We present the case of a 23-year-old man who was admitted to the emergency department due to thoracic trauma with a gunshot wound in the right fifth intercostal space with the anterior axillary line, with an outflow tract in the third intercostal space on the left parasternal line. The patient exhibited signs of cardiac tamponade and grade IV hemorrhagic shock. Bilateral tube thoracostomy was performed, yielding a substantial left hemothorax (1500mL). As the patient presented deterioration of hemodynamic instability despite adequate resuscitation maneuvers, prompted immediate transportation to the operating room to perform a sternotomy. A posterior brachiocephalic trunk injury was identified, consisting of a laceration of 60% of total circumference, with an extension of over 2cm. The distal portion of the injury was resected and reconstructed using a 6mm polytetrafluoroethylene graft, with a proximal graft anastomosis employing a lateral anchor technique and a distal graft anastomosis using a parachute technique, secured with 4-0 polypropylene vascular sutures. The patient's postoperative recovery progressed favorably, he remained in the intensive care unit for 5 days and in general hospitalization for an additional 4 days. Further interventions were not required. A control CT angiography was performed 3 months postoperatively, demonstrating complete graft patency.
Presentamos el caso de un varón de 23 años que ingresó al servicio de urgencias por traumatismo torácico con herida de bala en el quinto espacio intercostal derecho con la línea axilar anterior, y un tracto de salida en el tercer espacio intercostal en la línea paraesternal izquierda. El paciente presentaba signos de taponamiento cardiaco y shock hemorrágico grado IV. Se realizó toracostomía con inserción de tubo de tórax bilateral, identificado un hemotórax izquierdo sustancial (1.500mL). Como el paciente presentó deterioro de la inestabilidad hemodinámica a pesar de las adecuadas maniobras de reanimación, se motivó su traslado inmediato al quirófano para realizarle una esternotomía. Se identificó una lesión del tronco braquiocefálico posterior, consistente en una laceración del 60% de la circunferencia total, con una extensión superior a 2cm. La porción distal de la lesión se resecó y reconstruyó mediante un injerto de politetrafluoroetileno de 6mm, con una anastomosis del injerto proximal mediante técnica de anclaje lateral y una anastomosis del injerto distal mediante técnica de paracaídas, asegurada con suturas vasculares de polipropileno 4-0. La recuperación postoperatoria del paciente evolucionó favorablemente, permaneció cinco días en unidad de cuidado intensivo y en hospitalización general por cuatro días adicionales. No fueron necesarias más intervenciones. Se realizó una angiografía por TC de control a los tres meses del postoperatorio, demostrando permeabilidad completa del injerto.
