The incidence of long bone pseudarthrosis ranges from 2% to 10%, with the femur being the second most commonly affected bone. There are local and systemic factors that influence the development of this condition. Various implants such as plates, nails, external fixators and combinations of the foregoing, plus grafts and materials to facilitate consolidation are reported in the literature to treat pseudarthrosis.
ObjectiveTo present the special case study of a patient diagnosed with pseudarthrosis of the femur who presented with poliomyelitis sequelae.
Case reportA 40-year-old man with a history of poliomyelitis previously treated with osteosynthesis on 2 occasions due a fracture of the left femur. He was assessed and diagnosed with pseudarthrosis of the left femur with poliomyelitis sequelae. He underwent surgery with Luque rod fixation, frozen fibular graft and bone graft chips. His bones consolidated 12 months after the operation and he was able to resume normal activities at 16 months.
La pseudoartrosis en los huesos largos tiene una incidencia del 2 al 10%; el fémur ocupa el segundo lugar en frecuencia. Existen factores locales y sistémicos en el desarrollo de esta patología. Para su tratamiento está descrito el uso de diversos implantes, placas, clavos, fijadores externos y combinaciones entre los mismos, más aplicación de injerto y materiales que coadyuven en la consolidación.
ObjetivoPresentación de un caso especial con diagnóstico de pseudoartrosis en fémur que presenta secuelas de poliomielitis.
Caso clínicoHombre de 40 años con antecedente de poliomielitis, inicialmente tratado con osteosíntesis en 2 ocasiones por fractura de fémur izquierdo. Es valorado y se hace diagnóstico de pseudoartrosis de fémur izquierdo y secuelas de poliomielitis. Tratamiento enclavado con una barra de Luque, injerto de peroné congelado y chips. Tuvo una consolidación a los 12 meses postcirugía y su reincorporación a sus actividades fue a los 16 meses.
No single definition of pseudarthrosis has been universally accepted, but it tends to be recognised as a lack of bone consolidation characterised radiographically by rounded and sclerotic ends and obliteration of the medullary canal.1–5 The incidence of pseudarthrosis in the shafts of long bones ranges from 2% to 10%, with the femur being the second most commonly affected bone after the tibia.1–4,6 Its treatment represents a challenge for orthopaedic surgeons and many different methods to achieve consolidation have been reported, including plates, nails, external fixators and a range of implants, in combination with autologous and heterologous bone grafts and materials to facilitate bone consolidation.1–8
ObjectiveTo present a special case study of a patient with poliomyelitis sequelae diagnosed with diaphyseal pseudarthrosis of the femur and polio.
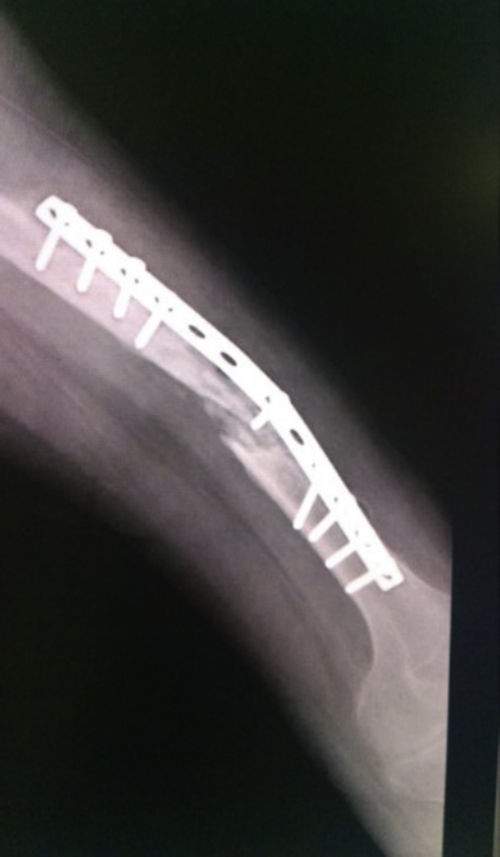
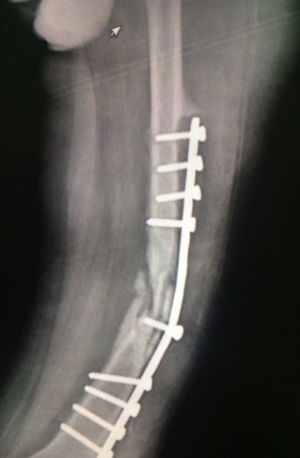
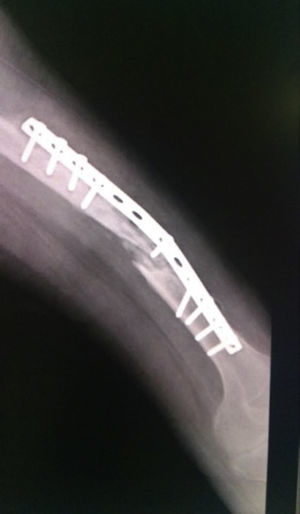
Case studyA 40-year-old male patient with poliomyelitis sequelae in the lower left limb who suffered a fall to the ground in August 2012. The patient was admitted to hospital where he was diagnosed with a fracture of the left femoral shaft and underwent DCP plate fixation with a poor outcome and rupture of osteosynthesis material. A narrow DCP plate with 12 holes and 9 screws was subsequently applied in September 2012, with an unsatisfactory outcome, persistent pain, deformity and walking disability. He was assessed again in August 2013 and clinically and radiologically diagnosed with uninfected atrophic pseudarthrosis of the femoral shaft with wear of osteosynthesis material and lateral reabsorption below the plate (Figs. 1 and 2).
