Endoscopic treatment of Zenker diverticulum is considered feasible, effective and safe. The use of the Ligasure™ vessel sealer provides adequate and quick dissection of tissue, achieving effective haemostasis.
Patients and methodsRetrospective, descriptive study of all patients with Zenker diverticulum who were treated by endoscopic diverticulotomy using Ligasure™. The procedure was performed in the endoscopy unit under deep sedation controlled by the endoscopist. Patients were subsequently admitted for observation and, after discharge, were followed-up in the outpatient clinic.
ResultsEight patients, 5 women and 3 men, mean age 78±15 years, 25% ASA I, 36% ASA II, 14% ASA III and 25% ASA IV. Main symptom: dysphagia. Diverticula size: 1–7cm. Technical success: 100%. Complications: one patient with upper gastrointestinal bleeding. Average stay: 24h. Seven patients: asymptomatic; one patient with partial improvement, requiring repeat endoscopic intervention. Surgery and morbidity and mortality: 0%.
ConclusionThe treatment of Zenker diverticulum by endoscopic diverticulotomy using the Ligasure™ vessel sealer is highly effective, fast and safe, and could be considered the treatment of choice.
El tratamiento endoscópico del divertículo de Zenker es considerado viable, efectivo y seguro. La utilización de la técnica sellado-sección mediante Ligasure™ proporciona una adecuada y rápida disección del tejido, logrando una hemostasia efectiva.
Pacientes y métodosEstudio retrospectivo, descriptivo, de todos los pacientes con divertículo de Zenker que fueron tratados a través de una diverticulotomía endoscópica utilizando el Ligasure™. El procedimiento se realizó en la unidad de endoscopias, bajo sedación profunda controlada por el endoscopista. Posteriormente, los pacientes ingresaron para observación y, después del alta, se realizó un seguimiento por consultas externas.
ResultadosOcho pacientes, 5 mujeres y 3 hombres, edad media: 78±15 años; 25% ASA I; 36% ASA II; 14% ASA III, y 25% ASA IV. Síntoma principal: disfagia. Tamaño de los divertículos: 1 a 7cm. Éxito técnico: 100%. Complicaciones: un paciente con HDA. Estancia media: 24h. Siete pacientes: asintomáticos; un paciente con mejoría parcial, necesitando reintervención endoscópica. Cirugía y morbimortalidad: 0%.
ConclusiónEl tratamiento del divertículo de Zenker mediante diverticulotomía endoscópica con Ligasure™ proporciona una gran eficacia, rapidez y seguridad, por lo que podría plantearse como primera elección de tratamiento.
Zenker diverticulum is a pharyngoesophageal diverticulum that was first described in 1769 by the English surgeon Abraham Ludlow, and later characterized in 1877 by the German pathologist Friedrich Albert von Zenker.1 The mucosa of the hypopharynx protrudes through an area of muscle weakness located between the inferior constrictor muscle of the pharynx and cricopharyngeal muscle.
It has a predilection for males between the ages of 70 and 80 years2 and estimates suggest that its incidence, though difficult to calculate because the disorder can be completely asymptomatic, is about 2 cases per 100,000.3
Dysphagia and regurgitation of food are the main symptoms, and it is primarily diagnosed by upper endoscopy or barium swallow.
Treatment, which is indicated when symptoms are persistent and progressive, can be surgical, currently diverticulectomy and myotomy, or endoscopic, in which the diverticular septum is dissected.
The first endoscopic treatment was performed in 1917 by Mosher using scissors, and procedure was abandoned after the patient died from mediastinitis. Later, in the 60s, Dohlman used diathermy to successfully cut through the septum.1,3,4
The difficulty of the procedure lies in removing the diverticular septum without making a deep dissection that could perforate the oesophagus. For this reason, various techniques have been developed in order to reduce the risk of perforation. In the largest published series of endoscopic diverticulotomy, the needle-knife or hook-knife were used for dissection, with high success rates. Other techniques, such as the EndoGIA Autosuture® stapler, lasers, argon plasma coagulation and, more recently, the dissect and seal technique using the Ligasure™ vessel sealing system have also been used.
