Introduction
The right to health information and, more specifically, the right to information on the illness and treatment alternatives is one of the basic pillars of the doctor-patient relationship and an internationally recognised right. Currently, the Law 41/2002 of Patient Autonomy and of the rights and obligations as regards clinical information and documentation recognised in its Article 5 on the rights of the patient to health information, which becomes, therefore, an obligation of the doctor.
Informing the patient is based on the right to health protection and on patient freedom. Its aim is to guarantee the success of treatment by providing the patient with the data which will enable him/her to accept and understand their illness, to organise and adapt their behaviour during treatment and it allows the doctor to give coherent explanations throughout, as well as justifying his advice and decisions during the disease process.
One of the characteristics which defines the specialty of Family Medicine is the development of a continuous relationship between the doctor and the patient.2 Therefore, information in primary care has some peculiarities, since it is a continuous and continued process, made up of the accumulation of small parts of the patients' lives and the sum of a collection of decisions which have to be taken each time, and which makes it different from the information process in the hospital environment. Several studies have been carried out to find out what information is given to the patient by questioning them directly; however, there is not much data obtained directly from the professionals themselves.
Several studies carried out in different countries agree that the motivation and satisfaction of family doctors has decreased significantly over the last few years and that discontent in these professionals is widespread. As a professional group, family doctors are at odds with the current situation in which they carry out their professional work and they present sufficiently unified opinions as regards the need to carry out specific reforms.3
The importance of professional satisfaction lies, among other factors, in that the quality of the services offered in a health system is directly related with the level of satisfaction of the professionals who work in it and its links to motivation. Ignoring the needs for satisfaction and motivation of the professionals can turn into situations characterised by a sense of distancing, depersonalising and professional inadequacy, and the subsequent loss in the quality of the services.
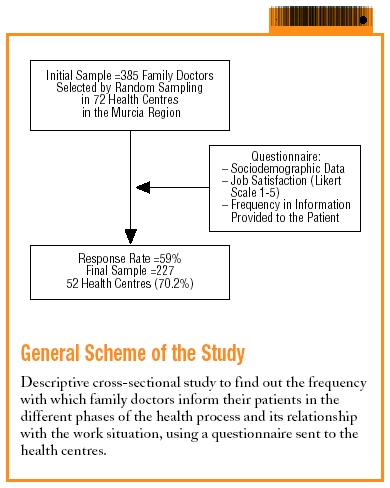
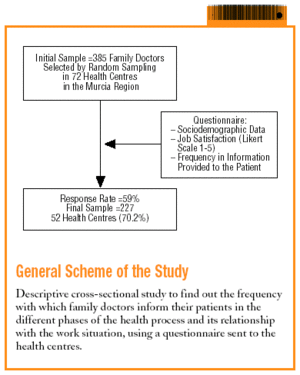
The objective of the study is to describe the information given to patients by primary care doctors during the care process and to analyse whether it is related to the socio-professional factors in which their care work is carried out.
Pacients and methods
Type of Study
Descriptive cross-sectional study.
Study Population
The sample was obtained from all the family doctors who practiced in the different health centres in the Murcia Region in the year 2002.
The size of the initial sample was 385, calculated with a P=.5, a precision of 5% and a 95% confidence level. The selection of the doctors was carried out by stratified random sampling.
The data was obtained by a validated and self-administered questionnaire. The brainstorming technique was used in the preparation of the questionnaire, in which 7 family doctors and 3 university lecturers took part.
To study the internal consistency in a first phase, the questionnaire was answered by 30 doctors who gave suggestions for improvement and, with the results obtained the Chronbach alpha test (*=.87) was applied, resulting in 11 items to define the
social/work factors (Table 1), 4 items which established job satisfaction in daily practice (measured using a 1 to 5 Likert scale), the belonging to a professional group, salary and conduct of their immediate superiors, and 5 items to evaluate the frequency in which the professionals informed their patients on the diagnosis, prognosis, treatment, complementary examinations, and the work and the social/family impact of its process.