The patient underwent an intramedullary nailing procedure on 08/08/2013 with a 4.5-mm diameter Luque rod (as the femoral canal measured 5mm in diameter), semi-tubular frozen fibular xenograft, one lateral rod and one anterior rod fixed with 3.5-mm cortical screws and bone graft chips.
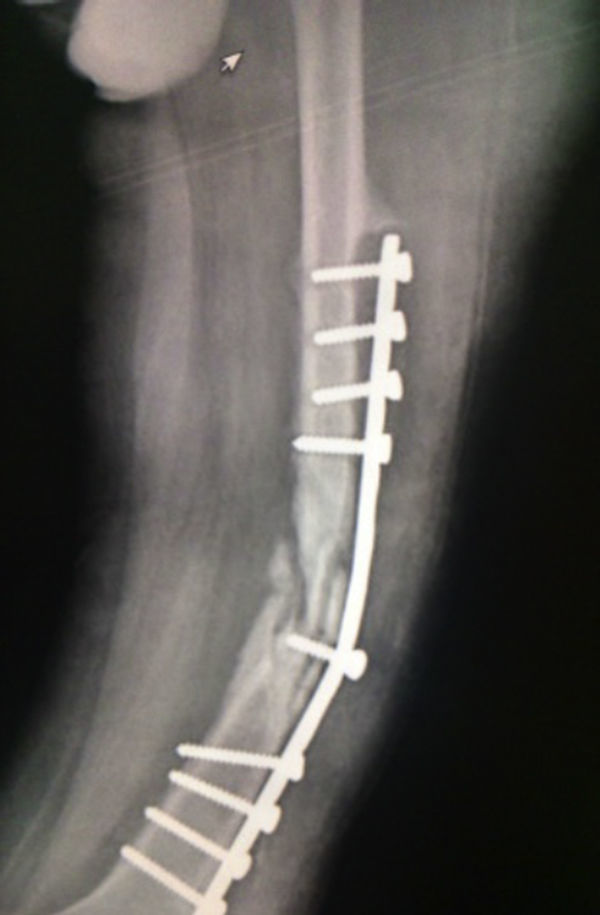
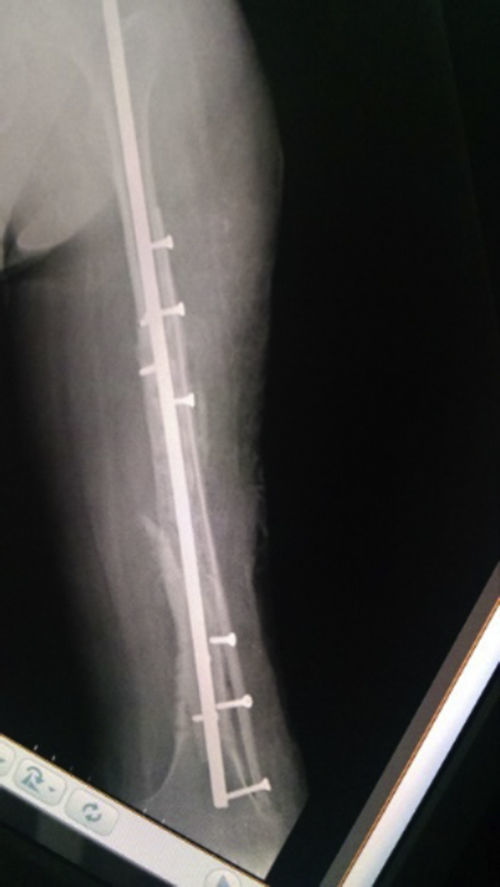
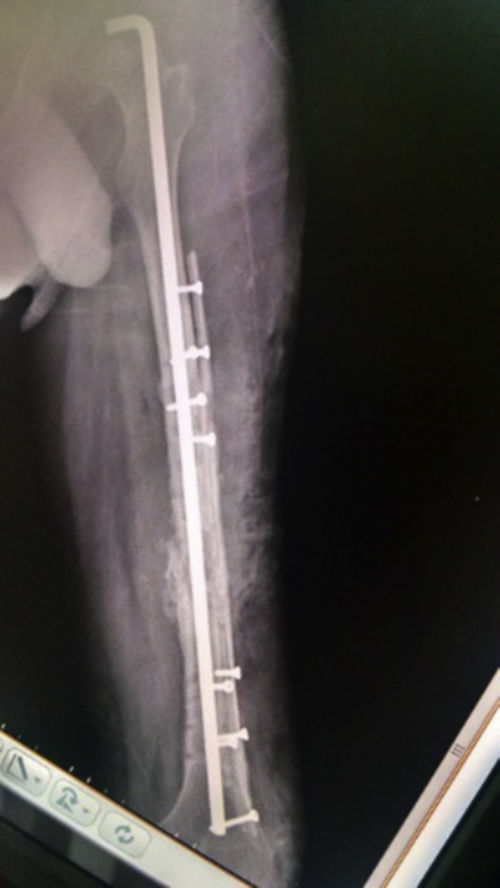
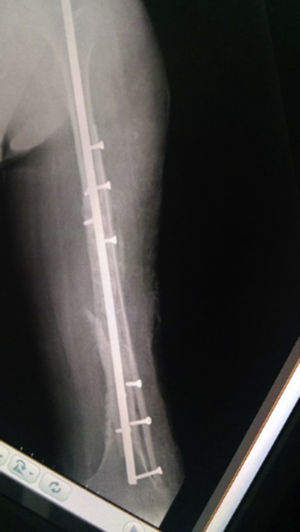
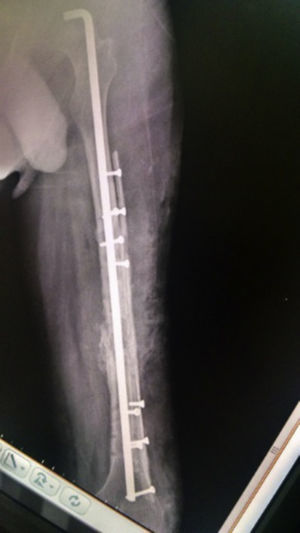
The patient progressed favourably, commencing partial-weight-bearing walking 4 months after surgery and complete weight-bearing at 7 months. Complete consolidation was radiographically confirmed at 12 months and the patient resumed the activities performed prior to the fracture 16 months after surgery (Figs. 3–5), experiencing no complications during the 36-month follow-up period.
DiscussionPoliomyelitis is estimated to have affected more than one million people worldwide and was the most common cause of childhood disability in the 1950s. Survivors from that period, who are now between 50 and 70 years old, suffer from morbidities collectively termed post-polio syndrome.9–11 A study by Mohammad et al. found that more than 96% of polio survivors had osteoporosis or osteopenia in the affected limb and the major osteoporotic fracture incidence in this cohort was as high as 38% over 5 years.12 Almost all fractures involved the femoral neck of the affected or atrophic limb.9,12,13 The other general factors that contribute to increased risk of osteoporosis and fragility fractures in this cohort of patients are likely to be elderly age, lack of physical activity due to muscle weakness and lack of sunlight exposure that leads to vitamin D deficiency.9
The femur is the second most common site of pseudarthrosis.1–5 Many local factors contribute to this condition, such as poor bone quality (as was the case with this patient who presented with poliomyelitis sequelae), a small femur and osteopenia secondary to abnormal weight-bearing and muscle hypotrophy. Other factors include vascularity, type of fracture and previous treatments (in the patient from this case study, two DCP plates were applied; the first broke and the second wore and detached without achieving consolidation of the initial fracture). Systemic factors also play a role, such as immunosuppression, chronic and degenerative diseases, smoking (the patient from this study