Osteoarthritis (OA) is a common disease affecting synovial joints. The main structure involved in the disorder is the articular cartilage, where softening and disintegration appear. Moreover, reactive phenomena such as vascular congestion and osteoblastic activity in the subarticular bone, new growth of bone (osteophytes) at the joint margins and capsular fibrosis are present1.
But if it is true that articular cartilage is the structure primarily involved, in many cases there are intermittent episodes of mild to moderate synovitis, with the possible presence of joint effusion. These changes are responsible for swelling and may contribute to the symptoms of the disease1.
According to what most authors assert1,2, mild synovitis is a feature of OA and changes in all the soft tissues of the joint appear during the course of the disease.
Table 1 shows the articular structures involved by OA.
During recent years sonography has become a reference diagnostic method in the examination of soft tissues. In particular, it has been successfully applied to the study of musculo-skeletal pathology, and recently its importance has also been widely appreciated in the evaluation of rheumatic diseases.
In fact thanks to its technical characteristics of noninvasiveness, low cost, and easy repeatability, sonography is actually considered one of the best imaging techniques for the evaluation and follow up of changes of articular soft tissues in rheumatic diseases3,4. Referring to OA, sonographic study of the osteoarthritic joint provides useful information about the status of articular cartilage, synovial membrane, synovial fluid, joint capsule, joint margins, bone surface and bursae.
In particular, articular cartilage can be studied at different joints such as the knee, the hip, the shoulder, the elbow, the first carpometacarpal joint, and the metacarpophalang eal joints. Of course, not all the different sites are studied with the same accuracy, the extent of information depending on the size of the acoustic windows5. In normal joints articular cartilage appears as an anechoic band with sharp edges lining the anterior surface of the bone. This sonographic pattern is due to the high water content (almost 85%) of the cartilage. When the degenerative processes appear, a part of the water is lost and scattered echoes appear within the band. For this reason it is possible to assert that sonography reveals the early signs of OA, when the disease is still asymptomatic and before the appearance of other alterations. During the course of the disorder irregularities of the interfaces also appear, and they can be detected by sonography. Another typical change of OA is the thinning of the cartilage, the extent of which can be carefully examined by sonography that is able to measure the exact thickness of the cartilage.
During the course of the intermittent episodes of mild to moderate synovitis, with the possible presence of joint effusion, sonography shows the hypertrophic synovial membrane and reveals the increased quantity of synovial fluid thereby detecting the amount of effusion.
Moreover, the irregularities of the bone surface and joint margins due to the presence of osteophytes are shown, as well as the frequent subluxation of some joints that may appear in OA.
The possible thickening of the joint capsule is also revealed.
Fluid collection within of the bursae are also well evaluated by sonography.
As some joints (such as the elbow, the ankle or the gleno-humeral joint) are uncommonly involved in OA, the present review will fundamentally examine the most frequently involved sites, even though we have to consider that similar changes may also be found in the more rarely involved joints.
The knee
The osteoarthritic knee is studied very carefully with sonography. In fact, this diagnostic imaging method makes it possible to evaluate most of the structures involved in the disease, carefully revealing the possible changes produced (table 2).
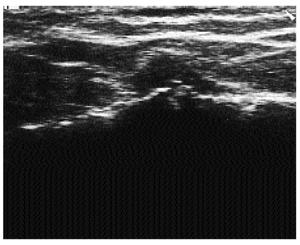
Articular cartilage of the femur is clearly depicted by sonography. Keeping the knee in full flexion it is possible to expose significant portions of the weight-bearing surface, that is the cartilage area that is more often affected by OA6. In a normal joint a sonolucent image with sharp margins is seen, lining the anterior surface of the condyles. Two interfaces are present (an anterior-synovial space-cartilage interface and a posterior-cartilage-bone interface). Its thickness is between 2 and 3 mm and it is usually greater at the center of the intercondylar notch than on lateral and medial condyles. Due to the loss of a part of the water, in the early phases of OA scattered echoes appear within the band (fig. 1) and the cartilage becomes hypoechoic. Later, blurring and irregularity of the sharp edges appear (fig. 1), with loss of the normal sharpness of the anterior-synovial space-cartilage interface and increased intensity of the posterior-bone-cartilage interface5. Finally, narrowing of the anechoic band is detected (fig. 2). As the exact thickness can be measured at different points it is possible to precisely detect the entity of the cartilaginous damage6.