Data Collection Method
The questionnaires were sent by post and it was requested that the primary care team managers distribute them to the family doctors at the selected centres and that they completed them voluntarily and anonymously. The responses were sent to the researcher in a sealed envelope.
Statistical Analysis
For the statistical analysis of the data the SPSS 11.0 package was used; the programs applied were simple frequency distribution and the association between variables (Pearson *2).
Results
The final sample was 227 family doctors, which represented a response rate of 59%. Out of a total of 72 primary care teams, 56 replied to the questionnaire (77.7% of primary care teams in the region).
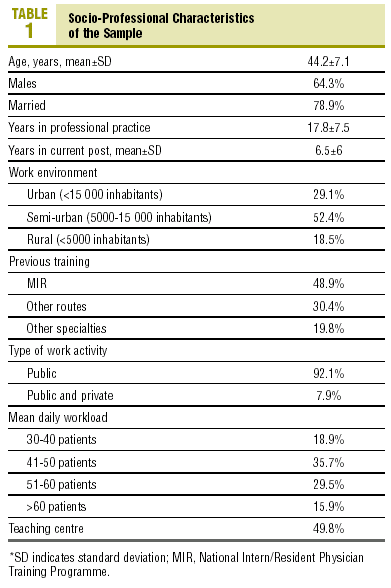
Social-Work Factors of the Professionals
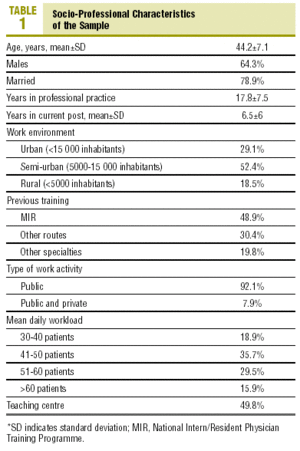
The social-work factors of the sample studied are set out in Table 1. The professionals surveyed were mainly in the 36-55 years age range (84.6%), males were almost double that of females, and the majority were married. The majority of doctors (52.4%) were in the group with 11-20 years of professional practice, followed by the group with 21-30 years experience (26%). As regards length of time in the post at the time of filling in the questionnaire, 30% were less than 3 years, followed by 26% with 3-5 years. These figures decreased progressively until arriving at the group who were more than 15 years (11%). The work environment where the majority of professionals practiced was a semi-urban one.
The previous training of these professionals was mainly through the National Intern/Resident Physician Training Programme (MIR) in Family and Community Medicine, and a small proportion had gained the title of Specialist by different assimilation courses or by other specialties.
They performed their activity mainly and exclusively in the public sector. The number of patients allocated to each doctor is generally between 1901-2100 (32.6%) and only 20.3% have less than 1500 registered patients. The majority of doctors see 41-50 patients per day and practice in a teaching centre.
Job Satisfaction of the Doctors
The mean levels of satisfaction of these doctors (determined using a Likert 1-5 scale, 5 being the highest level of satisfaction) as regards salary, belonging to a professional group, performance of their superiors and daily consultations are as follows, respectively: 2.59 (95% confidence interval [CI], 2.47-2.71); 3.24 (95% CI, 3.11-3.37); 2.33 (95% CI, 2.18-2.48); and 3.01 (95% CI, 2.89-3.13).
Information During the Phases of the Health Care Process
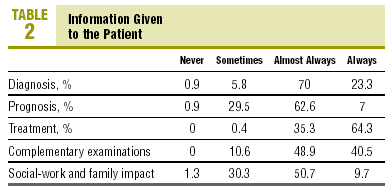
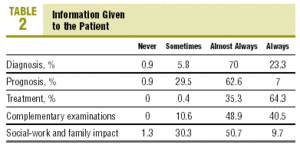
50.7% of the doctors only provided oral information to the patients; the remainder gave combined oral and written information. Only 23.3% of the doctors always informed the patient of the initial diagnosis. Exclusively, 7% of the doctors always informed the patient on the prognosis, a percentage which increased to 64.3% when it was information regarding therapeutic treatment. As regards the reason for complementary examinations, 40.5% always gave information. Finally, only 9.7% always gave information on the social-family and work impact which their illness can make. The questions asked and the percentages obtained are set out in Table 2.
