Morbid obesity is a very prevalent disease in western societies. Nonalcoholic steatohepatitis is a common entity among morbidly obese individuals, which is becoming established as an emerging indication for liver transplantation with the increasing number of surgical procedures aimed at improving weight and the metabolic syndrome. In certain patients who undergo purely malabsorptive procedures, a decline in hepatic function has been identified to the extent that some cases require liver transplantation. This has raised the controversy of whether to revert the bariatric procedure, and when is the most opportune time for doing so.
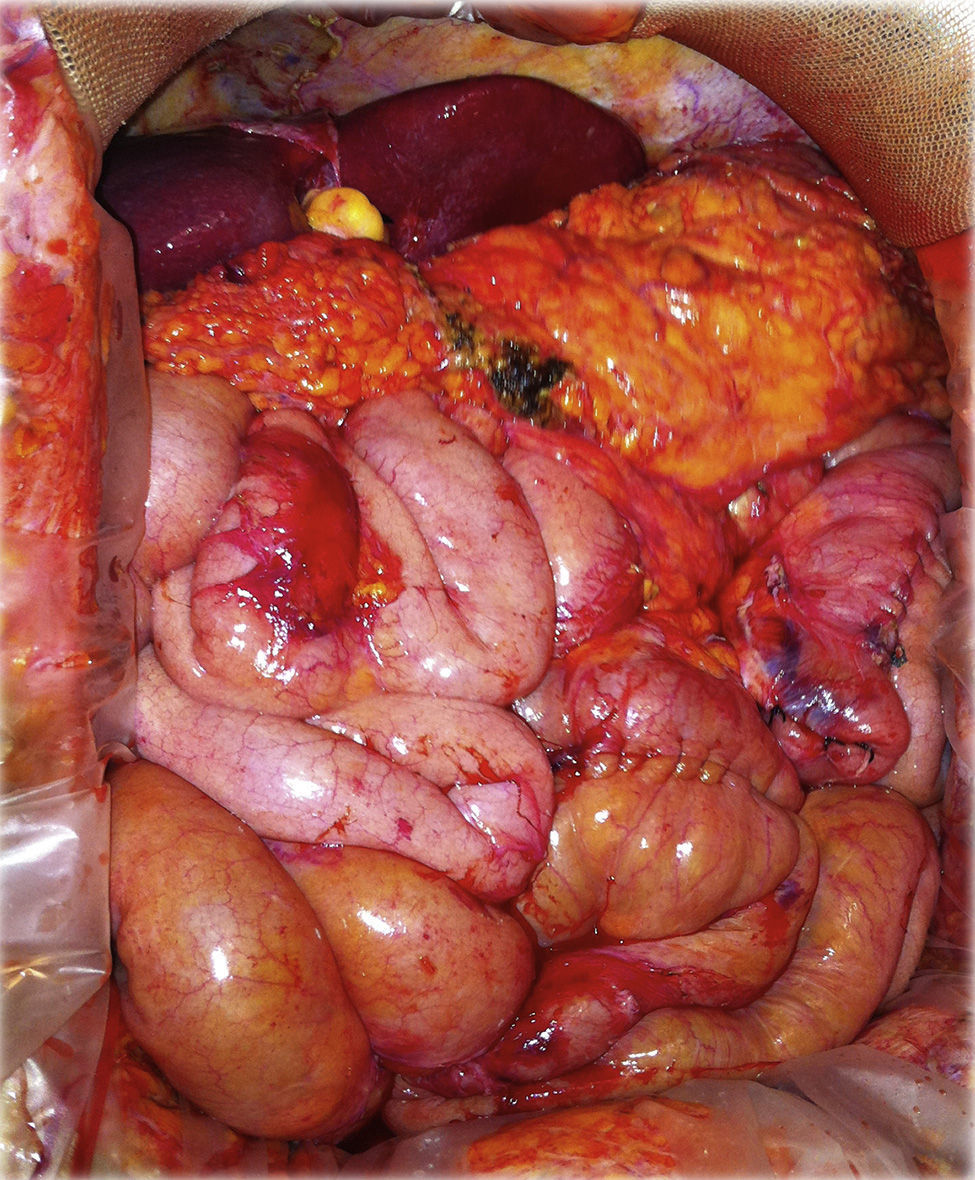
Our patient is a 35-year-old male who had undergone biliopancreatic diversion (Scopinaro procedure) 12 months earlier due to morbid obesity, which resulted in a weight loss of 120% of his previous excess weight and malnutrition (body mass index 18kg/m2). He was transferred to the ICU of our hospital because of progressive acute liver failure with clinical deterioration and MELD 40, which indicated a “code 0” liver transplantation. Orthotopic liver transplantation was carried out with an organ from a cadaveric donor, and the decision was made to revert the previous biliopancreatic diversion (Fig. 1). During the immediate postoperative period, the patient presented haemodynamic deterioration secondary to massive haemoperitoneum. Urgent exploratory laparotomy identified active bleeding at the jejunojejunal anastomosis, which was controlled. The other anastomoses were undamaged and showed no signs of leakage.
