Rickettsia sibirica mongolotimonae was isolated for the first time in 1992 in Beijing as a subspecies of R. sibirica from ticks from the Inner Mongolia region, hence its name.1 Its pathogenicity has been verified in humans, and although the number of cases described is small, in recent years it has been increasingly reported.2
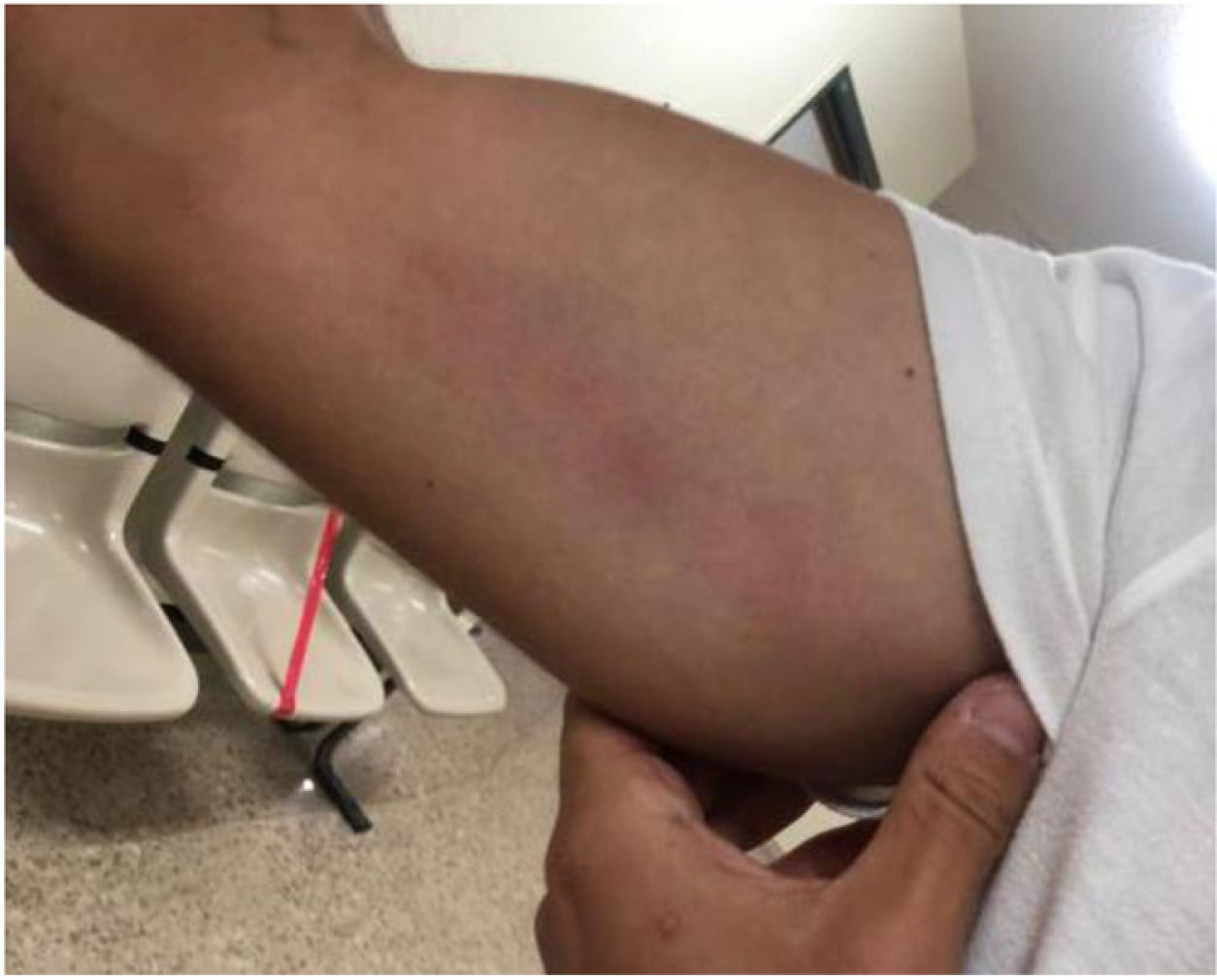
We present the case of a 29-year-old male with no medical history of interest who sought treatment at our centre in June 2021 for fever, general malaise, myalgia and headache lasting four days. He had returned two days earlier from a holiday in a rural area in the Luena Valley (Cantabria), in northern Spain, and said that he had suffered an insect bite on the outer side of his right forearm two days before the start of symptoms. On physical examination, his temperature was 38°C, his blood pressure was 110/70 mmHg and his heart rate was 90 bpm. He had a necrotic eschar on his right forearm of approximately 1 cm in diameter, accompanied by proximal lymphangitic streaking (Fig. 1) and a painful axillary adenopathy of approximately 1 cm not attached to deep planes. The rest of the examination was normal. The complete blood count showed a leukocyte count of 6,100, with an absolute lymphocyte count of 930, and normal haemoglobin and platelet counts. Biochemical test results, including transaminases, were normal, except for C-reactive protein, which was 16 mg/l (normal: <10.0 mg/l). There were no relevant findings on the chest X-ray. Detection of antibodies to Rickettsia, Borrelia, Francisella tularensis and Anaplasma phagocytophilum was negative, while a real-time PCR (polymerase chain reaction) test (performed at the Centro Nacional de Microbiología Carlos III, [Carlos III National Centre for Microbiology] in Majadahonda, Madrid) on a biopsy of the necrotic eschar was positive for Rickettsia sibirica mongolotimonae. The patient was treated with doxycycline 100 mg every 12 h for 10 days, showing progressive clinical improvement until complete recovery and disappearance of the skin lesions and adenopathy. Six months later he remains asymptomatic.
In addition to general symptoms such as fever, general malaise and myalgia, the skin manifestations of Rickettsia mongolotimonae are very characteristic, which allows for a rapid diagnosis of suspicion. As in our case, a small necrotic eschar on a limb is typically found in up to 90% of patients,3 and cases have even been described with multiple accompanying eschars. This lesion can be continued by reddish proximal lymphangitic streaking, which is identified in approximately 45% of cases and is accompanied by local adenopathies,4 for which the name lymphangitis-associated rickettsiosis (LAR) has been proposed.5 Other types of local lesions have also been described, such as erythematous papular rash on the trunk and limbs, lymphadenopathy and scarring alopecia.6 The infection is generally mild and responds well to treatment with tetracyclines, but cases with severe manifestations have been described, such as retinal vasculitis, hyponatraemia, shock, myopericarditis, encephalitis and acute renal failure.6
Diagnosis has improved remarkably since specific PCR studies have been available on biopsy samples or smears from skin eschar.6 Serological methods are less sensitive and have the drawback of cross-reactions with other Rickettsia that are present in our environment.7
In Europe, Rickettsia sibirica mongolotimonae has been isolated from ticks of the genera Rhipicephalus and Hyalomma, and the first infection in humans was diagnosed in 1996 in southern France.2 Since then, multiple cases have been reported, mostly in the Mediterranean region (France, Spain, Portugal, Greece and Turkey). Cases have also been reported in some African countries (Algeria, Egypt, Cameroon and South Africa).8 In Spain, several cases have been described, predominantly in the Mediterranean coastal region, and in the centre and north of the peninsula.9 As far as we have been able to ascertain, our case is the first reported case of contagion in the community of Cantabria.