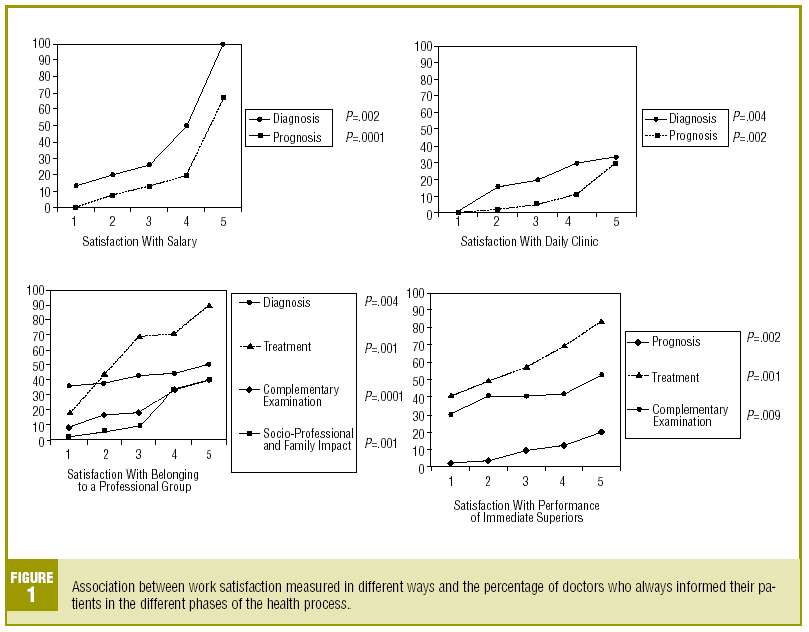
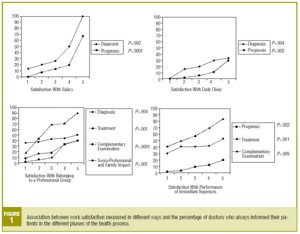
We observed that there is a statistically significant increase in the number of doctors who provide information to patients more frequently in the different phases of the care process when the level of professional satisfaction is higher in the various aspects assessed (Figure 1).
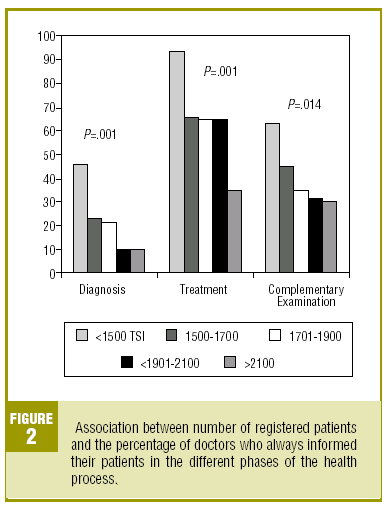
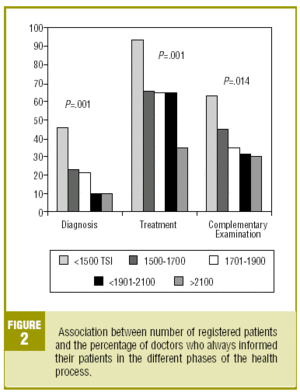
We found a statistically significant relationship between age and the information on the complementary examinations; those who, in the main, always inform their patients are the ones younger than 35 years (65%; P>.001). We also found a significant indirect relationship between the number of registered patients and the information provided to patients on the diagnosis, and the indications for the complementary examinations. The majority of professionals with less than 1500 registered patients always provided information on the diagnosis (45.7%; P<.001), treatment (93.5%; P<.001) and complementary examinations (63%; P=.014) (Figure 2).
