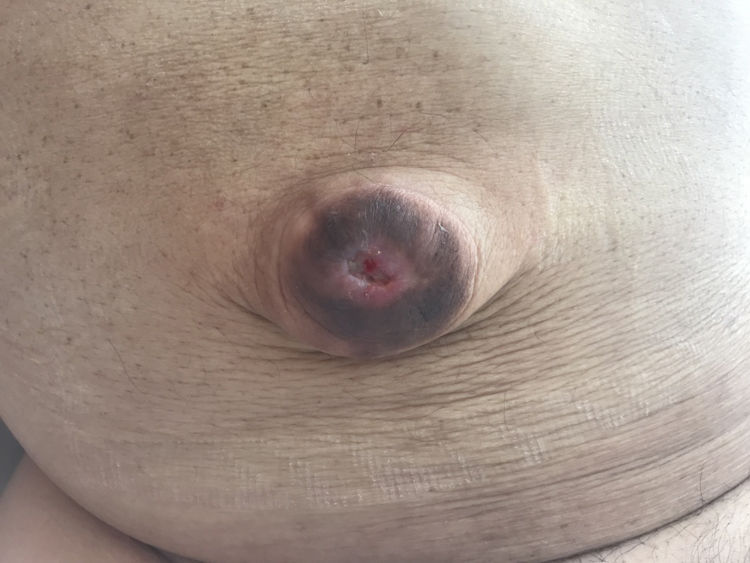
We present the case of a 61-year-old man with Child-Pugh stage C alcoholic liver cirrhosis, portal hypertension, esophageal varices, and refractory ascites requiring weekly paracentesis. The patient was not a candidate for a surgical or percutaneous portosystemic shunt (TIPS) due to high surgical and anesthetic risk, and liver transplantation was ruled out due to lack of alcohol abstinence. He came to the emergency room with spontaneous leakage of abundant fluid through the previously identified umbilical hernia. Upon examination, he presented signs of encephalopathy, abdominal ascites, no signs of peritoneal irritation, and an umbilical hernia with a skin ulcer measuring 3 cm in diameter that discharged abundant ascitic fluid (Fig. 1).
The patient was admitted, and conservative medical treatment was initiated with crystalloids, albumin, and empirical therapy with broad-spectrum antibiotics. Likewise, daily umbilical wound cleaning was prescribed, and a pigtail 8 Fr percutaneous abdominal drain was inserted to evacuate the ascitic fluid, thereby achieving complete closure of the umbilical-cutaneous fistula in 3 weeks. The patient was discharged without a drain system and remains asymptomatic in terms of the umbilical hernia after 6 months of follow-up.
Flood syndrome was first described in 1901 by Johnson, although the name is due to Frank B. Flood, who published the first case series in 1961.4,5 It is an uncommon complication that occurs in patients with advanced liver disease and ascites, with a high mortality rate of 30–50%.2,6 Its incidence is higher in patients with alcoholic liver cirrhosis, although cases have been reported of patients with ascites due to other etiologies, pregnant women and children with congenital umbilical hernia.2 The main causes that cause rupture are: increased intra-abdominal pressure associated with ascites, weakness of abdominal wall muscles due to poor nutritional status, and supraumbilical fascial defect due to possible recanalization of the umbilical vein.4 Paracentesis with removal of large volumes of fluid may increase the risk of developing hernias due to changes in intra-abdominal pressure during the procedure.6
In most cases (80%), the development of skin ulcers or necrosis precedes the rupture of the umbilical hernia and should be considered a sign of alarm.3,5 Complications of umbilical hernia rupture include: evisceration of the small intestine with possible incarceration, hypotension secondary to spontaneous large-volume paracentesis and the development of cellulitis, peritonitis and sepsis.2,3
There is much debate in the literature regarding the management of this type of hernias, and the only available evidence comes from case series.4 In selected cirrhotic patients with correctly controlled ascites and uncomplicated hernias, there is a tendency to perform scheduled surgery (aided or not by portosystemic shunt systems).6 However, the management of hernia rupture remains controversial, with reported morbidity rates of up to 71% and high mortality rates from 20% to 60%, depending on the series.4 For all these reasons, conservative treatment is of choice until the liver disease is compensated.5,7
Initial treatment consists of correct patient monitoring and stabilization, as well as the prevention of possible infectious complications through broad-spectrum antibiotic therapy.2,7 The wound should be covered with a sterile occlusive bandage. Adequate electrolyte replacement and albumin infusion may be necessary to compensate for the losses caused by ascites. Afterwards, in those patients with refractory ascites, fluid drainage is indicated to reduce wound discharge, with secondary intention closure of the defect, subsequently assessing the indication for delayed repair of the umbilical hernia.2,7
In short, the treatment of choice in Flood syndrome is conservative using temporary peritoneal diversion, volume and albumin replacement, and local wound treatment, which achieves secondary intention healing of the skin opening in most cases. Surgical treatment is indicated in the event of failure of medical treatment, although it entails high morbidity and mortality rates.
Please cite this article as: Blanco Terés L, Valdés de Anca Á, Correa Bonito A, Gancedo Quintana Á, Martín Pérez E. Síndrome de Flood: una grave complicación de la hernia umbilical. Cir Esp. 2020;98:490–491.