Patients and methodsWe conducted a retrospective study of all patients with Zenker diverticulum seen in the Gastroenterology Department of Río Carrión Hospital in Palencia between 2009 and 2015, who were treated with endoscopic diverticulotomy using the Ligasure™ system.
The following parameters were analysed: sex, age, ASA, preoperative symptoms, size of the diverticulum, technical success (defined as nearly total resection of the septum with no immediate complications), hospital stay, complications, outcomes of the endoscopic procedure, follow-up and need for surgery.
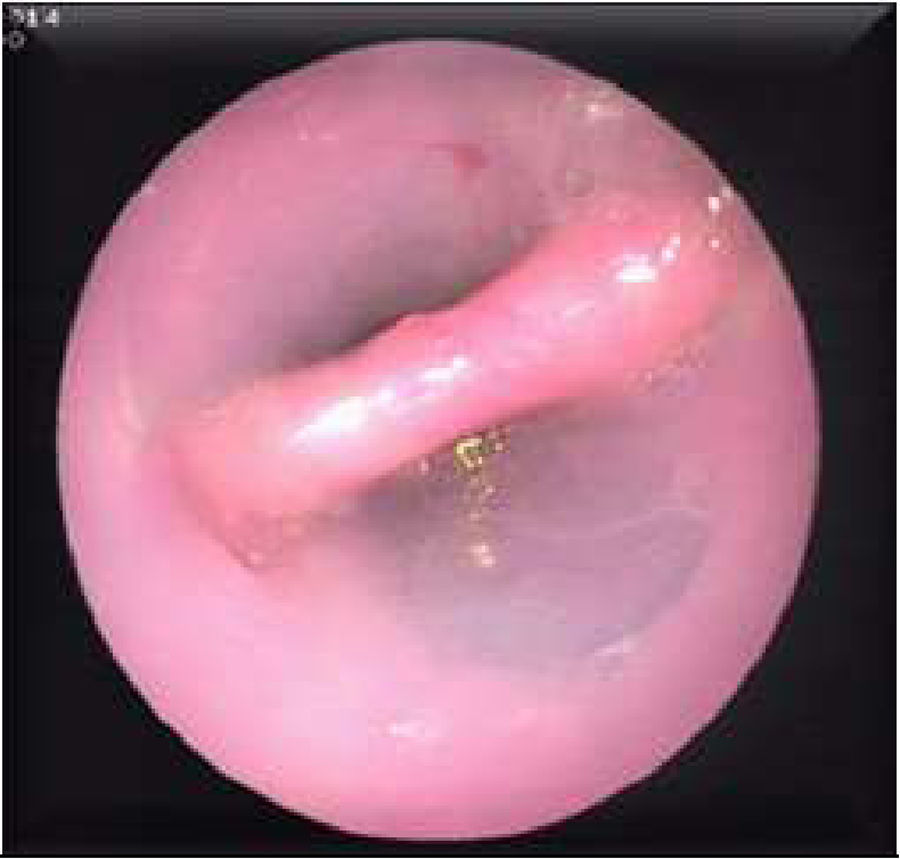
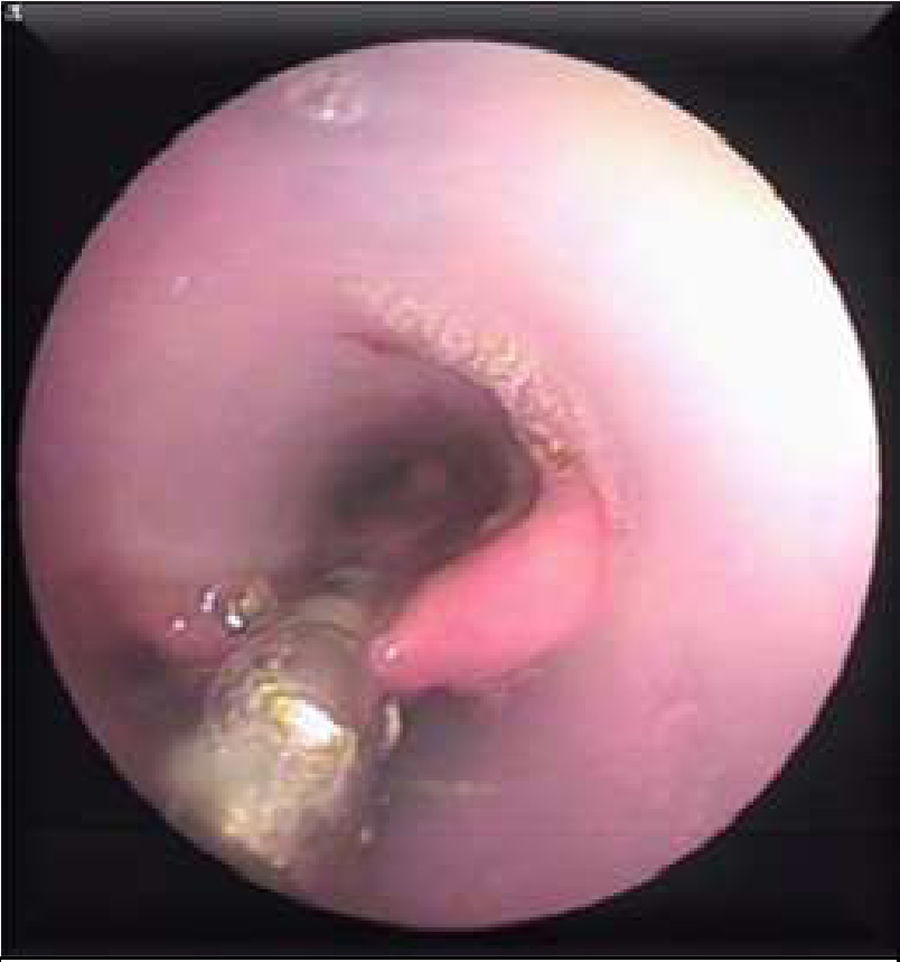
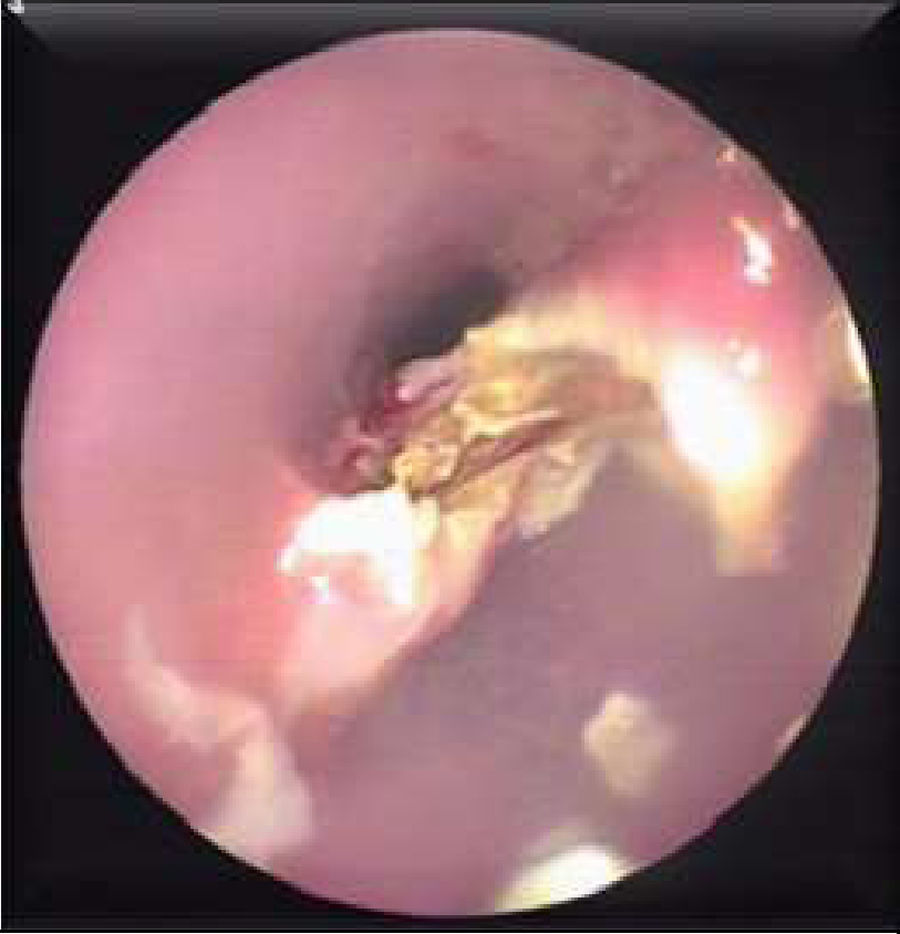
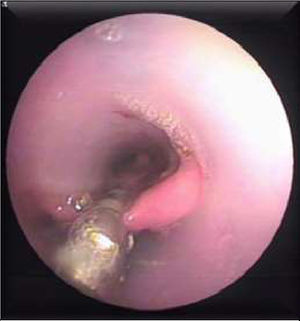
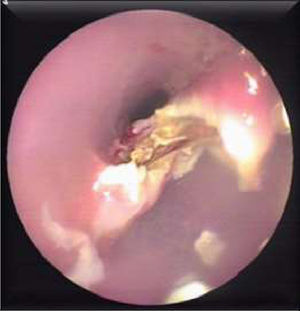
Patients were instructed to fast for at least 6h prior to the procedure. A few minutes before the endoscopy, they were given a dose of antibiotic (i.v. ceftriaxone 1g or i.v. amoxicillin/clavulanic acid 1g/125mg). The endoscopic technique was performed under deep sedation, using intravenous administration of propofol (Propofol Lipuro 10mg/ml, Braun) controlled by the endoscopist. The flexible endoscope (Fujinon EG-590WR Standard) was introduced to visualize the diverticulum and the oesophagus. A guide wire (0.035in.×450cm, Jagwire™ High Performance Guidewire, Boston Scientific) was introduced through the working channel to the stomach, and the endoscope was removed. A hole was made, manually, in the long flap of the 30cm long×22mm diameter double-lipped overtube (ZDO-22-30, Cook Medical, Limerick, Ireland) and the guide wire was threaded through this opening. Then the overtube was positioned under direct endoscopic vision. Threading the guide wire through the hole ensures that the long flap is positioned in the oesophageal lumen and the short flap is in the diverticulum, exposing the diverticular septum between the 2 flaps (Fig. 1). Diverticulum depth was measured from the start of the septal wall to the base of the diverticulum. Then, a smaller endoscope (Fujinon EG-270N5) was introduced into the diverticuloscope. With the septum clearly visualized, the Ligasure™ (5mm to 37cm, LS1500, Covidien, Medtronic) was introduced into the diverticuloscope in parallel with the endoscope. With a 2/3 seal setting (ForceTriad™ Energy Platform, COVIDIEN, Medtronic), the septum is initially coagulated and sealed laterally and then coagulated, sealed and cut in the centre in several cycles up to 2–3mm from the base of the diverticulum (Figs. 2 and 3). Approximately 1cm of septum was resected in each cycle, except in diverticula measuring 1cm, in which shorter cuts of about 2–3mm were made, due to the increased risk of perforation. At the end of each cycle, the area was inspected for signs of bleeding. Once the procedure was completed, patients were kept under observation for at least 24h. After this, if there were no signs of complications such as fever, chest pain or haematemesis, oral tolerance began with liquids at 6h, a soft diet at 24h, and normal diet was resumed after 7 days. Patients were followed up as outpatients.
ResultsA total of 8 patients (3 men and 5 women) were included, with a mean age of 78±15 years, 25% were ASA I, 36% were ASA II, 14% were ASA III, and 25% were ASA IV.