Trauma to the thoracic vessels is a highly critical and potentially life-threatening condition that can result from high or low energy trauma. Which encompass a broad range of injuries associated with a significantly elevated mortality rate. These injuries involve various structures such as the thoracic aorta and its primary branches, superior vena cava, thoracic segment of the inferior vena cava, innominate venous trunk, pulmonary artery and its main branches, pulmonary veins, as well as axillo-subclavian vessels.1
Thoracic trauma is the second cause of trauma related death following head trauma. It has been reported that 6% of thoracic trauma cases involve vascular injuries. Moreover, 32% of these injuries occurring in the thorax, primarily affecting the aorta. Thoracic trauma contributes to approximately 15% of deaths caused by traffic accidents and leads to a global mortality rate ranging from 5% to 15% among hospitalized patients, particularly in cases of severe thoracic injuries.2
Considering the high mortality rates and potential risks to the population, it is crucial to implement initial resuscitation measures and actively search for life-threatening injuries to determine the necessity of urgent thoracotomy. However, the management of thoracic vascular injuries poses a challenge due to the difficulty in diagnosis and its low incidence. Open surgery involving invasive repair of the vessel continues to be the primary approach for achieving proximal and distal control of the injury. Additionally, endovascular interventions employing balloon occlusion, embolization, and stents are utilized.3
The objective of this case report is to comprehensively review the essential surgical principles associated with the appropriate approach and treatment of penetrating chest trauma involving major thoracic vessel injuries. This report is prompted by the recognition of the significant responsibility that Latin American surgeons bear in overseeing emergency departments for trauma management
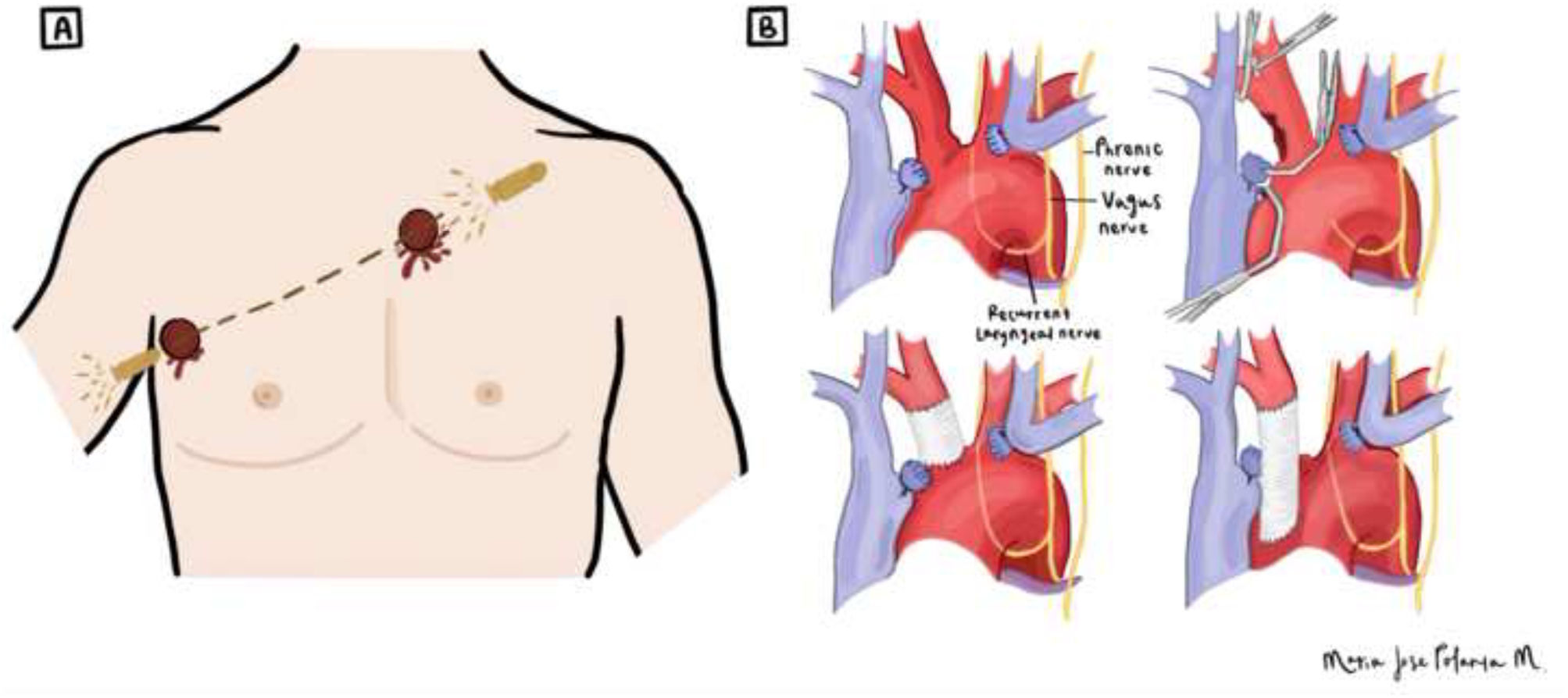
Case descriptionA 23-year-old male presented to a local emergency department with a transmediastinal gunshot wound entering the right hemithorax at the 5th intercostal space along the anterior axillary line and exiting the left hemithorax at the 3rd intercostal space along the left parasternal line (Fig. 1A), resulting in an unstable condition. His vital signs upon admission indicated a heart rate of 119 beats per minute, a blood pressure of 60/42mmHg, a temperature of 37°C, and a respiratory rate of 30 breaths per minute. The patient exhibited signs of cardiac tamponade, including dyspnea, tachypnea, pallor with mucocutaneous involvement, and grade IV hemorrhagic shock (blood loss>40% of total blood volume, systolic blood pressure<90mmHg, heart rate>120 beats per minute and signs of severe tissue hypoperfusion). Upon admission, bilateral tube thoracostomy was performed, yielding a substantial left hemothorax of 1500mL.
