The case relates to a 70-year-old woman from Pakistan, resident in Spain for 12 years, with a history of essential arterial hypertension and type 2 diabetes mellitus with regular metabolic control.
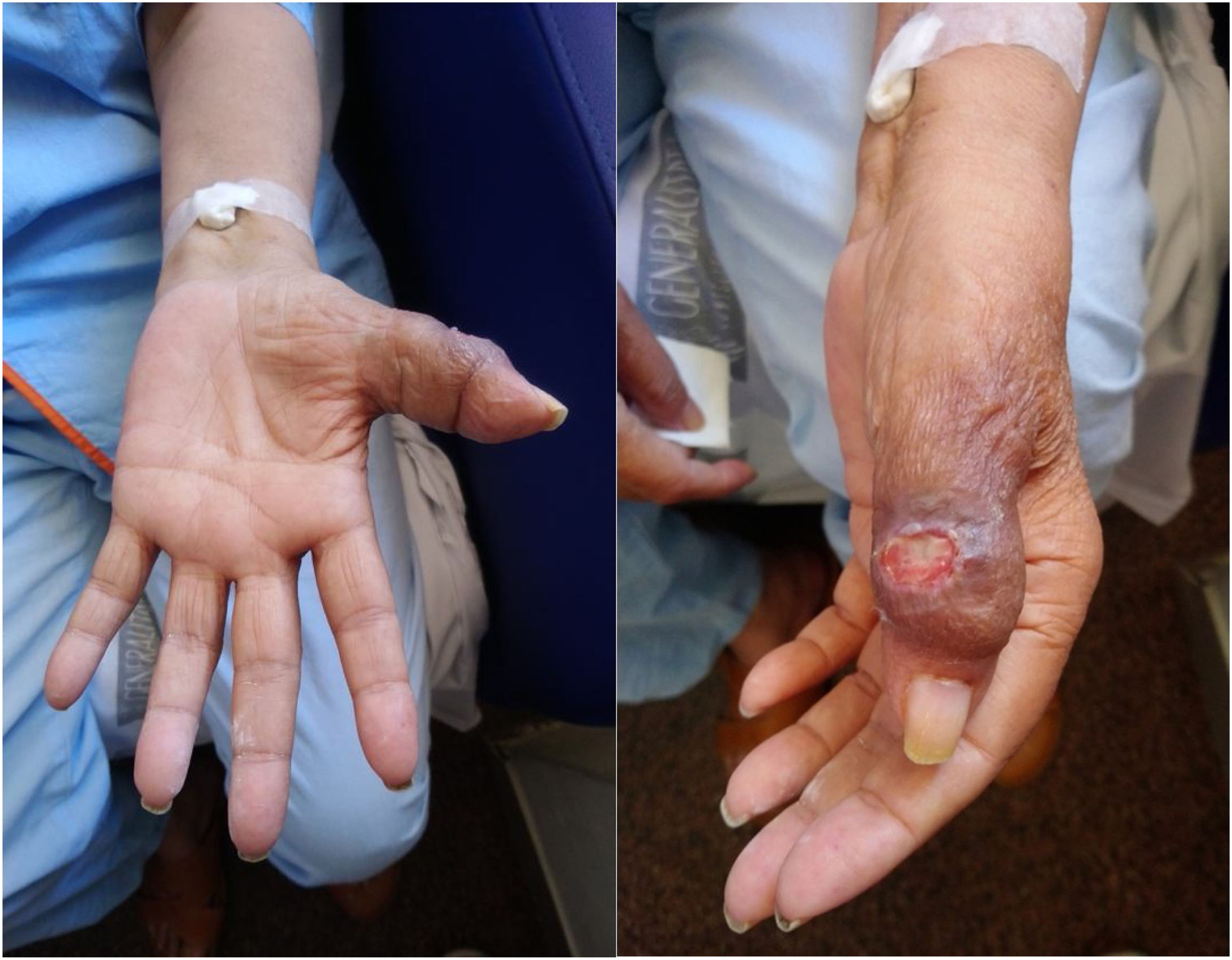
She went to the emergency department for dyspnoea on minimal exertion, where a massive left pleural effusion was observed after performing a chest X-ray. In addition, the patient presented marked swelling of the thumb of her left hand with skin ulceration (Fig. 1), which had prompted her to attend this same emergency department on two occasions five months previously, being treated with different antibiotic regimens without result.