smoked 5 cigarettes a day) and substance abuse, which, combined with the factors described above, are determining factors in the development of either hypertrophic or atrophic pseudarthrosis according to the classification proposed by Weber and Cech. The patient was radiologically confirmed to have atrophic pseudarthrosis, resulting in poor vascularity that further hindered treatment. Many different pseudarthrosis treatment approaches have been mentioned, such as the use of intramedullary nails, various types of plate and external fixators, coupled with the application of autologous grafts, xenografts, cell therapy for osteogenesis and osteogenesis induction, which have achieved a high cure rate in approximately 8–12 months.1–8 The patient from this study underwent intramedullary nailing with a Luque rod (given that the diameter of the medullary canal was 5mm), thereby preventing angular deformity, displacement and overriding fragments. Two semi-tubular frozen fibular grafts were fixed with 3.5-mm osteoinductive and osteoconductive cortical screws to prevent rotation, and bone graft chips were also used. Initial consolidation was observed at 4 months, with complete consolidation 12 months after surgery, comparable to the findings of other authors.1–8 It should be noted that intramedullary nailing with locking intramedullary nails, rather than Luque rods, would be the ideal treatment for this type of condition in an anatomically normal femur. However, a Luque rod was used as there is no nail on the market that corresponds to the 5-mm diameter of the medullary canal of the bone in this case. It is important to emphasise that it is the biomechanical principle applied that is fundamental, rather than the specific implant chosen from the wide range available. The use of various implants, which may not be ideal but are nonetheless useful, are extremely beneficial to populations of limited financial means and/or bones with anatomical abnormalities, as with this patient.
Reported complications in the treatment of pseudarthrosis include infection, rupture or wear of osteosynthesis material and persistent pseudarthrosis. The patient did not experience any complications and progressed satisfactorily, achieving consolidation of the pseudarthrosis and resumption of normal activities.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflict of interestThe authors declare that they have no conflict of interests.