Diagram illustrating (A) The gunshot trajectory of the patient; the bullet entered the right hemithorax at the 5th intercostal space along the anterior axillary line and exited the left hemithorax at the 3rd intercostal space along the left parasternal line. (B) The surgical reconstruction of the brachiocephalic trunk performed during surgery.
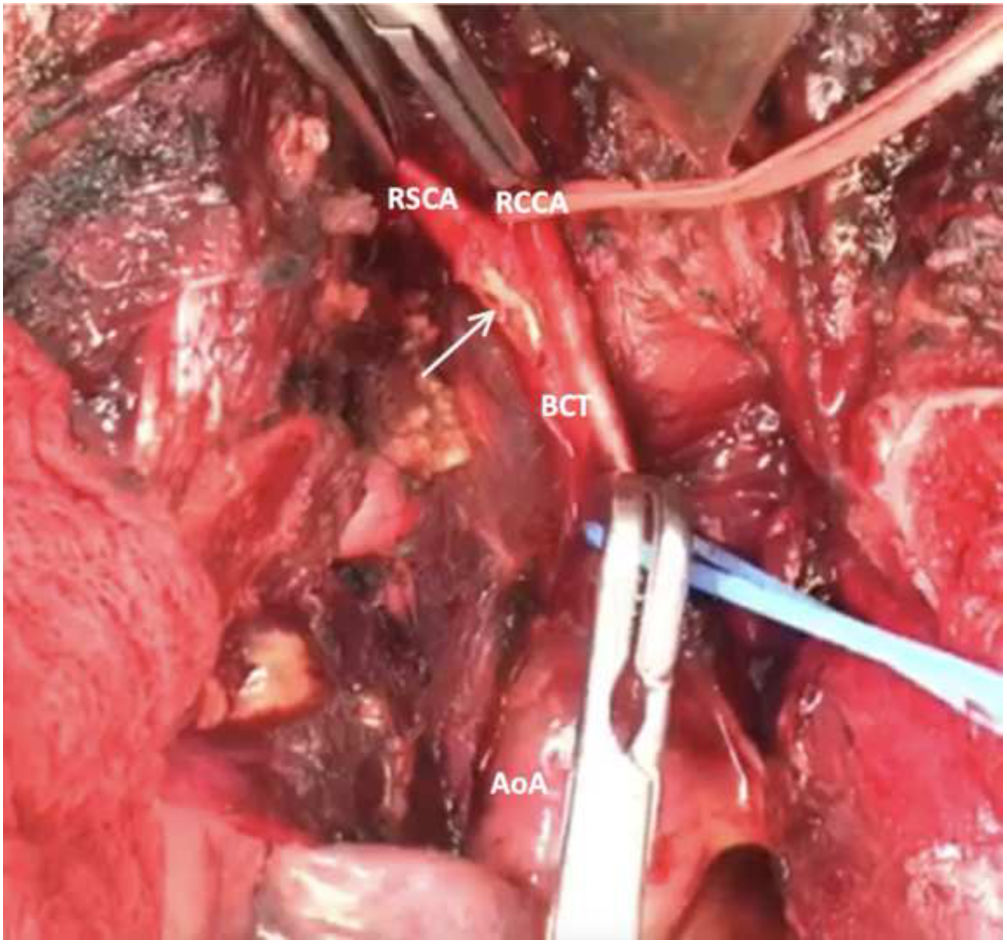
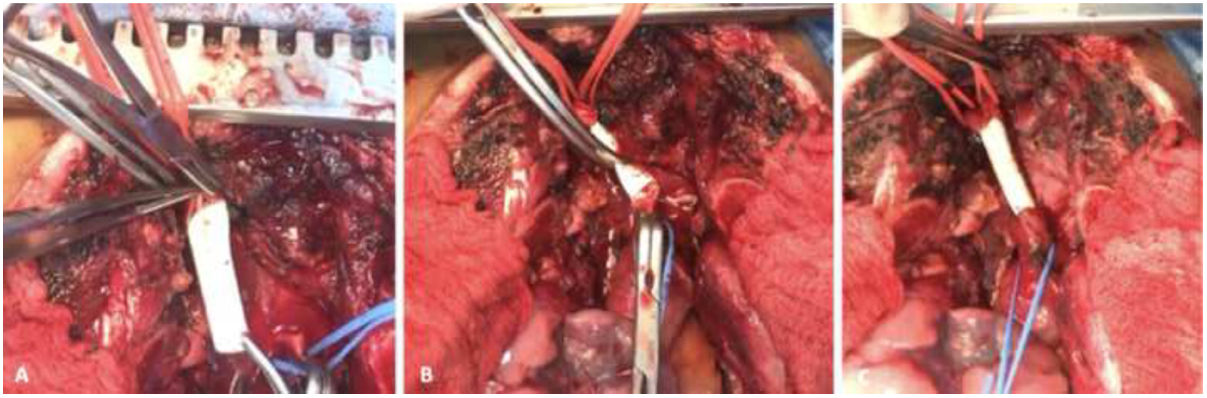
As the patient presented deterioration of hemodynamic instability despite adequate resuscitation maneuvers, prompted immediate transportation to perform a sternotomy. During the procedure, we dissected and ligated the left innominate vein, achieving proximal and distal control of the brachiocephalic trunk, right common carotid artery, and right subclavian artery. A posterior brachiocephalic trunk injury was identified, consisting of a laceration of 60% of total circumference, with an extension of over 2cm (Fig. 2). The patient does not exhibit any additional lesions on the heart ventricles, lungs, or other thoracic structures. The distal portion of the injury was resected and reconstructed using a 6mm polytetrafluoroethylene (PTFE) graft, with a proximal graft anastomosis employing a lateral anchor technique and a distal graft anastomosis using a parachute technique, secured with 4-0 polypropylene vascular sutures (Figs. 1B and 3). The patient received 48h of cefazolin antibiotic prophylaxis, which was subsequently discontinued. Systemic heparinization was initiated at a unique dose of 6500IU (dosage: 100IU/kg), followed by proximal–distal thrombectomy to prevent thromboembolic events. Protamine was not required to reverse the heparin administered during the surgical procedure.