In the ASA IV group, due to their high-risk clinical status, propofol for sedation was administered at a slower rate (150ml/h vs 200ml/h) to prevent secondary complications such as respiratory depression. We would add that the diverticuloscope helps protect the airway and prevents bronchoaspiration, which is often fatal in these patients.
It should be noted that all patients presented symptoms, mostly dysphagia and regurgitation, and the diverticula ranged in size from 1 to 7cm.
Average time from reaching the target level of sedation to completion of the procedure was 30min. The technical success rate was 100%, with an average stay of 24h.
In general, the patients presented no complications during hospitalization, except for one patient who was seen in the emergency room for non-severe haematemesis about a week after discharge. In this case, an upper gastrointestinal endoscopy was performed, which showed a clot attached to the resection site. No endoscopic therapy was required.
Of all the patients treated, only one presented partial clinical improvement. Diverticulotomy was repeated 3 months after the first intervention, following which the patient was asymptomatic.
Patients were followed up for an average of 20±16 months, without any clinical recurrence or need for reintervention.
DiscussionThe pathophysiology of Zenker diverticulum is not entirely clear. Some authors have suggested that it is caused by obstructive pathophysiology at the upper oesophageal sphincter that causes uncoordinated swallowing and impaired relaxation and spasm of the cricopharyngeal muscle. Other hypotheses point to histological alterations, such as muscle degeneration and fibrosis.4,5
Malignant transformation, however, is rare (0.5–1.5% of cases) due to the slow progression of the diverticulum. When it does occur, it most frequently manifests as squamous cell carcinoma.6
The ideal treatment for this disease, taking into account both safety and efficacy, has been much debated in recent years; however, there is insufficient scientific evidence on which to base a definitive strategy. Generally, surgery is preferred in young and/or low-risk patients, and endoscopic techniques in other patient groups.
In 2011, Lopes da Silveira et al. published a meta-analysis reviewing 5 comparative studies with a total of 630 patients diagnosed with Zenker diverticulum; 339 were treated with surgery and 291 endoscopically. The group treated endoscopically showed a mortality rate of 0.29%, 7% morbidity and 84% efficacy, while the surgical group showed a mortality of 0.35%, 5% morbidity and 85% efficacy.7 Outcomes, therefore, were largely similar between the two groups. However, none of the studies included in this meta-analysis were randomized and none used the Ligasure™ system.
Cañete-Gómez et al., meanwhile, described a series of 33 cases undergoing diverticulectomy and myotomy using open surgery. This group reported an immediate postoperative morbidity rate of 27.2% due to partial dehiscence of the diverticulectomy suture line and oesophagocutaneous fistula.8
In a more recent (2016) meta-analysis of 20 studies reporting endoscopic diverticulotomy in a total of 813 patients, the authors concluded that endoscopic resection of the diverticular septum was effective and safe, with a pooled success, adverse events, and recurrence rate of 91%, 11.6%, and 11%, respectively. In this study, nearly all complications were resolved conservatively, and no patient required surgery. It should be added that the endoscopic instruments and techniques used did not differ significantly, and only the use of a soft diverticuloscope was associated with a higher success rate.9 This meta-analysis did not include studies in which Ligasure™ was used.
