The use of botulinum toxin type A (BTX-A) together with preoperative progressive pneumoperitoneum (PPP) facilitates surgical repair of ‘loss of domain’ (LOD) hernias, while also reducing perioperative morbidity, mortality, and the recurrence rate in the medium and long term. These techniques have a low complication rate, but they are not without risks. We present the case of a patient with an LOD hernia who presented iatrogenic pneumothorax secondary to PPP.
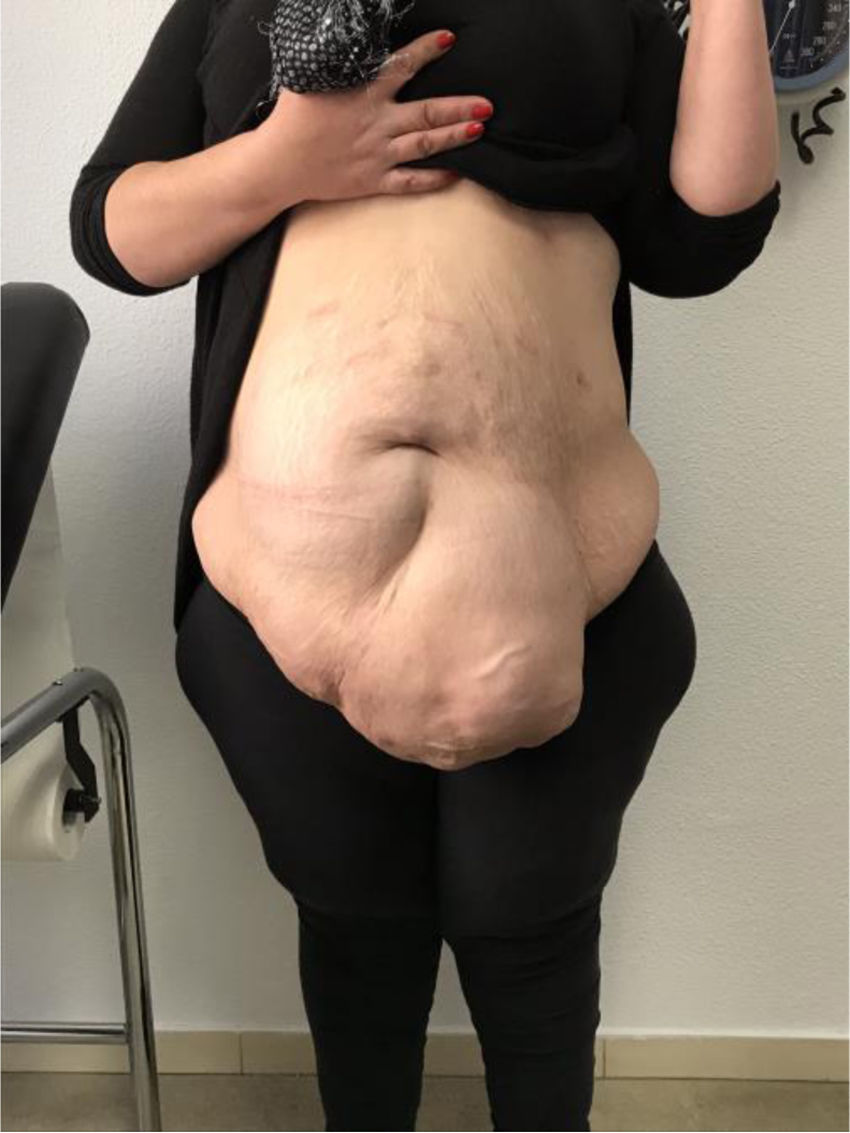
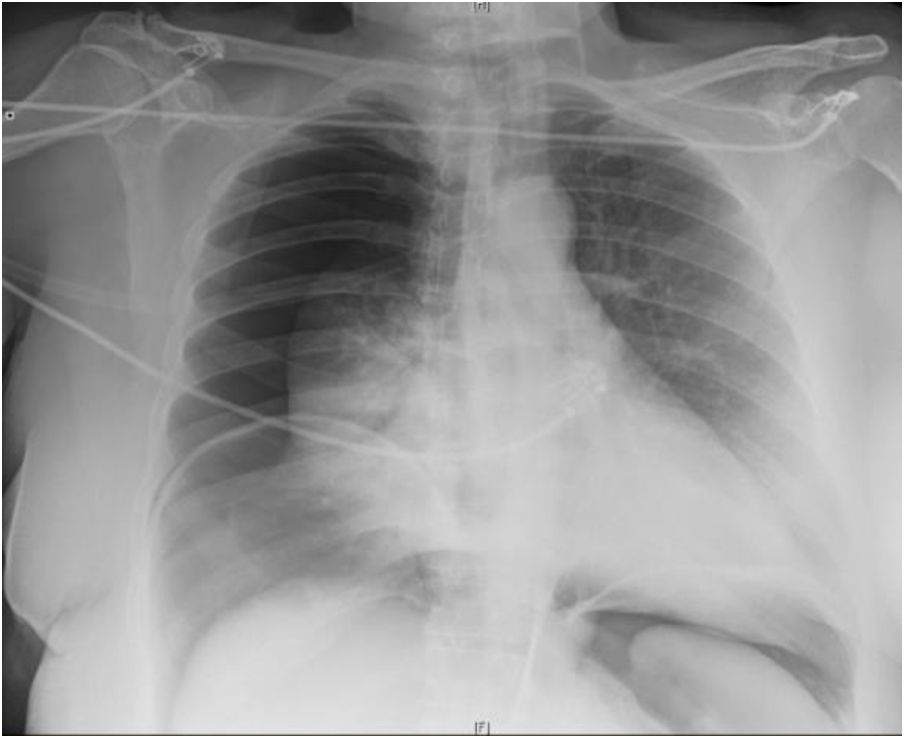
The patient is a 52-year-old woman who was hypertensive and morbidly obese (BMI: 41) after bariatric surgery and weight gain. She presented midline incisional hernia secondary to a previous cesarean section (M4M5 W3) (Fig. 1) with a Tanaka index of 45%, which had significantly affected her quality of life. Surgery was scheduled for surgical repair of the incisional hernia and dermolipectomy, preceded by preparation of the patient with BTX-A and PPP. Guided by ultrasound, 300 IU of BTX-A were administered to the lateral abdominal muscles (150 IU on each side) 5 weeks prior to surgery. PPP was performed through an 8 Fr pigtail catheter that had been placed under radiological guidance in the left hypochondrium (Palmer’s point), administering a volume of 1000–1500 cc of room air every 48 h on an outpatient basis for a total of 5 sessions, which the patient tolerated well. After the last session, the patient came to the emergency room with pleuritic pain in the right hemithorax, which increased with respiratory movements. In addition, she reported pain in the right shoulder and dyspnea. The patient was diagnosed with complete right pneumothorax (Fig. 2), and pleural drainage resulted in complete re-expansion. When the absence of air leakage was confirmed 24 h after chest tube placement, the patient was discharged from the hospital with a pleural drain connected to a portable device. The administration of PPP was continued, with 2 new sessions, until the day of surgery (total PPP volume: 10 000 cc), and no new leakage was observed through the thoracic drain. PPP was suspended 5 days prior to surgery. Surgery consisted of Rives-Stoppa incisional hernia repair and dermolipectomy. The endothoracic drain tube was removed on the 1st postoperative day, and the patient was discharged 72 h after surgery. There were no notable postoperative complications. One year after the procedure, the patient is asymptomatic and has had no evidence of recurrence.