Figure 1.Sonography of femoral articular cartilage of the knee. Scattered echoes, blurring and irregularities of the sharp edges.
Figure 2.Sonography of femoral articular cartilage of the knee. Narrowing of the band.
The synovial membrane is carefully studied by sonography. In fact, it is possible to measure its thickness and show the presence of villi and septa. In this way the episodic synovitis that may appear in OA is easily detected and useful information is obtained for disease and therapy monitoring.
The thickness of the synovial membrane is usually measured in the suprapatellar bursa, close to the patellar shadow7. This method assures the repeatability of the technique so that both the disease and therapy monitoring is possible. The synovial membrane appears as a homogeneous strip that lines the anterior bone surface of the femur and posterior surface of the quadriceps muscle. In a normal knee its thickness is between 2 and 3 mm. In an osteoarthritic joint the synovial membrane is usually thickened when synovitis is present (fig. 3).
Figure 3.Sonography of the knee. Thickening of the synovial membrane with presence of a villum and joint effusion.
In the lateral and medial recesses it also possible to examine the synovial membrane and to reveal the presence of villi and septa (fig. 3). In fact, these formations are usually present in the lateral and medial recesses, even though they can be found in any part of the joint cavity. They are usually a characteristic finding of rheumatoid arthritis and of some other inflammatory rheumatic diseases in which the proliferating synovial membrane has an invasive and destructive behavior. Nevertheless, they can also occasionally be found in OA, when episodic synovitis appears during the course of the disease.
Synovial fluid is very well evaluated, with anterior, lateral, medial and posterior scans. In fact, sonography may detect the quantity of this fluid, revealing the presence of joint effusion with very high sensitivity8. The physiological amount of synovial fluid in a normal knee is between 2 and 3 ml. Hydrarthrosis is demonstrated by the evidence of anechoic or hypoechoic collection within the joint cavity (fig. 3).
Sonography also provides generic information about the content of synovial fluid. In fact, when it is recent and in acute inflammation it usually appears anechoic. To the contrary when it contains manys cells, debris, fibrin masses scattered echoes appear and the fluid becomes hypoechoic.
With lateral and medial longitudinal scans it is possible to evaluate the regularity of the bone surfaces of the femur and the tibia. Osteophytes are easily detected, their presence being demonstrated by the finding of irregularity at the joint margins (fig. 4).
Figure 4.Sonographic demonstration of osteophytes over the medial aspect of the knee joint.
Another frequent alteration in OA is capsular fibrosis1. Sonography shows the thickening of the capsule, especially in posterior scans.
Evaluation of the calf may show the presence of Baker's cysts. They are frequently found in OA, especially when effusion is present and the gastrocnemius-semimembranosus bursa communicates with the joint cavity. Sonography gives useful information about their anatomic position, their dimension, their content, and their possible communication with the knee joint.
Performing multiple scans all around the knee joint it is also possible to examine the periarticular soft tissues and evalute the possible presence of anserine or pre-patellar bursitis, tendinitis of quadricipital or patellar tendons or alterations of collateral ligaments.
The wrist and the hand
OA of the wrist and the hand is quite frequent especially in females and it usually involves the carpometacarpal joint of the thumb and the interphalangeal joints2.
The first carpometacarpal joint is a saddle-shaped articulation between the trapezium and the base of the first-metacarpal bone. It has its own, very relaxed synovial membrane and a large capsule which allows great articular mobility1.