Discussion
Comparison with data from other studies is difficult, since in the majority of studies looked at, they included patients and health users as study subjects to evaluate the amount and quality of health information given, or in some cases, they were centred on direct observations of this situation in the clinic.4 However, our results come from the personal assessment of the doctors, with which we evaluate not specific operations, but the general performance which is normally practised as regards the providing of information to their patients.
It should be underlined that the patient's right to information can be dissociated from any act of will on their part, so the information does not always have to be conceived as a pre-condition of free therapeutic choice by the patient, but it does entail the right to know the state of their health and its process at all times. This right to health information not only applies to the ill patient, but also to the healthy one, to gain access to their right to health protection, which will allow them to adopt preventive measures or life attitudes which could benefit their state of health.5
The results obtained show that, in almost half the cases, the doctors provide information to the patient almost exclusively orally, while the remainder use a combination of oral and written. As regards the initial diagnosis, treatment and complementary examinations, a high percentage of family doctors always or almost always inform (93.3%, 99.6%, and 89.4%, respectively). These percentages decrease on information on the prognosis and the social-family impact of the process (69.7% and 60.7%, respectively), probably due to caution when faced with these 2 phases of the health process in primary care. However, it must be pointed out that the number of doctors who always inform only in the case of information on treatment, is in excess of 50% (64.3%), while information on the diagnosis (23.3%), the prognosis (7%), the complementary examinations (40.5%) and the social-work and family impact of the process (9.7%) is deficient. Therefore, we consider that compliance to the duty of informing does not reach sufficient levels, a fact which is in agreement with other investigations carried out in the primary care4 and hospital environment.8
There is serious concern, from the health sector, on the quality level of the care provided to the community, as well as the level of user satisfaction, but less attention is paid to the work-related health of health professionals themselves.
However, it has been established that professional dissatisfaction entails a serious social and economic cost, due to its effect on the work climate, the salary and the provision of health care.9 The level of quality of services provided in a health system is directly related with the level of satisfaction of the professionals who work in it, it highlights that their demoralisation is the main difficulty which the directors and managers of health centres have to face up to.10,11 Different factors which cause dissatisfaction in doctors have been investigated and in many studies, the perception of loss of autonomy has been identified as one of the most important factors.12-15 Different authors also mention that patient workload, bureaucracy, limited resources, the inadequate communication with medical specialists and the inability to maintain a continuous relationship with patients, particularly factors which limit patient care and decrease the quality of care, increase professional dissatisfaction.16-18 To the list of causes of dissatisfaction, specific problems can also be added, lack of incentives and professional salary.19,20
We have found that family doctors are dissatisfied, particularly as regards economic reward and with the performance of their immediate superiors, and only achieve an intermediate level of satisfaction or indifference as regards their daily practice and the belonging to a professional group. In Spain, other authors have shown this professional demotivation and dissatisfaction.21,22 It also needs to be taken into account that professional satisfaction affects patient satisfaction,23,24 since professional dissatisfaction can negatively influence the behaviour of the patient, as for example, in the compliance of medical treatment, bringing about a decrease in health quality.25
The results we have obtained show that professional satisfaction measured in several ways and health workload measured as the number of registered patients is significantly associated with the information provided to the patients. Generally, we observed that there is a progressive increase in the number of professionals who always inform as professional satisfaction increases, and the professionals with a lower number of registered patients inform their patients more. This enables us to highlight the negative consequences of professional dissatisfaction and the high health workload on the right to patient health information.
We can conclude that compliance with the right to information does not reach satisfactory sufficient levels. There is generalised work dissatisfaction among family doctors which negatively influences the rights of the patient to information. An acceptable workload significantly improves the information provided to patients.
Sufficient interest needs to be generated in the professional so that they accept the practical importance of clinical information in their work activity, not only as a legal requirement, but also as a therapeutic element of confidence and reinforcement in the health process.