During post-op, the patient presented ascites with associated renal failure and a need for haemofiltration. On the 8th day post-op, the patient experienced acute respiratory failure secondary to septic shock, which required re-admittance to the ICU, vasoactive drugs and mechanical ventilation. Abdominal ultrasound and CT scan ruled out surgical complications as well as an absence of alterations of the liver graft. After paracentesis, a culture of the ascitic fluid identified the presence of multi-resistant Enterococcus faecium, and Candida glabrata was detected in the bronchial suction culture. In the end, the patient died on the 18th day post-op in a situation of refractory septic shock. The pathology study of the explanted specimen demonstrated submassive hepatic necrosis with marked regenerative signs and severe macro-microvesicular steatosis.
The prevalence of obesity has increased in recent years, and nonalcoholic steatohepatitis is a condition that is increasing in frequency. Bariatric surgery plays an important role in the treatment of these patients as it results in weight loss, controls cardiovascular risk factors and improves associated metabolic syndrome.1 Nonetheless, the effect of bariatric surgery on liver function is controversial. Malabsorptive techniques, such as the Scopinaro procedure, are responsible for the development of postoperative hepatic complications, and there have been publications of cases of acute liver failure in small series.2 Geerts et al.2 published a Belgian multicentre study with a series of 10 patients who developed liver failure after bariatric surgery (Scopinaro in 9 patients and intestinal bypass in one) and received liver transplants. D’Albuquerque et al.3 published the cases of 3 patients with a history of bariatric surgery (1 gastric bypass and 2 biliopancreatic diversions) who later developed liver failure and received liver transplants between 7 and 24 months afterwards.
We currently do not understand the exact cause of this condition, although several physiopathological theories have been proposed that would result in the appearance of liver damage after malabsorptive procedures. One of the main factors involved is bacterial overgrowth of the excluded intestine, which would injure the mucosa, favouring bacterial translocation that would be responsible for the hepatocellular damage.2 The main factors that favour these processes are: absence of bile in the affected segment, decreased gastric acid secretion and altered intestinal motility. All these factors induce changes in the intestinal flora, as demonstrated by Drenick et al.4 Another related factor is the nutritional protein deficit associated with the procedure, which can increase fatty deposits in the liver.2 Acute liver failure is probably a consequence of the simultaneous action of these factors, together with other preoperative factors. This is aggravated by drastic weight loss, which generates the mobilisation of adipocytes and implicates a release of inflammatory mediators, which ultimately favours the lipotoxicity involved in steatohepatitis.5
For these reasons, some authors endorse simultaneous or sequential reversal of the bariatric procedure in patients who undergo liver transplantation as it meets three objectives: nutritional optimisation, elimination of factors that aggravate steatohepatitis and improved absorption of immunosuppressants. After a review of the published literature, we have only found isolated cases that concur with our actions and reverted the prior surgery during transplantation, such as the series published by Geerts et al.2 In one case that is especially interesting, the bariatric procedure was reverted 8 weeks post-transplantation due to the instability of the patient.
Thus, malabsorptive surgeries like the Scopinaro procedure entail a potential risk for associated hepatic failure and require strict patient follow-up with periodical liver function studies.
Currently, a predominance of restrictive procedures are being performed, which diminish the metabolic and histological alterations of steatohepatitis.6 Nonetheless, in spite of their safety profile, some cases of liver failure after bariatric surgery have likewise been published.3,7,8
Please cite this article as: Rodríguez Silva C, Fernández Aguilar JL, Sánchez Pérez B, Suárez Muñoz MÁ, Santoyo Santoyo J. Insuficiencia hepática aguda secundaria a cirugía bariátrica: una indicación de trasplante hepático. Cir Esp. 2016;94:113–114.