Gunshot wound of the bifurcation of the brachiocephalic trunk with compromise of the 60% of the vessel with injury of the right common carotid artery and the right subclavian artery (arrow). AoA: aortic arch, BCT: brachiocephalic trunk, RCCA: right common carotid artery, RSCA: right subclavian artery.
The patient's postoperative recovery progressed favorably, with approximately 200mL of postoperative bleeding collected through the chest tube. He remained in the intensive care unit for 5 days before being transferred to the general ward for an additional 4 days. No complications occurred, and the surgical site remained free from infection. Further interventions were not required. The patient did not receive antiplatelet treatment after hospital discharge. A control CT angiography was performed 3 months postoperatively, demonstrating complete graft patency.
DiscussionTrauma is a significant concern in the context of Latin America, representing a prevalent public health issue and a leading cause of mortality among the young population. Notably, rural regions exhibit elevated mortality rates due to the predominant location of trauma centers in major cities, resulting in limited access to quality care in smaller towns. The primary risk factors for trauma include male gender, young age, low socioeconomic status, and residing in rural areas,4 which were present in our patient.
Patients experiencing trauma may present varying degrees of hemodynamic instability, necessitating intervention such as immediate sternotomy is performed without preliminary diagnostic imaging to address potential life-threatening injuries promptly within the operating room. Conversely, in hemodynamically stable patients, additional diagnostic tools, such as angiotomography, can be employed to establish a precise diagnosis before proceeding to surgery.