The recent implementation of high frequency transducers has allowed the use of ultrasound techniques even for the evaluation of this joint9, giving the possibility to study most of the anatomic structures involved in OA.
The first carpometacarpal joint is examined with anterior, lateral and posterior longitudinal scans, with the wrist kept in a neutral position. The surfaces of the trapezium and the base of the first metacarpal bone appear as two hyperechoic strips. The capsule is represented as a thin echoic line bounding the joint cavity. The articular space has the appearance of a triangular hypoechoic area with the apex directhy at the articular cavity and the base bounded by the joint capsule8.
In OA of the first carpometacarpal joint, sonography is able to demonstrate the presence of effusion, evaluate the quantity of the fluid present and reveal irregularities of the bone margins.
During the episodic synovitis that may appear in OA the presence of effusion is shown by the appearance of a sonolucent area within the articular space with contemporaneous capsular distension. Measurement of the distance between the base and the apex of the triangular articular area provides reproducible and quantitative information about the amount of joint effusion. In fact, due to the increased pressure within the joint cavity in the presence of effusion the capsule is convex to the joint and the longest distance between the base and the apex of the triangle is increased; in particular a distance greater than 3.33 mm indicates the presence of joint effusion8.
In OA of the first carpometacarpal joint the bone surfaces appear irregular and the presence of osteophytes is even detectable. In asymptomatic OA these features may be the only sonographic finding.
The frequent subluxation of the joint in OA develops an adduction deformity, which combined with the bony swelling, causes the classical appareance of «squaring» of the thumb base. Sonography is able to show the projection of the bone surface caused by the subluxation. The joint capsule is examined quite carefully by ultrasound. This structure is often thickened in OA and sonography provides the possibility to detect this thickening. The recent ultrasonographic use of high frequency transducers has allowed accurate study of the proximal and distal interphalangeal joints of the hand.
A joint space appears as a small triangular shaped anechoic area on longitudinal scan, delimited by the extensor tendon and bone margins10.
The hallmarks of interphalangeal joint OA are the Heberden's and Bouchard's nodes. These firm swellings, maximal on the superolateral aspect of the joints, are the most striking and characteristic clinical finding of the disease. Mucous cysts may form during initial growth.
Sonography easily reveals possible irregularity of the bone surface and of the joint margins due to Heberden's and Bouchard's nodes (fig. 5).
Figure 5.Sonography of proximal interphalangeal joint. Irregularities of the joint margins due to the presence of a Heberden's node.
Mucous cysts may also be studied. Sonography shows the presence of subcutaneous anechoic areas in the superolateral aspect of the joints.
With the joint in maximal flexion a portion of articular cartilage is evaluated and it is possible to reveal thinning and margin irregularity.
During inflammatory episodes the ultrasonographic technique shows the presence of effusion within the joint, documented by the appearance of anechoic collection within the joint space.
The joint capsule may also be studied by sonography that easily shows the frequent thickening of this structure in osteoarthritic interphalangeal joints.
The evaluation of metacarpophalangeal joints is particulary useful both in the detection of cartilaginous changes and effusion. With longitudinal dorsal scans keeping the proximal phalanx in active flexion, study of articular cartilage of the metacarpophalangeal heads is possible. In normal joints it appears as a thin (0.2-0.4 mm), regular, and sharply defined hypo-anechoic band9. In OA, irregularities of the sharp edges, narrowing of the band and scattered echoes within are revealed.
The presence of effusion is demonstrated when anechoic fluid collection appears within the joint cavity and the capsule is convex to the articular space.
The hip
Pain in the hip region may arise from several different structures and may be caused by various diseases. Of these, coxofemural OA is one of the most frequent. Radiologically, OA of the hip is easily diagnosed when subchondral sclerosis, marginal osteophytes and superolateral joint space narrowing are present. The most difficult situation to diagnose occurs in early OA, when the patient feels hip pain and has a normal radiograph. Effusion is often present in patients without radiological signs of OA. In these cases effusion may depict an early sign of the degenerative process11.