Endoscopic treatment has several advantages compared with surgery. Firstly, a shorter intervention; in our hospital the procedure lasted about 30min; this is in line with the study published by Noguera-Aguilar et al. who reported an average of 33min for each procedure.4 Secondly, neither general anaesthesia nor hyperextension of the neck is required; the hospital stay is shorter, and return to oral intake takes place earlier. Furthermore, endoscopic re-intervention, if needed, is equally safe, and if unsuccessful, surgical treatment is not contraindicated.10 Another advantage of this technique is cost. Shane et al. showed that, although the cost of endoscopy and surgery is similar, the shorter hospital stay associated with diverticuloscopy significantly reduces the total cost of the treatment.11
Diverticulotomy, involving myotomy with the needle-knife scalpel and later with the hook-knife, has been the gold standard for many years, and has a high success rate. However, it is not without its drawbacks: on the one hand, the needle-knife presents risk of perforation or abscess formation in up to 23% of cases due to the downward pressure used during incision, and up to 12 cycles may be needed to achieve complete septostomy in particularly fatty septa.12 If bleeding occurs, coagulation is delayed and other methods, such as argon plasma coagulation (APC), are needed.13,14 On this subject, Huberty et al. and Brueckner et al. each published an article on diverticulotomy using the needle-knife and hook-knife, respectively, and reported a similar rate of successful outcomes and complication with both techniques. Both studies observed a high recurrence rate of 23% vs 30%, respectively. This could be related to incomplete resection of the diverticulum. In both cases, most recurrences were resolved with further endoscopic procedures.13,14
Another technique is EndoGIA Autosuture® stapler. This has proven difficult to handle with the endoscope, and its diameter (12mm) can obstruct visualization during the procedure, leaving around 1cm of the distal end of the diverticulum unresected.1,4,10
Similarly, the laser method requires a microscope and tissue is left virtually unsealed. In addition, several studies have shown a high risk of recurrence and endoscopic perforation.1,3,4,10
The Ligasure™ system uses heat and pressure to coagulate and seal vessels and tissue bundles up to 7mm in diameter without dissection or isolation. A blade located on the shaft can be used to divide the sealed tissue. The instrument has several advantages over the techniques described above: with a diameter of just 5mm it takes up little space and is very easy to handle. It is also highly precise and can deliver small, controlled septal incisions of up to 1cm in length. The tissue is dissected and sealed in the same movement. In addition, the Ligasure Impact™ includes electrocoagulation for improved control of the bleeding that may occur during the procedure.
Other strategies can also increase the safety of the procedure, such as incomplete resection of the septum (leaving around 3–5mm at the distal end to avoid oesophageal perforation and mediastinitis) and the possibility of placing endoscopic clips to ensure the resected septum is properly sealed. Nevertheless, we did not need to use clips in any patients included in our study. This was an added advantage over other techniques, in which clips are placed as a matter of course. In conclusion, the Ligasure speeds up endoscopic diverticulotomy, improves safety, delivers good septum resection and minimizes postoperative recovery time.
In addition, comparing studies using Ligasure™, despite their small sample size, with studies using the needle-knife or hook-knife shows a significantly lower rate of recurrence in the former. In both our study and that of Noguera-Aguilar et al. in 2014, no patient presented recurrence of symptoms during the follow-up period.4 Nielsen et al., however, published a study with 15 patients, and reported a recurrence rate of 13% (2 patients)1; we attribute our zero recurrence rate to a more complete resection of the septum in the first procedure.
The only disadvantage of this technique, in our opinion, is the need to introduce the Ligasure™ in parallel with the diverticuloscope, which can reduce visualization of the diverticular septum.
In our hospital, we have used Ligasure™ for dissection of the septum since endoscopic diverticulotomy was introduced in 2009, and we therefore cannot compare our results with those obtained from other techniques in our setting. Similarly, there are no prospective, randomized studies comparing this technique with other endoscopic or surgical strategies; however, our experience has been highly satisfactory, since only 1 patient in our series required re-intervention, and in that case the outcome was also successful.
ConclusionIn conclusion, we believe that diverticulotomy performed using Ligasure™ is a minimally invasive technique with excellent results in the treatment of Zenker diverticulum. We also believe that this technique will become the strategy of choice in this pathology, irrespective of patient age and surgical risk. More prospective, randomized studies are needed to explore the benefits of this technique, although this is scarcely feasible given the low incidence of this disease.
Conflicts of interestThe authors declare that there are no conflicts of interest.
Please cite this article as: Moreira da Silva BA, Germade A, Pérez Citores L, Maestro Antolin S, Santos F, Sánchez Barranco F, et al. Diverticulotomía endoscópica utilizando Ligasure™. Gastroenterol Hepatol. 2017;40:80–84.