The repair of abdominal wall hernias with loss of domain is an important surgical challenge due to the complexity of the surgical technique as well as the associated morbidity and mortality. The most serious complications are compartment syndrome and acute respiratory failure. There is no universally accepted definition of a loss of domain hernia1. Generally, this concept encompasses abdominal wall hernias in which the volume of the herniated abdominal content is of such a magnitude that its reinsertion without the use of specialized techniques would cause abdominal compartment syndrome. Tanaka et al. and Sabbagh et al. developed 2 methods to define this concept objectively and to guide the need for preoperative techniques. Both techniques are based on volumetric measurements of the abdominal cavity and the hernia sac using computed tomography (CT) images2,3. At our hospital, we use PPP together with BTX-A when the Tanaka index is greater than 25%.
BTX-A4,5 and PPP6 are 2 techniques used to prepare the abdominal cavity preoperatively in order to reduce perioperative morbidity and mortality. BTX-A is used to achieve reversible relaxation of the abdominal flat muscles for tension-free closure of the abdominal wall. Meanwhile, pneumoperitoneum is created to increase the volume of the abdominal cavity (thereby improving lung functionality) as well as to promote adhesiolysis, which facilitates the surgical technique5,7,8.
The use of PPP has a low rate of complications, although there have been reports of intra-abdominal infection, infection of the intra-abdominal drain site, subcutaneous emphysema, decompensation of underlying pulmonary diseases, or seroma6.
In our case, the pneumothorax that the patient developed was probably caused by the insufflation of a large volume of air over a short period of time that was greater than the patient’s abdominal cavity was able to accommodate. Mouguin describes pneumothorax as a possible complication after PPP9. There are no clear recommendations or studies on the frequency or volume of insufflation. Although some authors recommend measuring the intra-abdominal pressure to determine the insufflation volume (with the aim of not exceeding 12–15 mmHg), other authors recommend basing this decision on the patient’s own tolerance, as in our case10. It is important to closely monitor patients during PPP treatment, while also maintaining a high degree of suspicion in order to quickly identify and treat complications that may arise10.
Despite the serious complication that our patient presented, this did not prevent us from continuing with the preoperative plan, and the operation was able to be completed with excellent results.
PPP is a very useful technique for the preoperative preparation of patients with giant abdominal wall hernias. It is a safe technique, but it is not without complications. It is important to closely monitor patients and maintain a high degree of suspicion for early diagnosis and treatment. In most patients, the development of complications does not prevent the surgery from being completed successfully.
Please cite this article as: de la Fuente Añó A, Valdés de Anca Á, Milián Goicoechea H, Rofso Raboso P, Blanco Terés L. Neumotórax iatrogénico tras neumoperitoneo progresivo preoperatorio. Cir Esp. 2021;99:694–696.