During admission, a chest computed tomography (CT) scan was performed, which revealed bilateral pleural effusion, more predominant in the left hemithorax, subpleural nodules and adenopathies in the left mammary chain, with no lesions found in the lung parenchyma. The biochemical analysis of the pleural fluid revealed a lymphocytic exudate. However, the conventional and mycobacteria cultures were negative.
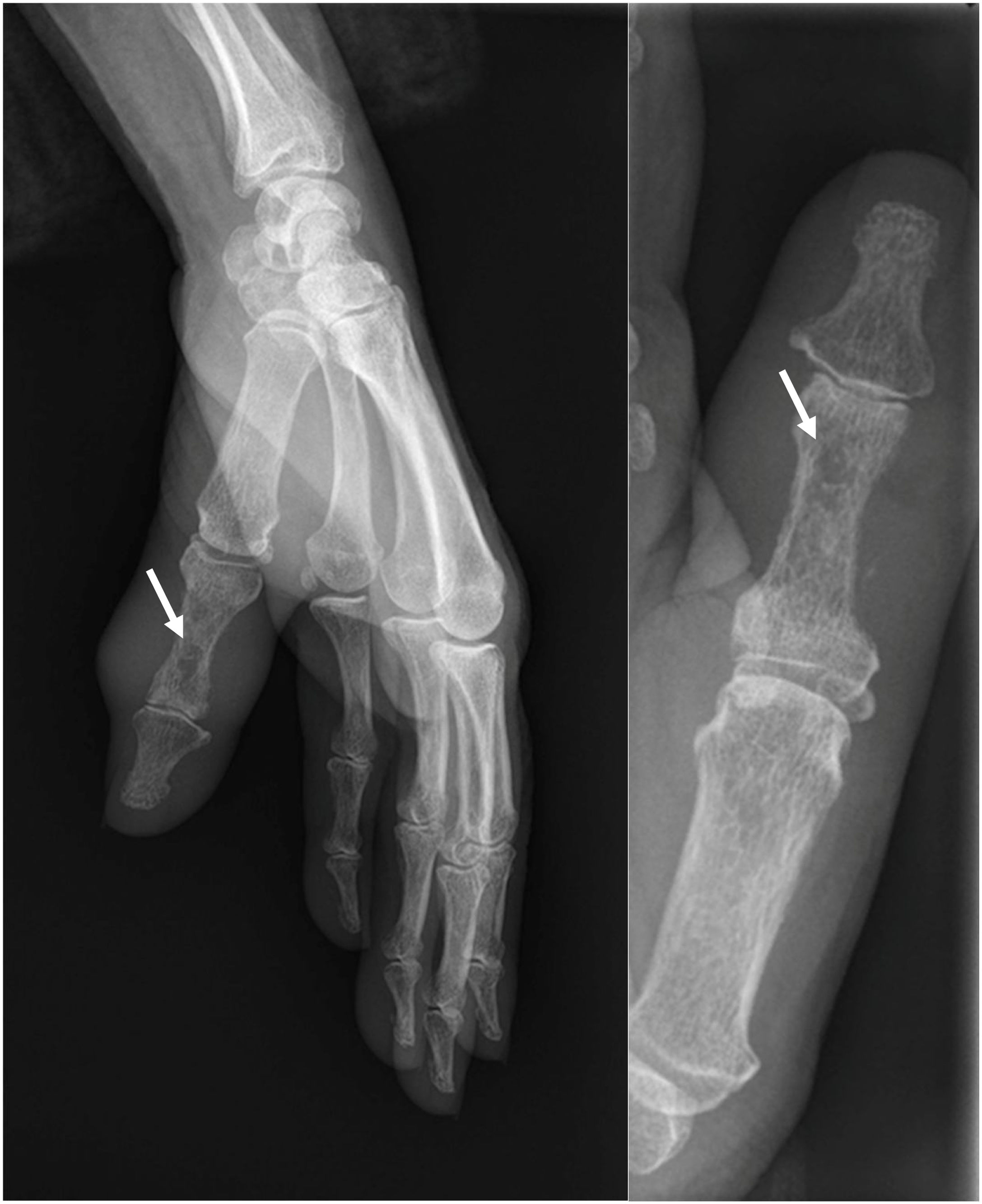
The hand X-rays taken in the emergency department five months earlier were reviewed and a central hypodensity was evidenced on the diaphysis of the proximal phalanx of the thumb of her left hand (Fig. 2). The nuclear magnetic resonance (NMR) showed osteomyelitis in the proximal phalanx of her thumb with a soft tissue mass.