Unfortunately sonography is not able to accurately study articular cartilage because the ultrasonic beam is un able to pass through the bone7. For this reason articular cartilage is only partially visible with sonography, and the portion of cartilage shown is not the weight bearing area that is usually the most involved zone in OA.
To the contrary, ultrasound makes it possible to reveal the presence of synovitis and represents a valid help for the clinician who needs to evaluate a painful osteoarthritic hip. In fact, clinical examination of the hip is often unable to correctly evaluate the presence of effusion or the signs of synovitis of the hip joint. In particular, measuring the longest distance between the bone surface of the femur and the joint capsule effusion is demonstrated12. In normal conditions this distance is usually not more than 7 mm. When synovitis is present the capsule moves away from the bone surface and the distance increases. An ultrasonographic distance, of more than 7 mm between the hip joint capsule and the femur or a difference between the right and the left hips of more than 1 mm indicates joint effusion.
Moreover, evaluation of the echotexture of the joint cavity makes it possible to differentiate the presence of fluid collection by hypertrophic synovial tissue.
Irregularity of the bone surface of the head and the neck of the femur is easily detected by ultrasound, as are possible changes of the joint margins due to the presence of osteophytes.
The capsule is often thickened in OA. Sonography is able to examine this structure and evaluate possible thickening.
The acromokoclavicular joint
Degenerative changes occur early and frequently in the acromokoclavicular joint, because the incomplete disc of the adult articulation cannot compensate for the incongruity of the joint surfaces13.
A quite frequent cause of shoulder pain is osteoarthritic involvement of acromokoclavicular joint. As the precision of clinical examination studies of the acromokoclavicular joint are low14, and as shoulder pain is a frequent cause of attendance to both Rheumatologic and Orthopedic Units, the usefulness of sonography of the acromokoclavicular joint should always be considered in the evaluation of a painful shoulder, during the course of rheumatological clinical practise.
In fact sonography easily reveals possible irregularity of the bone surface and the joint margins (fig. 6) due to osteophytes15. It also shows the presence of joint effusion4, that is demonstrated when the capsule is convex to the articular space with simultaneous appearance of anechoic area within the joint cavity (fig. 6).
Figure 6.Sonography of the acromioclavicular joint. Irregularities of the joint margins (ostyeophyte) and joint effusion.
The joint capsule may also be quite carefully examined by sonography. This structure is often thickened in OA and the ultrasonographic technique detects possible thickening.
The possible subluxation of the joint in OA develops a deformity which may be well examined by sonograpy. In fact, it is able to show the projection of the bone surface caused by the subluxation.
The foot
In the osteoarthritic foot the most frequently involved joint is the first metatarsophalangeal joint. Sonography reliably reveals possible irregularity of the bone surface and of joint margins due to osteophytes.
In the presence of effusion it shows an anechoic area within the joint cavity with simultaneous convexity of the capsule.
Thickening of the joint capsule is frequently demonstrated.
Quite often in OA of the first metatarsophalangeal joint, especially when hallux valgus is present, bursitis over the medial aspect of the joint appears and may be well studied by sonography, showing fluid collection within the bursa.
Conclusions
This review analyzes the validity of sonography in OA, discussing the importance and limits of the ultrasonographic technique in the evaluation of the alterations that appear during the course of the disease. In most cases the early changes are detected with high accuracy. Standard radiography shows changes in bony structures but it is not able to demonstrate the early alterations of articular cartilage, to show the presence of effusion and to evaluate the conditions of periarticular soft tissues. Other imaging techniques, such as computed tomography and particulary magnetic resonance imaging, are of value but their high cost and low availability limit routine use.
In conclusion, sonography is a useful and important dignostic imaging method in the detection and monitoring of osteoarthritic joints.
The non-invasiveness and low cost of this technique justify its widespread application during recent years.