We read with great interest the recent article by Martinez-Lapiscina et al., “Epileptic seizures and lipoma of the corpus callosum: cause or finding”.1 As the authors demonstrate, “intracranial lipomas can cause epileptic seizures and their correct diagnosis has prognostic and therapeutic implications”.
Some years ago we published a case of lipoma of the corpus callosum in a 42-year-old male who died suddenly due to food aspiration as a result of an epileptic seizure while he was dining. A neuropathological study revealed two curvilinear lipomas located at the top of the genu of the corpus callosum (2.5cm×0.7cm and 1.5cm×0.5cm, respectively). These consisted of mature adipose tissue and were very well vascularised. They were not associated with developmental abnormalities of the corpus callosum.2
It is noteworthy that our patient had presented two previous seizures at 28 and 40 years of age, so he had undergone EEG, CT and MRI scans; these showed “brain fat”, as reported by the family (we did not have access to medical records). The patient was not following anticonvulsant therapy, since no clinical indication was considered. This fact was confirmed by a negative result in the chemical–toxicological analysis performed.
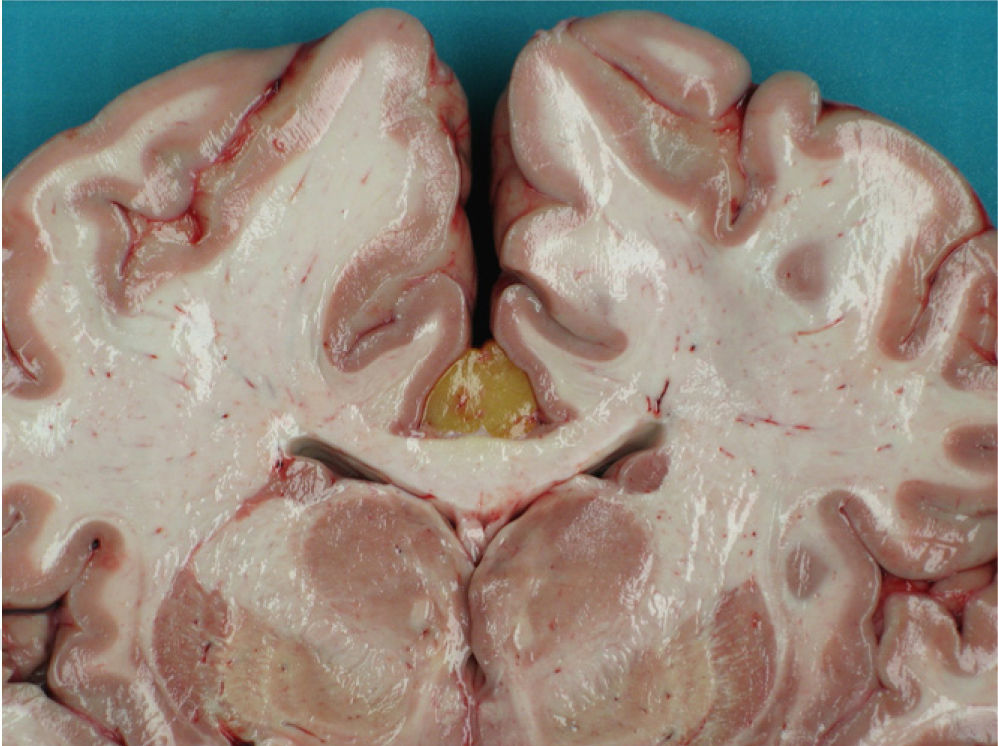
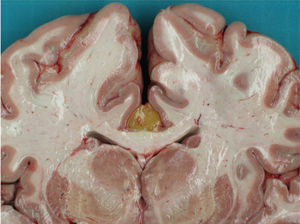
Recently, we had another case of lipoma of the corpus callosum as an incidental finding during the autopsy of a 41-year-old woman who died suddenly due to digestive pathology. It was a tubulonodular lipoma measuring 2cm×4cm, of interhemispheric location, situated in the anterior corpus callosum. It was not associated to any dysgenesis or other neuronal migration abnormalities (Fig. 1). Although the patient had not presented epileptic seizures, she had a history of headache and mild psychomotor retardation. The facies was somewhat coarse, with frontal prominence and low-set ears, suggesting a defect in the development of the midline, as other authors have mentioned.3–5 Intracranial lipomas are rare congenital malformations, representing only 0.03–0.08% of all intracranial masses.2,3 In the past 6–1/2 years, we have performed a total of 6011 legal autopsies at our department and found only 2 exposed cases of lipomas of the corpus callosum (an incidence of 0.03%).
We completely agree with the view expressed by the authors when they mention that intracranial lipomas can cause epileptic seizures, so a higher prevalence of lipomas should be considered in the epileptic population. On the other hand, anticonvulsant therapy may be necessary in these cases, especially in symptomatic patients.
Finally, we consider that, in addition to diagnosing the cause of death, a forensic pathologist is required to explain the pathophysiological mechanisms of the disease, as well as any possible aetiologies and risk factors involved. This is the philosophy that we attempt to apply during our daily work.
Please cite this article as: Lucena Romero JS, et al. Comentarios a la carta del editor publicada por Martínez-Lapiscina et al: «Crisis epiléptica y lipoma del cuerpo calloso: causa o hallazgo». Neurología. 2011;27:57–8.