An abdominal and pelvic CT was requested to rule out neoplastic origin of the pleural effusion, which revealed spondylodiscitis at the level of T12-L1 associated with an abscess in the left psoas, suggestive of Pott’s disease.
Clinical courseFollowing the results of the different complementary tests, disseminated tuberculosis was established as the first diagnostic suspicion. Both the Mantoux and QuantiFERON-TB tests were positive. Finally, the decision was taken to take a pleural sample by thoracoscopy and the histological study confirmed suspicion of caseating granulomatous pleuritis in the anatomical pathology. However, it was the study using a molecular biology technique of the purulent material obtained from the skin ulcer after an open biopsy that allowed us to identify the Mycobacterium tuberculosis DNA and thus confirm our diagnostic suspicion of extrapulmonary tuberculosis. No resistances were detected.
Treatment with isoniazid, rifampin, pyrazinamide and ethambutol was initiated, and a few days later the patient presented gastrointestinal intolerance and liver toxicity with elevated transaminases and cholestatic enzymes. The anti-tuberculous treatment was suspended until liver biochemistry normalised and the same drugs were reintroduced sequentially, the last one being rifampin due to the suspicion that it was responsible for the liver toxicity. Following this, the treatment was well tolerated. The scheduled total duration of treatment is 12 months.
Closing remarksTuberculous dactylitis is an uncommon form of bone tuberculosis1. Given that extrapulmonary tuberculosis does not have such a significant epidemiological impact as the pulmonary forms, especially in countries with a low prevalence of infection, diagnostic delay is common. In fact, in our patient, despite debuting with extrapulmonary tuberculosis in the form of dactylitis, it was not recognised until the appearance of pleural effusion five months later.
The time elapsing from the patient’s arrival in Spain to diagnosis is also striking. The greatest risk of reactivation of tuberculosis in immigrants is known to occur in the first two to five years after arrival in the country of destination. However, in our case, the diagnosis was made 12 years later, which would be consistent with new published data that support the hypothesis that the risk of reactivation could remain high for more than 10 years after arrival2.
Tuberculous dactylitis is an entity with an insidious clinical course. Swelling without major cutaneous inflammatory signs, low-intensity pain and functional impotence are usually the most common presentation symptoms3–5. Occasionally, over time, the bone lesion can fistulise to the skin and produce a skin ulcer, as in our case, which can facilitate bacterial superinfection3.
Although clinical and imaging tests help us to establish the suspected diagnosis, they do not provide pathognomonic data, so a histological and microbiological study by means of culture and/or PCR is required to obtain the definitive diagnosis1,4.
Regarding treatment, prolonged regimens are recommended: the first two months with four drugs (isoniazid, rifampin, pyrazinamide and ethambutol), followed by 6–10 months with dual therapy with isoniazid and rifampicin6,7. According to case series, a complete remission of the lesion is achieved in most cases1,4,5. However, complications include joint ankylosis and bone fracture, especially in advanced lesions, as in our case.
Liver toxicity due to anti-tuberculous drugs, whose incidence reported in the literature fluctuates between 4% and 19%8, and is an adverse effect that often hinders therapeutic management of the infection. Three of the four classic drugs used in the treatment of tuberculosis (isoniazid, rifampin and pyrazinamide) are potentially hepatotoxic, making it difficult to identify the responsible agent, considering that combination boosts the toxicity phenomenon. This can limit optimal treatment of the disease and favour therapeutic failure and/or the appearance of resistance. Therefore, following the withdrawal of drugs in the event of liver toxicity (bilirubin ≥3 mg/dl, transaminase levels five times higher than the upper limit of normal in asymptomatic patients or three times higher in symptomatic patients), and the subsequent normalisation of liver biochemistry, it is important to reintroduce treatment, although there is no consensus as to how this should be done. The most prudent approach would seem to be progressive withdrawal, restarting the drugs one by one. Rifampicin is known to usually produce a more cholestatic pattern in laboratory tests than hepatic cytolysis, hence it is advisable to restart it last in this situation, as in our case; whereas, if we are faced with an elevation predominantly in transaminases, isoniazid and pyrazinamide should be introduced last, since they are probably responsible for the liver toxicity9.
In conclusion, tuberculosis with atypical presentation should be incorporated into our clinical reasoning, especially in the immigrant population from areas with a high prevalence of the disease.