Sternotomy provides optimal visualization of mediastinal structures, including the anterior heart and great vessels, thereby facilitating diverse surgical interventions5. It is particularly advantageous when the injury is located medially to the midclavicular line. Moreover, sternotomy enables a quicker postoperative recovery without significantly compromising pulmonary function in contrast to the effects observed with anterolateral thoracotomy.2,3
For control of the brachiocephalic trunk, median sternotomy is used, allowing proximal control at its origin from the aortic arch, with possible extension into the right neck if distal control is required. Repair generally involves exclusion and bypass, commonly at the artery's origin.6 These lesions due to their rarity and localization in a challenging anatomical territory, exhibit elevated morbidity and mortality rates. Therefore, a profound understanding of the anatomy is indispensable for effective treatment of these uncommon lesions.
The choice of the arterial graft material remains a debate. Studies have highlighted the potential of expanded PTFE as a substitute graft for small arteries and veins. In a study by Vaughan et al., the efficacy of PTFE prostheses in treating vascular wounds following trauma was investigated. All patients who underwent segmental repair of axillary, brachial, femoral, and popliteal vessels maintained robust distal pulses and viable extremities. Remarkably, none of the grafts thrombosed or became infected, even when soft-tissue injuries were encountered during the repair. In situations requiring interposition graft placement to restore distal flow in small arteries and veins, PTFE grafts prove themselves as viable prostheses.7
Several studies suggest that autologous vein grafts serve as a viable option when suitable veins are available, as they exhibit a comparable rate of complications to PTFE during a 62-month follow-up period. Upon subgroup analysis of complications, autologous vein grafts demonstrated an 8-year freedom from complication rate of 77%, while PTFE exhibited only a 31% rate for the same outcome.8 Furthermore, a comparison between Dacron® and PTFE grafts revealed no significant differences in primary and secondary patency rates after a 2-year period.9 PTFE grafts maintained their integrity even in the presence of staphylococcal infection, experiencing fewer disruptions compared to Dacron. Regardless of the graft material employed, it is imperative to thoroughly clean trauma sites, remove devitalized tissue, and cover repairs with healthy tissue to achieve an optimal postoperative outcomes.
Over the past decade, an endovascular approach to treating vascular trauma has gained prominence due to its established effectiveness in treatment, coupled with a reduction in morbidity and mortality rates. A study conducted in Chile by Bergoeing et al. demonstrated 100% graft patency over a 24-month follow-up period in eight patients with traumatic lesions in the supra-aortic vessels, who were treated with an endograft. Notably, only one patient exhibited partial collapse of the endograft, necessitating the use of an additional bare metal stent to maintain patency.10 In contrast, in our resource-limited setting and given the urgent surgical requirement, an open approach was deemed necessary for our patient.
A similar case was presented by Oliveira et al., in which a traumatic fistula formed between the brachiocephalic trunk and vein following a gunshot trauma. Successful vessel reconstruction was performed using polypropylene sutures without the implementation of a vascular graft.10 Blunt trauma can also result in thoracic vessel injury. Shiddiqi et al. reported a case involving traumatic aortic dissection, brachiocephalic trunk injury, and right diaphragm injury in a patient who was struck by a motor vehicle. Vascular repair was achieved through a Dacron graft with complete patency after two months.11
We observe certain limitations in our study, given its monocentric, observational, and descriptive nature, which focused on a single case presentation. However, it is essential to emphasize the significance of reporting such cases in the context of chest trauma. This practice is pivotal for establishing a multicentric database that can serve as a valuable resource for future studies in Colombia and Latin America. In Colombia, general surgeons typically serve as the initial responders for trauma cases, underscoring the importance of sharing information about the approach and treatment of this medical condition. Such knowledge dissemination can lead to improvements in the outcomes of chest trauma management within our population, especially in resource-limited settings.
ConclusionChest trauma accompanied by thoracic vessel injuries is a critical clinical condition that places life at risk. An optimal clinical approach, intraoperative recognition of these injuries, and a thorough understanding of human anatomy are essential components for the successful management of trauma patients. Further studies and advancements in this area are imperative to continually refine our approach and optimize patient care.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this investigation.
Informed consentInformed consent was obtained from the patient for the publication of this article.
FundingNone funding declared from the authors.
Conflict of interestsThe authors declare that they have no conflict of interest.